CXR Views & Quality - The Setup
- Standard Views:
- PA (Posteroanterior): Beam passes back to front; preferred view, less cardiac magnification.
- AP (Anteroposterior): Beam passes front to back; often for portable/bedside CXRs.
- Lateral: Left side against detector; complements PA view.
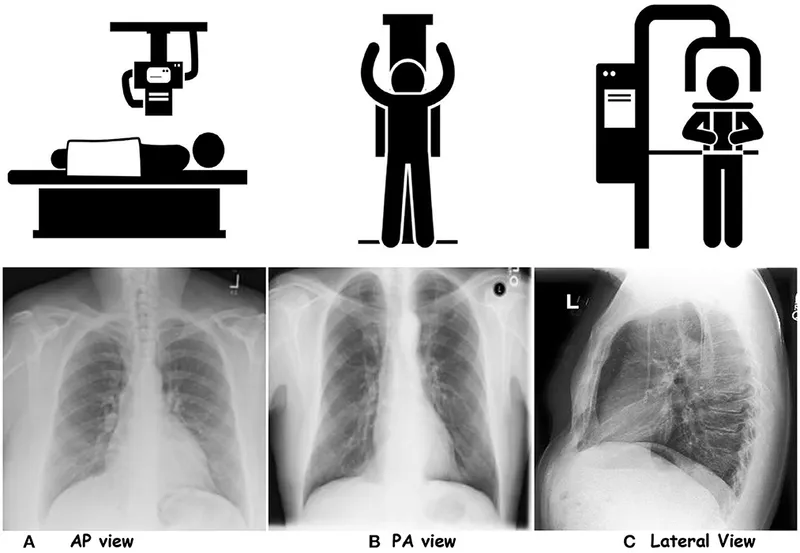
- Quality Assessment (📌 RIPE):
- Rotation: Medial ends of clavicles equidistant from spinous processes.
- Inspiration: Diaphragm at 8-10th posterior ribs.
- Penetration: Thoracic spine visible behind the heart.
⭐ In AP views, the heart appears magnified because it is further from the detector. This can mimic cardiomegaly.
Mediastinal Contours - Lines & Stripes
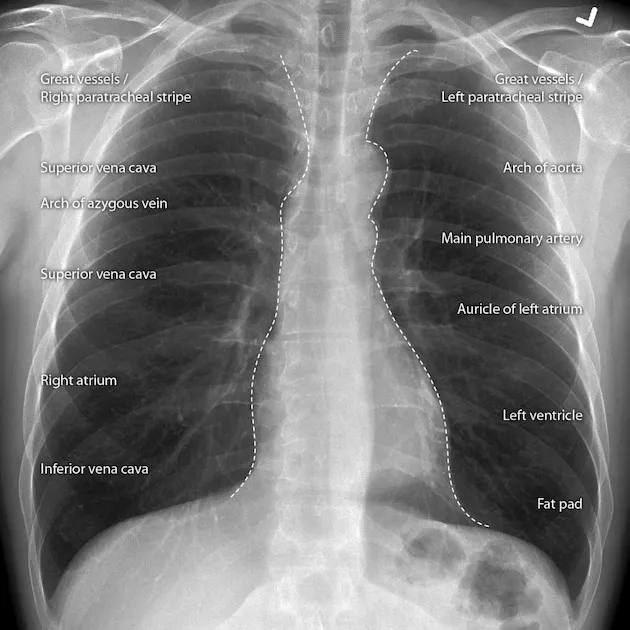
- Anterior Junction Line: Oblique line from clavicles to aortic arch; represents visceral/parietal pleura apposition.
- Posterior Junction Line: Straight line superior to the aortic arch.
- Paratracheal Stripes: Represent the tracheal wall, pleura, and fat.
- Right: Normally <4mm. Thickening suggests lymphadenopathy, pleural effusion, or tracheal pathology.
- Left: More variable; superior to the aortic arch.
- Azygoesophageal Recess: Interface between the right lung and azygos vein/esophagus.
⭐ A convex bulge or displacement of the Azygoesophageal Recess is a reliable sign of subcarinal lymphadenopathy (e.g., lung cancer, sarcoidosis).
Cardiac Silhouette - Heart's Shadow
- Represents the 2D shadow of the heart and great vessels on a chest radiograph.
- Cardiothoracic Ratio (CTR):
- Normally < 0.5 on a posteroanterior (PA) film.
- Calculated as maximal cardiac width divided by maximal thoracic width.
- A CTR > 0.5 suggests cardiomegaly.
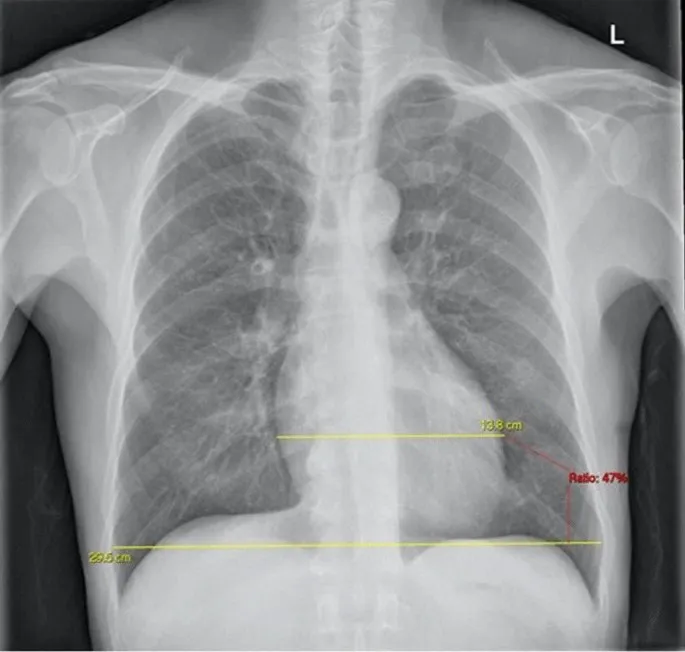
- Borders (PA View):
- Right: Superior vena cava, right atrium.
- Left: Aortic knob, pulmonary trunk, left atrial appendage, and left ventricle.
⭐ On a lateral chest X-ray, the right ventricle occupies the retrosternal space anteriorly, while the left atrium is the most posterior chamber. Esophageal displacement can signal left atrial enlargement.
Hila, Lungs, & Pleura - The Breathing Space
- Hila (Lung Roots): Complex of bronchi, arteries, veins, and lymphatics. The left hilum is typically higher than the right.
- Lung Fields & Fissures: Right lung has 3 lobes; Left has 2.
- Horizontal (minor) fissure: Separates RUL/RML.
- Oblique (major) fissures: Separate lower lobes from the lobes above.
- Pleura & Recesses: Visceral and parietal layers form a potential space.
- Costophrenic angles: Sharp, acute angles formed by the diaphragm and ribs. Blunting suggests pleural effusion.
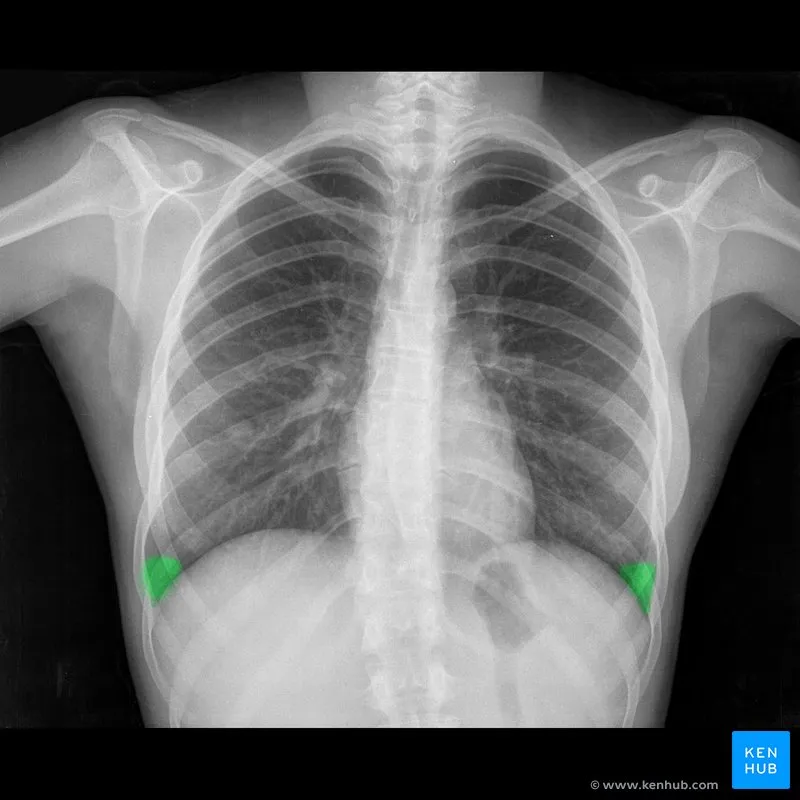
⭐ Pleural Effusion: On an upright CXR, fluid blunts the costophrenic angle. ~200-300 mL of fluid is required to be visible on a PA view, often forming a meniscus shape.
High‑Yield Points - ⚡ Biggest Takeaways
- The aortic knob represents the distal aortic arch; its effacement can indicate an aneurysm or mass.
- The carina, the tracheal bifurcation, is normally found at the T4-T5 vertebral level.
- The right hemidiaphragm is typically higher than the left due to the underlying liver.
- A cardiothoracic ratio >0.5 on a PA chest X-ray is a key sign of cardiomegaly.
- Blunting of the posterior costophrenic angles on a lateral view indicates pleural effusion.
- The left hilum is generally higher than the right.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

