Cervical Fascia Layers - Neck's Nifty Napkins
-
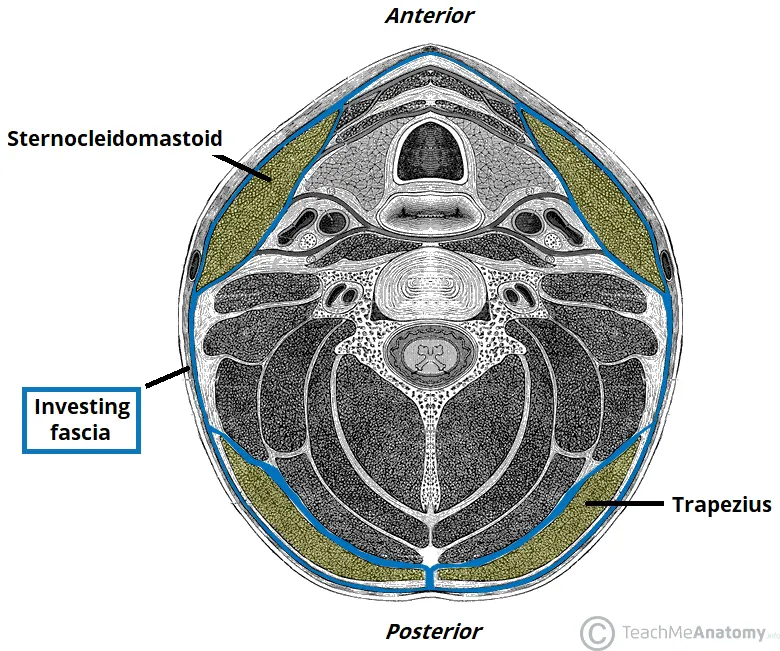
Superficial Cervical Fascia:
- Contains platysma muscle, cutaneous nerves, blood vessels, and lymphatics.
-
Deep Cervical Fascia (3 Layers):
- Investing Layer: Surrounds the entire neck; splits to enclose sternocleidomastoid and trapezius muscles.
- Pretracheal Layer: Encloses thyroid gland, trachea, and esophagus.
- Prevertebral Layer: Surrounds the vertebral column and associated muscles.
-
Carotid Sheath:
- A unique fascial column receiving contributions from all three deep layers.
- Contents: Common/Internal Carotid Artery, Internal Jugular Vein, Vagus Nerve (CN X).
⭐ Infections in the "danger space" (retropharyngeal space) can readily spread inferiorly into the posterior mediastinum.
Key Fascial Spaces - Corridors of Concern
-
Retropharyngeal Space
- Location: Between buccopharyngeal fascia (anteriorly) and alar fascia (posteriorly).
- Clinical Significance: Pathway for infection from pharynx/esophagus to spread inferiorly into the superior mediastinum.
-
"Danger Space" (Alar Space)
- Location: Between alar fascia (anteriorly) and prevertebral fascia (posteriorly).
- Clinical Significance: Most dangerous route for infection spread.
⭐ Infections in the "danger space" can travel from the base of the skull directly to the diaphragm and posterior mediastinum, leading to severe complications like acute mediastinitis.
-
Prevertebral Space
- Location: Posterior to the danger space, anterior to vertebral bodies.
- Clinical Significance: Infection can erode into vertebral bodies, causing osteomyelitis.
-
Submandibular & Masticator Spaces
- Source: Most commonly from dental infections (e.g., abscessed mandibular molar).
- 💡 Ludwig's Angina: Rapidly spreading cellulitis of the submandibular space, potentially causing fatal airway compromise from tongue elevation and glottic edema.
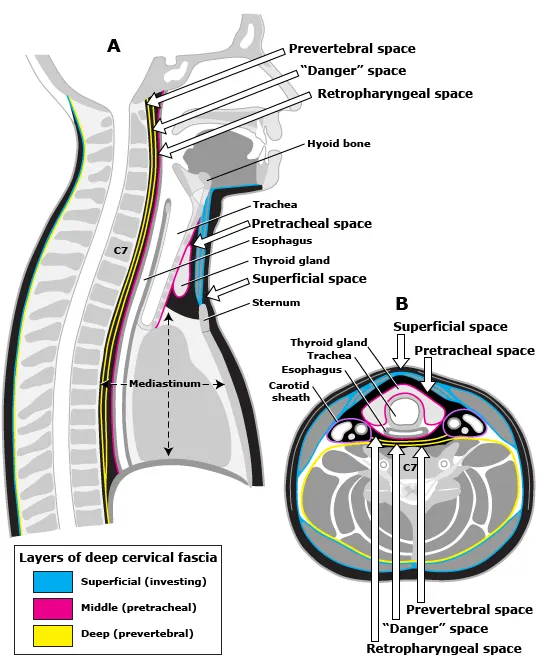
Infection Spread - Pathways to Peril
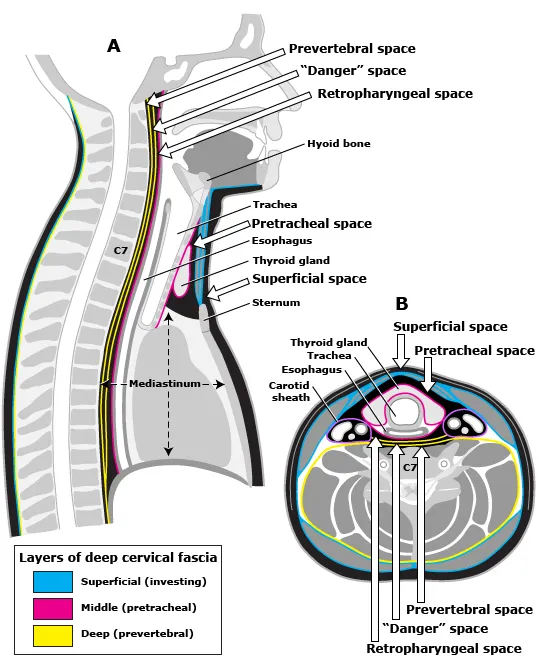
- Odontogenic, pharyngeal, or tonsillar infections can erode through fascial layers, spreading rapidly along paths of least resistance.
- Retropharyngeal Space: Between buccopharyngeal & alar fascia. Drains into the superior mediastinum.
- "Danger Space": Between alar & prevertebral fascia. This space provides a direct, rapid conduit from the skull base to the diaphragm.
- Ludwig's Angina: Aggressive, bilateral cellulitis of the submandibular space; can cause fatal airway obstruction.
⭐ Infections in the "danger space" are the most feared, as they can descend directly into the posterior mediastinum, leading to necrotizing mediastinitis with a mortality rate approaching 50%.
High-Yield Points - ⚡ Biggest Takeaways
- The danger space, between the alar and prevertebral fascia, is the most critical route for infection spread to the posterior mediastinum.
- Infections in the retropharyngeal space can travel down to the superior mediastinum.
- Ludwig's angina is a rapidly spreading cellulitis of the submandibular space that can cause acute airway obstruction.
- The pretracheal space offers a direct path for infection to the anterior mediastinum.
- Cavernous sinus thrombosis can arise from infections in the danger triangle of the face.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

