X-ray Physics - From Electrons to Exposure
-
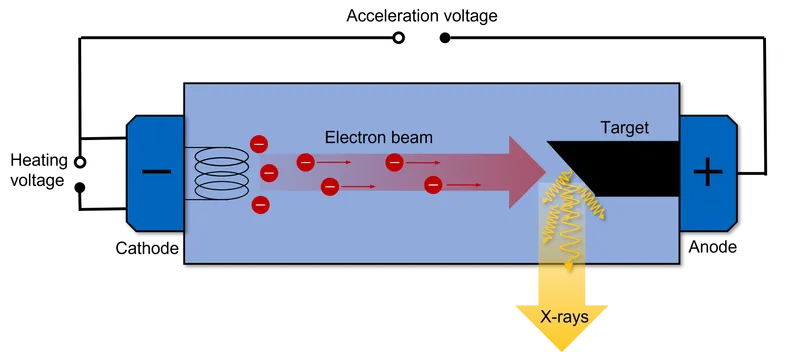
Generation: Electrons from a heated cathode are accelerated by high voltage (kVp) and strike a tungsten anode. <1% of energy becomes X-rays; the rest is heat.
-
Production Mechanisms:
- Bremsstrahlung: "Braking radiation." Primary source. Electron decelerates near the anode nucleus, emitting a photon. Creates a continuous energy spectrum.
- Characteristic: High-energy electron ejects an inner-shell electron; an outer electron fills the vacancy, emitting a photon of discrete energy.
-
Beam Control:
- kVp (Kilovoltage peak): Controls photon quality (energy/penetrability).
- mAs (Milliampere-seconds): Controls photon quantity (number/exposure).
⭐ The Anode Heel Effect causes higher X-ray intensity on the cathode side. Position the thicker body part under the cathode for uniform image density.
Radiodensity - The 5 Shades of Grey
Describes how tissues absorb X-ray radiation, creating a spectrum from black (radiolucent) to white (radiopaque). This is determined by the atomic number and physical density of the tissue.
- Air: Black (most radiolucent)
- Found in lungs, bowel gas.
- Fat: Dark grey
- Seen in subcutaneous layers, around organs.
- Water / Soft Tissue: Light grey
- Includes muscle, blood, and solid organs.
- Bone / Calcium: Off-white
- Represents bones, calcified stones.
- Metal / Contrast: Bright white (most radiopaque)
- Surgical hardware, barium.
📌 Mnemonic (Black → White): Air Fat Water Bone Metal.
⭐ Pathologies are often visible due to displaced radiodensities. Air appearing in the peritoneum (pneumoperitoneum) is a classic sign of bowel perforation.
Interpretation Principles - An Analyst's ABCs
📌 ABCDE systematic approach prevents missed findings.
- A: Airway & Adequacy
- Trachea midline? Carina angle.
- RIPE: Rotation, Inspiration (≥8 posterior ribs), Projection (PA vs. AP), Exposure.
- B: Bones & Soft Tissues
- Scan ribs, clavicles, vertebrae for fractures, lytic/blastic lesions.
- C: Cardiac & Mediastinum
- Cardiac silhouette size, aortic knob.
⭐ A cardiothoracic ratio > 0.5 on a PA chest X-ray suggests cardiomegaly.
- D: Diaphragm
- Sharp costophrenic angles. Right hemidiaphragm slightly elevated over left.
- E: Everything Else (Lungs/Lines)
- Lung fields for infiltrates, effusions, pneumothorax. Check for tubes/lines.
Views & Projections - What's Your Angle?
- PA (Posteroanterior): Standard CXR. Beam travels back-to-front, minimizing heart magnification.
- AP (Anteroposterior): Portable/ICU setting. Beam travels front-to-back, magnifying the heart.
- Lateral: Side view, crucial for localizing opacities seen on frontal views.
- Lateral Decubitus: Patient lying on their side; detects small pleural effusions.
- Oblique: Rotated view, useful for ribs and specific joints.
⭐ A normal cardiothoracic ratio (< 0.5) is only valid on an inspiratory PA film. AP films artificially enlarge the cardiac silhouette.
- X-rays utilize five basic radiodensities: Air (blackest), Fat, Water (soft tissue), Bone, and Metal (whitest).
- Radiolucent structures (e.g., air-filled lungs) appear dark, while radiopaque structures (e.g., bone) appear white.
- Always obtain at least two orthogonal views (e.g., PA and lateral) to properly localize a finding in 3D space.
- The PA view is preferred for chest imaging as it minimizes cardiac magnification.
- A systematic approach (e.g., ABCDEs) is crucial for interpretation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

