Ethics & Law

On this page
Foundations of Consent, Capacity, and End-of-Life Law
A 78-year-old woman with advanced dementia is admitted with aspiration pneumonia. Her daughter insists on intravenous antibiotics, but the patient repeatedly pulls out the cannula and becomes distressed when staff approach. The medical team must navigate the legal framework governing consent and capacity , balancing the patient's best interests against family wishes. Understanding the statutory principles that underpin these decisions is not merely academic-it determines whether treatment proceeds, who makes decisions when patients cannot, and how we respect autonomy while protecting vulnerable individuals.
-
Valid consent requires three elements:
- Capacity: Patient must understand, retain, weigh, and communicate their decision
- Information: Material risks disclosed in terms the patient understands (Montgomery ruling 2015)
- Voluntariness: Decision free from coercion or undue influence
-
Mental Capacity Act 2005 statutory principles:
- Presumption of capacity unless proven otherwise
- Right to make unwise decisions (capacity-specific, not outcome-dependent)
- All practicable steps to support decision-making before declaring incapacity
- Best interests if lacking capacity
- Least restrictive option
-
Capacity assessment is decision-specific and time-specific
- Patient may have capacity for simple decisions (e.g., what to eat) but not complex ones (e.g., refusing life-sustaining treatment)
- Fluctuating capacity requires assessment at optimal times
📌 Mnemonic: URAC for capacity assessment-Understand information, Retain it, Appreciate/weigh consequences, Communicate decision
| Legal Framework | Applicability | Key Threshold |
|---|---|---|
| Mental Capacity Act 2005 | Adults ≥16 years lacking capacity | Two-stage test: impairment AND functional inability |
| Adults with Incapacity (Scotland) Act 2000 | Scotland only | Benefit, least restrictive, patient's wishes |
| Common law (emergency) | All patients when capacity assessment impractical | Immediate necessity to save life/prevent deterioration |
Foundations of Consent, Capacity, and End-of-Life Law
2 - Pathways of Decision-Making: The Mental Capacity Act Framework
The Mental Capacity Act establishes a two-stage test that moves from diagnostic threshold to functional assessment. First, does the patient have an impairment or disturbance of mind or brain functioning? This could be delirium, dementia, learning disability, mental illness, or even temporary states like intoxication or acute confusion. Crucially, diagnosis alone never determines capacity-a patient with schizophrenia may retain full capacity for medical decisions. The second stage asks whether this impairment prevents the patient from understanding, retaining, weighing, or communicating the specific decision at hand . This functional approach protects autonomy while recognizing genuine vulnerability.
-
Stage 1: Diagnostic threshold
- Impairment/disturbance must be present (temporary or permanent)
- Examples: delirium (ACB score >3), stroke affecting communication, severe depression with nihilistic beliefs
-
Stage 2: Functional test (all four must be assessable)
- Understand: Can patient grasp information about treatment, alternatives, consequences?
- Retain: Hold information long enough to make decision (minutes sufficient)
- Weigh/Appreciate: Use information to evaluate options in context of their values
- Communicate: Express choice by any means (speech, writing, blinking, Makaton)
-
Best interests decisions when capacity lacking:
- Consult advance decisions, Lasting Power of Attorney (LPA), family views
- Consider patient's past/present wishes, beliefs, values
- Not determined by age, appearance, or assumptions about quality of life
- Court of Protection involvement for major decisions (withdrawal of life-sustaining treatment, serious medical treatment disputes)
| Advance Planning Tool | Legal Authority | Limitations |
|---|---|---|
| Advance Decision to Refuse Treatment (ADRT) | Legally binding if valid and applicable | Must be specific; cannot demand treatment; life-sustaining refusal needs written, witnessed signature |
| Lasting Power of Attorney (Health & Welfare) | Attorney makes decisions when donor lacks capacity | Cannot override valid ADRT; must act in donor's best interests |
| Advance Statement (wishes) | Not legally binding but must be considered | Guides best interests; weaker than ADRT |
2 — Pathways of Decision-Making: The Mental Capacity Act Framework
3 - Clinical Application: Assessing Capacity and Obtaining Consent
A 45-year-old man with alcohol dependence syndrome presents with haematemesis. He refuses endoscopy, stating "I don't want cameras inside me." Does he have capacity? The assessment begins with optimizing conditions-treating his Wernicke's encephalopathy with IV thiamine, waiting until his blood alcohol drops below 80 mg/dL, and using visual aids to explain the procedure . You document that he understands endoscopy identifies bleeding sources, retains this through questioning, weighs the risk of rebleeding (15% without intervention) against procedural risks (<1% perforation), and clearly communicates refusal. Despite the "unwise" decision, he has capacity-his refusal stands.
-
Practical capacity assessment steps:
- Optimize environment: quiet space, hearing aids, interpreters, family support
- Provide information in accessible format: pictures, simple language, repeat key points
- Test understanding: "Tell me in your own words what this treatment does"
- Assess weighing: "What might happen if you don't have this treatment?" "What concerns you most?"
- Document thoroughly: specific questions asked, responses given, reasoning
-
Emergency treatment without consent:
- Common law permits immediate treatment when capacity assessment impractical
- Scope limited to immediate necessity (stabilize, not definitive treatment)
- Example: Intubate unconscious trauma patient, but defer non-urgent surgery until capacity assessed
-
Consent for procedures: information disclosure post-Montgomery:
- Material risks: those a reasonable person in patient's position would attach significance to
- Include frequency, severity, and alternatives
- For endoscopy: perforation 1:1000, bleeding 1:100, sedation risks, alternative of CT angiography
🚩 Red Flag: Never assume incapacity based on diagnosis, age, or communication difficulty. A patient with severe learning disability may have capacity for simple treatment decisions if information presented accessibly.
| Clinical Scenario | Capacity Likely? | Action |
|---|---|---|
| Delirium with AMT <7 | Unlikely | Treat in best interests; reassess daily |
| Dementia (MMSE 18) refusing antibiotics | Possibly-assess specifically | Full URAC assessment; consider reasons for refusal |
| Intoxicated (GCS 14) refusing sutures | Unlikely | Treat if urgent; defer if can wait until sober |
| Psychosis refusing antipsychotics | Variable | Assess insight; MHA if mental disorder causing risk |
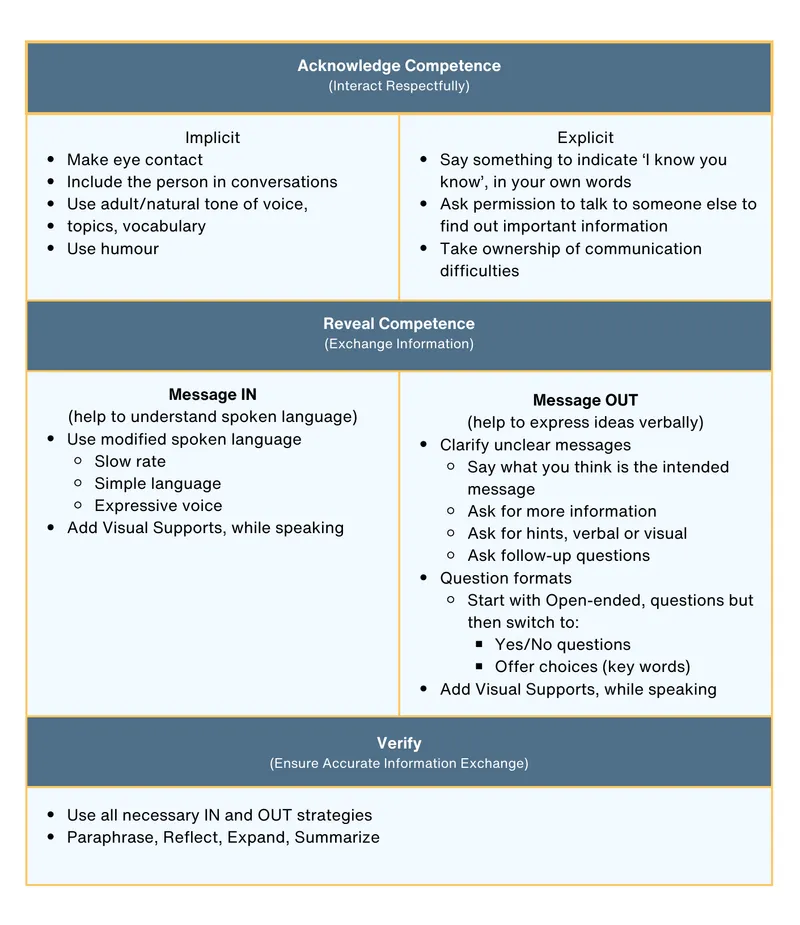

3 — Clinical Application: Assessing Capacity and Obtaining Consent
4 - Analyzing Complex Cases: When Capacity is Disputed
The challenge intensifies when families disagree with capacity assessments or patients make decisions that seem to defy self-preservation. A 32-year-old Jehovah's Witness with postpartum haemorrhage (Hb 52 g/L) refuses blood transfusion. She clearly understands she may die, appreciates the consequences for her newborn, weighs this against her religious beliefs, and communicates refusal consistently . Her capacity is intact-yet her husband demands you override her decision. The law is unambiguous: a capacitous adult's refusal is absolute, even if it results in death. Contrast this with a patient whose severe depression causes nihilistic delusions ("I'm already dead, treatment is pointless")-here, the mental disorder directly impairs weighing ability, potentially negating capacity.
-
Discriminating genuine incapacity from unwise decisions:
- Incapacity: Unable to engage with reasoning process, no appreciation of consequences
- Unwise but capacitous: Engages with information, weighs according to personal values (even if clinician disagrees)
-
Common pitfalls in capacity assessment:
- Assuming fluctuating capacity means permanent incapacity (assess at optimal times)
- Conflating disagreement with incapacity ("patient refuses so must lack capacity")
- Failing to address reversible causes (pain, hypoglycaemia, constipation affecting cognition)
- Overlooking coercion from family members
| Distinguishing Feature | Has Capacity | Lacks Capacity |
|---|---|---|
| Understanding | Repeats information accurately | Cannot grasp basic concepts despite repeated explanation |
| Retention | Holds information during conversation | Forgets within seconds; cannot recall discussion |
| Weighing | Relates decision to personal values/beliefs | Cannot engage with consequences; reasoning absent |
| Communication | Expresses clear choice (even if fluctuating) | Unable to indicate preference by any means |
4 — Analyzing Complex Cases: When Capacity is Disputed
5 - Evaluating End-of-Life Decisions: Legal and Ethical Frameworks
A 68-year-old man with motor neurone disease has created an Advance Decision refusing mechanical ventilation when he loses capacity to swallow. Six months later, he develops aspiration pneumonia with type 2 respiratory failure . The ADRT is valid (written, signed, witnessed, specifies life-sustaining treatment refusal), applicable (current situation matches described scenario), and not overridden by subsequent actions. The medical team must respect it, even if his family pleads for ventilation. NICE NG108 emphasizes that advance care planning discussions should occur early in progressive diseases, documenting specific treatments the patient would refuse and circumstances triggering those refusals.
-
Withdrawing/withholding life-sustaining treatment:
- Legally equivalent (no distinction between acts and omissions in best interests framework)
- Requires best interests assessment if patient lacks capacity
- Clinically assisted nutrition and hydration (CANH) is medical treatment-can be withdrawn if not in best interests
- Court of Protection involvement required for CANH withdrawal in prolonged disorders of consciousness
-
DNACPR decisions (ReSPECitation guidelines):
- Made when CPR unlikely to succeed OR not in patient's best interests
- Discuss with patient if they have capacity and discussion not causing disproportionate harm
- Document rationale clearly; review regularly
- Does NOT mean withholding other treatments (common misconception)
-
Palliative sedation vs euthanasia:
- Doctrine of double effect: Intending symptom relief, accepting death as foreseen but unintended consequence
- Proportionate doses of morphine/midazolam for refractory symptoms are lawful
- Intentionally causing death remains unlawful in UK
| Medication | Indication in End-of-Life Care | Typical Dose |
|---|---|---|
| Morphine sulfate | Pain, breathlessness | 2.5-5 mg SC/IV PRN; 10-30 mg/24h CSCI |
| Midazolam | Agitation, distress, terminal restlessness | 2.5-5 mg SC PRN; 10-30 mg/24h CSCI |
| Hyoscine butylbromide | Respiratory secretions ("death rattle") | 20 mg SC PRN; 60-120 mg/24h CSCI |
| Levomepromazine | Nausea, agitation (refractory) | 6.25-12.5 mg SC PRN; 25-100 mg/24h CSCI |

5 — Evaluating End-of-Life Decisions: Legal and Ethical Frameworks
6 - Synthesis: Integrating Law, Ethics, and Clinical Complexity
An 82-year-old woman with severe dementia (MMSE 8) develops recurrent aspiration pneumonia. She has no ADRT or LPA. Her daughter insists on PEG feeding; her son argues "Mum would never want this." The MDT convenes a best interests meeting . Evidence suggests PEG feeding in advanced dementia does not improve survival or quality of life (NICE NG108), and the patient resists oral feeding, suggesting possible food refusal as an expression of residual autonomy. After consulting both children, reviewing care home records of her previous statements, and considering her current distress with interventions, the team concludes PEG insertion is not in her best interests. This synthesis requires balancing legal obligations (presumption to sustain life), ethical principles (respect for autonomy, non-maleficence), clinical evidence, and family perspectives-recognizing that family do not have legal decision-making authority but their insights into the patient's values are crucial.
-
Special populations requiring tailored approaches:
- Learning disabilities: Use accessible communication tools; involve carers who know patient well; capacity may be present for specific decisions with support
- Mental illness under Mental Health Act: MHA authorizes treatment for mental disorder only; physical health decisions still require consent or capacity assessment
- Young people 16-17: Can consent to treatment (Family Law Reform Act 1969) but refusal can be overridden by court if life-threatening
-
Resolving disputes:
- Independent Mental Capacity Advocate (IMCA) for unbefriended patients
- Second opinions from senior clinicians
- Court of Protection for serious medical treatment disputes, CANH withdrawal, or organ donation decisions
-
Recent legal precedents shaping practice:
- Montgomery v Lanarkshire (2015): Shifted consent from professional to patient-centered standard
- Aintree v James (2013): Best interests not determined by family preferences or clinical opinion alone-patient's wishes paramount
- Re Y (2017): CANH withdrawal in prolonged disorders of consciousness requires court approval
| Clinical Challenge | Legal Framework | Practical Approach |
|---|---|---|
| Patient lacks capacity, no family | IMCA referral mandatory | Local authority appoints advocate; best interests meeting includes IMCA |
| Family demands futile treatment | Clinicians not obligated to provide futile treatment | Explain clinical reasoning; offer second opinion; court if unresolved |
| Fluctuating capacity (delirium) | Assess at best times; defer non-urgent decisions | Treat delirium; reassess daily; use capacity-supporting strategies |
| Pregnant patient refusing treatment | Fetus has no legal rights; mother's autonomy absolute | Respect refusal if capacitous; psychiatric assessment if capacity doubted |
6 — Synthesis: Integrating Law, Ethics, and Clinical Complexity
High Yield Summary
Key Take-Aways:
- Valid consent requires capacity, information (material risks post-Montgomery), and voluntariness-all three elements must be present
- Mental Capacity Act 2005: Two-stage test (diagnostic impairment AND functional inability to understand/retain/weigh/communicate)
- Capacity is decision-specific and time-specific-never assume global incapacity based on diagnosis
- Advance Decision to Refuse Treatment is legally binding if valid, applicable, and not overridden; must be written/witnessed for life-sustaining treatment refusal
- Best interests decisions require consulting family, considering patient's wishes/values, and choosing least restrictive option-not determined by family preferences or clinical opinion alone
- Withdrawing and withholding treatment are legally equivalent; CANH withdrawal in prolonged disorders of consciousness requires Court of Protection approval
- DNACPR decisions require discussion with capacitous patients unless causing disproportionate harm; do not equate to withholding all treatment
Essential Ethics & Law Numbers/Formulas:
| Legal Threshold | Value/Criterion |
|---|---|
| Age of consent to treatment | 16 years (England/Wales) |
| ADRT for life-sustaining treatment | Must be written, signed, witnessed |
| AMT threshold suggesting delirium | <7/10 (capacity assessment still required) |
| Montgomery standard | Material risk disclosure-what reasonable patient would want to know |
| Emergency treatment scope | Immediate necessity only; reassess capacity when practical |
Key Principles/Pearls:
- Presume capacity unless proven otherwise-burden of proof on assessor, not patient
- "Unwise decision" does not equal incapacity; patient with capacity can refuse life-saving treatment
- Document capacity assessments meticulously: specific questions, responses, reasoning process, and decision reached
- Family have no automatic legal decision-making authority for adults (unless appointed as LPA)-their role is informing best interests
- Avoid common error: assuming patient who cannot communicate lacks capacity-explore all communication methods (blinking, assistive technology)
Quick Reference:
| Scenario | Legal Authority | Action |
|---|---|---|
| Capacitous refusal of life-saving treatment | Common law autonomy | Respect refusal; document thoroughly |
| Incapacitous patient, no ADRT/LPA | Mental Capacity Act best interests | MDT decision; consult family for values/wishes |
| Valid ADRT refusing ventilation | Advance Decision legally binding | Follow ADRT; do not ventilate |
| Emergency, capacity unknown | Common law necessity | Treat immediately; reassess capacity when stable |
| CANH withdrawal in PVS | Court of Protection jurisdiction | Apply to court before withdrawal |
High Yield Summary
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




