Circle of Willis - The Brain's Roundabout
- Anastomotic ring of arteries at the base of the brain, providing collateral circulation.
- Connects the anterior (carotid) and posterior (vertebrobasilar) circulatory systems.
- Function: Protects against ischemia by providing alternative blood routes if a major artery is occluded.
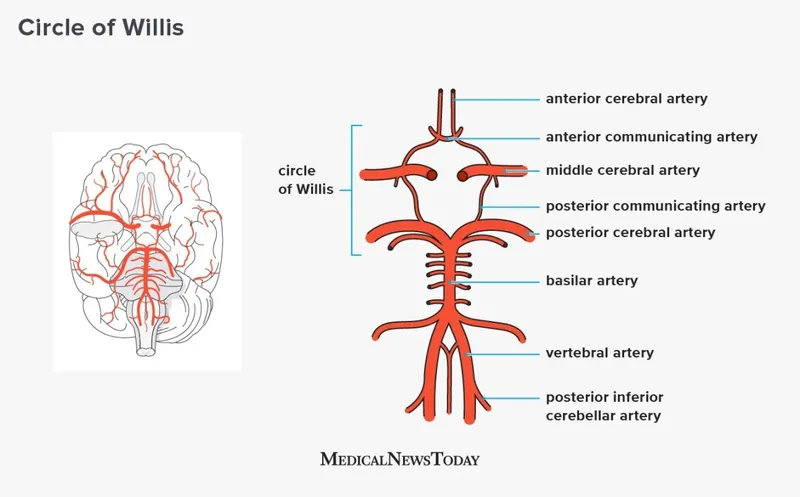
- Major Components:
- Anterior Cerebral Artery (ACA)
- Anterior Communicating Artery (AComm)
- Internal Carotid Artery (ICA) terminus
- Posterior Cerebral Artery (PCA)
- Posterior Communicating Artery (PComm)
⭐ Clinical Pearl: Anatomical variations are common. A complete, textbook circle is present in only ~20-25% of individuals, increasing stroke risk if a feeding artery is compromised.
Collateral Pathways - The Brain's Backup Plan
- Function: Provides redundancy in cerebral blood flow to protect against ischemia/infarction when a major vessel is occluded or stenosed.
- Primary Anastomotic Routes:
- Anterior Communicating A. (ACoA): Connects the left and right Anterior Cerebral Arteries (ACAs).
- Posterior Communicating A. (PCoA): Connects the Internal Carotid Artery (ICA) system with the Vertebrobasilar system (via the Posterior Cerebral Artery - PCA).
- Extracranial to Intracranial Collaterals:
- Crucial when major intracranial arteries are occluded.
- Ophthalmic Artery: Retrograde flow from branches of the External Carotid Artery (e.g., facial artery, maxillary artery) can supply the Ophthalmic Artery, which then feeds the ICA.
⭐ Clinical Pearl: The classic, complete Circle of Willis is present in only ~20-25% of individuals. Anatomical variations are common and are a major risk factor for transient ischemic attacks (TIAs) or strokes if a contributing artery becomes stenosed.
Clinical Significance - When Flow Goes Wrong
- Failure of collateral circulation leads to ischemic stroke. The clinical deficit depends on the territory of the occluded vessel.
- Vulnerability is significantly increased by:
- Anatomical variations (very common).
- Atherosclerosis narrowing the communicating arteries.
- Ischemic Penumbra: Brain tissue surrounding the core infarct; it is hypoperfused but still viable and potentially salvageable if blood flow is restored promptly.
⭐ A complete, patent Circle of Willis is found in only ~20-25% of individuals. This high frequency of anatomical variation is a primary determinant of the extent and severity of a stroke following a major vessel occlusion.
High‑Yield Points - ⚡ Biggest Takeaways
- The Circle of Willis is the brain's most critical arterial anastomosis, essential for collateral circulation.
- It provides redundancy in blood supply, protecting the brain from ischemia during arterial occlusion.
- Key connectors are the Anterior Communicating (ACOM) and Posterior Communicating (PCOM) arteries.
- Anatomical variations are common, often resulting in an incomplete circle and increasing stroke risk.
- Junction points, especially the ACOM, are frequent sites for saccular (berry) aneurysms.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

