Key Thoracic Levels - A Bird's-Eye View
- T2: Suprasternal notch
- T4: Sternal angle (of Louis) - Aortic arch, Tracheal bifurcation
- T8: Inferior Vena Cava (IVC) hiatus
- T9: Xiphoid process
- T10: Esophageal hiatus
- T12: Aortic hiatus
⭐ The Sternal Angle at T4 is a critical landmark, marking the carina and the division between superior and inferior mediastinum.
📌 Mnemonic (Diaphragmatic Apertures): I ate ten eggs at twelve (IVC at T8, Esophagus at T10, Aorta at T12).
Superior Mediastinum - Great Vessel Gala
- Location: Superior to the transverse thoracic plane (sternal angle at T4/T5 disc) and inferior to the thoracic inlet.
- Vascular Layers (Anterior → Posterior):
- Veins: Superior Vena Cava (SVC), Left & Right Brachiocephalic veins.
- Arteries: Aortic Arch and its three great branches (Brachiocephalic trunk, L. Common Carotid a., L. Subclavian a.).
- Other Key Contents:
- Thymus, Trachea, Esophagus.
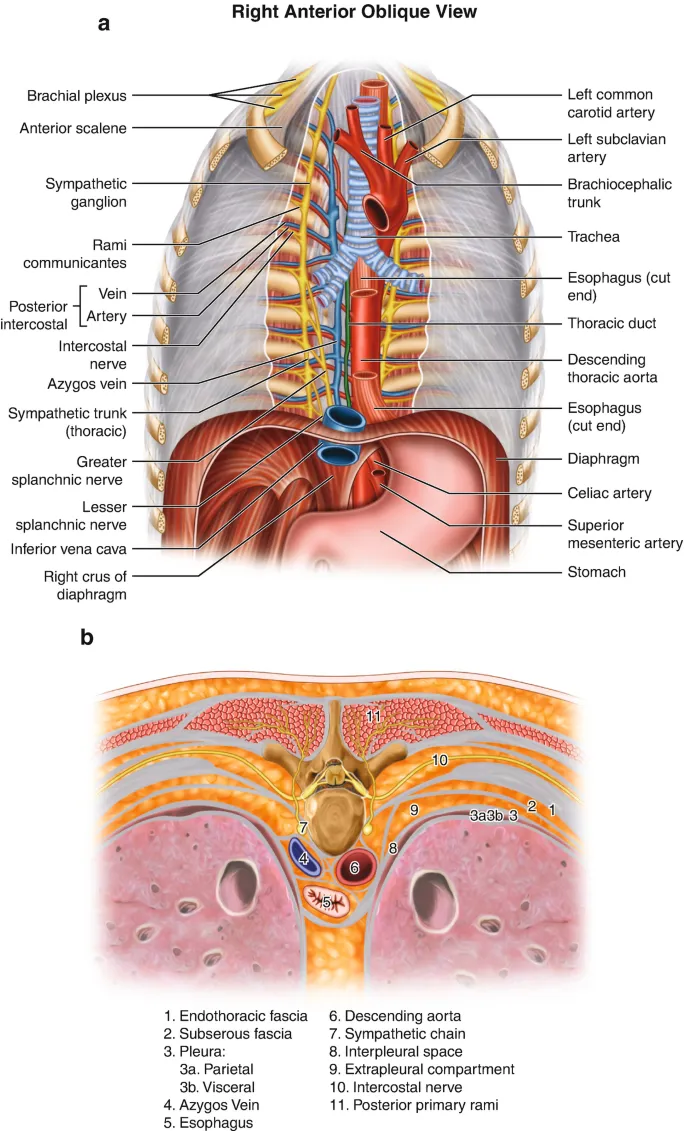
- Nerves (Vagus, Phrenic) & Thoracic Duct.
⭐ The left recurrent laryngeal nerve hooks under the aortic arch here, making it vulnerable during thoracic surgery (e.g., PDA ligation), causing hoarseness if damaged.
The Sternal Angle - Highway T4/T5
- Location: Articulation of manubrium & sternal body; marks the T4/T5 intervertebral disc.
- A critical plane where multiple structures begin, end, or cross.
- 📌 Mnemonic: RAT PLAT
- Rib 2 articulation
- Aortic Arch begins & ends
- Tracheal bifurcation (Carina)
- Pulmonary trunk bifurcation
- Ligamentum arteriosum
- Azygos vein drains into SVC
- Thoracic duct crosses
⭐ The thoracic duct crosses from right to left at this level, a key landmark for identifying it during surgical procedures. It is the largest lymphatic vessel in the body.
Cardiac & Hilar Views - Heart of the Matter
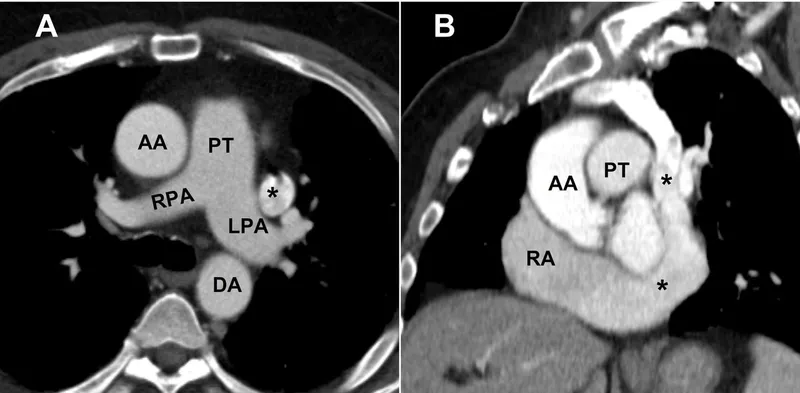
- Level T5-T8: Visualizes all four cardiac chambers, pericardium, and great vessels (ascending/descending aorta, pulmonary trunk).
- Key Structures:
- Heart: Right ventricle (most anterior), left atrium (most posterior).
- Hilum: Pulmonary arteries, veins, and main bronchi bundle together.
- 📌 RALS: Right pulmonary Artery is Anterior to bronchus; Left is Superior.
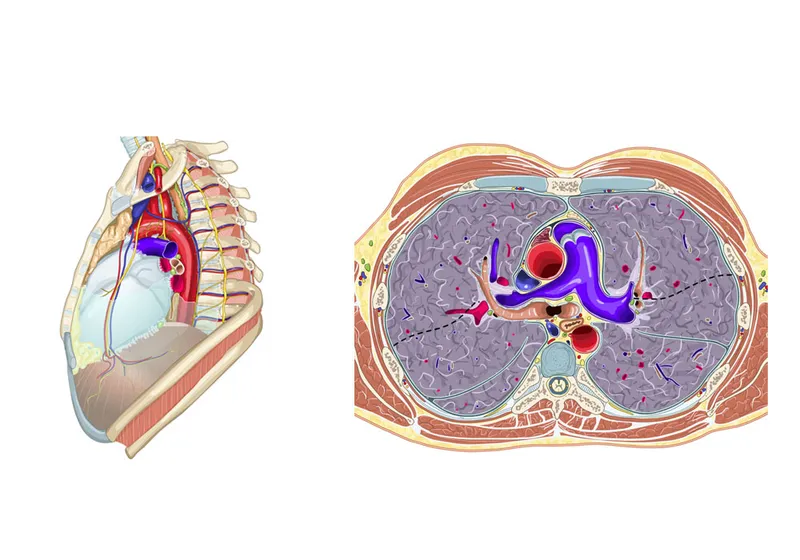
⭐ The transverse pericardial sinus, located posterior to the aorta and pulmonary trunk, is a critical landmark for surgeons to clamp the great vessels during cardiac surgery.
Diaphragmatic Hiatuses - The Great Escape
- Structures passing through the diaphragm at key vertebral levels.
- 📌 Mnemonic: I 8 10 Eggs At 12
- T8 (Caval Opening): Inferior Vena Cava (IVC), Right Phrenic nerve branches.
- T10 (Esophageal Hiatus): Esophagus, Vagus nerve (CN X).
- T12 (Aortic Hiatus): Aorta, Thoracic duct, Azygos vein.
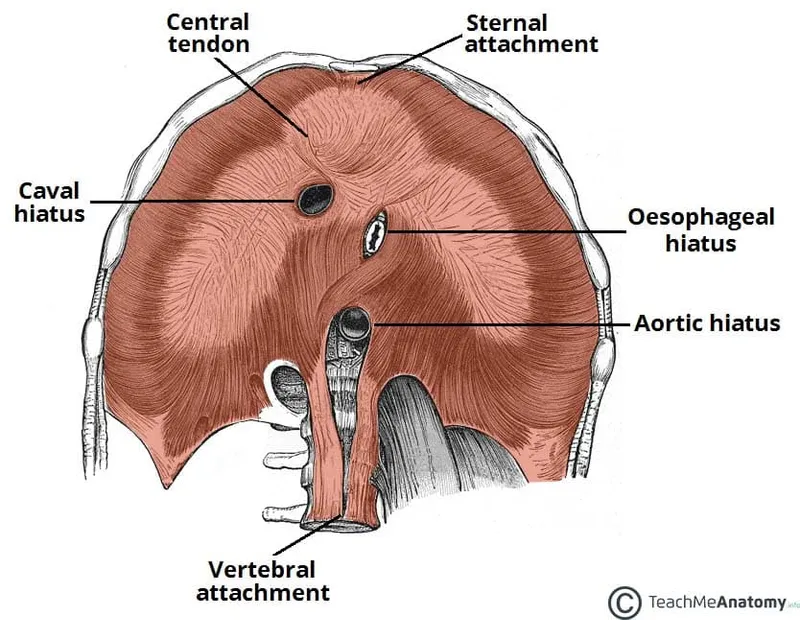
⭐ The esophageal hiatus is a common site for hiatal hernias, where abdominal contents (like the stomach) protrude into the thorax, potentially causing GERD.
- The sternal angle (T4/T5) is a critical landmark where the aortic arch begins/ends and the trachea bifurcates.
- The pulmonary trunk also divides, and the azygos vein arches over the right lung root to enter the SVC.
- The thoracic duct crosses from right to left at approximately the T5 vertebral level.
- Remember the relationship of the pulmonary artery to the main bronchus with the mnemonic RALS (Right Anterior, Left Superior).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

