Surface Anatomy - Mapping the Body
-
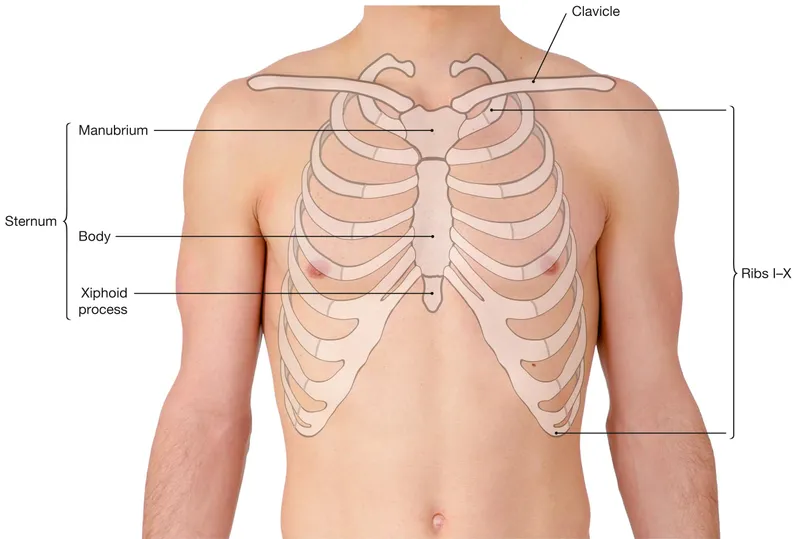
Key Thoracic Landmarks:
- Suprasternal Notch: Palpable dip, level with T2/T3 vertebrae.
- Sternal Angle (of Louis): Manubriosternal joint, level with T4/T5 IV disc. Articulates with the 2nd rib. Marks aortic arch & tracheal bifurcation.
- Xiphoid Process: Level with T9 vertebra; inferior border of heart.
-
Key Abdominal Landmarks:
- McBurney's Point: Two-thirds from umbilicus to ASIS. Tenderness suggests appendicitis.
- Mid-inguinal Point: Midway between ASIS & pubic symphysis. Femoral artery pulse/access.
⭐ The Sternal Angle is a vital landmark at the T4/T5 level, marking the 2nd rib, tracheal bifurcation, and aortic arch boundary.
Thoracic Landmarks - Navigating the Cage
-
Sternal Angle (of Louis): Key palpable landmark. Articulates with the 2nd rib, the starting point for counting ribs and intercostal spaces (ICS).
- Marks the level of the T4/T5 intervertebral disc.
- Site of tracheal bifurcation into primary bronchi.
- Location of the aortic arch.
-
Intercostal Neurovascular Bundle: Runs along the inferior margin of each rib.
- 📌 Mnemonic: VAN (Vein, Artery, Nerve) from superior to inferior.
- For procedures (e.g., thoracentesis, nerve block), the needle is inserted superior to the rib below to avoid injury.
-
Thoracentesis: Performed at mid-axillary line, typically in the 8th or 9th ICS during expiration.
⭐ The Sternal Angle marks the T4/T5 vertebral level, the bifurcation of the trachea, and the beginning/end of the aortic arch.
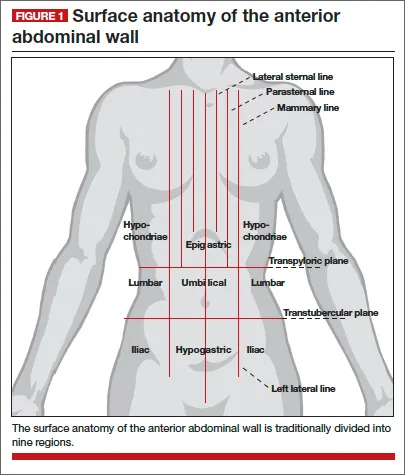
Abdominal Landmarks - Belly's Treasure Map
- Xiphoid Process: Sternum's inferior tip, superior abdominal boundary.
- Costal Margin: Lower border of the rib cage.
- Iliac Crest: Palpable superior border of the ilium, at the L4 vertebral level (lumbar puncture).
- Anterior Superior Iliac Spine (ASIS): Bony point at the anterior end of the iliac crest.
- Umbilicus: Scar at the T10 dermatome level.
Key Clinical Points:
- McBurney's Point: Located one-third of the distance from the ASIS to the umbilicus. Maximal tenderness here is a classic sign of acute appendicitis.
- Murphy's Point: Intersection of the right mid-clavicular line and the costal margin. Elicits Murphy's sign in acute cholecystitis.
⭐ The transpyloric plane, midway between the jugular notch and pubic symphysis, is a crucial horizontal plane transecting the pylorus, gallbladder fundus, and renal hila.
Limb Landmarks - Access & Nerve Blocks
- Upper Limb Access:
- Axillary Sheath: Palpate axillary artery medial to coracobrachialis. Site for axillary nerve block targeting terminal brachial plexus branches.
- Brachial Plexus Blocks: Interscalene (shoulder surgery; risk phrenic n. palsy), Supraclavicular (arm/forearm; risk pneumothorax).
- Wrist: Median n. (b/w palmaris longus/FCR tendons), Ulnar n. (lateral to FCU tendon).
- Lower Limb Access:
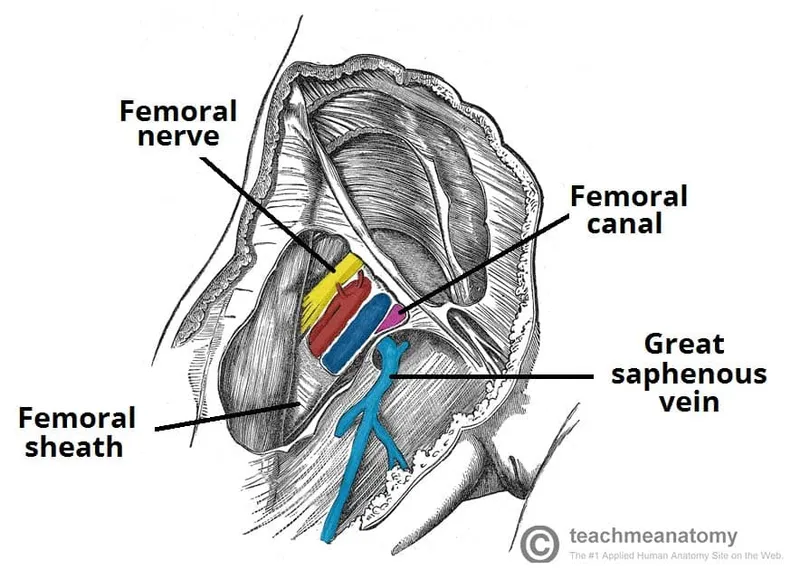
- Femoral Triangle: 📌 NAVEL (Lat→Med): Nerve, Artery, Vein, Empty Space, Lymphatics. Crucial for vascular access & femoral nerve block.
- Sciatic Nerve Block: Midway between greater trochanter and ischial tuberosity.
⭐ Interscalene Block Complication: Anesthetizing the brachial plexus between the scalene muscles (C5-C7 roots/trunks) has a near 100% incidence of transient ipsilateral phrenic nerve palsy, causing diaphragmatic paralysis.
- Central line placement targets the internal jugular vein, found between the sternal and clavicular heads of the sternocleidomastoid muscle.
- Thoracentesis is safely performed in the midaxillary line at the 8th or 9th intercostal space to avoid lung or liver injury.
- Lumbar puncture aims for the L3-L4 or L4-L5 interspace, identified by the line connecting the iliac crests.
- McBurney's point, for appendicitis, is one-third the distance from the ASIS to the umbilicus.
- Cricothyrotomy provides emergency airway access through the cricothyroid membrane.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

