Chronic Paediatric Conditions

On this page
Epidemiology and Core Definitions: Understanding the Burden
A 7-year-old girl presents with polyuria and weight loss; across the corridor, a 5-year-old boy has just experienced his second unprovoked seizure. These scenarios represent two of the most prevalent chronic conditions in paediatric medicine. affects approximately 215,000 children under 15 years globally, with UK incidence rising at 3-4% annually. has even greater reach, affecting 1 in 200 children, making it the most common serious neurological condition in paediatrics. Understanding their epidemiology shapes service provision, family support, and long-term outcome planning.
-
Type 1 Diabetes (T1D): Autoimmune destruction of pancreatic β-cells leading to absolute insulin deficiency
- UK incidence: 24.5 per 100,000 children annually
- Peak presentation ages: 4-6 years and 10-14 years
- Accounts for >95% of childhood diabetes cases
- Male:female ratio approximately 1:1
-
Epilepsy: Recurrent tendency to unprovoked seizures (≥2 unprovoked seizures >24 hours apart, or 1 seizure with high recurrence risk)
- UK prevalence: 5-10 per 1,000 children
- 70% diagnosed before age 20 years
- Idiopathic epilepsy accounts for 60-65% of cases
- Mortality rate: 1.2 per 1,000 person-years (general population: 0.1)
| Parameter | Type 1 Diabetes | Epilepsy |
|---|---|---|
| UK Prevalence | 2 per 1,000 children | 5-10 per 1,000 children |
| Annual Incidence | 24.5 per 100,000 | 60 per 100,000 |
| Median Age at Diagnosis | 10-14 years | 5-6 years |
| Male:Female Ratio | 1:1 | 1.2:1 |
📌 Mnemonic for T1D Presentation: The 4 T's - Toilet (polyuria), Thirsy (polydipsia), Tired (lethargy), Thinner (weight loss)
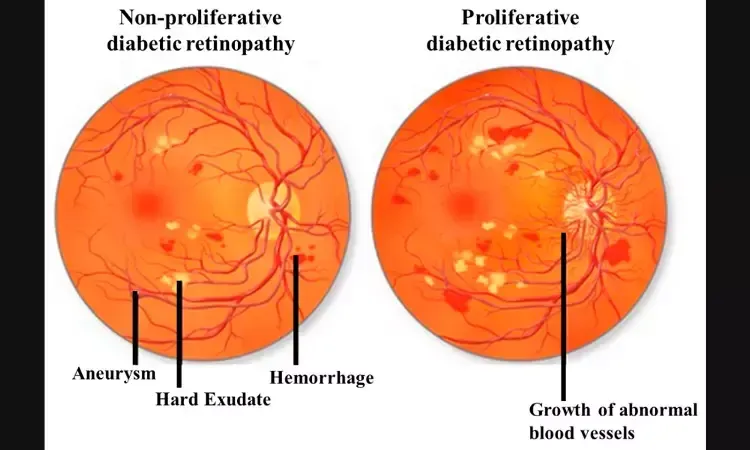
Epidemiology and Core Definitions: Understanding the Burden
Pathophysiological Mechanisms: From Molecular to Clinical
The pathogenesis of involves genetic susceptibility (HLA-DR3/DR4 haplotypes confer 50% risk), environmental triggers (viral infections, dietary factors), and immune dysregulation leading to insulitis. β-cell destruction occurs over months to years, with clinical presentation when 80-90% are destroyed. In contrast, represents diverse mechanisms: ion channelopathies (SCN1A mutations in Dravet syndrome), structural abnormalities (cortical dysplasia), or acquired insults (hypoxic-ischemic injury). The final common pathway is neuronal hyperexcitability from imbalance between excitatory (glutamate) and inhibitory (GABA) neurotransmission.
-
T1D Pathophysiology:
- Autoantibodies: GAD, IA-2, ZnT8 (present in 85-90% at diagnosis)
- Progressive β-cell loss → impaired first-phase insulin response → postprandial hyperglycemia
- Absolute insulin deficiency → lipolysis → ketogenesis → DKA risk
- Counter-regulatory hormone excess (glucagon, cortisol, catecholamines) exacerbates hyperglycemia
-
Epilepsy Pathophysiology:
- Genetic: Ion channel mutations (Na⁺, K⁺, Ca²⁺ channels) alter neuronal excitability
- Structural: Hippocampal sclerosis, focal cortical dysplasia create epileptogenic foci
- Metabolic: Glucose transporter defects (GLUT1 deficiency) impair neuronal energy
- Acquired: Febrile seizures, head trauma, CNS infections trigger epileptogenesis
| Mechanism | Type 1 Diabetes | Epilepsy |
|---|---|---|
| Primary Defect | Autoimmune β-cell destruction | Neuronal hyperexcitability |
| Key Molecules | Insulin, C-peptide, autoantibodies | Glutamate, GABA, ion channels |
| Onset Pattern | Subacute (weeks-months) | Variable (acute to chronic) |
| Reversibility | Irreversible | Potentially reversible (60-70%) |

Pathophysiological Mechanisms: From Molecular to Clinical
Clinical Application: Diagnosis and Initial Management
A 9-year-old presents with 3-week history of excessive thirst, nocturia, and 4kg weight loss. Random glucose is 18.2 mmol/L; venous pH 7.32, ketones 3.8 mmol/L. NICE NG18 guides immediate management: confirm diabetes (HbA1c ≥48 mmol/mol or fasting glucose ≥7.0 mmol/L), assess for DKA (pH <7.3 or bicarbonate <15 mmol/L), and initiate insulin therapy within 24 hours. Meanwhile, a 6-year-old experiences a 90-second episode of staring, unresponsiveness, and lip-smacking. Witnessed second episode 3 weeks later. NICE NG217 recommends specialist assessment within 2 weeks for first unprovoked seizure, EEG within 4 weeks, and neuroimaging (MRI preferred) to identify structural causes.
-
T1D Diagnostic Criteria (WHO):
- Symptoms + random glucose ≥11.1 mmol/L, OR
- Fasting glucose ≥7.0 mmol/L (no caloric intake 8 hours), OR
- HbA1c ≥48 mmol/mol (≥6.5%)
- C-peptide <200 pmol/L confirms insulin deficiency
-
DKA Assessment (NICE NG18):
- Hyperglycemia (glucose >11 mmol/L)
- Ketonemia (β-hydroxybutyrate >3.0 mmol/L) or ketonuria (2+ on dipstick)
- Acidosis (pH <7.3 or bicarbonate <15 mmol/L)
- Severity: Mild (pH 7.2-7.29), Moderate (pH 7.1-7.19), Severe (pH <7.1)
-
Epilepsy Diagnosis (NICE NG217):
- Clinical: ≥2 unprovoked seizures >24 hours apart, OR
- 1 seizure + EEG showing epileptiform activity + structural abnormality
- EEG sensitivity: 50% after first seizure, 80-90% after multiple recordings
- MRI brain: identifies structural causes in 15-20% (cortical dysplasia, tumors, vascular malformations)
| Investigation | Type 1 Diabetes | Epilepsy |
|---|---|---|
| First-line | Random/fasting glucose, HbA1c | EEG (awake and sleep) |
| Confirmatory | C-peptide, autoantibodies | Video-EEG telemetry |
| Imaging | Not routine (consider if atypical) | MRI brain (all first seizures) |
| Timeframe | Same-day assessment | Specialist within 2 weeks |
🚩 Red Flag: In suspected DKA, never give insulin bolus without IV fluids first-risks cerebral edema from rapid osmotic shifts.

Comparative Analysis: Distinguishing Features and Pitfalls
Both conditions present diagnostic challenges. New-onset T1D can mimic urinary tract infection (polyuria), eating disorders (weight loss), or behavioral problems (irritability). Key discriminator: random glucose >11.1 mmol/L is diagnostic; urinalysis showing glycosuria without infection confirms suspicion. Epilepsy diagnosis requires distinguishing seizures from syncope (gradual vs. sudden onset, prolonged vs. brief loss of consciousness), breath-holding spells (cyanosis, triggered by distress), or parasomnias (occur from sleep, stereotyped movements). EEG epileptiform discharges (sensitivity 50% first recording, 80-90% with repeat sleep-deprived studies) provide objective evidence, but normal EEG doesn't exclude epilepsy-diagnosis remains clinical.
-
T1D Differential Diagnosis:
- Type 2 diabetes: Older age, obesity, acanthosis nigricans, family history
- Monogenic diabetes (MODY): Family history, non-obese, GAD antibody-negative
- Stress hyperglycemia: Resolves with illness resolution, HbA1c normal
- Diabetes insipidus: Polyuria without hyperglycemia, low urine osmolality
-
Epilepsy Differential Diagnosis:
- Syncope: Prodrome (lightheadedness), pallor, brief duration (<30 seconds), rapid recovery
- Psychogenic non-epileptic seizures: Eyes closed during event, prolonged duration, no postictal confusion
- Migraine with aura: Visual symptoms, gradual spread, followed by headache
- Parasomnias: Occur exclusively from sleep, no daytime events
| Feature | Seizure | Syncope |
|---|---|---|
| Onset | Sudden, no warning | Gradual, prodrome common |
| Duration | 1-3 minutes | <30 seconds |
| Color Change | Cyanosis possible | Pallor typical |
| Postictal State | Confusion 5-15 minutes | Rapid full recovery |
| Injury Risk | High (falls, tongue-biting) | Lower (gradual collapse) |
⭐ Clinical Pearl: C-peptide <200 pmol/L distinguishes T1D from T2D (preserved in T2D). In epilepsy, prolactin rises 10-20 minutes post-seizure (not in psychogenic seizures), but short half-life limits clinical utility.
Evidence-Based Management: Treatment Protocols and Monitoring
NICE NG18 mandates multiple daily injection (MDI) regimen or continuous subcutaneous insulin infusion (CSII/pump) for all children with T1D. Initial total daily dose: 0.5-1.0 units/kg/day, split 50% basal (once-daily long-acting analog: glargine, detemir, degludec) and 50% bolus (rapid-acting analog: lispro, aspart, glulisine) with meals using carbohydrate counting (1 unit per 10-15g carbohydrate). Target HbA1c ≤48 mmol/mol without disabling hypoglycemia. Continuous glucose monitoring (CGM) or flash glucose monitoring recommended for all. management follows NICE NG217: first-line monotherapy based on seizure type-sodium valproate for generalized seizures (contraindicated in females of childbearing potential due to teratogenicity), carbamazepine or lamotrigine for focal seizures. Start low, titrate slowly to minimize adverse effects. Target: seizure freedom with minimal side effects. Aim for monotherapy; if ineffective after 2 appropriate trials, refer to tertiary epilepsy center.
-
T1D Insulin Regimens:
- MDI: Basal-bolus (e.g., glargine 0.3 units/kg once daily + aspart 0.15 units/kg per meal)
- CSII: Basal rate 0.4-0.6 units/kg/day, bolus calculator based on carb ratio and correction factor
- Sick day rules: Continue basal, increase monitoring, check ketones if glucose >14 mmol/L
-
Epilepsy First-Line Medications (NICE NG217):
- Focal seizures: Carbamazepine (10-20 mg/kg/day divided BID), lamotrigine (1-5 mg/kg/day)
- Generalized tonic-clonic: Sodium valproate (20-30 mg/kg/day divided BID), lamotrigine
- Absence seizures: Ethosuximide (20 mg/kg/day divided BID), sodium valproate
- Myoclonic seizures: Sodium valproate, levetiracetam (20-40 mg/kg/day divided BID)
| Medication | Starting Dose | Target Dose | Key Adverse Effects |
|---|---|---|---|
| Carbamazepine | 5 mg/kg/day | 10-20 mg/kg/day | Rash, hyponatremia, diplopia |
| Lamotrigine | 0.5 mg/kg/day | 1-5 mg/kg/day | Stevens-Johnson syndrome (slow titration essential) |
| Sodium Valproate | 10 mg/kg/day | 20-30 mg/kg/day | Weight gain, tremor, teratogenicity |
| Levetiracetam | 10 mg/kg/day | 20-40 mg/kg/day | Behavioral changes, somnolence |
⚠️ Warning: Never abruptly stop anti-epileptic drugs-risks rebound seizures and status epilepticus. Taper over 2-3 months minimum.
Evidence-Based Management: Treatment Protocols and Monitoring
Advanced Integration: Complex Cases and Special Considerations
A 14-year-old with T1D presents with recurrent severe hypoglycemia (glucose <3.0 mmol/L) despite optimized insulin regimen. Investigations reveal hypoglycemia unawareness (loss of autonomic warning symptoms) and impaired counter-regulatory response. Management requires technology integration: emphasizes hybrid closed-loop systems (automated insulin delivery adjusted by CGM readings) reducing hypoglycemia by 40% versus standard therapy. Simultaneously, structured education addressing hypoglycemia fear and glucose variability is essential. In epilepsy, drug-resistant epilepsy (failure of 2 appropriate medications) affects 30% of children. guidelines recommend early tertiary referral for video-EEG telemetry, advanced neuroimaging (3T MRI with epilepsy protocol), and consideration of epilepsy surgery (temporal lobectomy achieves 60-80% seizure freedom in mesial temporal sclerosis), vagal nerve stimulation, or ketogenic diet (50% responder rate in drug-resistant cases).
-
T1D Special Populations:
- Adolescents: HbA1c typically 10-15 mmol/mol higher due to insulin resistance, autonomy challenges
- Exercise: Reduce bolus insulin 30-50% before activity, consume 15-30g carbohydrate per hour
- Sick days: Never omit insulin; increase monitoring to 2-4 hourly; seek help if persistent ketones >1.5 mmol/L
-
Epilepsy Complications:
- SUDEP (Sudden Unexpected Death in Epilepsy): Risk 1:4,500 child-years; higher with uncontrolled generalized tonic-clonic seizures
- Status epilepticus: Seizure >5 minutes requires buccal midazolam 0.5 mg/kg (max 10 mg) or rectal diazepam 0.5 mg/kg
- Cognitive impact: 30-40% have comorbid learning difficulties; screen annually
| Complication | Type 1 Diabetes | Epilepsy |
|---|---|---|
| Acute Life-Threatening | DKA (1-2% annual risk) | Status epilepticus (5% lifetime risk) |
| Chronic Morbidity | Retinopathy, nephropathy (rare <10 years) | Cognitive impairment (30-40%) |
| Mortality | 0.1-0.2 per 1,000 person-years | 1.2 per 1,000 person-years |
| Quality of Life Impact | High (daily management burden) | Moderate (driving restrictions, injury risk) |
💎 Clinical Pearl: In drug-resistant epilepsy, early surgical evaluation is critical-outcomes are best when surgery occurs within 2 years of diagnosis, before secondary generalization develops.
Advanced Integration: Complex Cases and Special Considerations
High Yield Summary
Key Take-Aways:
- T1D requires same-day specialist assessment; target HbA1c ≤48 mmol/mol with MDI or CSII using CGM for all children
- DKA management: IV fluids first (10 mL/kg 0.9% saline), then insulin 0.05-0.1 units/kg/hour; never bolus insulin
- Epilepsy diagnosis is clinical; EEG supports but normal EEG doesn't exclude diagnosis (50% sensitivity first recording)
- First-line epilepsy treatment: carbamazepine/lamotrigine for focal seizures; valproate for generalized (avoid in females)
- Drug-resistant epilepsy (30% of cases) requires tertiary referral after 2 failed appropriate medications for surgical evaluation
- SUDEP risk 1:4,500 child-years; highest with uncontrolled generalized tonic-clonic seizures
- Status epilepticus (seizure >5 minutes) requires immediate buccal midazolam 0.5 mg/kg or rectal diazepam 0.5 mg/kg
Essential Chronic Paediatric Conditions Numbers:
| Parameter | Value | Clinical Significance |
|---|---|---|
| T1D HbA1c Target | ≤48 mmol/mol | Balance glycemic control with hypoglycemia risk |
| DKA Definition | pH <7.3 + ketones >3.0 mmol/L | Requires immediate hospital admission |
| Hypoglycemia Threshold | <3.0 mmol/L | Treat with 15g fast-acting carbohydrate |
| Epilepsy Drug Failure | 2 appropriate trials | Defines drug-resistant epilepsy |
| Status Epilepticus | Seizure >5 minutes | Emergency requiring benzodiazepine |
| SUDEP Risk | 1:4,500 child-years | Counsel families on seizure control importance |
Key Principles:
- Technology transforms T1D management: hybrid closed-loop systems reduce hypoglycemia 40% versus MDI
- Never stop anti-epileptic drugs abruptly-taper over minimum 2-3 months to prevent rebound seizures
- C-peptide <200 pmol/L confirms T1D; distinguishes from T2D where C-peptide preserved
- Sodium valproate contraindicated in females of childbearing potential due to teratogenicity (neural tube defects 1-2%)
- Epilepsy surgery achieves 60-80% seizure freedom in appropriate candidates; best outcomes when performed early
Quick Reference:
| Condition | Emergency Management | Monitoring | Long-term Target |
|---|---|---|---|
| T1D DKA | 10 mL/kg 0.9% saline, then insulin 0.05-0.1 units/kg/hr | Hourly glucose, 2-hourly venous gas | Resolution: pH >7.3, ketones <0.6 mmol/L |
| Hypoglycemia | 15g glucose, repeat in 15 min if needed | CGM/flash monitoring | Time in range 70-180 mg/dL >70% |
| Status Epilepticus | Buccal midazolam 0.5 mg/kg (max 10 mg) | Seizure diary, medication adherence | Seizure freedom |
| Drug-Resistant Epilepsy | Tertiary referral after 2 failed medications | Video-EEG telemetry, 3T MRI | Consider surgery/VNS/ketogenic diet |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




