Acute Paediatrics

On this page
Recognising the Unwell Child: Initial Assessment and Red Flags
A 15-month-old boy presents to the emergency department at 2 AM with a 12-hour history of fever. His parents report he's been "not himself" - refusing feeds, unusually quiet, and difficult to console. This scenario encapsulates the diagnostic challenge of the : distinguishing the 95% with self-limiting viral illness from the 5% with serious bacterial infection (SBI) requiring urgent intervention. Similarly, when a 4-year-old arrives with acute breathlessness and audible wheeze , rapid recognition of severity determines whether treatment occurs in the waiting room or resuscitation bay. Mastery of danger signs and immediate recognition criteria forms the foundation of safe acute paediatric practice.
-
Temperature thresholds requiring heightened vigilance:
- <3 months with fever ≥38°C: automatic sepsis pathway activation
- 3-6 months with fever ≥39°C: high-risk category per NICE NG143
- Fever duration >5 days: consider Kawasaki disease, occult bacterial focus
-
NICE Traffic Light System for febrile children (NG143):
- Green (low risk): normal colour, responds normally, strong cry, stays awake, normal skin/eyes
- Amber (intermediate): pallor reported by parent, not responding normally, reduced activity, dry mucous membranes
- Red (high risk): pale/mottled/ashen/blue, appears ill to healthcare professional, no response to social cues, weak/high-pitched cry, reduced skin turgor
-
Immediate wheeze severity markers:
- Life-threatening asthma: SpO₂ <92%, silent chest, poor respiratory effort, altered consciousness, cyanosis
- Acute severe: SpO₂ 92-95%, too breathless to talk/feed, heart rate >140 (2-5yr) or >125 (>5yr), respiratory rate >40 (2-5yr) or >30 (>5yr)
- Peak flow <50% predicted indicates severe attack in children >5 years
| Age Group | Respiratory Rate (breaths/min) | Heart Rate (beats/min) | Systolic BP (mmHg) |
|---|---|---|---|
| <1 year | 30-40 | 110-160 | 70-90 |
| 1-2 years | 25-35 | 100-150 | 80-95 |
| 2-5 years | 25-30 | 95-140 | 80-100 |
| 5-12 years | 20-25 | 80-120 | 90-110 |
🚩 Red Flag: A quiet, still child is more concerning than a screaming one. Altered responsiveness indicates potential cerebral hypoperfusion or hypoxia.

Recognising the Unwell Child: Initial Assessment and Red Flags
Understanding Fever Pathophysiology and Bronchospasm Mechanisms
Fever represents a regulated upward shift in hypothalamic set-point, triggered when circulating pyrogens - primarily interleukin-1β, interleukin-6, and tumour necrosis factor-α - cross the blood-brain barrier or act on circumventricular organs. This distinguishes true fever from hyperthermia (failure of thermoregulation). The evolutionary advantage of fever remains debated, but temperatures 38.5-40°C enhance neutrophil function and reduce viral replication. However, fever alone causes significant parental anxiety and accounts for 30% of paediatric emergency presentations, creating a tension between reassurance and vigilance for the .
-
Pathophysiological fever response:
- Exogenous pyrogens (bacterial endotoxin, viral particles) → macrophage activation
- Endogenous pyrogen release → prostaglandin E₂ synthesis in hypothalamus
- Peripheral vasoconstriction and behavioural changes (seeking warmth) raise core temperature
- Antipyretic mechanism: paracetamol inhibits COX-3 centrally; ibuprofen inhibits COX-1/2 peripherally
-
Bronchospasm pathophysiology in :
- Viral-induced wheeze (predominant <5 years): direct epithelial damage → inflammatory mediator release → smooth muscle contraction
- Atopic asthma (predominant >5 years): allergen cross-linking IgE on mast cells → histamine, leukotrienes, prostaglandins → bronchospasm + mucosal oedema + mucus hypersecretion
- Triple pathology: airway smooth muscle contraction (reversible within minutes), mucosal inflammation (hours), mucus plugging (days)
-
Why β₂-agonists work rapidly:
- Salbutamol binds airway smooth muscle β₂-receptors → adenylyl cyclase activation → ↑cAMP → myosin light chain kinase inhibition → bronchodilation within 5-15 minutes
- Peak effect 30-60 minutes; duration 4-6 hours

⭐ Clinical Pearl: Fever height correlates poorly with SBI risk - a child with 39.5°C and normal behaviour is lower risk than one with 38.5°C and reduced responsiveness. The Traffic Light System incorporates this clinical gestalt.
Understanding Fever Pathophysiology and Bronchospasm Mechanisms
Systematic Clinical Approach: From Recognition to Action
An 8-month-old girl arrives with 24-hour fever and irritability. Her mother reports she cried when her nappy was changed. You note she has reduced wet nappies over the past 12 hours. Temperature is 39.2°C, heart rate 165, capillary refill time 3 seconds centrally. This presentation demands systematic assessment using NICE NG143 criteria to determine whether empirical antibiotics are indicated before investigation results return. The structured approach to the prevents both over-investigation of well children and missed SBI in those with subtle signs.
-
Structured fever assessment sequence:
- ABC assessment first: airway patency, work of breathing, perfusion markers (CRT, pulse volume, BP)
- Focused history: fever duration/height, fluid intake, urine output, rash evolution, contact history, travel, immunisation status
- Systematic examination:
- Cardiovascular: CRT <2 seconds (normal), tachycardia for fever (expected 10 bpm per °C rise)
- Respiratory: work of breathing, focal signs suggesting pneumonia
- ENT: throat examination (avoid if stridor/drooling), ear drums
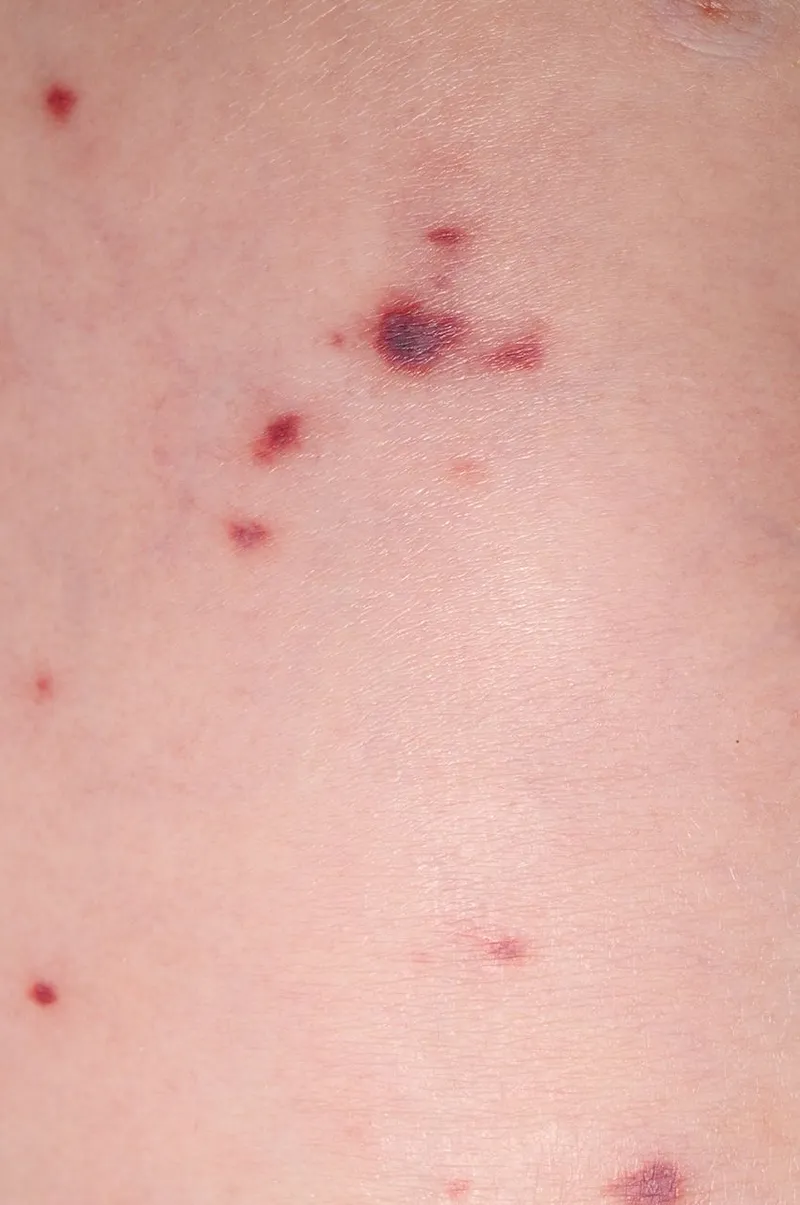
- Skin: petechiae/purpura (glass test), Kawasaki features (polymorphous rash, conjunctivitis, strawberry tongue)
- Neurological: GCS, neck stiffness (unreliable <18 months), fontanelle
-
Acute wheeze systematic approach per NICE NG80:
- Immediate assessment: ability to speak in sentences, SpO₂ on room air, respiratory rate, accessory muscle use, wheeze character
- Severity classification determines location of treatment:
- Moderate: SpO₂ ≥92%, talking in phrases, no life-threatening features → treat in ED
- Severe: SpO₂ 92-95%, too breathless to talk → senior review, consider IV access
- Life-threatening: SpO₂ <92%, silent chest, exhaustion → resuscitation team activation
-
Red flag examination findings requiring immediate escalation:
- Non-blanching rash with fever (meningococcal disease until proven otherwise)
- Bulging fontanelle, neck stiffness, photophobia (meningitis)
- Reduced consciousness (GCS <15 or not responding to parents)
- Bile-stained vomiting (intestinal obstruction)
- Focal neurological signs, status epilepticus
| Investigation | Indication in Febrile Child | Positive Threshold |
|---|---|---|
| Blood culture | Red features OR amber + temp ≥39°C | Growth at 24-48h |
| Urine dipstick/culture | Non-specific illness <3yr, especially <6mo | Nitrites OR leukocytes + symptoms |
| Lumbar puncture | <1 month with fever OR signs of meningism | WCC >20, protein >0.4g/L, glucose <50% blood |
| Chest X-ray | Fever + tachypnoea + focal signs | Consolidation, air bronchograms |
Systematic Clinical Approach: From Recognition to Action
Distinguishing Serious Pathology from Benign Illness
The diagnostic challenge in acute paediatrics lies in pattern recognition among undifferentiated presentations. A febrile child with coryza, normal behaviour, and good fluid intake likely has viral upper respiratory tract infection - but 1-2% will have urinary tract infection, and 0.5% will have bacteraemia. Similarly, most preschool wheeze episodes are viral-induced and self-limiting, but missing the child with inhaled foreign body or cardiac failure has catastrophic consequences. The and demand systematic approaches that balance sensitivity (catching serious illness) with specificity (avoiding unnecessary intervention).
-
Discriminating SBI from viral illness:
- Positive predictors of SBI: temperature ≥40°C, ill appearance, CRP >80 mg/L, procalcitonin >0.5 ng/mL, WCC >15×10⁹/L or <5×10⁹/L
- Negative predictors: well appearance, normal behaviour, clear viral focus (coryza, viral exanthem)
- Urinary tract infection: most common occult SBI in <3 years (5-7% of febrile infants), especially girls and uncircumcised boys
- Occult bacteraemia: reduced to <0.5% post-pneumococcal conjugate vaccine (PCV) and Haemophilus influenzae type b (Hib) vaccine
-
Asthma versus alternative wheeze causes:
- Viral-induced wheeze: age <3 years, episodic with viral infections only, no interval symptoms, family history less prominent
- Multi-trigger wheeze/asthma: interval symptoms, exercise-induced symptoms, atopic history (eczema, allergic rhinitis), response to inhaled corticosteroids
- Cardiac wheeze: signs of heart failure (hepatomegaly, gallop rhythm, poor feeding), failure to thrive
- Foreign body aspiration: sudden onset, unilateral wheeze, reduced air entry one side, history of choking episode
| Feature | Viral URTI | Serious Bacterial Infection |
|---|---|---|
| Appearance | Well, playful between fever spikes | Persistently unwell, lethargic |
| Fever pattern | Responds to antipyretics | Poor response to antipyretics |
| Hydration | Normal urine output | Reduced wet nappies, dry mucous membranes |
| Inflammatory markers | CRP <40, WCC normal | CRP >80, WCC >15 or <5 |
| Duration | Improves by day 3-5 | Worsening or persistent >5 days |
📌 Mnemonic for AMBER features: PANDA - Pallor, Activity reduced, Not responding normally, Dry mucous membranes, Age 3-6 months with fever ≥39°C
Distinguishing Serious Pathology from Benign Illness
Evidence-Based Management and Escalation Thresholds
A 3-year-old with acute severe asthma receives back-to-back salbutamol via spacer (10 puffs every 20 minutes for 3 doses) plus oral prednisolone 20 mg. After 1 hour, respiratory rate remains 45/min and SpO₂ is 93% on room air. This clinical trajectory - failure to improve despite maximal first-line therapy - triggers escalation per NICE NG80 guidelines. Similarly, the aged 6 weeks with temperature 38.5°C and no obvious focus requires empirical IV ceftriaxone 50 mg/kg after septic screen, regardless of how well they appear, because SBI risk exceeds 10% in this age group.
-
Febrile child management thresholds per NICE NG143:
- <1 month with fever: immediate hospital admission, full septic screen (blood culture, urine culture, lumbar puncture), IV antibiotics (cefotaxime 50 mg/kg TDS + amoxicillin 50 mg/kg TDS to cover Listeria)
- 1-3 months with fever: hospital assessment, septic screen, empirical antibiotics if any amber/red features
- >3 months with red features: blood culture, urine sample, consider CRP/FBC, empirical antibiotics if ill appearance
- Antipyretic dosing: paracetamol 15 mg/kg QDS (max 4g/24h), ibuprofen 10 mg/kg TDS (max 30 mg/kg/24h) - for distress, not routinely to reduce temperature
-
Acute wheeze escalation pathway:
- First-line: salbutamol 10 puffs via spacer (or 2.5-5mg nebulised), repeat every 20 minutes up to 3 doses, plus prednisolone 20 mg (2-5yr) or 30-40 mg (>5yr)
- Second-line (if inadequate response): continuous salbutamol nebulisers, ipratropium bromide 250 mcg nebulised (added to salbutamol), IV magnesium sulphate 40 mg/kg over 20 minutes (max 2g)
- Third-line (life-threatening): IV salbutamol infusion (loading 15 mcg/kg, then 1-5 mcg/kg/min), aminophylline (if not on oral theophylline), senior anaesthetic review for possible intubation
-
When to investigate versus treat empirically:
- Investigate first if stable, amber features, clear focus (e.g., tonsillitis, viral exanthem)
- Treat empirically first if unstable, red features, age <1 month, immunocompromised
- Urine sample essential if no clear focus in <3 years (clean catch preferred; catheter if urgent; avoid bag specimens for culture)
| Antibiotic | Indication | Dose | Route |
|---|---|---|---|
| Ceftriaxone | Suspected sepsis >1 month | 50-80 mg/kg OD (max 4g) | IV |
| Cefotaxime | Suspected sepsis <1 month | 50 mg/kg TDS | IV |
| Amoxicillin | Added <1 month for Listeria | 50 mg/kg TDS | IV |
| Co-amoxiclav | Pneumonia | 25 mg/kg TDS (max 625mg) | PO/IV |
🚩 Red Flag: In acute asthma, a rising PaCO₂ (>6 kPa) indicates exhaustion and impending respiratory failure - this child needs senior anaesthetic assessment for possible intubation, not just more bronchodilators.
Evidence-Based Management and Escalation Thresholds
Comprehensive Discharge Planning and Safety-Netting
An 18-month-old with fever and viral URTI is ready for discharge after 2 hours of observation. Before leaving, parents need specific written and verbal safety-netting advice: return immediately if non-blanching rash develops, if child becomes unrousable, or if fever persists beyond 5 days. This structured approach to the reduces re-attendance for parental anxiety while ensuring genuine deterioration is recognised. Similarly, a child recovering from moderate acute asthma requires discharge with personalised asthma action plan, inhaled corticosteroid prescription, and GP follow-up within 48 hours.
-
Febrile child discharge criteria:
- Temperature <38°C for ≥1 hour post-antipyretic
- Taking oral fluids adequately
- Normal behaviour (smiling, playing, responding to parents)
- Parents confident to monitor at home
- Clear safety-netting advice provided (verbal + written)
-
Safety-netting advice for parents:
- Return immediately if: non-blanching rash, drowsiness/difficult to wake, neck stiffness, unusual cry, refusing all fluids for >8 hours, reduced urine output
- Contact GP/NHS 111 if: fever persists >5 days, new symptoms develop, parental concern increases
- Expected course: viral illnesses typically worsen days 2-3, improve day 4-5; fever may spike to 39-40°C but should respond to antipyretics
-
Acute wheeze discharge planning:
- Criteria: SpO₂ >95% on room air, respiratory rate normal for age, minimal work of breathing, salbutamol requirement <4-hourly
- Discharge prescriptions: prednisolone 3-day course (20-40 mg OD depending on age), salbutamol inhaler + spacer, consider initiating ICS if recurrent episodes
- Follow-up: GP/asthma nurse within 48 hours, paediatric respiratory clinic if life-threatening attack or poor control
- Personalised asthma action plan: usual medications, how to recognise worsening, when to increase treatment, when to seek help
-
Parent education strategies:
- Demonstrate inhaler technique with spacer (5 breaths per puff for young children, single breath for older children)
- Explain difference between reliever (salbutamol - blue) and preventer (ICS - brown/orange)
- Address fever myths: fever itself does not cause brain damage; tepid sponging is unnecessary and distressing
- Provide written information sheet with red flag symptoms highlighted
| Inhaler Device | Age Range | Technique Key Points |
|---|---|---|
| pMDI + spacer + face mask | <3 years | 5 breaths per puff, seal mask to face |
| pMDI + spacer + mouthpiece | 3-5 years | 5 breaths per puff, lips sealed around mouthpiece |
| pMDI + spacer (self-administered) | >5 years | Single deep breath per puff, 10-second hold |
| Dry powder inhaler | >6 years | Rapid deep inhalation, 10-second hold |
⭐ Clinical Pearl: Most parents over-dress febrile children. Advise one layer of clothing, room temperature 18-20°C, and fluids to comfort. Aggressive cooling measures (cold baths, fans) cause distress and shivering, which paradoxically raises core temperature.
Comprehensive Discharge Planning and Safety-Netting
High Yield Summary
Key Take-Aways:
- Traffic Light System is mandatory for all febrile children - red features require immediate intervention; amber features require senior review within 2 hours; green features allow discharge with safety-netting
- Age <3 months with fever ≥38°C is high-risk - automatic hospital assessment, septic screen, and empirical IV antibiotics (cefotaxime + amoxicillin if <1 month)
- Acute severe asthma defined by SpO₂ 92-95% - requires back-to-back salbutamol, oral prednisolone, and escalation to ipratropium/IV magnesium if inadequate response after 1 hour
- Non-blanching rash with fever is meningococcal disease until proven otherwise - immediate IM/IV benzylpenicillin (or ceftriaxone) without waiting for investigations
- Urine sample essential in febrile children <3 years without obvious focus - UTI is the most common occult serious bacterial infection (5-7% of febrile infants)
- Rising PaCO₂ in acute asthma indicates respiratory failure - requires senior anaesthetic assessment for possible intubation, not just escalation of bronchodilators
- Safety-netting is a clinical skill, not an afterthought - specific red flags, expected illness trajectory, and when/how to seek further help must be communicated clearly
Essential Acute Paediatrics Numbers:
| Parameter | Threshold | Action |
|---|---|---|
| Fever in <1 month | Any fever ≥38°C | Full septic screen + IV antibiotics |
| Fever in 1-3 months | ≥39°C or amber/red features | Hospital assessment + investigations |
| SpO₂ in acute wheeze | <92% | Life-threatening - resus team |
| CRP | >80 mg/L | Suggestive of bacterial infection |
| Salbutamol dose | 10 puffs via spacer | Repeat every 20 min up to 3 doses |
| Prednisolone dose | 20 mg (2-5yr), 30-40 mg (>5yr) | Single dose, continue 3 days |
| IV magnesium | 40 mg/kg over 20 min (max 2g) | For severe asthma not responding |
Key Principles:
- Well appearance trumps fever height - a child with 40°C who is playful and drinking is lower risk than one with 38.5°C who is lethargic and refusing fluids
- Viral-induced wheeze predominates <3 years; atopic asthma >5 years - treatment principles identical, but prognosis differs (most viral wheezers outgrow symptoms by school age)
- Antibiotics do not shorten viral illness - prescribing for parental reassurance increases resistance and medicalises normal childhood illness
- Inhaler technique matters more than device choice - 10 puffs via spacer equals one nebuliser dose if technique correct; most children use inhalers incorrectly without regular checks
Quick Reference Red Flags:
- Non-blanching rash + fever → meningococcal disease
- Bile-stained vomiting → intestinal obstruction
- Bulging fontanelle → raised intracranial pressure
- Silent chest in wheeze → life-threatening asthma
- Reduced consciousness (not responding to parents) → sepsis/meningitis/hypoxia
- Capillary refill time >3 seconds → shock
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




