Gross Anatomy - The Cord's Protective Layers
- Vertebral Column: Bony housing for the spinal cord.
- Epidural Space: Contains fat, veins. Site for epidural anesthesia.
- Meninges (Superficial to Deep): 📌 Mnemonic: DAP
- Dura Mater: "Tough mother." Outermost, durable layer.
- Arachnoid Mater: Web-like layer. Creates the subarachnoid space filled with Cerebrospinal Fluid (CSF).
- Pia Mater: "Tender mother." Adheres directly to the spinal cord. Forms denticulate ligaments (anchoring cord laterally) and the filum terminale (anchoring inferiorly).
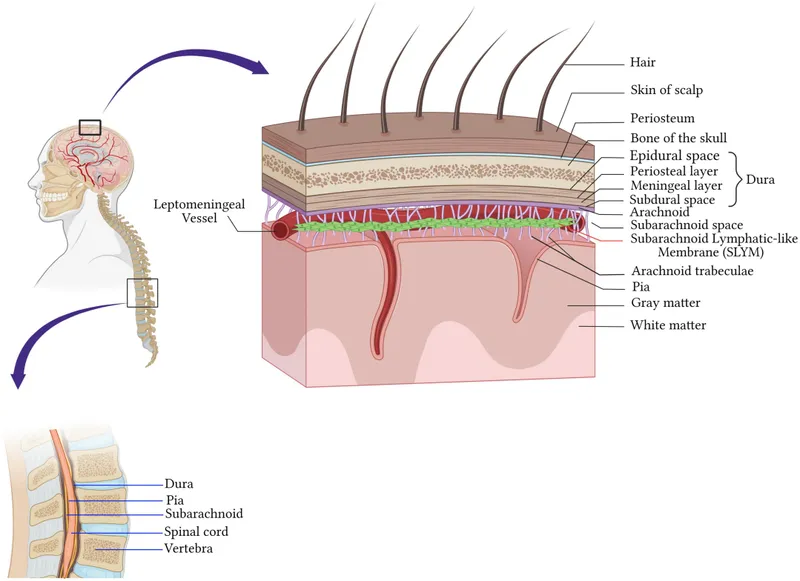
⭐ Clinical Pearl: During a lumbar puncture (spinal tap), the needle must pierce the dura and arachnoid mater to enter the subarachnoid space to sample CSF. The spinal cord ends at L1-L2, but the dural sac extends to S2.
Gray Matter - The Central Butterfly
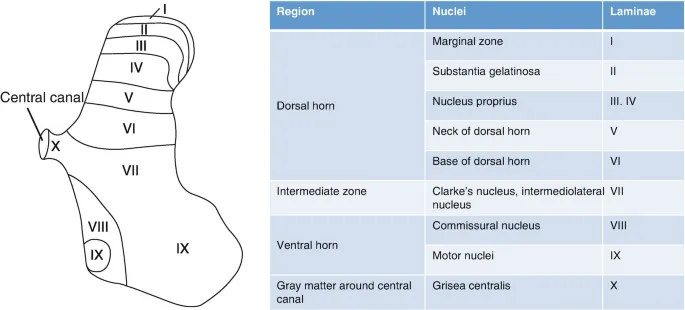
- Dorsal (Posterior) Horn: Sensory input (afferent).
- Substantia Gelatinosa: Pain & temperature modulation.
- Nucleus Proprius: Light touch & proprioception.
- Ventral (Anterior) Horn: Motor output (efferent) to skeletal muscle.
- Contains α- and γ-motor neurons.
- Somatotopically organized.
- Intermediate Zone & Lateral Horn: Autonomic nervous system.
- Lateral Horn (T1-L2): Sympathetic preganglionic neurons.
- Sacral Parasympathetic Nucleus (S2-S4): Parasympathetic preganglionic neurons.
⭐ Exam Favorite: Ventral horn organization is key: axial/proximal muscles are represented medially, while distal limb muscles are lateral. Flexor motor neurons are located dorsally to extensor neurons.
White Matter Tracts - Information Superhighways
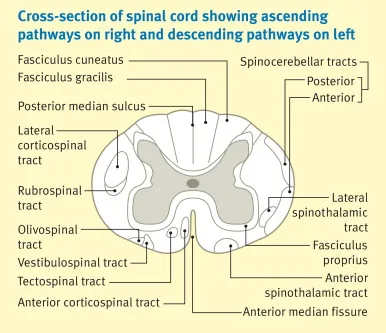
-
Ascending (Sensory) Tracts: Sensory data travels up to the brain.
- Dorsal Column-Medial Lemniscus:
- Function: Fine touch, vibration, proprioception.
- Decussation: Medulla.
- Spinothalamic Tract (Anterolateral):
- Function: Pain, temperature, crude touch.
- Decussation: Spinal cord (anterior commissure).
- Spinocerebellar Tracts:
- Function: Unconscious proprioception to cerebellum.
- Dorsal Column-Medial Lemniscus:
-
Descending (Motor) Tracts: Motor commands travel down from the brain.
- Lateral Corticospinal Tract:
- Function: Voluntary motor control of limbs.
- Decussation: Pyramids (caudal medulla).
- Lateral Corticospinal Tract:
⭐ Brown-Séquard Syndrome (Hemi-section): Ipsilateral UMN weakness, loss of vibration/proprioception below lesion. Contralateral loss of pain/temperature starting 2-3 segments below lesion.
High‑Yield Points - ⚡ Biggest Takeaways
- The spinal cord terminates at the L1-L2 vertebral level; lumbar punctures target the cauda equina.
- Dorsal columns (gracilis, cuneatus) sense proprioception, vibration, and fine touch, decussating in the medulla.
- Spinothalamic tract senses pain, temperature, and crude touch, decussating in the spinal cord.
- Lateral corticospinal tract is the primary motor pathway for voluntary movement, decussating in the pyramids.
- Central gray matter contains cell bodies; surrounding white matter contains myelinated axons (tracts).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

