Screening & Prevention

On this page
Foundations of Screening & Prevention in Primary Care
A 52-year-old woman attends your surgery requesting a "full body MOT" after her friend was diagnosed with ovarian cancer. She's asymptomatic and has no family history of malignancy. This encounter exemplifies the daily challenge GPs face: distinguishing evidence-based screening from the "worried well" phenomenon. Understanding the principles underpinning enables you to counsel patients effectively about which interventions genuinely reduce morbidity and mortality, rather than simply detecting disease earlier without benefit.
Screening is the systematic application of a test to identify individuals at sufficient risk of a disorder to warrant further investigation or direct preventive action, among persons who have not sought medical attention on account of symptoms. This differs fundamentally from diagnostic testing in symptomatic patients.
-
Prevention hierarchy with specific examples:
- Primary prevention: Preventing disease occurrence (smoking cessation, statins for CVD risk >10%)
- Secondary prevention: Early detection in asymptomatic phase (cervical screening, BP monitoring)
- Tertiary prevention: Reducing complications of established disease (diabetic retinopathy screening)
-
UK National Screening Committee (UK NSC) framework criteria:
- Condition: important health problem with understood natural history
- Test: simple, safe, acceptable with agreed cut-off and quality assurance
- Treatment: effective intervention for identified disease
- Programme: evidence from RCTs of mortality/morbidity benefit, cost-effectiveness demonstrated
📌 Mnemonic: SCREEN = Simple test, Condition important, Reliable evidence, Early treatment effective, Economically sound, No harm outweighing benefit
| UK Screening Programme | Target Population | Screening Interval | Key Metric |
|---|---|---|---|
| AAA ultrasound | Men aged 65 | One-off | Aortic diameter ≥3.0 cm |
| Cervical (HPV primary) | Women 25-64 | 3-5 years | hrHPV status |
| Bowel (FIT) | Adults 60-74 | 2 years | Hb ≥10 μg/g faeces |
| Breast mammography | Women 50-71 | 3 years | Mammographic density |
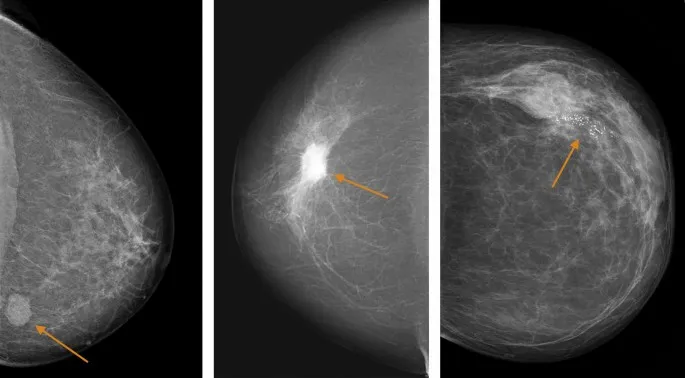
Foundations of Screening & Prevention in Primary Care
Wilson-Jungner Principles and Evidence Hierarchies
The 1968 Wilson-Jungner criteria remain the cornerstone of screening programme evaluation, though modern interpretation incorporates health economic analysis and ethical considerations around informed choice. When the UK NSC rejected prostate cancer screening using PSA despite its widespread use in other countries, this decision exemplified evidence-based restraint: the ERSPC trial showed an NNT of 781 men screened over 13 years to prevent one prostate cancer death, with significant overdiagnosis and treatment-related harms.
-
Wilson-Jungner criteria applied to :
- Natural history adequately understood (e.g., cervical intraepithelial neoplasia progression to cancer over 10-15 years)
- Recognisable latent/early symptomatic stage (detectable disease before symptoms emerge)
- Facilities for diagnosis and treatment available (infrastructure for colposcopy, treatment capacity)
- Agreed policy on whom to treat (clear referral thresholds, e.g., CIN2+ requires treatment)
-
Evidence hierarchy for screening interventions:
- Level 1: Systematic reviews/meta-analyses of RCTs showing mortality reduction (e.g., NLST for low-dose CT lung cancer screening)
- Level 2: Individual RCTs with disease-specific mortality endpoints
- Level 3: Cohort studies with surrogate outcomes (incidence of advanced disease)
- Insufficient: Case-control studies, ecological data, expert opinion alone
-
Population vs individual benefit paradox:
- Population benefit: AAA screening prevents 4-5 deaths per 10,000 men screened
- Individual risk: 96% of screened men derive no benefit, some experience anxiety from surveillance
- Prevention paradox: Large population benefit from small individual risk reduction
Wilson-Jungner Principles and Evidence Hierarchies
Implementing Opportunistic Screening and Brief Interventions
A 38-year-old man attends for an ankle sprain review. His notes show BMI 32, smoker of 15 cigarettes daily, and no BP recording for 3 years. This "opportunistic" consultation represents a critical window for . NICE PH16 emphasizes that brief advice delivered opportunistically in primary care increases smoking quit rates by 1-3% (NNT 50-120 for one additional quitter at 6 months), with minimal time investment (30-180 seconds).
-
Patient selection for opportunistic screening:
- Risk stratification tools: QRISK3 ≥10% warrants statin discussion; QDiabetes score identifies pre-diabetes candidates
- Systematic case-finding: BP check every 5 years (age 40+), or annually if 135-139/85-89 mmHg
- Targeted approaches: Alcohol screening (AUDIT-C) in patients with elevated GGT, depression, or recurrent injuries
-
Delivering brief interventions per :
- Very Brief Advice (VBA): 30 seconds using ASK-ADVISE-ACT framework
- Brief intervention: 5-10 minutes incorporating behavior change techniques
- Effectiveness: Alcohol brief interventions reduce consumption by 20g/week (95% CI 10-30g), NNT 8 for reducing hazardous drinking
⭐ Clinical Pearl: Frame screening as "routine health maintenance" rather than suspicion of disease. Say "We recommend BP checks every few years for everyone over 40" rather than "I'm concerned about your blood pressure."
- Opportunistic screening appropriate for:
- Hypertension (office BP, ABPM if ≥140/90 mmHg)
- Type 2 diabetes (HbA1c in high-risk groups: BMI >30, South Asian ethnicity, family history)
- Atrial fibrillation (manual pulse check age 65+, irregular rhythm → ECG)
- Depression (case-finding questions in chronic disease, postnatal period)
Implementing Opportunistic Screening and Brief Interventions
Analyzing Screening Test Performance and Biases
Understanding sensitivity, specificity, and predictive values transforms screening from a binary "positive/negative" exercise into a probabilistic clinical decision. The FIT test for bowel cancer screening (threshold ≥10 μg Hb/g faeces) demonstrates this complexity: sensitivity 79% for colorectal cancer, specificity 94%, but PPV only 5.9% due to low prevalence (0.8% in screening population). This means 94% of positive tests represent false positives requiring colonoscopy without finding cancer-an acceptable trade-off given the mortality benefit.
| Screening Test | Sensitivity | Specificity | PPV (Prevalence 1%) | NNT to Prevent 1 Death |
|---|---|---|---|---|
| Mammography (50-70y) | 75-85% | 95-97% | 10-15% | 377 (10-year screening) |
| Cervical cytology | 55-65% | 95-98% | 8-12% | 900 (lifetime screening) |
| FIT (bowel) | 79% | 94% | 5.9% | 377 (one screening round) |
| AAA ultrasound | 95% | 98% | 45% | 200 (one-off screening) |
-
Lead-time bias: Earlier detection without mortality benefit creates illusion of prolonged survival
- Example: Neuroblastoma screening detected tumors 18 months earlier but no reduction in mortality-many regressed spontaneously
- Critical distinction: 5-year survival from diagnosis ≠ mortality reduction from randomization
-
Length-time bias: Screening preferentially detects slow-growing cancers with better prognosis
- Aggressive cancers present symptomatically between screening rounds (interval cancers)
- Overestimates screening effectiveness if not accounted for in trial design
-
Overdiagnosis: Detection of disease that would never cause symptoms/death
- Estimated 19% of breast cancers detected by screening represent overdiagnosis
- Thyroid cancer screening in South Korea increased incidence 15-fold without mortality reduction
-
Number Needed to Harm (NNH) considerations per :
- Bowel screening: NNH 14 for serious colonoscopy complication (perforation, bleeding)
- Cervical screening: 1 in 1,000 women experience severe anxiety requiring psychological support
Analyzing Screening Test Performance and Biases
Balancing Harms and Benefits in Shared Decision-Making
A 68-year-old woman with COPD (FEV1 55% predicted) receives a positive FIT result. Her frailty score is 4/9, she lives alone, and expresses fear about colonoscopy. This scenario demands sophisticated risk-benefit analysis incorporating patient values. emphasizes that informed choice requires presenting absolute risks in natural frequencies (e.g., "8 in 1,000 women screened will avoid dying from bowel cancer") rather than relative risk reductions that inflate perceived benefit.
-
Risk communication frameworks:
- Absolute risk: "Your 10-year CVD risk is 18%-that's 18 in 100 people like you having a heart attack or stroke"
- NNT framing: "We'd need to treat 28 people like you for 5 years to prevent one stroke-the other 27 wouldn't benefit"
- Visual aids: Icon arrays showing 100 faces with outcomes highlighted
-
Harms requiring explicit discussion:
- Psychological: Anxiety from false positives (30-50% experience significant worry)
- Physical: Procedural complications (colonoscopy perforation 1 in 1,000)
- Opportunity cost: Resources diverted from symptomatic patients
- Overtreatment: DCIS treatment (surgery/radiotherapy) for lesions that may never progress
-
Shared decision-making tools:
- Decision aids (e.g., NHS bowel screening leaflet with quantified outcomes)
- Option grids comparing screening vs no screening with probabilities
- Teach-back method: "Can you tell me in your own words what we've discussed?"
🚩 Red Flag: Never coerce screening participation. Document informed refusal: "Patient declines bowel screening after discussion of benefits/harms. Understands can re-access service. Will revisit at annual review."
Balancing Harms and Benefits in Shared Decision-Making
Integrating Screening into Practice Systems and QOF
Modern general practice requires systematic approaches to prevention that don't rely on clinician memory. A practice with 8,000 patients will have approximately 450 patients eligible for diabetic retinopathy screening, 320 requiring cervical screening recall, and 80 men due AAA screening annually. Without robust call-recall systems integrated with and , vulnerable patients-precisely those at highest risk-are systematically missed.
-
Practice-level strategies:
- Population health management: Stratify practice population by risk (e.g., QRISK3 ≥20% for intensive CVD prevention)
- Automated recall systems: Template-driven prompts for BP checks, smoking status updates (annual QOF requirement)
- Care navigation: Healthcare assistants deliver NHS Health Checks (age 40-74, 5-yearly), freeing GP capacity
-
QOF integration (2024/25 indicators):
- CVD-PP001: 80% of patients with hypertension have BP ≤140/90 mmHg (or personalised target)
- DM007: 70% of diabetic patients achieve HbA1c ≤58 mmol/mol
- SMOK002: Smoking status recorded annually for all patients aged 15+
-
Multi-morbidity approaches:
- Prioritize interventions with multiple benefits (e.g., metformin for pre-diabetes + NAFLD + PCOS)
- Avoid screening cascade in limited life expectancy (<5 years)-bowel screening unlikely to benefit if severe heart failure
- De-prescribing: Stop statins if frailty score >6 and patient preference favors quality over quantity
Integrating Screening into Practice Systems and QOF
High Yield Summary
Key Take-Aways:
- Screening requires RCT evidence of mortality/morbidity reduction, not just earlier detection-lead-time bias creates survival illusion
- Wilson-Jungner criteria remain fundamental: condition important, test acceptable, treatment effective, programme cost-effective
- PPV depends on prevalence-low prevalence means most positive screening tests are false positives requiring further investigation
- NNT for screening is large (200-900) because most screened individuals don't benefit; harms (overdiagnosis, false positives) affect many more
- Opportunistic interventions (VBA for smoking, AUDIT-C for alcohol) have NNT 8-120 with minimal time investment
- Shared decision-making requires absolute risks in natural frequencies, not relative risk reductions
- Practice systems (automated recall, risk stratification) prevent vulnerable populations being systematically missed
Essential Screening & Prevention Numbers:
| Metric | Formula/Threshold | Clinical Application |
|---|---|---|
| Sensitivity | TP/(TP+FN) | Proportion with disease correctly identified |
| Specificity | TN/(TN+FP) | Proportion without disease correctly identified |
| PPV | TP/(TP+FP) | Probability disease present if test positive |
| NNT | 1/ARR | Number needed to screen to prevent 1 event |
| CVD risk threshold | QRISK3 ≥10% | Offer statin (atorvastatin 20 mg) |
| Hypertension threshold | ≥140/90 mmHg office | Confirm with ABPM/HBPM before treatment |
Key Principles/Pearls:
- Frame screening as "routine health maintenance" to reduce patient anxiety about disease suspicion
- Document informed refusal explicitly-patients can decline screening after understanding benefits/harms
- Avoid screening cascade in limited life expectancy (<5 years)-focus on symptom control and quality
- FIT-positive patients require colonoscopy within 2 weeks (2-week-wait pathway) even if low PPV
- Overdiagnosis (detecting disease never causing harm) affects 19% of screen-detected breast cancers
Quick Reference:
| Screening Programme | Age Range | Interval | Positive Threshold |
|---|---|---|---|
| AAA ultrasound | Men 65 | One-off | ≥3.0 cm diameter |
| Breast mammography | Women 50-71 | 3 years | Suspicious lesion |
| Cervical (HPV) | Women 25-64 | 3-5 years | hrHPV positive |
| Bowel FIT | Adults 60-74 | 2 years | ≥10 μg Hb/g faeces |
| Diabetic retinopathy | All diabetics | Annual | Any retinopathy |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




