Sacral Plexus - Nerve Root Rundown
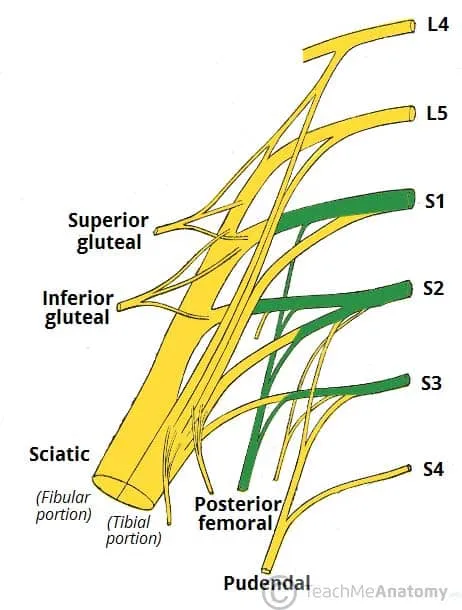
- Roots: Formed from the anterior rami of spinal nerves L4-S4.
- Key Nerves & Roots:
- Superior Gluteal (L4-S1): Innervates gluteus medius, minimus.
- Inferior Gluteal (L5-S2): Innervates gluteus maximus.
- Sciatic (L4-S3): Composed of tibial and common peroneal divisions.
- Pudendal (S2-S4): Innervates perineum. 📌 Superior gluteal, Inferior gluteal, Sciatic, Pudendal.
⭐ The common peroneal nerve is the most frequently injured nerve in the lower limb, often due to its superficial position at the fibular neck, leading to foot drop.
Sacral Dermatomes - The Sensation Map

- S1: Lateral aspect of the foot, heel, and sole.
- S2: Posterior thigh and calf.
- S3: Medial aspect of the thigh and perineum.
- S4-S5: Perianal region, forming concentric rings.
⭐ Saddle Anesthesia: Numbness in the S2-S5 distribution (buttocks, perineum, inner thighs) is a classic sign of Cauda Equina Syndrome, a surgical emergency.
📌 Mnemonic: Think "S is for Saddle" - the S2-S5 dermatomes cover the area that contacts a horse saddle.
Sacral Myotomes - Motorway to Movement
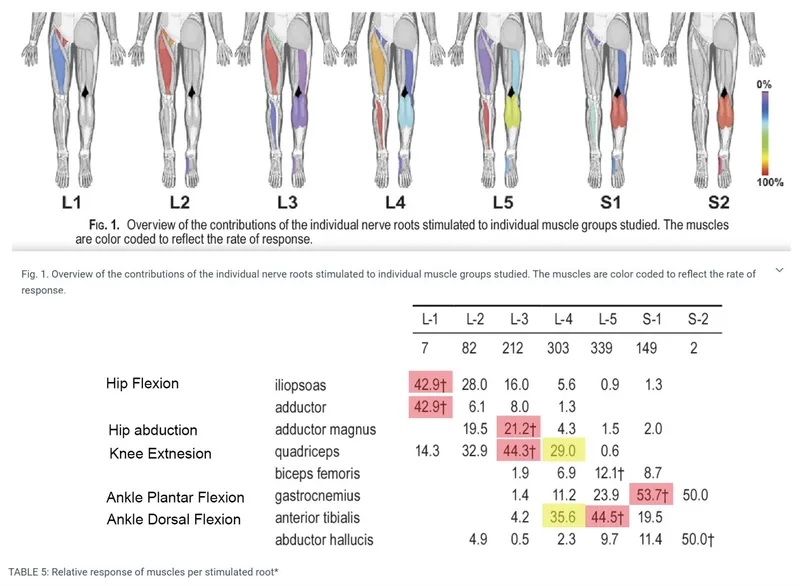
- S1: Primarily drives ankle plantarflexion (e.g., standing on tiptoes). Also involved in foot eversion and hip extension.
- Key muscles: Gastrocnemius, soleus.
- S2: Governs toe flexion and contributes to ankle plantarflexion.
- S3-S4: Innervate intrinsic foot muscles and, critically, the external urethral and anal sphincters for urinary and fecal continence.
- The "anal wink" reflex tests the integrity of S3-S4.
- 📌 Mnemonic: "S2, S3, S4 keeps the pee and poop off the floor."
⭐ The Achilles tendon reflex (ankle jerk) is the classic clinical test for the integrity of the S1 nerve root.
Clinical Correlations - Sacral Nerve Syndromes
-
Cauda Equina Syndrome (CES): Medical emergency from compression of lumbar, sacral, and coccygeal nerve roots.
- Etiology: Disc herniation (most common), tumor, trauma, abscess.
- Presentation: Asymmetric, radicular pain; saddle anesthesia (S2-S5); bowel/bladder dysfunction (late finding); LMN signs only (hyporeflexia, flaccid paralysis).
-
Conus Medullaris Syndrome: Injury to the terminal spinal cord (L1-L2).
- Presentation: Sudden, symmetric symptoms; less severe radicular pain; early bowel/bladder dysfunction; mixed UMN & LMN signs.
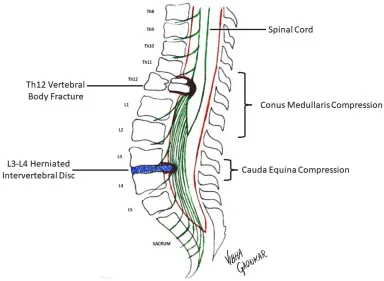
⭐ Exam Favorite: Conus Medullaris syndrome often presents with a combination of upper motor neuron (hyperreflexia) and lower motor neuron (fasciculations) signs, as it involves both the spinal cord and nerve roots.
High‑Yield Points - ⚡ Biggest Takeaways\n\n> * S1 radiculopathy classically presents with a lost Achilles reflex and weakness in plantarflexion.\n> * S2-S4 roots control bowel, bladder, and erectile function (parasympathetic).\n> * Saddle anesthesia (perineal numbness) is the key sign of S3-S5 involvement.\n> * Cauda Equina Syndrome is a surgical emergency: look for saddle anesthesia, urinary retention, and fecal incontinence.\n> * The anal wink reflex (S3-S5) is a vital physical exam test for sacral nerve integrity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

