Gross Anatomy - The Right-Sided Giant
- Location: Right upper quadrant (RUQ), deep to ribs 7-11.
- Lobes (Anatomical):
- Large right lobe, smaller left lobe.
- Posterior: caudate & quadrate lobes.
- Ligaments:
- Falciform: Attaches liver to anterior abdominal wall.
- Ligamentum Teres (Round Ligament): Remnant of fetal umbilical vein.
- Coronary & Triangular: Attach superior liver to diaphragm.
- Dual Blood Supply:
- Hepatic Artery Proper (30%): Oxygenated blood.
- Portal Vein (70%): Nutrient-rich blood from GI tract.
⭐ Exam Favorite: The functional division of the liver is based on blood supply, not the falciform ligament. Cantlie's line, from the IVC fossa to the gallbladder fossa, separates the true right and left functional lobes.
Vasculature & Biliary Tree - The Hepatic Highway
- Dual Blood Supply:
- Portal Vein (75%): Nutrient-rich blood from the gut.
- Proper Hepatic Artery (25%): Oxygen-rich blood.
- Venous Drainage: Central vein → Hepatic veins → Inferior Vena Cava (IVC).
- Portal Triad: Contained within the hepatoduodenal ligament; consists of the proper hepatic artery, hepatic portal vein, and common hepatic duct.
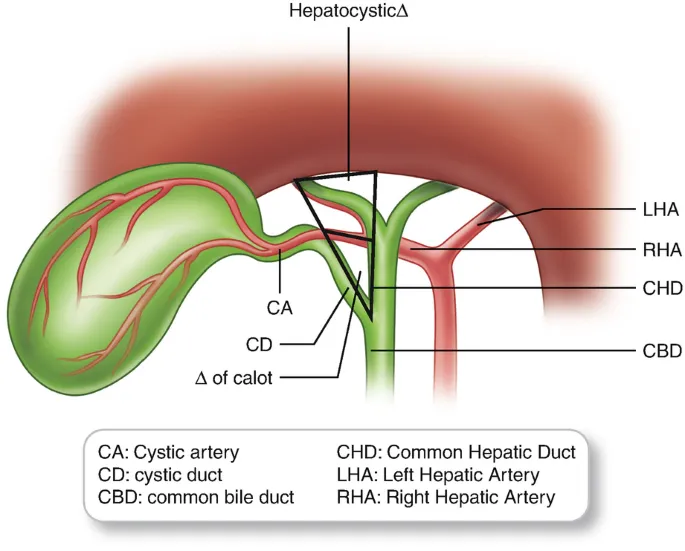
⭐ Triangle of Calot: A critical surgical landmark for cholecystectomy. Its boundaries are the cystic duct, common hepatic duct, and the inferior border of the liver. The cystic artery is typically found within this triangle.
Gallbladder & Friends - Bile's Waiting Room
- Function: Stores & concentrates bile produced by the liver.
- Anatomy:
- Pear-shaped sac in a fossa on the liver's visceral surface.
- Parts: Fundus, Body, Neck (continuous with cystic duct).
- Bile Flow:
- Cystic Duct + Common Hepatic Duct → Common Bile Duct (CBD).
- CBD joins the main pancreatic duct, emptying into the duodenum via the Ampulla of Vater, regulated by the Sphincter of Oddi.
- Neurovascular:
- Artery: Cystic a. (from Right Hepatic a.).
- Innervation: Vagus (contracts), Sympathetics (relax).
⭐ Calot's Triangle: Critical surgical landmark for cholecystectomy. Boundaries: Cystic duct (inferiorly), common hepatic duct (medially), and inferior liver edge (superiorly). Contains the cystic artery.
Clinical Correlations - When Plumbing Fails
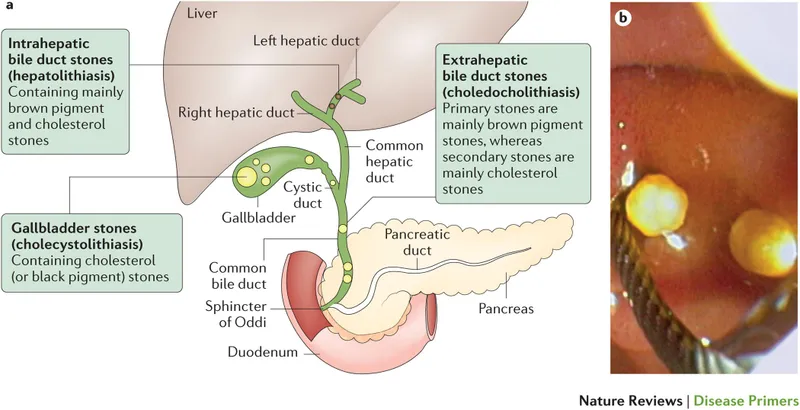
- Cholelithiasis (Gallstones): Often asymptomatic. Can cause biliary colic (RUQ pain). Risk factors (📌 4 F's): Female, Fat, Fertile, Forty.
- Cholecystitis: Gallbladder inflammation from cystic duct obstruction.
- Presents with steady RUQ pain, fever, ↑ WBC.
- Positive Murphy's sign.
- Ascending Cholangitis: Biliary tree infection from obstruction (e.g., choledocholithiasis).
- Charcot's Triad: Jaundice, Fever, RUQ Pain.
⭐ Most gallstones (~80%) are cholesterol stones, which are radiolucent on X-ray.
High‑Yield Points - ⚡ Biggest Takeaways
- The portal triad (hepatic artery, portal vein, common bile duct) runs within the hepatoduodenal ligament.
- Calot's triangle (cystic duct, common hepatic duct, liver edge) is the surgical landmark for the cystic artery.
- Gallbladder inflammation refers pain to the right shoulder via the phrenic nerve (C3-C5).
- The common bile duct joins the main pancreatic duct at the ampulla of Vater.
- Liver's dual blood supply: portal vein (~75%) and hepatic artery (~25%).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

