Growth, Development & Safeguarding

On this page
Foundations of Child Assessment: Growth, Development & Safeguarding
A 15-month-old boy attends for routine review. His weight has dropped from the 50th to the 9th centile over 6 months, and his mother reports he's "fussy with food." During examination, you notice multiple bruises on his shins and a healing burn on his forearm. This scenario encapsulates the integrated approach required in child health: recognizing normal developmental variants, identifying concerning growth patterns , and maintaining vigilance for safeguarding concerns . Understanding these foundations is essential for any clinician working with children.
Essential Growth Parameters:
- Weight: Most sensitive indicator of acute nutritional status
- Birth weight doubles by 5 months, triples by 12 months
- Weight faltering: drop across ≥2 centile spaces over 3-6 months
- Length/Height: Reflects chronic nutritional status and genetic potential
- Average birth length: 50cm; increases by 25cm in first year
- Mid-parental height calculation: [(maternal height + paternal height) ± 13cm] / 2 (add 13cm for boys, subtract for girls)
- Head circumference: Critical marker of brain growth
- Average birth: 35cm; increases by 12cm in first year
- Measure until age 2 years routinely; beyond if concerns
| Parameter | Birth | 6 months | 12 months | 2 years |
|---|---|---|---|---|
| Weight (kg) | 3.5 | 7.5 | 10 | 12.5 |
| Length (cm) | 50 | 67 | 75 | 87 |
| Head circumference (cm) | 35 | 43 | 47 | 49 |
Developmental Milestones:
- Gross motor: Sitting unsupported by 9 months, walking independently by 18 months
- Fine motor and vision: Pincer grip by 12 months, tower of 3 cubes by 18 months
- Speech and hearing: 6 words by 18 months, 2-word phrases by 2 years
- Social and emotional: Stranger anxiety by 8 months, symbolic play by 2 years
📌 Mnemonic - SOCS: Sit 6 months, Out walking 12 months, Climb stairs 18 months, Sentences 2 years
Safeguarding Terminology:
- Child abuse: Physical, emotional, sexual, neglect (NICE NG76 categories)
- Significant harm: Threshold for statutory intervention under Children Act 1989
- Child in need: Requires additional support but below harm threshold
- Child protection plan: Multi-agency framework when child at risk of significant harm

Foundations of Child Assessment: Growth, Development & Safeguarding
2 - Pathophysiology of Growth Disorders and Safeguarding Impact
Growth is regulated by complex interactions between genetic programming, nutritional intake, hormonal axes (particularly growth hormone-IGF-1), and psychosocial environment. When a child experiences chronic stress from abuse or neglect , cortisol hypersecretion suppresses growth hormone secretion, leading to psychosocial short stature. Similarly, inadequate nutrition-whether from poverty, parental mental health issues, or deliberate withholding-disrupts the anabolic processes essential for normal growth . Understanding these mechanisms helps clinicians recognize when growth faltering signals underlying safeguarding concerns rather than organic pathology.
Growth Hormone-IGF-1 Axis:
- Growth hormone (GH) secreted in pulsatile fashion from anterior pituitary
- Stimulates hepatic IGF-1 production, which mediates skeletal and soft tissue growth
- Chronic stress → elevated cortisol → suppressed GH secretion → reduced IGF-1
- Malnutrition → reduced IGF-1 synthesis despite adequate GH
Neurodevelopmental Impact of Adversity:
- Toxic stress disrupts developing neural architecture
- Hippocampal volume reduction affects memory and learning
- Prefrontal cortex changes impair executive function
- Chronic activation of stress response systems → lifelong health consequences
| Mechanism | Physiological Effect | Clinical Manifestation |
|---|---|---|
| Cortisol excess | GH suppression | Reduced height velocity |
| Malnutrition | Reduced IGF-1 synthesis | Weight faltering, muscle wasting |
| Chronic stress | Hippocampal atrophy | Developmental delay, learning difficulties |
| Neglect | Reduced stimulation | Speech/language delay, attachment disorders |
2 — Pathophysiology of Growth Disorders and Safeguarding Impact
3 - Clinical Assessment: Integrating Growth Monitoring and Safeguarding
A 3-year-old girl presents with recurrent "accidents." Her weight is on the 2nd centile despite mid-parental height suggesting 50th centile. She avoids eye contact and doesn't engage in play. You notice finger-shaped bruises on her upper arms. This scenario demands systematic assessment: plotting growth trends, conducting age-appropriate developmental screening, and recognizing injury patterns inconsistent with the history . NICE NG76 emphasizes that safeguarding is everyone's responsibility-unexplained growth faltering warrants exploration of the home environment .
Growth Chart Interpretation:
- Plot all measurements on appropriate UK-WHO charts (0-4 years) or UK90 (4-18 years)
- Calculate centile position and assess trajectory over time
- Red flags: Crossing ≥2 centile spaces, height/weight discordance, head circumference concerns
- Consider corrected age for prematurity until age 2 years
Developmental Screening Tools:
- Ages and Stages Questionnaire (ASQ-3): Parent-completed, validated for 2-66 months
- Schedule of Growing Skills II (SOGS-II): Clinician-administered, comprehensive assessment
- Strengths and Difficulties Questionnaire (SDQ): Behavioral screening for 3-17 years
🚩 Red Flag: Any developmental regression or loss of previously acquired skills requires urgent investigation
Safeguarding Assessment Framework:
- History: Detailed account from child (if verbal), parent, and any witnesses
- Document verbatim in quotation marks
- Note delays in seeking care, changing explanations
- Examination: Full body examination in good lighting
- Document all injuries: size, shape, color, location (body map)
- Photograph with consent (or without if child protection concern)
- Investigations: Guided by clinical findings and differential diagnosis
- Skeletal survey if <2 years with suspected physical abuse
- Bleeding screen if unexplained bruising
3 — Clinical Assessment: Integrating Growth Monitoring and Safeguarding
4 - Differential Diagnosis: Organic Versus Non-Organic Growth Faltering
Distinguishing organic causes of growth faltering from neglect or abuse requires careful analysis. Organic conditions typically present with specific clinical features: coeliac disease with diarrhea and abdominal distension, congenital heart disease with feeding difficulties and respiratory symptoms, or endocrine disorders with characteristic growth patterns . In contrast, non-organic failure to thrive often shows dramatic catch-up growth when adequate nutrition is provided in hospital, and may coexist with other safeguarding indicators . The challenge lies in recognizing that organic and safeguarding issues can coexist-a child with genuine medical needs may also experience neglect.
Key Discriminating Features:
| Feature | Organic Cause | Non-Organic (Neglect) |
|---|---|---|
| Growth pattern | Proportionate short stature or specific organ involvement | Weight affected before height |
| Hospital feeding | Limited catch-up | Rapid catch-up growth (>1g/kg/day) |
| Parental interaction | Appropriate concern | Disengaged, inconsistent attendance |
| Associated features | Specific symptoms (diarrhea, dyspnea) | Multiple missed appointments, poor hygiene |
| Development | May be delayed if chronic illness | Often global delay with social/emotional impact |
Common Organic Causes:
- Gastrointestinal: Coeliac disease (anti-TTG >10x upper limit), cow's milk protein allergy, chronic constipation
- Cardiac: Congenital heart disease (increased metabolic demands)
- Endocrine: Hypothyroidism (TSH >10 mU/L), growth hormone deficiency (height velocity <4cm/year)
- Renal: Chronic kidney disease (eGFR <60 mL/min/1.73m²)
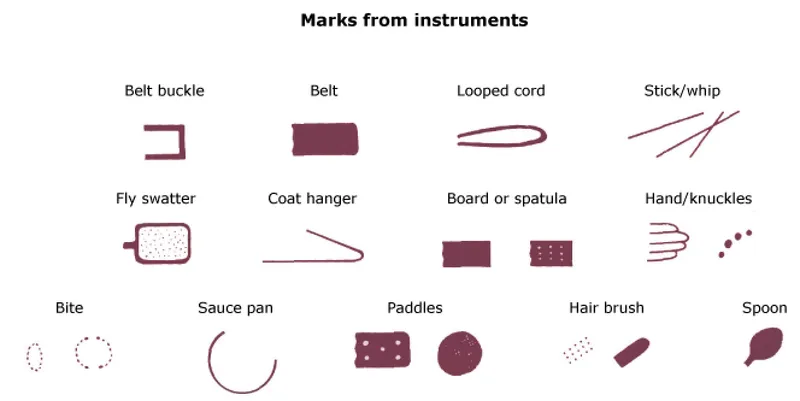
Concerning Injury Patterns:
- High specificity for abuse: Bruising in non-mobile infants, patterned injuries (hand/implement marks), injuries to ears/neck/genitals
- Burns: Clear demarcation lines suggest immersion; cigarette burns are circular and uniform
- Fractures: Metaphyseal corner fractures, posterior rib fractures, multiple fractures at different stages
⭐ Clinical Pearl: The younger the child and the more severe/unusual the injury, the higher the index of suspicion for non-accidental injury.
4 — Differential Diagnosis: Organic Versus Non-Organic Growth Faltering
5 - Clinical Decision-Making: When to Refer and Escalate
A 10-month-old with weight drop from 75th to 25th centile over 3 months requires systematic evaluation. NICE NG143 recommends considering safeguarding referral if growth faltering is unexplained after initial assessment or if there are additional concerns about parenting capacity . Simultaneously, investigate organic causes: coeliac serology, thyroid function, and consider dietitian input for feeding assessment . The decision to escalate depends on multiple factors: severity of growth faltering, presence of additional safeguarding indicators, parental engagement, and response to initial interventions.
Growth Faltering Referral Thresholds:
- Urgent pediatric assessment: Weight loss >5% in infants, crossing ≥3 centile spaces, head circumference concerns
- Dietitian referral: All cases of confirmed growth faltering
- Safeguarding referral: Unexplained faltering + parental non-engagement, coexisting neglect indicators, or deliberate withholding of food
Safeguarding Escalation Framework:
- Level 1 (Universal services): Health visitor support, parenting programs
- Level 2 (Early help): Multi-agency assessment, family support worker
- Level 3 (Child in need): Social services involvement, coordinated support plan
- Level 4 (Child protection): Immediate risk of significant harm, strategy discussion, Section 47 investigation
| Concern Level | Action | Timeframe |
|---|---|---|
| Mild growth faltering, engaged parents | Monitor, dietitian input | Review 2-4 weeks |
| Moderate faltering, some concerns | Early help assessment | Within 1 week |
| Severe faltering or abuse suspicion | Safeguarding referral | Same day |
| Immediate risk | Emergency pediatric admission | Immediate |
🚩 Red Flag: Never delay safeguarding referral to complete organic investigations-both pathways can proceed simultaneously.
5 — Clinical Decision-Making: When to Refer and Escalate
6 - Holistic Management: Optimizing Growth and Ensuring Safety
Managing a child with growth concerns and potential safeguarding issues requires coordinated multi-agency working. A 2-year-old with faltering growth due to parental mental health difficulties needs nutritional rehabilitation, developmental support, and family interventions addressing the underlying stressors . The care plan must balance supporting the family with ensuring child safety . Recent evidence emphasizes the importance of trauma-informed approaches that recognize adverse childhood experiences while maintaining clear boundaries about acceptable parenting standards.
Nutritional Rehabilitation:
- Energy requirements: 1.5-2x estimated average requirement for catch-up growth
- High-calorie foods: Fortified milk (providing 100 kcal/100ml), calorie-dense snacks
- Supplementation: Consider multivitamin, vitamin D (400 IU daily), iron if deficient
- Monitoring: Weekly weights initially, then fortnightly until established growth trajectory
Developmental Support:
- Speech and language therapy: If language delay identified
- Occupational therapy: For fine motor or sensory concerns
- Educational psychology: If learning difficulties or behavioral issues
- Attachment-based interventions: Video interaction guidance, Theraplay
Family Support Interventions:
- Address parental mental health, substance misuse, domestic abuse
- Practical support: foodbank referrals, housing advocacy, debt advice
- Parenting programs: evidence-based interventions (e.g., Triple P, Incredible Years)
| Intervention | Target | Expected Outcome |
|---|---|---|
| Dietitian-led feeding plan | Nutritional intake | Weight gain >20g/day (infants) |
| Health visitor home visits | Feeding observation, parent support | Improved feeding practices |
| Family support worker | Practical assistance | Reduced family stressors |
| Child protection plan | Safety monitoring | Risk reduction, clear contingency plans |
6 — Holistic Management: Optimizing Growth and Ensuring Safety
High Yield Summary
Key Take-Aways:
- Growth faltering is defined as crossing ≥2 centile spaces over 3-6 months; always consider both organic causes and safeguarding concerns
- Developmental milestones: sitting 6 months, walking 12 months, 6 words by 18 months, 2-word phrases by 2 years-regression is always concerning
- High-specificity injury patterns for abuse include bruising in non-mobile infants, metaphyseal fractures, posterior rib fractures, and patterned injuries
- NICE NG76 emphasizes safeguarding is everyone's responsibility-unexplained growth faltering warrants exploration of home environment
- Rapid catch-up growth (>1g/kg/day) when adequate nutrition provided suggests non-organic cause
- Multi-agency working is essential: never delay safeguarding referral to complete organic investigations
- Mid-parental height calculation helps identify children growing below genetic potential: [(maternal + paternal height) ± 13cm] / 2
Essential Growth, Development & Safeguarding Numbers:
| Parameter | Critical Value | Clinical Significance |
|---|---|---|
| Weight faltering | ≥2 centile spaces drop | Requires investigation |
| Birth weight milestones | Double by 5 months, triple by 12 months | Expected growth trajectory |
| Height velocity | <4 cm/year after age 3 | Suggests growth hormone deficiency |
| Developmental red flags | No sitting by 9 months, no walking by 18 months | Requires assessment |
| Safeguarding referral | Same day if immediate risk | Mandatory timeframe |
| Catch-up growth | >1 g/kg/day (infants) | Suggests adequate nutrition provided |
Key Principles/Pearls:
- Always plot growth on appropriate centile charts and assess trajectory over time-single measurements are less informative than trends
- The younger the child and the more unusual the injury location (ears, neck, genitals), the higher the suspicion for non-accidental injury
- Organic and non-organic causes can coexist-a child with genuine medical needs may also experience neglect
- Document safeguarding concerns meticulously: verbatim quotes, body maps for injuries, and contemporaneous notes are crucial for child protection proceedings
- Trauma-informed practice recognizes adverse childhood experiences while maintaining clear standards for child safety
Quick Reference:
| Assessment Tool | Age Range | Purpose |
|---|---|---|
| UK-WHO growth charts | 0-4 years | Weight, length, head circumference |
| ASQ-3 | 2-66 months | Developmental screening |
| SDQ | 3-17 years | Behavioral/emotional screening |
| Skeletal survey | <2 years | Suspected physical abuse investigation |
High Yield Summary
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




