Safe Prescribing

On this page
Recognising High-Risk Medicines in Clinical Practice
A 78-year-old woman with atrial fibrillation arrives at the GP surgery requesting a repeat prescription for warfarin. Her INR last week was 2.3, but she mentions she's started taking "something herbal" for joint pain. This scenario encapsulates the vigilance required when prescribing - medications where small errors in selection, dosing, or monitoring can result in catastrophic patient harm. The Institute for Safe Medication Practices identifies several drug classes requiring enhanced scrutiny, with anticoagulants and insulin consistently topping lists of medications causing preventable deaths. Understanding which medicines demand heightened attention forms the foundation of safe prescribing practice.
High-risk medicine categories requiring systematic safeguards:
-
Anticoagulants - warfarin, DOACs, heparins
- Account for 25% of medication-related hospital admissions in UK
- Therapeutic index narrower than most clinicians appreciate
- protocols reduce major bleeding by 40-60%
-
Insulin and hypoglycaemic agents
- Contribute to 10-15% of serious medication incidents
- Errors often involve dose, timing, or insulin type confusion
- Severe hypoglycaemia (glucose <3.0 mmol/L) can cause permanent neurological damage
-
Opioids and sedatives
- Respiratory depression risk increases exponentially with dose
- Morphine equivalence calculations frequently miscalculated
-
Chemotherapy and immunosuppressants
- Methotrexate weekly dosing errors remain common despite decades of warnings
- Mercaptopurine/azathioprine interactions with allopurinol can be fatal
📌 Mnemonic - PINCH: Potassium (and other electrolytes), Insulin, Narcotics, Chemotherapy, Heparin/anticoagulants
| High-Risk Category | Annual UK Incidents | Most Common Error Type | Mortality Risk |
|---|---|---|---|
| Anticoagulants | ~12,000 serious events | Dose/monitoring failure | 5-8% major bleeds |
| Insulin | ~8,000 serious events | Wrong insulin type/dose | 2-3% severe hypo |
| Opioids | ~6,000 serious events | Dose calculation error | 1-2% respiratory arrest |
| Methotrexate | ~2,000 serious events | Daily instead of weekly | 10-15% if uncorrected |
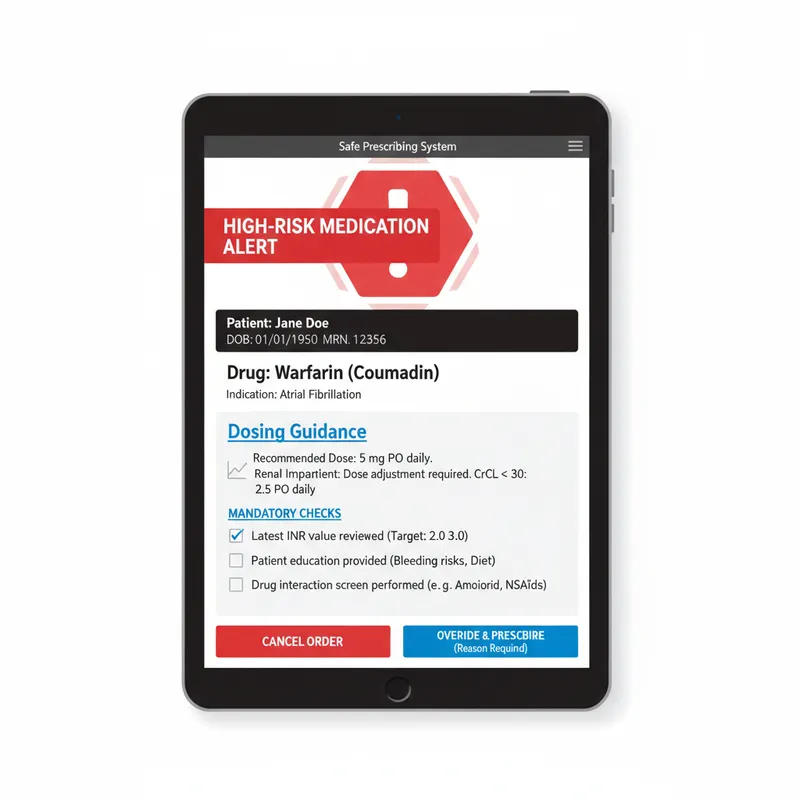
Recognising High-Risk Medicines in Clinical Practice
Understanding Why These Medicines Demand Enhanced Safety Protocols
The pharmacological properties that make certain medications highly effective also render them potentially lethal. share common characteristics: narrow therapeutic indices where the difference between therapeutic and toxic doses may be as small as 10-20%, steep dose-response curves where small dose changes produce disproportionate effects, and irreversible or difficult-to-reverse adverse effects. For anticoagulants, the balance between preventing thrombosis and causing haemorrhage operates within a remarkably narrow window - warfarin's therapeutic INR range of 2.0-3.0 represents only a 50% difference in anticoagulation intensity, yet INR >5.0 increases major bleeding risk 10-fold.
Pharmacological principles underlying high-risk classifications:
-
Therapeutic index (TI = LD50/ED50) considerations
- Warfarin TI approximately 2-3 (compare to amoxicillin TI >100)
- monitoring compensates for narrow TI
- Digoxin therapeutic range 0.5-2.0 ng/mL, toxic effects >2.5 ng/mL
-
Insulin pharmacodynamics create vulnerability
- Rapid-acting analogues peak 30-90 minutes post-injection
- Long-acting insulins provide 24-hour coverage with no peak
- protocols prevent type confusion (Novorapid vs Lantus)
- Dose timing errors: giving Novorapid at bedtime instead of mealtime causes nocturnal hypoglycaemia
-
Renal clearance dependencies
- DOACs (dabigatran, rivaroxaban, apixaban, edoxaban) require dose reduction when CrCl <50 mL/min
- Enoxaparin accumulation in renal impairment increases bleeding risk 3-4 fold
- NICE NG196 mandates annual renal function monitoring for all anticoagulated patients
| Medication | Therapeutic Range | Toxic Level | Monitoring Frequency | Reversal Agent |
|---|---|---|---|---|
| Warfarin | INR 2.0-3.0 | INR >5.0 | Weekly initially, then monthly | Vitamin K, PCC |
| Digoxin | 0.5-2.0 ng/mL | >2.5 ng/mL | 6-12 monthly | Digoxin-specific antibody |
| Lithium | 0.4-1.0 mmol/L | >1.5 mmol/L | 3-monthly when stable | None (haemodialysis) |
Understanding Why These Medicines Demand Enhanced Safety Protocols
Implementing Systematic Safety Checks in Clinical Scenarios
A 65-year-old man with type 2 diabetes presents for insulin initiation after metformin and gliclazide failed to achieve HbA1c <53 mmol/mol. Your prescribing approach must incorporate multiple safety layers: selecting appropriate insulin formulation, calculating starting dose based on weight and current glycaemic control, ensuring patient understands injection technique and timing, and establishing monitoring protocols. guidance recommends starting basal insulin (e.g., Lantus 10 units once daily or 0.1-0.2 units/kg) with clear written instructions distinguishing it from mealtime insulin. For anticoagulation scenarios, protocols require baseline assessment including renal function, bleeding risk scores (HAS-BLED), and drug interaction screening before first dose.
Systematic pre-prescribing safety checks:
-
For insulin initiation (NICE NG17 recommendations)
- Confirm insulin type, strength (usually U-100), and device (pen vs vial)
- Starting dose basal insulin: 10 units or 0.1-0.2 units/kg once daily
- Written plan: when to inject (bedtime for basal), how to store (fridge until opened)
- Hypoglycaemia recognition: symptoms when glucose <4.0 mmol/L
- Self-monitoring: fasting glucose target 5.0-7.0 mmol/L
-
For anticoagulation (warfarin or DOAC)
- CrCl calculation (Cockcroft-Gault) - determines DOAC dosing
- Bleeding risk: HAS-BLED score (≥3 indicates high risk, requires enhanced monitoring)
- Drug interactions: check BNF - particularly NSAIDs, antibiotics, antifungals
- Patient information: what to do if bleeding occurs, when to seek help
-
Monitoring protocols post-initiation
- Warfarin: INR day 3-4, then twice weekly until stable, then monthly
- Insulin: daily fasting glucose initially, HbA1c every 3-6 months
- DOACs: annual renal function, FBC (detect bleeding), LFTs
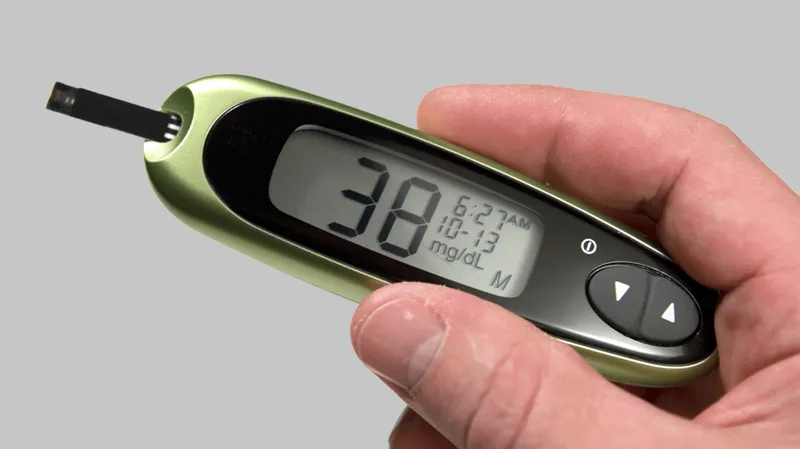
Implementing Systematic Safety Checks in Clinical Scenarios
Analysing Common Error Patterns in High-Risk Prescribing
Systematic analysis of medication incidents reveals predictable failure patterns. errors cluster around five categories: dose calculation mistakes (particularly weight-based dosing and unit conversions), look-alike/sound-alike drug confusion (Novorapid vs Novomix, heparin vs Hep-Flush), omitted monitoring (missing INR checks leading to over-anticoagulation), inadequate patient counselling (patients unaware of hypoglycaemia symptoms), and prescribing during transitions of care (hospital discharge errors). data shows 25% of insulin errors involve confusion between rapid-acting and long-acting formulations, while 30% involve 10-fold dose errors (prescribing 50 units instead of 5 units).
High-frequency error patterns and prevention strategies:
-
Dose calculation errors
- Insulin: confusing total daily dose with single-injection dose
- Enoxaparin: using actual body weight instead of capped weight (maximum 150 kg for treatment dosing)
- Morphine: incorrect opioid rotation calculations (morphine:oxycodone ratio 2:1, but individual variation significant)
-
Look-alike/sound-alike (LASA) confusion
- Novorapid (rapid-acting) vs Novomix (biphasic) - both in similar devices
- Heparin 1,000 units/mL vs 5,000 units/mL vs 25,000 units/mL concentrations
- Prevention: Tall Man lettering (NOVOrapid vs NovoMIX), separate storage
-
Monitoring omissions
- 15-20% of warfarin patients miss scheduled INR checks
- Consequences: INR >8.0 found incidentally, requiring vitamin K reversal
- Electronic flagging systems reduce missed monitoring by 60-70%
| Error Type | Frequency (% of incidents) | Typical Consequence | Prevention Strategy |
|---|---|---|---|
| Wrong insulin type | 25% | Hypo/hyperglycaemia | Separate storage, clear labelling |
| 10-fold dose error | 15% | Severe hypo/over-anticoagulation | Independent double-check |
| Missed monitoring | 20% | Delayed detection of toxicity | Automated alerts |
| LASA confusion | 18% | Wrong drug administered | Tall Man lettering |
Analysing Common Error Patterns in High-Risk Prescribing
Evaluating Complex Prescribing Decisions in Challenging Cases
A 72-year-old woman with atrial fibrillation (CHA₂DS₂-VASc score 4) requires anticoagulation, but she's had two falls in the past month and takes NSAIDs for osteoarthritis. This scenario demands sophisticated risk-benefit analysis. guidance indicates that fall risk alone rarely contraindicates anticoagulation - patients would need to fall 295 times annually for fall-related bleeding risk to outweigh stroke prevention benefit. However, the NSAID combination increases GI bleeding risk 3-4 fold, necessitating NSAID cessation or PPI co-prescription. decision frameworks incorporate bleeding risk (HAS-BLED), stroke risk (CHA₂DS₂-VASc), patient preferences, and practical factors like cognitive ability to manage monitoring.
Critical decision points for high-risk prescribing:
-
When to prescribe anticoagulation despite bleeding concerns
- CHA₂DS₂-VASc ≥2 in men, ≥3 in women - anticoagulation benefit typically outweighs risk
- HAS-BLED score ≥3 - doesn't contraindicate, but requires enhanced monitoring
- Consider DOAC over warfarin (40% lower intracranial bleeding risk)
-
When to withhold or modify therapy
- Active bleeding - temporarily withhold, investigate, treat cause
- CrCl <15 mL/min - most DOACs contraindicated (apixaban possible at reduced dose)
- Platelet count <50 × 10⁹/L - bleeding risk outweighs benefit in most cases
-
Insulin dose adjustment in acute illness
- Illness/infection increases insulin requirements 20-50%
- Reduced oral intake - continue basal insulin (prevents DKA), reduce/omit mealtime insulin
- "Sick day rules": never stop basal insulin, check glucose 4-hourly, seek help if glucose >15 mmol/L
| Clinical Scenario | CHA₂DS₂-VASc | HAS-BLED | Recommendation | Rationale |
|---|---|---|---|---|
| AF, previous stroke, no bleeding history | 5 | 1 | Anticoagulate (DOAC preferred) | High stroke risk, low bleeding risk |
| AF, age 65, hypertension, recurrent falls | 3 | 3 | Anticoagulate with caution | Falls don't outweigh stroke risk |
| AF, active PUD, previous GI bleed | 2 | 4 | Defer until bleeding controlled | Active bleeding = absolute contraindication |
Evaluating Complex Prescribing Decisions in Challenging Cases
Developing Team-Based Safety Strategies and Institutional Safeguards
Effective high-risk medication safety transcends individual prescriber competence, requiring robust institutional systems. safety frameworks incorporate electronic prescribing systems with hard-stop alerts for critical interactions (e.g., preventing methotrexate daily prescribing), mandatory independent double-checks for high-risk drugs (two practitioners verify insulin dose before administration), standardised monitoring protocols embedded in electronic health records, and structured patient education programs. initiatives include colour-coded insulin storage (rapid-acting in one fridge section, long-acting in another), pre-printed insulin charts eliminating handwriting errors, and pharmacist-led insulin counselling before first dose. programs establish dedicated anticoagulation clinics with nurse-led INR monitoring, achieving time-in-therapeutic-range (TTR) >70% compared to <60% with usual care.
Multi-layered institutional safety interventions:
-
Electronic prescribing safeguards
- Dose range checking: alerts if insulin dose >1 unit/kg or warfarin >10 mg
- Drug interaction screening: automatic alerts for DOAC + NSAID combinations
- Renal dose adjustment prompts: system suggests reduced dose when CrCl <50 mL/min
-
Standardised protocols and checklists
- Insulin initiation checklist: 8-point verification (right patient, drug, dose, time, route, documentation, patient understanding, hypoglycaemia plan)
- Anticoagulation reversal protocols: immediate access to vitamin K, prothrombin complex concentrate, idarucizumab (dabigatran reversal)
-
Patient empowerment strategies
- Written information: NICE-approved patient decision aids for anticoagulation
- Alert cards: patients carry cards stating anticoagulant type, dose, prescriber contact
- Self-monitoring programs: patient self-testing INR reduces major bleeding by 30%
-
Multidisciplinary team roles
- Pharmacists: medication reconciliation at admission/discharge (prevents 60% of prescribing errors)
- Specialist nurses: anticoagulation clinics, diabetes nurse educators
- Clinical governance: monthly review of medication incidents, root cause analysis

Developing Team-Based Safety Strategies and Institutional Safeguards
High Yield Summary
Key Take-Aways:
- High-risk medicines (anticoagulants, insulin, opioids, chemotherapy) account for 60% of preventable medication-related deaths despite representing <5% of prescriptions
- Therapeutic index <3 defines high-risk drugs - warfarin, digoxin, lithium require regular monitoring to maintain narrow therapeutic ranges
- Systematic safety checks include dose verification, renal function assessment, drug interaction screening, and structured monitoring protocols
- Common error patterns: 10-fold dose errors, LASA confusion (Novorapid vs Novomix), missed monitoring, inadequate patient counselling
- Falls rarely contraindicate anticoagulation (would require 295 falls/year to outweigh stroke prevention benefit), but active bleeding mandates temporary withholding
- Institutional safeguards (electronic alerts, double-checks, pharmacist reviews) reduce high-risk medication errors by 60-70%
Essential Safe Prescribing Numbers:
| Parameter | Critical Value | Clinical Action |
|---|---|---|
| Warfarin INR | >5.0 | Omit dose, consider vitamin K 1-5 mg PO |
| Warfarin INR | >8.0 | Vitamin K 5 mg PO, check for bleeding |
| Hypoglycaemia | <4.0 mmol/L | 15-20 g quick-acting carbohydrate |
| Severe hypoglycaemia | <3.0 mmol/L | Consider IM glucagon 1 mg or IV glucose |
| DOAC dose reduction | CrCl <50 mL/min | Reduce dose (drug-specific) |
| HAS-BLED score | ≥3 | Enhanced monitoring, address modifiable risks |
Key Principles/Pearls:
- Never prescribe methotrexate daily - weekly dosing only (except for acute leukaemia in specialist centres)
- "When in doubt, check renal function" - CrCl determines dosing for DOACs, enoxaparin, many antibiotics
- Insulin dose adjustments: increase by 2-4 units (10-20%) every 3-4 days based on fasting glucose trends, not single readings
- DOACs don't require monitoring, but annual renal function and FBC checks are mandatory (NICE NG196)
- Anticoagulation reversal: warfarin (vitamin K + PCC), dabigatran (idarucizumab), Xa inhibitors (andexanet alfa if available)
Quick Reference:
| High-Risk Drug | Starting Dose | Monitoring | Key Interaction | Reversal |
|---|---|---|---|---|
| Warfarin | 5 mg daily (3 mg if elderly) | INR day 3-4, then weekly | Antibiotics, NSAIDs | Vitamin K, PCC |
| Apixaban | 5 mg BD (2.5 mg if ≥2 of: age ≥80, weight ≤60 kg, creatinine ≥133) | Annual CrCl, FBC | NSAIDs increase bleeding | Andexanet alfa |
| Basal insulin | 10 units or 0.1-0.2 units/kg once daily | Daily fasting glucose | Steroids increase requirements | IV glucose, glucagon |
| Enoxaparin (treatment) | 1.5 mg/kg once daily (max 150 kg) | Anti-Xa if renal impairment | NSAIDs, antiplatelets | Protamine sulphate |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app






