Cardiology

On this page
Defining the Cardiovascular Landscape: Classifications and Diagnostic Criteria
The 52-year-old man in your clinic has a blood pressure of 156/98 mmHg on three separate occasions, a BMI of 31, and his father died of a myocardial infarction at age 58. Before you can calculate his cardiovascular risk or choose therapy, you must first understand the precise definitions that underpin modern cardiology. The classification systems for distinguish stage 1 (140-159/90-99 mmHg) from stage 2 (≥160/100 mmHg) hypertension, while divides patients by left ventricular ejection fraction: reduced (HFrEF, LVEF <40%), mildly reduced (HFmrEF, 40-49%), and preserved (HFpEF, ≥50%). Meanwhile, employs the CHA₂DS₂-VASc score to stratify stroke risk, transforming clinical features into actionable thresholds.
Hypertension Classification (NICE NG136):
- Stage 1: Clinic BP 140-159/90-99 mmHg AND ABPM/HBPM ≥135/85 mmHg
- Treat if <80 years with target organ damage, CVD, renal disease, diabetes, or QRISK ≥10%
- Stage 2: Clinic BP ≥160/100 mmHg AND ABPM/HBPM ≥150/95 mmHg
- Offer treatment to all patients regardless of age
- Stage 3 (hypertensive emergency): Clinic systolic ≥180 mmHg or diastolic ≥120 mmHg
- Same-day specialist assessment if signs of papilloedema or retinal haemorrhage
Heart Failure Phenotypes:
- HFrEF: LVEF <40%, responds to ACE-I/ARB, beta-blockers, mineralocorticoid receptor antagonists, SGLT2 inhibitors
- HFpEF: LVEF ≥50%, NT-proBNP >125 pg/mL, structural/functional abnormalities
- Limited pharmacological options; SGLT2 inhibitors (dapagliflozin) now evidence-based
- Epidemiology: 920,000 people in UK have diagnosed heart failure; 5-year mortality ~50%
| Condition | Key Diagnostic Threshold | Population Prevalence (UK) |
|---|---|---|
| Hypertension (treated) | Clinic BP ≥140/90 mmHg | 31% adults (14 million) |
| Atrial fibrillation | Irregularly irregular pulse + ECG confirmation | 2.5% (1.4 million) |
| Heart failure | NT-proBNP >2000 pg/mL (urgent echo within 2 weeks) | 1.5% adults |
| Stable angina | Typical chest pain + obstructive CAD | 2.1% adults |
📌 Mnemonic for HFpEF diagnosis (HFA-PEFF): P-BNP elevated, Echocardiographic abnormalities, Functional testing abnormal, Fibrosis/structural changes
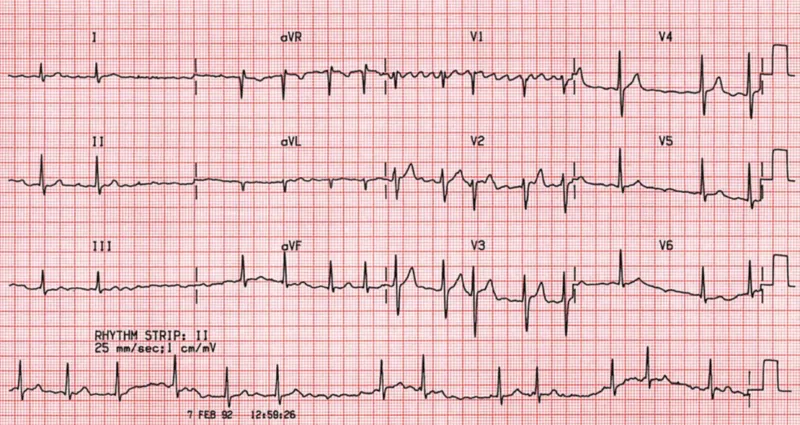

Defining the Cardiovascular Landscape: Classifications and Diagnostic Criteria
Understanding Cardiovascular Pathophysiology: From Risk to Acute Events
Why does a 10 mmHg reduction in systolic blood pressure reduce stroke risk by 27% and ischaemic heart disease by 17%? The answer lies in understanding how endothelial dysfunction, arterial stiffness, and atherosclerotic plaque progression interact over decades. quantifies this cumulative burden by integrating age, sex, ethnicity, smoking, diabetes, chronic kidney disease, atrial fibrillation, rheumatoid arthritis, cholesterol ratio, systolic BP, and BMI into a 10-year CVD risk percentage. When progresses to , the pathophysiology shifts from stable plaque with fixed stenosis causing demand-supply mismatch to plaque rupture with thrombosis causing acute myocardial injury.
Atherosclerosis Progression:
- Fatty streak (age 10-20): Lipid accumulation in intima, macrophage foam cells
- Fibrous plaque (age 30-40): Smooth muscle proliferation, collagen cap formation
- Complex plaque (age 50+): Necrotic core, thin fibrous cap (<65 μm = vulnerable plaque)
- Rupture triggers platelet aggregation → thrombus formation
- 70% of acute MI occur at sites with <50% stenosis pre-event
QRISK3 Calculation Principles:
- Estimates 10-year risk of CVD (MI, stroke, TIA, angina)
- High risk: ≥10% → offer statin (atorvastatin 20 mg)
- Moderate risk: 5-9.9% → discuss lifestyle + consider statin
- Recalculate every 5 years if not on treatment
Atrial Fibrillation and Stroke Risk:
- AF increases stroke risk 5-fold through left atrial appendage thrombus formation
- CHA₂DS₂-VASc score: Congestive HF (1), Hypertension (1), Age ≥75 (2), Diabetes (1), Stroke/TIA (2), Vascular disease (1), Age 65-74 (1), Sex (female, 1)
- Score ≥2 (men) or ≥3 (women): offer anticoagulation
- DOACs preferred over warfarin (apixaban 5 mg BD, rivaroxaban 20 mg OD, edoxaban 60 mg OD)
Understanding Cardiovascular Pathophysiology: From Risk to Acute Events
Diagnostic Pathways: From Symptoms to Confirmation
A 68-year-old woman presents with 20 minutes of crushing central chest pain radiating to her left arm, associated with nausea and sweating. Your immediate ECG shows 3 mm ST elevation in leads V2-V4. This is an anterior STEMI requiring immediate catheter lab activation within 120 minutes of first medical contact. Contrast this with the 55-year-old man with exertional chest tightness relieved by rest: you arrange CT coronary angiography as first-line investigation per NICE CG95, which has 95% sensitivity and 83% specificity for obstructive coronary disease. demands troponin measurement at 0 and 3 hours (high-sensitivity assays), while requires NT-proBNP followed by echocardiography within 2 weeks if >2000 pg/mL or 6 weeks if 400-2000 pg/mL. diagnosis relies on echocardiographic criteria: severe aortic stenosis defined as valve area <1.0 cm², mean gradient >40 mmHg, or peak velocity >4.0 m/s.
Acute Coronary Syndrome Diagnostic Algorithm:
- STEMI criteria: ST elevation ≥2.5 mm (men <40 years), ≥2 mm (men ≥40 years), ≥1.5 mm (women) in V2-V3, OR ≥1 mm in other contiguous leads
- Activate catheter lab immediately; door-to-balloon <90 minutes
- NSTEMI/Unstable angina: Troponin elevation (hs-cTnI >99th percentile) without ST elevation
- GRACE score determines timing of angiography (<72 hours if high risk)
| Investigation | Sensitivity | Specificity | Clinical Use |
|---|---|---|---|
| High-sensitivity troponin (3-hour protocol) | 98-99% | 85-90% | Rule out ACS |
| CT coronary angiography | 95% | 83% | First-line for stable chest pain |
| Exercise ECG | 68% | 77% | Limited role; superseded by CT |
| NT-proBNP >400 pg/mL | 95% | 44% | Rule out heart failure |
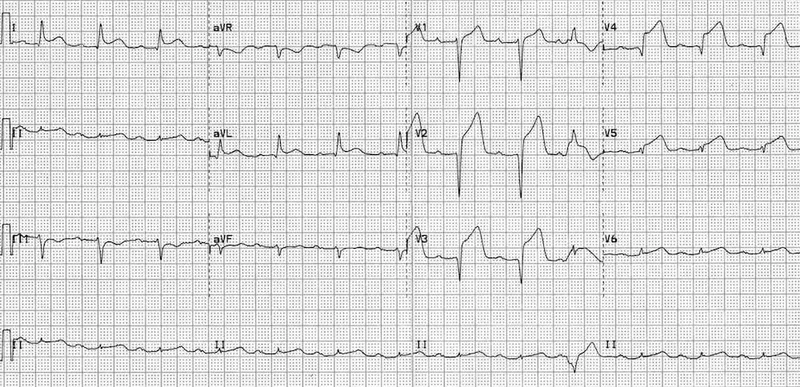
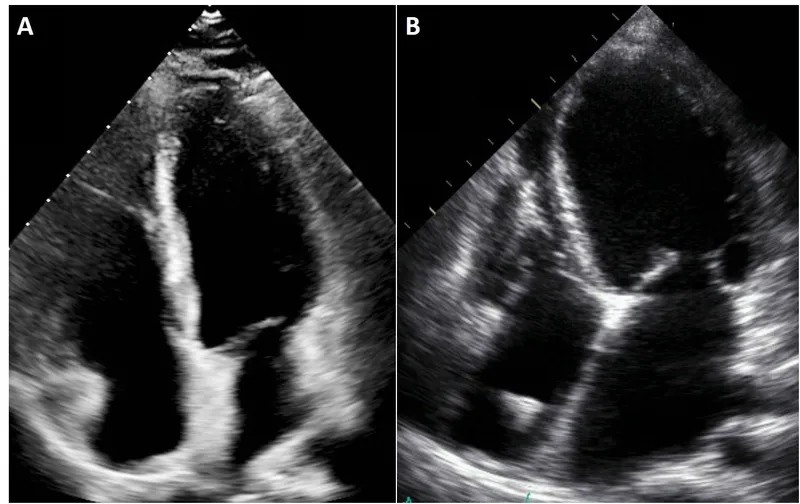
Diagnostic Pathways: From Symptoms to Confirmation
Differentiating Cardiovascular Presentations: Key Clinical Discriminators
Why does one patient with chest pain need immediate catheter lab activation while another requires outpatient CT angiography? The answer lies in precise clinical phenotyping. presents with palpitations, dyspnoea, or stroke, distinguished from ventricular tachycardia by irregularly irregular pulse and absent P waves. requires differentiation of primary (95%) from secondary causes (renal artery stenosis, Conn's syndrome, phaeochromocytoma), triggered by age <40, resistant hypertension (≥4 drugs), or hypokalaemia. is distinguished from ACS by symptom duration (<15 minutes vs. >20 minutes) and troponin dynamics.
Chest Pain Differentials:
- Cardiac: Troponin elevation, ECG changes, radiation to arms/jaw
- STEMI: ST elevation, immediate catheter lab
- NSTEMI: Troponin rise without ST elevation, risk-stratified management
- Stable angina: Exertional, <15 minutes, normal resting ECG
- Non-cardiac: Pleuritic (worse on inspiration), positional (pericarditis/MSK), oesophageal (meal-related)
| Feature | STEMI | NSTEMI | Stable Angina | Pericarditis |
|---|---|---|---|---|
| Pain duration | >20 min | >20 min | <15 min | Continuous |
| ECG | ST elevation | ST depression/T inversion | Normal or old changes | Widespread ST elevation + PR depression |
| Troponin | Elevated | Elevated | Normal | Normal or mildly elevated |
| Management urgency | Immediate PCI | Risk-stratified (GRACE) | Outpatient CT-CA | NSAIDs + colchicine |
Heart Failure vs. COPD Exacerbation:
- HF: Orthopnoea, paroxysmal nocturnal dyspnoea, raised JVP, S3 gallop, bilateral basal creps
- NT-proBNP >2000 pg/mL strongly suggests HF
- COPD: Wheeze, hyperinflation, prolonged expiration, smoking history
- NT-proBNP <300 pg/mL makes HF unlikely
🚩 Red Flag: Hypokalaemia (<3.5 mmol/L) + hypertension → screen for primary aldosteronism (aldosterone:renin ratio >750 pmol/mU)
Differentiating Cardiovascular Presentations: Key Clinical Discriminators
Evidence-Based Management: From Guidelines to Bedside
NICE NG136 revolutionised hypertension management by mandating ambulatory or home BP monitoring to confirm diagnosis, preventing overtreatment of white-coat hypertension (10% of patients). First-line therapy depends on age and ethnicity: ACE inhibitors (ramipril 2.5-10 mg OD) or ARBs (losartan 50-100 mg OD) for age <55 and non-Black ethnicity; calcium channel blockers (amlodipine 5-10 mg OD) for age ≥55 or Black ethnicity. informs statin therapy: atorvastatin 20 mg for primary prevention if QRISK ≥10%, targeting non-HDL reduction >40%. management follows the "four pillars": ACE-I/ARB (ramipril target 10 mg OD), beta-blocker (bisoprolol target 10 mg OD), mineralocorticoid receptor antagonist (spironolactone 25 mg OD), and SGLT2 inhibitor (dapagliflozin 10 mg OD). requires surgical intervention when severe symptomatic aortic stenosis develops (valve replacement) or severe mitral regurgitation causes symptoms/LV dysfunction.
Hypertension Step-Up Therapy:
- Step 1: ACE-I/ARB (age <55, non-Black) OR CCB (age ≥55 or Black)
- Step 2: ACE-I/ARB + CCB
- Step 3: ACE-I/ARB + CCB + thiazide-like diuretic (indapamide 2.5 mg OD)
- Step 4 (resistant): Add spironolactone 25 mg OD (if K+ ≤4.5 mmol/L) OR alpha/beta-blocker
| Drug Class | Example + Dose | Monitoring | Key Contraindication |
|---|---|---|---|
| ACE inhibitor | Ramipril 10 mg OD | U&E at 1-2 weeks (Cr rise <30% acceptable) | Bilateral renal artery stenosis |
| Beta-blocker | Bisoprolol 10 mg OD | HR >50 bpm, avoid if HR <50 or SBP <90 | Asthma, heart block |
| MRA | Spironolactone 25 mg OD | K+ <5.0 mmol/L at 1 week | K+ >5.0 mmol/L, eGFR <30 |
| SGLT2 inhibitor | Dapagliflozin 10 mg OD | eGFR >25 mL/min | T1DM, DKA risk |
Anticoagulation for AF (NICE NG196):
- CHA₂DS₂-VASc ≥2 (men) or ≥3 (women): Offer DOAC
- Apixaban 5 mg BD (2.5 mg BD if ≥2 of: age ≥80, weight ≤60 kg, Cr ≥133 μmol/L)
- Rivaroxaban 20 mg OD with food (15 mg if CrCl 30-49 mL/min)
- HAS-BLED score: Assesses bleeding risk but does NOT contraindicate anticoagulation if CHA₂DS₂-VASc indicates benefit
Evidence-Based Management: From Guidelines to Bedside
Complex Integration: Multimorbidity and Special Populations
The 78-year-old woman with HFrEF (LVEF 28%), atrial fibrillation (CHA₂DS₂-VASc 5), stage 3b CKD (eGFR 38 mL/min), and recent GI bleed exemplifies modern cardiology's complexity. She requires anticoagulation (apixaban 2.5 mg BD given age, weight, and renal function) despite bleeding history because stroke risk (8.5%/year) exceeds bleeding risk. Her HFrEF therapy demands careful uptitration: start ramipril 1.25 mg OD (half-dose due to CKD), monitor creatinine rise <30%, add bisoprolol 1.25 mg OD once stable, then spironolactone 12.5 mg OD (monitoring K+ weekly initially). management in diabetic patients requires aggressive risk factor modification: target HbA1c <53 mmol/mol, BP <130/80 mmHg, and LDL <1.8 mmol/L with high-intensity statin. in pregnancy mandates switching from DOACs (teratogenic) to low-molecular-weight heparin (enoxaparin 1 mg/kg BD). post-PCI requires dual antiplatelet therapy (aspirin 75 mg + ticagrelor 90 mg BD) for 12 months, with bleeding risk assessed using PRECISE-DAPT score.
Renal Impairment Drug Adjustments:
- eGFR 30-60: Reduce ramipril dose by 50%, avoid spironolactone if K+ >4.5
- eGFR <30: Avoid metformin, reduce DOAC doses, consider dialysis if symptomatic uraemia
- SGLT2 inhibitors: Continue if eGFR >25 (cardiovascular benefit persists)
| Complication | Incidence Post-MI | Prevention Strategy |
|---|---|---|
| Recurrent MI | 10% at 1 year | Dual antiplatelet therapy 12 months |
| Heart failure | 25% at 5 years | Early ACE-I + beta-blocker |
| Ventricular arrhythmia | 5% in first 48 hours | Correct electrolytes, consider ICD if LVEF <35% at 6 weeks |
| Stroke (AF post-MI) | 2-3%/year | Anticoagulation if CHA₂DS₂-VASc ≥2 |
⭐ Clinical Pearl: In triple therapy (DOAC + aspirin + P2Y12 inhibitor post-PCI in AF), limit duration to 1 week for stable CAD, 1 month for ACS, then switch to DOAC + single antiplatelet (usually clopidogrel 75 mg) to reduce bleeding risk
Complex Integration: Multimorbidity and Special Populations
High Yield Summary
Key Take-Aways:
- Hypertension diagnosis requires ABPM/HBPM confirmation (≥135/85 mmHg); stage 2 (≥160/100) warrants treatment regardless of age
- QRISK ≥10% triggers statin therapy (atorvastatin 20 mg); recalculate every 5 years
- STEMI demands immediate PCI (<90 minutes door-to-balloon); NSTEMI uses GRACE score for risk stratification
- HFrEF "four pillars": ACE-I/ARB + beta-blocker + MRA + SGLT2 inhibitor, uptitrated to target doses
- AF anticoagulation indicated if CHA₂DS₂-VASc ≥2 (men) or ≥3 (women); DOACs preferred over warfarin
- NT-proBNP >2000 pg/mL requires echo within 2 weeks; 400-2000 pg/mL within 6 weeks
- Dual antiplatelet therapy (aspirin + ticagrelor) for 12 months post-ACS/PCI
Essential Cardiology Numbers:
| Parameter | Threshold | Action |
|---|---|---|
| QRISK | ≥10% | Offer atorvastatin 20 mg |
| NT-proBNP | >2000 pg/mL | Urgent echo (2 weeks) |
| Troponin rise | >99th percentile | Diagnose MI; risk-stratify |
| LVEF | <40% | HFrEF: start four-pillar therapy |
| CHA₂DS₂-VASc | ≥2 (men) / ≥3 (women) | Anticoagulate |
| Aortic stenosis | Valve area <1.0 cm² | Consider AVR if symptomatic |
Key Principles:
- Ambulatory BP monitoring prevents overtreatment of white-coat hypertension (affects 10% of patients)
- High-sensitivity troponin at 0 and 3 hours achieves 98-99% sensitivity for ACS
- ACE-I/ARB creatinine rise <30% is acceptable; indicates haemodynamic effect, not nephrotoxicity
- HAS-BLED score informs bleeding risk but does NOT contraindicate anticoagulation if CHA₂DS₂-VASc indicates benefit
- SGLT2 inhibitors (dapagliflozin 10 mg) benefit HFrEF regardless of diabetes status; continue if eGFR >25
Quick Reference:
| Condition | First-Line Investigation | First-Line Treatment | Escalation Trigger |
|---|---|---|---|
| Hypertension | ABPM/HBPM | ACE-I (age <55) or CCB (age ≥55) | BP remains >140/90 on monotherapy |
| Stable angina | CT coronary angiography | Aspirin + statin + anti-anginal (GTN PRN) | Symptoms despite 2 anti-anginals |
| HFrEF | Echo + NT-proBNP | ACE-I + beta-blocker → add MRA + SGLT2i | Persistent NYHA III-IV despite therapy |
| AF | ECG + echo + TFTs | Rate/rhythm control + anticoagulation if indicated | Symptomatic despite rate control |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












