Common Infections

On this page
Recognising Common Infections: Foundations and Key Pathogens
A 45-year-old woman presents to her GP with a painful, red, swollen area on her lower leg that has developed over 48 hours. This scenario exemplifies the bread-and-butter of infectious diseases practice in the UK, where skin and soft tissue infections account for approximately 10% of hospital admissions. Understanding the epidemiology and microbiology of common infections is essential for appropriate empirical therapy and effective antimicrobial stewardship . Community-acquired infections differ fundamentally from healthcare-associated infections in their causative organisms and resistance patterns.
Key Infection Categories and Epidemiology:
-
Community-acquired infections: Most commonly caused by Streptococcus pyogenes (Group A Strep), Staphylococcus aureus (MSSA), and Escherichia coli
- Cellulitis incidence: 200 per 100,000 population annually in the UK
- Recurrence rate: 8-20% within 3 years
-
Healthcare-associated infections (HAIs): Defined as infections occurring ≥48 hours after hospital admission
- Incidence: 6.4% of inpatients in UK acute hospitals
- Key pathogens: MRSA, Pseudomonas aeruginosa, Clostridioides difficile
-
Antibiotic resistance patterns in the UK:
- MRSA prevalence in bloodstream infections: ~5% (down from 30% in 2006)
- E. coli resistance to fluoroquinolones: ~15-20%
- Carbapenemase-producing Enterobacterales (CPE): emerging threat, <1% but increasing
| Infection Type | Leading Pathogen | Second Most Common | Key Risk Factor |
|---|---|---|---|
| Cellulitis | Streptococcus pyogenes | Staphylococcus aureus | Lymphoedema, obesity |
| Surgical site infection | Staphylococcus aureus | Coagulase-negative staphylococci | Prolonged surgery >2h |
| Diabetic foot infection | Polymicrobial | S. aureus + anaerobes | Neuropathy, PVD |
| Hospital-acquired pneumonia | Pseudomonas aeruginosa | MRSA | Mechanical ventilation |
📌 Mnemonic for Cellulitis Risk Factors: "LOVED" - Lymphoedema, Obesity, Venous insufficiency, Eczema/dermatitis, Diabetes
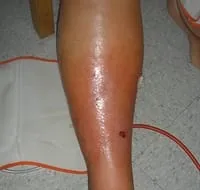
Recognising Common Infections: Foundations and Key Pathogens
2 - Pathophysiology and Clinical Presentations of Skin and Soft Tissue Infections
Understanding how bacteria breach the skin's protective barrier helps explain why certain patients develop severe infections while others remain unaffected. In cellulitis, Streptococcus pyogenes produces hyaluronidase and streptokinase, enzymes that break down connective tissue and allow rapid spread through tissue planes. The host inflammatory response-mediated by cytokines like IL-1 and TNF-α-causes the characteristic erythema, warmth, and oedema. This pathophysiological insight underpins why anti-inflammatory measures alone fail and why early antibiotic therapy targeting streptococci is critical in managing skin and soft tissue infections .
Key Pathophysiological Mechanisms:
-
Bacterial virulence factors:
- S. pyogenes: M protein (inhibits phagocytosis), exotoxins (superantigens causing toxic shock)
- S. aureus: Panton-Valentine leukocidin (PVL) toxin causes necrotising pneumonia and skin abscesses
- Clostridium perfringens: α-toxin (phospholipase) causes gas gangrene through myonecrosis
-
Host defence breakdown:
- Disrupted skin barrier (trauma, eczema, tinea pedis) allows bacterial entry
- Impaired lymphatic drainage (post-surgery, lymphoedema) reduces immune cell trafficking
- Neutrophil dysfunction (diabetes, immunosuppression) permits uncontrolled bacterial proliferation
Clinical Presentations by Depth:
-
Superficial infections (epidermis/dermis):
- Impetigo: honey-crusted lesions, highly contagious
- Erysipelas: raised, well-demarcated, bright red plaque with peau d'orange texture
-
Deep infections (subcutaneous tissue):
- Cellulitis: poorly demarcated erythema, systemic features (fever >38°C, tachycardia)
- Abscess: fluctuant, localised collection requiring drainage
2 — Pathophysiology and Clinical Presentations of Skin and Soft Tissue Infections
3 - Diagnostic Approach and NICE Guideline Application
A 68-year-old man with type 2 diabetes presents with a 3-day history of right leg pain, erythema extending from ankle to knee, and fever. His observations show temperature 38.7°C, heart rate 105 bpm, blood pressure 128/82 mmHg. NICE guideline NG141 recommends using the Eron classification to guide management decisions for cellulitis . This systematic approach, integrated with antimicrobial stewardship principles , ensures appropriate treatment intensity while minimising unnecessary hospital admissions.
Diagnostic Investigations:
-
Bedside tests:
- Mark cellulitis border with indelible pen: track progression/regression
- Swab only if purulent discharge present (culture yield <5% in non-purulent cellulitis)
- Capillary blood glucose: exclude hyperglycaemia
-
Laboratory investigations:
- FBC: WCC >15×10⁹/L suggests bacterial infection
- CRP: typically >50 mg/L in cellulitis; trend more useful than absolute value
- Blood cultures: indicated if systemically unwell (positive in <5% of cellulitis)
- Renal function: guide antibiotic dosing
-
Imaging (when diagnostic uncertainty):
- Ultrasound: differentiate cellulitis from DVT or abscess (sensitivity 98% for abscess)
- MRI: suspected necrotising fasciitis (gas in tissue planes, fascial enhancement)
| Eron Class | Systemic Features | Comorbidities | Management Setting | Antibiotic Route |
|---|---|---|---|---|
| I | None | None | Community | Oral |
| II | None | Present (diabetes, obesity) | Community | Oral |
| III | Present (fever, tachycardia) | ± comorbidities | Hospital | IV initially |
| IV | Sepsis or limb-threatening | Any | Hospital + surgical | IV + surgery |
3 — Diagnostic Approach and NICE Guideline Application
4 - Differential Diagnosis and Treatment Failure Analysis
Distinguishing cellulitis from its mimics prevents inappropriate antibiotic use-a cornerstone of antimicrobial stewardship . Up to 30% of suspected cellulitis cases are misdiagnosed, leading to unnecessary antibiotics and delayed appropriate treatment. Key differentiators include unilateral versus bilateral presentation, presence of systemic features, and specific clinical signs.
Critical Discriminators:
-
Cellulitis versus venous eczema/stasis dermatitis:
- Cellulitis: unilateral, acute onset (<72h), fever, elevated inflammatory markers
- Venous eczema: bilateral, chronic/subacute, no fever, normal CRP, haemosiderin deposition
-
Cellulitis versus DVT:
- Both cause unilateral leg swelling and pain
- DVT: calf tenderness, Homan's sign (unreliable), D-dimer >500 ng/mL
- Ultrasound Doppler definitive (sensitivity 97% for proximal DVT)
-
Treatment failure causes in skin and soft tissue infections :
- Incorrect diagnosis (most common)
- Inadequate source control (undrained abscess)
- Resistant organism (MRSA, β-lactamase producers)
- Inadequate dosing or poor tissue penetration
| Feature | Cellulitis | Venous Eczema | DVT | Necrotising Fasciitis |
|---|---|---|---|---|
| Onset | Acute (<3 days) | Chronic/subacute | Acute | Hyperacute (<24h) |
| Laterality | Unilateral | Usually bilateral | Unilateral | Unilateral |
| Pain severity | Moderate | Mild | Moderate | Severe (out of proportion) |
| Systemic features | Present | Absent | Absent | Severe (shock) |
| CRP | >50 mg/L | <10 mg/L | <20 mg/L | >150 mg/L |
🚩 Red Flag: Pain out of proportion to clinical findings + rapidly progressive erythema + systemic toxicity = necrotising fasciitis until proven otherwise. LRINEC score ≥6 suggests necrotising infection (sensitivity 68%, specificity 85%).
4 — Differential Diagnosis and Treatment Failure Analysis
5 - Evidence-Based Treatment Selection and De-escalation
NICE guideline NG141 recommends flucloxacillin as first-line empirical therapy for cellulitis, targeting the most common pathogens (streptococci and staphylococci). The choice reflects local antimicrobial resistance patterns and the principle of using narrow-spectrum agents when possible-central to antimicrobial stewardship . Treatment duration should be the minimum effective period, typically 5-7 days for uncomplicated cellulitis, with clinical response (defervescence, reduced erythema) guiding decisions rather than arbitrary completion of courses.
First-Line Empirical Therapy:
-
Cellulitis (non-purulent):
- Flucloxacillin 500mg-1g QDS PO (or 1-2g QDS IV if Class III/IV)
- Duration: 5-7 days (extend if slow response)
- Penicillin allergy: clarithromycin 500mg BD or doxycycline 200mg stat then 100mg OD
-
Cellulitis near eyes/nose (risk of MRSA):
- Add vancomycin 15-20mg/kg BD IV or teicoplanin 400mg OD IV
- Target vancomycin trough 10-15 mg/L
-
De-escalation principles:
- Switch IV to oral when afebrile >24h, able to take oral, improving clinically
- Bioavailability of flucloxacillin PO ~50%, so may need higher oral dose
- Stop antibiotics when clinical resolution achieved (not based on CRP normalisation)
| Clinical Scenario | First-Line Antibiotic | Dose | Duration | MRSA Cover Needed? |
|---|---|---|---|---|
| Uncomplicated cellulitis | Flucloxacillin | 500mg QDS PO | 5-7 days | No |
| Severe cellulitis (Class III) | Flucloxacillin | 1-2g QDS IV | Until afebrile 24h, then switch PO | No |
| Diabetic foot infection | Co-amoxiclav | 625mg TDS PO | 7 days | Consider if recent healthcare contact |
| Post-surgical wound | Flucloxacillin + gentamicin | 2g QDS IV + 5mg/kg OD IV | Review at 48h | Yes if high risk |
⭐ Clinical Pearl: If cellulitis not improving after 48h of flucloxacillin, consider: (1) Is it really cellulitis? (2) Is there an abscess needing drainage? (3) Is MRSA or Gram-negative cover needed? Avoid reflexive escalation without reassessing diagnosis.
5 — Evidence-Based Treatment Selection and De-escalation
6 - Complex Cases and Stewardship Interventions
A 72-year-old woman with recurrent cellulitis (fourth episode in 18 months) presents a stewardship challenge: does she need prophylactic antibiotics? NICE NG141 recommends prophylaxis only after ≥2 episodes in 12 months, using phenoxymethylpenicillin 500mg OD-BD for at least 6-12 months. This approach, integrating principles from antimicrobial stewardship and understanding of skin and soft tissue infections , balances infection prevention against antibiotic resistance risks.
Recurrent Cellulitis Management:
-
Identify and address predisposing factors:
- Treat tinea pedis (entry portal for bacteria)
- Manage lymphoedema (compression, skin care)
- Optimise diabetes control (HbA1c <53 mmol/mol)
- Weight reduction if obese (BMI >30)
-
Prophylactic antibiotic criteria (NICE NG141):
- ≥2 episodes within 12 months
- Phenoxymethylpenicillin 500mg OD-BD or erythromycin 250mg BD if penicillin-allergic
- Continue 6-12 months, then trial cessation
Stewardship Audit Metrics:
- Percentage of cellulitis patients receiving flucloxacillin first-line (target >80%)
- Median time to IV-to-oral switch (target <72h)
- Inappropriate antibiotic prescribing rate for cellulitis mimics (target <10%)
- Compliance with 5-7 day treatment duration (target >75%)
| Stewardship Intervention | Implementation Strategy | Expected Impact | Measurement |
|---|---|---|---|
| Clinical decision support | Electronic alert for cellulitis diagnosis suggesting flucloxacillin | Increase guideline compliance by 25% | Audit prescribing data |
| IV-to-oral switch protocol | Pharmacy-led review at 48-72h | Reduce IV antibiotic days by 30% | Total IV days per admission |
| Diagnostic stewardship | Mandatory CRP for suspected cellulitis | Reduce inappropriate antibiotics by 15% | Prescriptions for cellulitis mimics |
| Prophylaxis review | Annual assessment of ongoing need | Reduce unnecessary prophylaxis by 20% | Patients on prophylaxis >12 months |
6 — Complex Cases and Stewardship Interventions
High Yield Summary
Key Take-Aways:
- Cellulitis is primarily caused by Streptococcus pyogenes and Staphylococcus aureus; blood cultures positive in <5% of cases
- Eron classification guides management: Class I/II outpatient oral therapy, Class III/IV hospital admission with IV antibiotics
- Flucloxacillin 500mg-1g QDS for 5-7 days is first-line for uncomplicated cellulitis per NICE NG141
- Up to 30% of suspected cellulitis cases are mimics (venous eczema, DVT); misdiagnosis is the commonest cause of treatment failure
- Prophylaxis with phenoxymethylpenicillin 500mg OD-BD indicated after ≥2 episodes in 12 months
- De-escalate IV to oral when afebrile >24h and clinically improving; stop antibiotics at clinical resolution, not CRP normalisation
- LRINEC score ≥6 suggests necrotising fasciitis (sensitivity 68%); pain out of proportion to findings is critical red flag
Essential Common Infections Numbers:
| Parameter | Value | Clinical Significance |
|---|---|---|
| Cellulitis incidence | 200 per 100,000/year | Common presentation in primary and secondary care |
| CRP threshold | >50 mg/L | Supports bacterial cellulitis diagnosis |
| WCC in cellulitis | >15×10⁹/L | Suggests significant bacterial infection |
| Treatment duration | 5-7 days | Minimum effective period for uncomplicated cases |
| Recurrence rate | 8-20% within 3 years | Justifies prophylaxis consideration |
| MRSA bloodstream prevalence | ~5% | Low; routine MRSA cover not needed |
Key Principles:
- Antimicrobial stewardship begins with accurate diagnosis-treat the patient, not the CRP
- Narrow-spectrum antibiotics (flucloxacillin) preferred over broad-spectrum to minimise resistance
- Source control (abscess drainage) essential; antibiotics alone insufficient for collections
- IV-to-oral switch when clinically appropriate reduces costs, line complications, and hospital stay
- Address underlying risk factors (lymphoedema, tinea pedis) to prevent recurrence
Quick Reference:
| Clinical Question | Answer |
|---|---|
| First-line antibiotic for cellulitis? | Flucloxacillin 500mg-1g QDS PO |
| When to admit? | Eron Class III/IV (systemic features or limb-threatening) |
| When to add MRSA cover? | Periorbital/perinasal location, recent healthcare contact, known MRSA carrier |
| Treatment duration? | 5-7 days (uncomplicated); extend if slow response |
| Prophylaxis indication? | ≥2 episodes in 12 months |
| Red flag for necrotising infection? | Pain out of proportion + rapid progression + systemic toxicity |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




