Quick Overview
Diabetic emergencies-DKA and HHS-are life-threatening complications requiring immediate recognition and structured management. DKA predominantly affects Type 1 diabetes; HHS occurs in Type 2. Both demand meticulous fluid resuscitation, insulin therapy, and electrolyte monitoring per NICE NG17 guidelines. Mortality in HHS reaches 15-20% vs 1-5% in DKA.
Core Facts & Concepts
Diagnostic Criteria (NICE NG17):
| Parameter | DKA | HHS |
|---|---|---|
| Glucose | >11 mmol/L | >30 mmol/L (typically) |
| pH | <7.3 | >7.3 |
| Bicarbonate | <15 mmol/L | >15 mmol/L |
| Ketones | >3 mmol/L (blood) or 2+ (urine) | <3 mmol/L |
| Osmolality | Usually <320 mOsm/kg | >320 mOsm/kg |
📊 Calculated Osmolality: 2(Na + K) + Glucose + Urea (all in mmol/L)

Fluid Resuscitation Protocol:
- 0.9% NaCl first-line (NOT Hartmann's initially)
- 1L over 1st hour, then 1L over 2 hours (×2), then 1L over 4 hours (×2)
- Add 0.45% NaCl if osmolality not falling despite adequate positive fluid balance (HHS)
- Switch to 10% glucose when capillary glucose <14 mmol/L (continue insulin)
💊 Fixed-Rate IV Insulin (FRIII):
- 0.1 units/kg/hour (typically 5-7 units/hour for 70kg adult)
- Continue long-acting insulin analogues; STOP short-acting
- Target ketone reduction: 0.5 mmol/L/hour
- Target glucose reduction: 3 mmol/L/hour
Potassium Replacement Thresholds:
| Serum K+ (mmol/L) | Action |
|---|---|
| <3.5 | Senior review; replace before insulin |
| 3.5-5.5 | Add 40 mmol KCl/L to fluids |
| >5.5 | No replacement; recheck hourly |
Problem-Solving Approach
Step-by-Step Management:
- Immediate: IV access (2 lines), bloods (VBG, U&E, glucose, ketones, FBC, cultures), ECG
- Fluid resuscitation: 0.9% NaCl per protocol above
- Start FRIII: 0.1 units/kg/hour via pump (separate line from fluids)
- Potassium replacement: Per table above-check hourly initially
- Identify precipitant: Infection (40%), non-compliance (25%), MI, pancreatitis
- Monitor hourly: Ketones, glucose, K+, VBG (until pH >7.3)
- Resolution criteria (DKA): pH >7.3 AND ketones <0.6 mmol/L AND bicarbonate >15 mmol/L
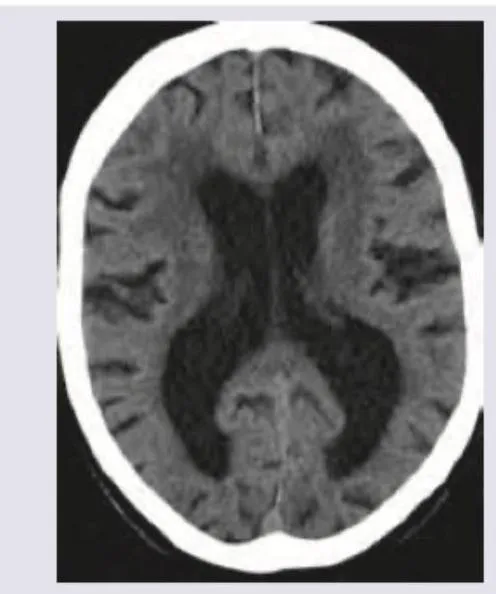
🚩 Red Flags-Cerebral Oedema (1-2% of DKA, mainly children/young adults):
- Headache, altered consciousness, bradycardia
- Risk factors: Age <5 years, severe acidosis (pH <7.1), rapid fall in glucose/osmolality
- Management: Hypertonic saline (2.7% or 3%) 2.5-5mL/kg over 10-15 minutes; senior/ICU input immediately
⚠️ Warning: Never stop IV insulin until ketones <0.6 mmol/L AND eating/drinking-causes rebound ketoacidosis. Overlap SC insulin by 30-60 minutes before stopping FRIII.
Analysis Framework
DKA vs HHS-Key Discriminators:
| Feature | DKA | HHS |
|---|---|---|
| Onset | Hours-days | Days-weeks |
| Dehydration | Moderate (5-8L deficit) | Severe (8-12L deficit) |
| Age group | Younger (Type 1) | Older (Type 2) |
| Ketosis | Prominent | Minimal/absent |
| Thrombosis risk | Low | High (25%-requires prophylactic LMWH) |
| Cerebral oedema | 1-2% (children) | Rare |
Precipitants (Mnemonic):
📌 Remember: The 5 I's - Infection (40%), Infarction (MI), Insufficient insulin, Intoxication (alcohol), Iatrogenic (steroids, thiazides)
Visual Aid
Key Points Summary
✓ DKA triad: Glucose >11, ketones >3, pH <7.3 (bicarbonate <15)
✓ HHS: Osmolality >320, minimal ketosis, severe dehydration (8-12L deficit)
✓ FRIII: 0.1 units/kg/hour; reduce ketones by 0.5 mmol/L/hour; glucose by 3 mmol/L/hour
✓ Potassium: Replace if <5.5 mmol/L (40 mmol/L in fluids); never start insulin if K+ <3.5
✓ Cerebral oedema: Rare but fatal; suspect if headache/drowsiness worsening; give hypertonic saline immediately
✓ HHS: Thromboprophylaxis mandatory (LMWH); slower fluid replacement to avoid osmotic demyelination
✓ Resolution: pH >7.3 AND ketones <0.6 AND bicarbonate >15-overlap SC insulin before stopping FRIII
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

