Ultrasound Physics & Probes - Wave Wrangling
- Piezoelectric Effect: Transducer crystals convert electrical energy to mechanical sound waves & vice versa.
- Acoustic Impedance (Z): Resistance to sound travel. $Z = \text{density} (\rho) \times \text{propagation speed} (c)$. Echoes are generated at interfaces of tissues with different Z values.
- Frequency vs. Penetration Trade-off:
- High frequency (>7 MHz): ↑ resolution, ↓ penetration (superficial structures).
- Low frequency (2-5 MHz): ↓ resolution, ↑ penetration (deep structures).
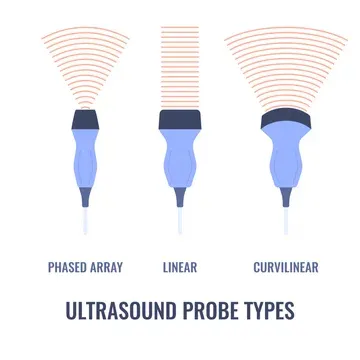
- Probe Selection:
- Linear: High frequency; vascular, thyroid.
- Curvilinear (Convex): Low frequency; abdomen, OB/GYN.
- Phased Array: Low frequency, small footprint; cardiac.
- 📌 Linear for Lumps (superficial), Curvilinear for Core (deep).
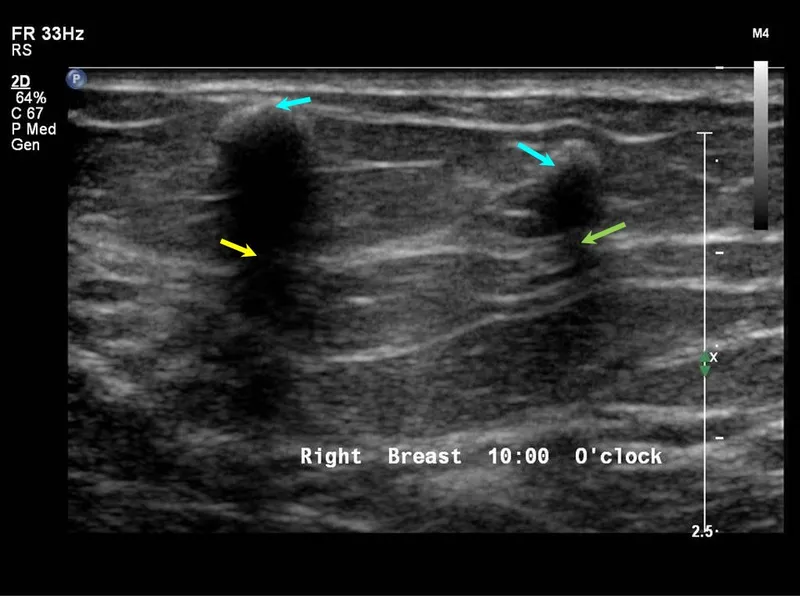
⭐ The brightness of an echo (echogenicity) is determined by the difference in acoustic impedance between two tissues. Large differences (e.g., soft tissue-bone) create bright, hyperechoic interfaces.
Echogenicity & Terminology - Reading the Shadows
-
Echogenicity: Tissue's ability to reflect ultrasound waves. Brightness on screen.
- Hyperechoic: White/bright (e.g., bone, stones). High reflection.
- Hypoechoic: Dark gray (e.g., solid organs, muscle). Low reflection.
- Anechoic: Pure black (e.g., simple fluid, cysts). No reflection.
- Isoechoic: Same brightness as surrounding tissue.
-
Key Artifacts:
- Acoustic Shadowing: Dark area behind a bright, dense object (e.g., gallstone) that blocks sound waves.
- Posterior Acoustic Enhancement: Bright area behind a fluid-filled structure (e.g., cyst) as sound travels with less resistance.
⭐ In a FAST exam, anechoic (black) fluid collections in potential spaces like Morison's pouch are a critical finding suggestive of hemoperitoneum.
Doppler & M-Mode - Going with the Flow
- Doppler Effect: Measures frequency shift of returning echoes to assess blood flow velocity and direction.
- Doppler Equation: $Δf = (2 f₀ v \cos θ) / c$
- 📌 BART: Blue Away, Red Toward the transducer.
- Doppler Types:
- Color: Average velocity & direction. Risk of aliasing.
- Power: ↑ sensitivity for low flow (e.g., testicular torsion), no direction info.
- Pulsed-Wave (PW): Site-specific velocity. Aliasing at high velocity.
- Continuous-Wave (CW): High velocity, no aliasing. Lacks depth specificity.
- M-Mode (Motion Mode):
- Single beam plotted against time. High temporal resolution.
- Uses: Valve motion, wall thickness, fetal heart rate.
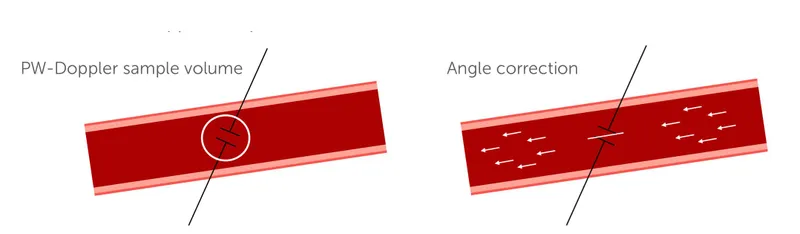
⭐ For accurate flow velocity, the Doppler angle (θ) should be < 60°. As θ approaches 90°, cosine θ approaches 0, and the detected velocity is falsely low or absent.
Key Artifacts - Glitches in the Matrix
- Artifacts are errors in imaging that do not correspond to actual anatomy. Understanding them is key to correct interpretation.
| Artifact | Appearance | Cause & Clinical Pearl |
|---|---|---|
| Acoustic Shadowing | Signal void deep to a highly attenuating structure (e.g., bone, gallstone). | Clean (sharp) shadows suggest calcification. Dirty (fuzzy) shadows suggest gas. |
| Acoustic Enhancement | Increased signal intensity deep to a weakly attenuating structure (e.g., cyst). | 💡 Classic sign of a simple fluid-filled cyst (e.g., in breast, ovary, kidney). |
| Reverberation | Multiple, equally spaced linear echoes. | Caused by sound bouncing between two highly reflective surfaces. Comet tail is a subtype. |
| Mirror Image | A structure appears on both sides of a strong reflector (e.g., diaphragm). | Common to see the liver mirrored in the thorax above the diaphragm. |
⭐ Acoustic enhancement (posterior enhancement) is a crucial feature used to characterize fluid-filled structures like simple cysts, distinguishing them from solid masses which typically cause shadowing or have no effect.
- Ultrasound uses sound waves; tissue echogenicity depends on acoustic impedance.
- Hyperechoic (bright) structures like bone reflect many waves; anechoic (dark) structures like cysts reflect none.
- Use high-frequency probes for superficial structures (better resolution) and low-frequency for deep structures (better penetration).
- Posterior acoustic enhancement occurs deep to fluid; acoustic shadowing occurs deep to solids like gallstones.
- Doppler assesses blood flow: Blue is away from the probe, Red is towards it (BART).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

