Dermatomes - The Body's Wiring
A dermatome is an area of skin supplied by sensory fibers from a single spinal nerve root. Testing key dermatomes with light touch or pinprick helps localize neurologic lesions.
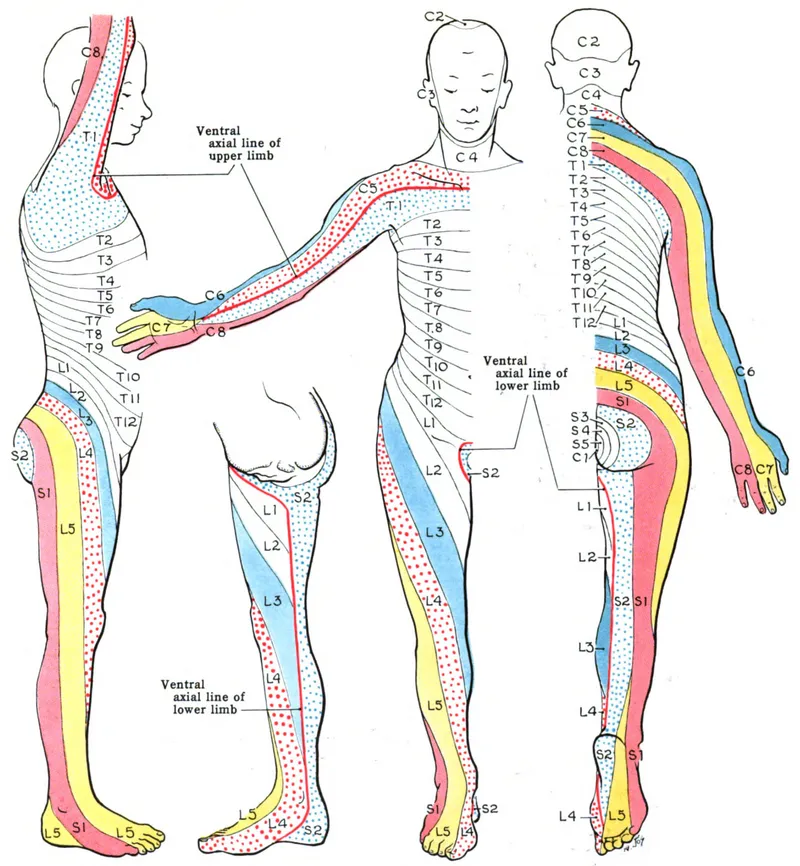
- C5: Lateral shoulder/arm (deltoid badge area)
- C6: Lateral forearm, thumb, and index finger
- C7: Middle finger
- C8: Medial forearm, ring and little finger
- T4: Nipple line (📌 T4 at the T-pore)
- T10: Umbilicus (📌 T10 at the belly but-ten)
- L4: Medial leg and medial malleolus
- L5: Dorsum of the foot and great toe
- S1: Lateral malleolus and little toe
⭐ The C1 nerve root has no sensory component, so there is no C1 dermatome.
Key Landmarks - A Dermatome Tour

- C2/C3: Posterior head and neck.
- C4: Shoulder area, clavicle.
- C6: Thumb (radial side of forearm).
- C7: Middle finger.
- C8: Little finger (ulnar side of forearm).
- T4: Nipple line.
- 📌 Mnemonic: T4 at the teet-pore (nipple).
- T10: Umbilicus.
- 📌 Mnemonic: T10 at the belly but-ten (belly button).
- L1: Inguinal ligament.
- L4: Medial malleolus (knee and medial leg).
- L5: Dorsum of the foot, big toe.
- S1: Lateral malleolus, little toe.
- S2-S4: Perianal region (saddle anesthesia).
⭐ Exam Favorite: The three middle fingers often have overlapping innervation. C6 classically supplies the thumb/index, C7 the middle finger, and C8 the ring/little finger, but variations are common. Remember the "6-shooter" gesture: thumb and index finger make a "gun" shape, innervated by C6.
Sensory Testing - The How-To Guide
- Patient: Eyes closed to prevent visual feedback. Explain the procedure clearly.
- Baseline: First, test on an area with normal sensation (e.g., the face) to establish a baseline for the patient.
- Procedure: Test key sensory points bilaterally, comparing sides. Move from impaired to normal areas.
- Stimuli: Use a cotton wisp (light touch) and a neurotip (pinprick). Apply stimulus for 1-2 seconds. Test in an unpredictable pattern to avoid patient anticipation.
⭐ For C6, the most reliable sensory testing point is the pulp of the thumb. This is a frequent exam question focus for differentiating cervical nerve root compression.
High‑Yield Points - ⚡ Biggest Takeaways
- C5 covers the lateral shoulder (deltoid badge area).
- C6 supplies the thumb; C7 the middle finger; C8 the little finger.
- T4 is at the nipple line; T10 is at the umbilicus.
- L4 covers the medial malleolus; L5 the dorsum of the foot.
- S1 is tested at the lateral malleolus and heel.
- Always test both spinothalamic (pinprick) and DCML (light touch) tracts.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

