Fundamentals - Radioactive Reporters
- Radiotracer: A radioisotope (e.g., Tc-99m) attached to a pharmaceutical that targets specific tissues or physiological processes.
- Key Emissions:
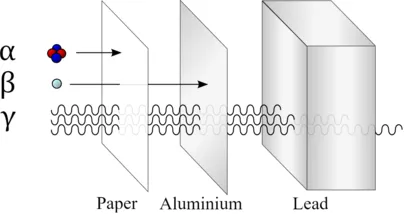
- Alpha ($α$, $^4_2$He nucleus): High energy, but very low tissue penetration. Not used for diagnostic imaging.
- Beta ($β$, electron/positron): Moderate penetration. Positron ($β^+$) emission is the basis for PET imaging.
- Gamma ($γ$, photon): High penetration, easily exits the body. Ideal for external imaging with a gamma camera (SPECT).
- 📌 Gamma Gives Good imaging.
⭐ Technetium-99m (Tc-99m) is the most common radioisotope for SPECT imaging due to its ideal 140 keV gamma emission and 6-hour half-life.
SPECT vs. PET - Functional Fireworks
| Feature | SPECT (Single-Photon Emission CT) | PET (Positron Emission Tomography) |
|---|---|---|
| Principle | Detects single gamma rays from a radiotracer. | Detects two gamma rays from positron-electron annihilation. |
| Tracers | Gamma emitters (e.g., Technetium-99m, $^{99m}$Tc). | Positron emitters (e.g., $^{18}$F-FDG). |
| Resolution | Lower spatial resolution. | Higher spatial resolution & sensitivity. |
| Cost | Less expensive, more available. | More expensive, less available. |
| Uses | * Bone scans (metastases) * Myocardial perfusion * Brain (seizure foci) | * Oncology (staging, monitoring) * Myocardial viability * Neurology (dementia) |
⭐ PET/CT with $^{18}$F-FDG is a cornerstone of oncology imaging. Malignant cells exhibit high glucose metabolism (Warburg effect), leading to intense FDG uptake, which helps differentiate tumors from benign lesions and locate metastases.
High-Yield Applications - A Scan for All Seasons
-
Cardiology (Myocardial Perfusion): SPECT with Thallium-201 or $Tc^{99m}$-sestamibi to detect ischemia/infarction. Compares rest vs. stress (exercise/pharmacologic) images.
-
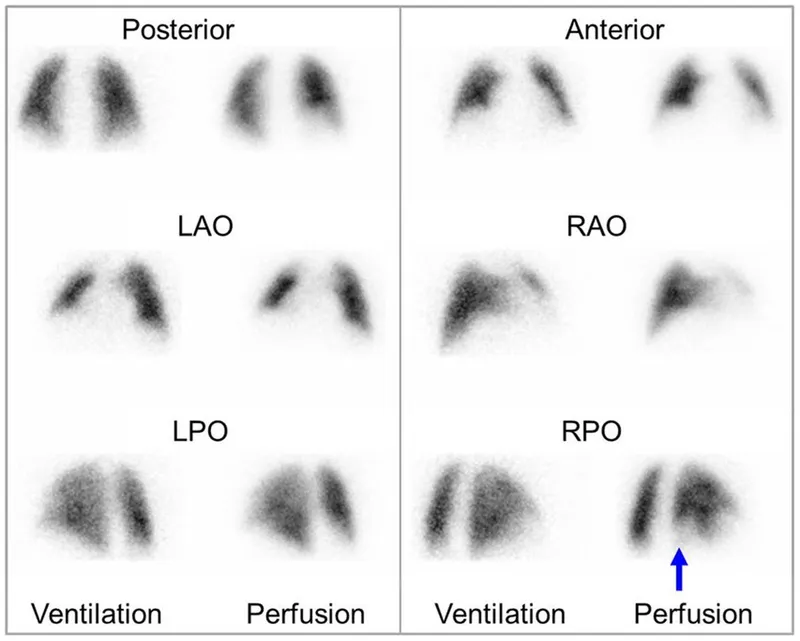
Pulmonology (V/Q Scan): For pulmonary embolism diagnosis, especially when CT angiography is contraindicated (e.g., renal failure, pregnancy). Uses $Xe^{133}$ for ventilation & $Tc^{99m}$-MAA for perfusion.
-
Endocrinology:
- Thyroid Scan: $I^{123}$ uptake assesses function. "Hot" nodules are hyperfunctioning (usually benign); "cold" nodules have ↓uptake (higher cancer risk).
- Parathyroid Scan: $Tc^{99m}$-Sestamibi localizes hyperfunctioning adenomas.
-
Gastrointestinal:
- HIDA Scan: $Tc^{99m}$-iminodiacetic acid analogs. Non-visualization of the gallbladder suggests cholecystitis.
- GI Bleed Scan: $Tc^{99m}$-labeled RBCs detect active extravasation.
-
Oncology/MSK:
- Bone Scan: $Tc^{99m}$-MDP (methylene diphosphonate) for metastatic disease, fractures, osteomyelitis. 📌 MDP = "Marrow/Disease Pointer".
- PET Scan: $F^{18}$-FDG shows metabolic activity. Used for cancer staging and monitoring treatment response.
⭐ A V/Q scan showing a "mismatched defect" (perfusion defect without a corresponding ventilation defect) is highly specific for a pulmonary embolism.
Radiation Safety - Handle With Care
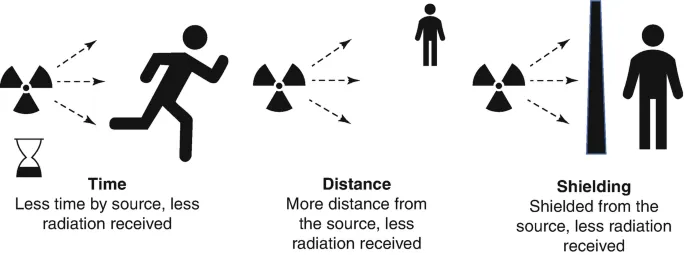
- ALARA Principle: As Low As Reasonably Achievable. Minimize radiation dose by optimizing:
- Time: ↓ exposure time.
- Distance: ↑ distance from the source.
- Shielding: Use lead aprons & barriers.
- Contraindications: Pregnancy is an absolute contraindication. Breastfeeding is a relative one (requires temporary cessation).
- Post-Scan Advice: Hydrate to accelerate radiotracer excretion. Limit close contact with children & pregnant women.
⭐ A patient's radiation dose from a typical nuclear scan (e.g., bone scan) is comparable to a few years of natural background radiation.
High‑Yield Points - ⚡ Biggest Takeaways
- PET scans use FDG to find metabolically active tissues like tumors or inflammation.
- HIDA scans diagnose acute cholecystitis when the gallbladder is not visualized.
- V/Q scans identify pulmonary embolism through a ventilation-perfusion mismatch.
- Bone scans are highly sensitive for bony metastases, fractures, and osteomyelitis.
- On a thyroid scan, "cold" nodules have a higher malignancy risk than "hot" nodules.
- Gallium scans help localize inflammation and tumors like lymphoma and sarcoidosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

