Quick Overview
Pain assessment is fundamental to primary care consultations, affecting diagnosis, management, and patient outcomes. NICE NG193 emphasizes a biopsychosocial approach to chronic pain (>3 months duration), recognizing pain as an experience beyond tissue damage. Effective assessment distinguishes acute from chronic mechanisms and identifies when specialist referral is warranted.
Core Facts & Concepts
Pain Classification by Duration:
- Acute pain: <3 months, tissue damage-related, usually nociceptive
- Chronic primary pain: >3 months, biopsychosocial factors dominant, not better explained by another condition
- Chronic secondary pain: >3 months, underlying disease identifiable
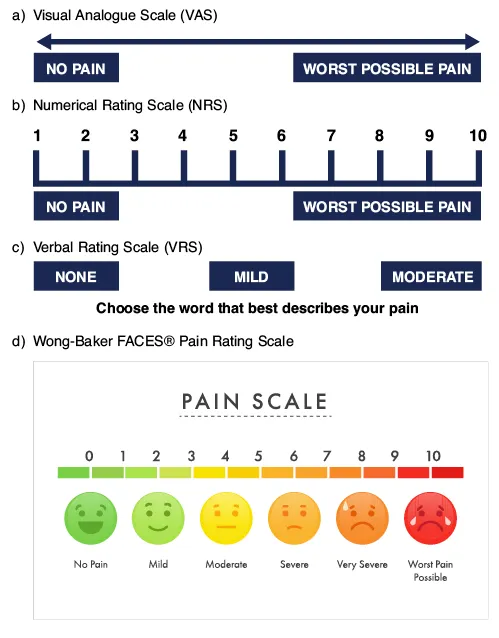
Assessment Tools (NICE NG193):
- Numeric Rating Scale (NRS): 0-10 score, simple but unidimensional
- Visual Analogue Scale (VAS): 0-100mm line, more sensitive to change
- Brief Pain Inventory (BPI): Assesses intensity AND functional impact (walking, work, sleep, mood)
- PEG Scale: Pain intensity, Enjoyment, General activity (3-item functional tool)
Biopsychosocial Model Components:
- Biological: Tissue pathology, nociceptive/neuropathic mechanisms
- Psychological: Catastrophizing, fear-avoidance, depression (40% comorbidity)
- Social: Work disability, family dynamics, cultural beliefs
📊 Key Numbers:
- Chronic pain affects 43% of UK population
- 30-50% develop chronic pain after surgery/trauma
- Functional impact more predictive than intensity for disability
Problem-Solving Approach
Structured Pain Assessment (6-Step):
-
Characterize pain: SOCRATES (Site, Onset, Character, Radiation, Associated symptoms, Timing, Exacerbating/relieving, Severity)
-
Quantify intensity: Use validated scale consistently (NRS 0-10 most practical)
-
Assess functional impact: "What can't you do because of pain?" (work, sleep, activities, relationships)
-
Screen psychological factors:
- Depression (PHQ-2): "Low mood/loss of interest for 2 weeks?"
- Anxiety (GAD-2): "Feeling anxious/unable to control worry?"
- Catastrophizing: "Do you fear pain means serious harm?"
-
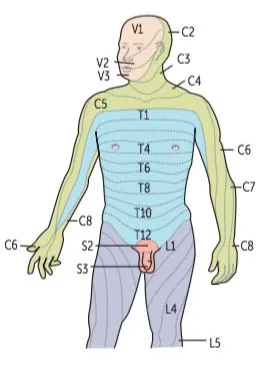
Identify pain mechanism:
- Nociceptive: Aching, localized, movement-related
- Neuropathic: Burning, shooting, numbness (DN4 questionnaire ≥4/10)
- Nociplastic: Widespread, disproportionate, central sensitization
-
Red flags for urgent referral: 🚩 Progressive neurological deficit 🚩 Suspected malignancy (unexplained weight loss, night pain) 🚩 Cauda equina symptoms (saddle anaesthesia, bladder/bowel dysfunction)
Analysis Framework
Acute vs Chronic Pain Mechanisms:
| Feature | Acute Pain | Chronic Primary Pain |
|---|---|---|
| Duration | <3 months | >3 months |
| Mechanism | Nociceptive (tissue damage) | Nociplastic (central sensitization) |
| Pathology | Identifiable cause | No proportionate structural cause |
| Prognosis | Self-limiting | Persistent, fluctuating |
| Management | Treat underlying cause | Biopsychosocial rehabilitation |
| Opioid role | Short-term may be appropriate | Avoid (NICE NG193) |
When to Refer to Specialist Pain Services (NICE NG193):
- Severe pain (NRS ≥7/10) unresponsive to primary care management
- Significant functional impairment despite 3-month trial of multidisciplinary approach
- Complex psychological comorbidity (PTSD, severe depression)
- Diagnostic uncertainty requiring specialist investigation
- Need for interventional procedures (nerve blocks, spinal cord stimulation)
Visual Aid
NICE NG193 Chronic Pain Management Principles:
| Component | Intervention | Avoid |
|---|---|---|
| First-line | Exercise programs, psychological therapy (CBT, ACT) | Opioids, gabapentinoids |
| Pharmacological | Antidepressants (duloxetine, amitriptyline) for specific conditions only | Paracetamol, NSAIDs long-term |
| Self-management | Pacing, goal-setting, sleep hygiene | Passive treatments (TENS, acupuncture) |
| Review | 8-12 weeks, focus on function not pain scores | Pain intensity as sole outcome |
Key Points Summary
✓ Chronic pain definition: >3 months duration; requires biopsychosocial assessment not just pain scores
✓ Functional assessment essential: Use BPI or PEG scale to measure impact on activities, work, sleep-more predictive than intensity alone
✓ NICE NG193 rejects: Opioids, gabapentinoids, paracetamol, NSAIDs for chronic primary pain management
✓ First-line chronic pain: Supervised exercise programs + psychological therapy (CBT/ACT); antidepressants only for specific neuropathic conditions
✓ Specialist referral triggers: Severe unresponsive pain (NRS ≥7), significant disability after 3-month primary care trial, red flags, complex comorbidity
✓ Pain mechanisms matter: Nociceptive (tissue damage) vs neuropathic (nerve injury, DN4 ≥4) vs nociplastic (central sensitization)-guide different management
✓ Psychological screening mandatory: 40% depression comorbidity; PHQ-2 and catastrophizing assessment change prognosis and treatment approach
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

