Layers of the Skin - The Body's Armor
-
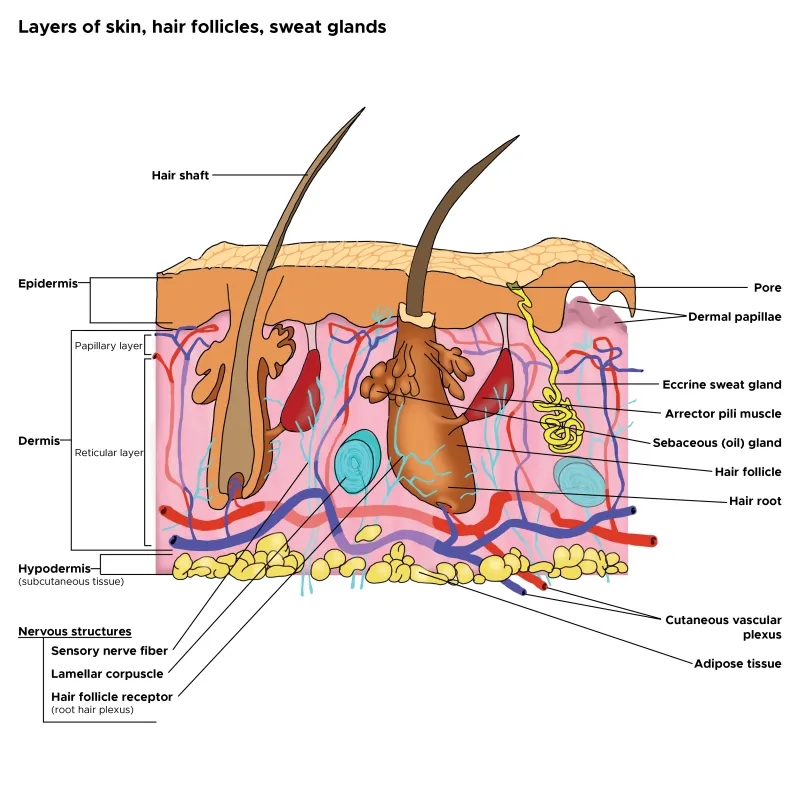
Epidermis: Avascular, keratinized stratified squamous epithelium. Layers from superficial to deep:
- S. Corneum: Anucleated cells, keratin.
- S. Lucidum: Clear layer; only in thick skin (palms/soles).
- S. Granulosum: Keratohyalin granules.
- S. Spinosum: Desmosomes (intercellular bridges).
- S. Basale: Mitotically active stem cells, melanocytes.
- 📌 Mnemonic: Come, Let's Get Sun Burned.
-
Dermis: Supports epidermis; contains blood vessels, nerves, and appendages.
- Papillary Layer: Loose connective tissue.
- Reticular Layer: Dense, irregular connective tissue.
⭐ Langerhans cells (dendritic, antigen-presenting immune cells) are most prominent in the Stratum Spinosum.
Cells of the Epidermis - The Skin's Crew
- Keratinocytes (~90%): The workhorses. Originate in the basal layer, mature upwards. Produce keratin for strength and form the waterproof barrier.
- Melanocytes (~5%): Located in the stratum basale. Synthesize melanin pigment from tyrosine, protecting against UV radiation. Derived from the neural crest.
- Langerhans Cells (2-3%): Dendritic cells in the stratum spinosum. Act as antigen-presenting cells (APCs). 📌 Birbeck granules (tennis-racket shape) are characteristic.
- Merkel Cells (~1%): Found in the stratum basale. Slow-adapting mechanoreceptors for light touch.
⭐ Albinism results from a normal number of melanocytes but a lack of tyrosinase, the key enzyme for melanin production.

Skin Appendages - Hairy, Sweaty, Oily Bits
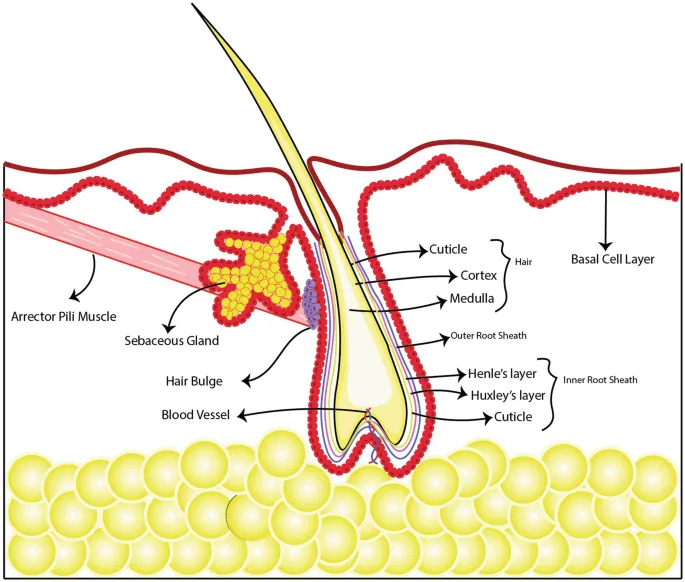
- Hair Follicles
- Anchors hair shaft; associated with arrector pili muscles (piloerection).
- Cycles: Anagen (growth), Catagen (involution), Telogen (rest).
- Sebaceous Glands
- Produce oily/waxy sebum; lubricates skin & hair.
- Holocrine secretion: whole cell disintegrates.
- Outflow is typically into a hair follicle.
- Sweat (Sudoriferous) Glands
- Eccrine: Everywhere; for thermoregulation. Secretes watery sweat via merocrine secretion.
- Apocrine: Axillae, genitals. Active at puberty. Viscous, odorless fluid that bacteria make odorous.
⭐ High-Yield: Despite the name, apocrine sweat glands also use merocrine secretion (exocytosis), not apocrine secretion (decapitation). This is a common exam trap!
Dermatomes & Innervation - The Nerve Map
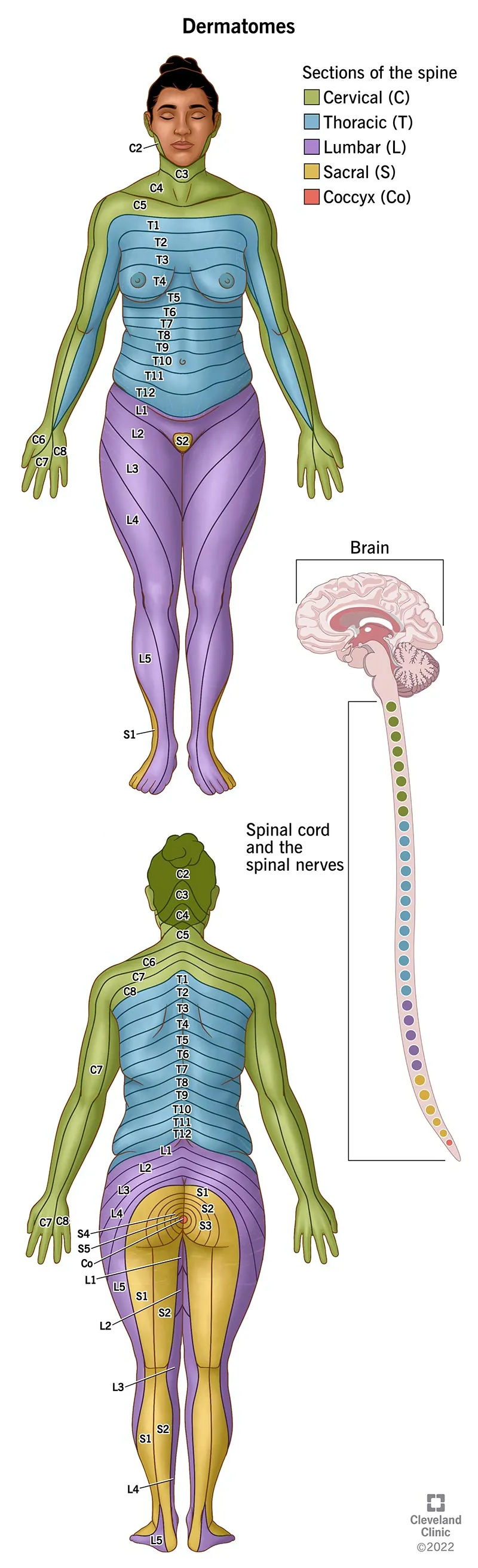
- A dermatome is an area of skin supplied by sensory fibers from a single spinal nerve (dorsal root).
- Key anatomical landmarks for testing:
- C4: High collar shirt (clavicles/upper shoulders)
- T4: Nipple line (teat pore)
- T10: Umbilicus (belly but-ten)
- L4: Kneecaps (down on all L4s)
- S2-S4: Perineal sensation
⭐ Herpes zoster (shingles) infection causes a painful, unilateral vesicular rash that is limited to a single dermatome and does not cross the midline.
Burns & Healing - Trial by Fire
-
Classification (Depth):
- 1st: Epidermis only (e.g., sunburn); erythema, painful.
- 2nd: Epidermis + Dermis; blistering, very painful.
- 3rd: Full-thickness; white/leathery, painless.
- 4th: Extends to fascia, muscle, or bone.
-
Severity: Total Body Surface Area (TBSA) via "Rule of Nines."
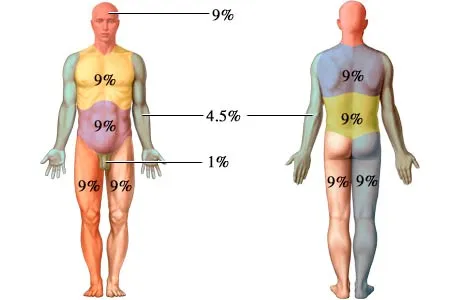
-
Healing Phases:
⭐ Curling's Ulcer: Acute gastric stress ulcer in proximal duodenum post-severe burn. Caused by ↓ plasma volume → ischemia of gastric mucosa.
High‑Yield Points - ⚡ Biggest Takeaways
- The epidermis is avascular and its layers can be recalled with the mnemonic: Come, Let's Get Sun Burned.
- Neural crest cells are the origin for both melanocytes (in the stratum basale) and Merkel cells (sensory receptors).
- Langerhans cells, found in the stratum spinosum, are bone marrow-derived antigen-presenting cells.
- Pemphigus vulgaris (anti-desmosome) vs. Bullous pemphigoid (anti-hemidesmosome) are key autoimmune blistering diseases.
- Third-degree burns are painless because they destroy nerve endings.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

