Pathophysiology - Sweet Vessel Sabotage
Chronic hyperglycemia fuels vascular damage through multiple pathways:
- Macrovascular Disease: Accelerated atherosclerosis.
- Affects larger arteries, especially infrapopliteal (tibial, peroneal).
- Leads to stenosis and occlusion.
- Microvascular Disease:
- Capillary basement membrane thickening, impaired perfusion.
- Endothelial cell damage.
- Key Mechanisms:
- Endothelial Dysfunction: ↓ Nitric Oxide ($NO$) synthesis/bioavailability, ↑ Endothelin-1.
- AGEs (Advanced Glycation End Products): Accumulate, causing vascular stiffness, inflammation, prothrombotic state.
- Oxidative Stress: ↑ Reactive Oxygen Species (ROS) damage endothelium.
- Inflammation: Chronic low-grade inflammation.
- Neuropathy's Vascular Impact:
- Autonomic neuropathy: impaired vasoregulation, AV shunting.
- Sensory/Motor neuropathy (e.g., Charcot foot): abnormal pressures, ulceration, ↑ infection risk, ↑ vascular demand.
⭐ Diabetic patients often develop infrapopliteal arterial disease, affecting tibial and peroneal arteries more severely than non-diabetics.

Clinical Presentation & Diagnosis - Foot's SOS Signals
- Symptoms: Intermittent claudication, rest pain, non-healing ulcers, gangrene.
- Signs: Diminished/absent pulses; skin changes (shiny, atrophic, hair loss); dependent rubor, pallor on elevation. 📌 Chronic PAD "SOS": Skin changes, Ongoing pain, Slow/absent pulses.
- Key Diagnostics:
- Ankle-Brachial Index (ABI): $ABI = \text{Highest Ankle Systolic Pressure} / \text{Highest Brachial Systolic Pressure}$.
- PAD: ABI < 0.9. CLI: ABI < 0.4.
- Toe-Brachial Index (TBI): TBI < 0.7 (esp. if ABI unreliable due to calcification).
- Doppler & Duplex Ultrasound: Initial imaging.
- CTA/MRA, DSA (gold standard): Detailed anatomy & intervention planning.
- Ankle-Brachial Index (ABI): $ABI = \text{Highest Ankle Systolic Pressure} / \text{Highest Brachial Systolic Pressure}$.
⭐ Monofilament testing primarily assesses neuropathy, but its findings often coexist with vascular disease, indicating high-risk foot.
Classification Systems - Grading the Grief
Classification systems are crucial for assessing diabetic foot disease severity and guiding management.
| System | Key Components Assessed | Vascular Assessment Detail | Clinical Significance |
|---|---|---|---|
| Wagner | Ulcer depth, Gangrene (Grades 0-5) | Indirect (gangrene implies ischemia) | Simple for initial grading. Grade 4 (forefoot), 5 (extensive) = severe ischemia. |
| PEDIS | Perfusion, Extent, Depth, Infection, Sensation | Explicit "Perfusion" (e.g., ABI, TcPO2) | Comprehensive, good for multidisciplinary assessment. |
| WIFI | Wound, Ischemia, foot Infection | Explicit "Ischemia" (Grades 0-3; e.g., ABI, SPP, TcPO2) | Stratifies amputation risk, guides revascularization. |
Management Strategies - Saving Soles & Stems
- Conservative & Medical Therapy:
- Risk factor control: Glycemia (HbA1c < 7%), BP < 130/80 mmHg, statins, antiplatelets (Aspirin/Clopidogrel).
- Lifestyle: Crucial smoking cessation, structured exercise.
- Pharmacologic: Cilostazol for claudication symptoms.
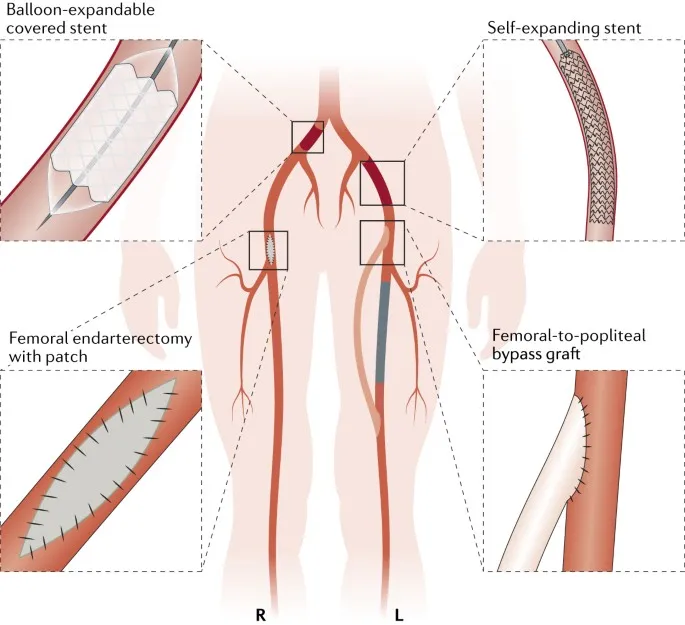
- Revascularization Options:
- Endovascular (EVT): PTA, stenting, atherectomy. Often first-line for suitable lesions.
- Surgical Bypass: Autogenous vein (e.g., saphenous) preferred for extensive disease or failed EVT.
- Wound Care & Adjunctive Measures:
- Local: Debridement, appropriate dressings, infection control.
- Offloading: Essential (e.g., Total Contact Cast).
- Hyperbaric Oxygen Therapy (HBOT): Adjunctive for select non-healing wounds.
- Amputation (Last Resort):
- For non-salvageable limb, uncontrolled sepsis, or to save life.
⭐ For diabetic patients with CLI & extensive infrapopliteal disease, distal bypass with autogenous vein offers best long-term patency if EVT is unsuitable.
High‑Yield Points - ⚡ Biggest Takeaways
- Diabetic foot ulcers (DFU) primarily result from neuropathy and peripheral artery disease (PAD).
- Wagner and University of Texas (UT) systems are key for DFU classification.
- Ankle-Brachial Index (ABI) < 0.9 suggests PAD; ABI < 0.4 indicates critical limb ischemia.
- Management pillars: glycemic control, wound care, offloading, and revascularization if PAD is present.
- Charcot neuroarthropathy is a major, deforming complication requiring prompt recognition.
- Multidisciplinary team approach and patient education are crucial for limb salvage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

