Anterior Communicating Artery - The Frontal Link
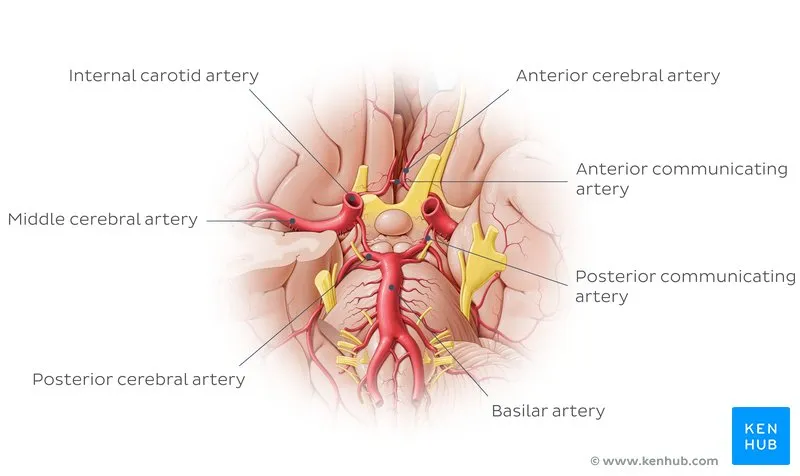
- Function: A short vessel that connects the left and right Anterior Cerebral Arteries (ACAs), completing the anterior part of the Circle of Willis.
- Location: Situated superior to the optic chiasm.

- Clinical Significance:
- Most common site for saccular (berry) aneurysms.
- Rupture leads to subarachnoid hemorrhage (SAH).
- Compression from an aneurysm can cause:
- Visual defects: Bitemporal hemianopia (due to pressure on the optic chiasm).
- Frontal lobe syndrome: Personality changes, abulia (lack of initiative), and executive dysfunction.
⭐ High-Yield: Aneurysms of the AComm are the most frequent cause of subarachnoid hemorrhage in the Circle of Willis. Sudden, severe "thunderclap" headache is a classic presentation.
Posterior Communicating Artery - The Side Connector
- Bridge Function: Connects the anterior circulation (Internal Carotid Artery) to the posterior circulation (Posterior Cerebral Artery).
- Anatomical Course: Travels posteriorly from the ICA, passing superior to the oculomotor nerve (CN III), to anastomose with the PCA.
- Key Branches: Gives rise to small thalamoperforating arteries.
- Supply: Thalamus (anterior and ventral nuclei), hypothalamus, optic chiasm, and mammillary bodies.
- Clinical Pearl: Common site for berry aneurysms.
⭐ A classic exam scenario involves a PCom aneurysm compressing the ipsilateral oculomotor nerve (CN III). This leads to a fixed, dilated pupil (“blown pupil”), ptosis, and a “down and out” gaze due to unopposed CN IV and VI action.
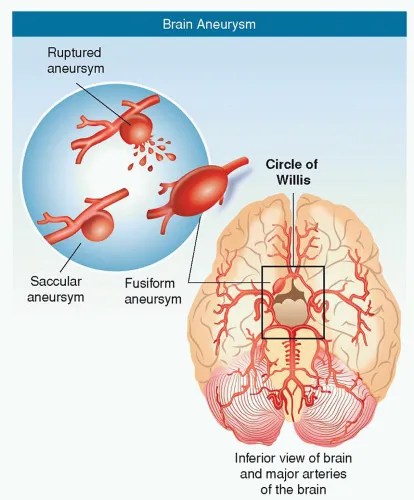
Aneurysms & Strokes - When Links Break
- Berry (saccular) aneurysms: Congenital weaknesses in arterial walls, predisposing to rupture. They are the most common cause of non-traumatic subarachnoid hemorrhage (SAH).
- Anterior Communicating Artery (AComm): Most common site. Rupture can cause SAH, while compression of the optic chiasm may lead to bitemporal hemianopia.
- Posterior Communicating Artery (PComm): Aneurysms at the junction with the internal carotid artery can compress the oculomotor nerve (CN III).
⭐ A PComm aneurysm classically presents with a painful CN III palsy: the eye is deviated "down and out," with ptosis and a fixed, dilated pupil (mydriasis) due to compression of superficial parasympathetic fibers.
High‑Yield Points - ⚡ Biggest Takeaways
- The Anterior Communicating Artery (ACommA) is the most common site of saccular (berry) aneurysms.
- The Posterior Communicating Artery (PCommA) is the second most common site.
- Rupture of these aneurysms is a major cause of subarachnoid hemorrhage (SAH).
- ACommA aneurysms can compress the optic chiasm, causing bitemporal hemianopia.
- PCommA aneurysms can cause CN III palsy, with a fixed, dilated pupil and a “down and out” eye.
- They provide critical collateral circulation between hemispheres and circulations.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

