Phases of Healing - The Repair Crew
📌 Mnemonic: I Prefer Many Red Apples (Inflammation, Proliferation, Maturation/Remodeling)
- Hemostasis: Platelets, fibrin clot formation.
- Inflammatory Phase (0-3 days):
- Cells: Neutrophils (PMNs), Macrophages (M1/M2).
- Mediators: Cytokines (TNF-α, IL-1, IL-6), PDGF, VEGF.
- Proliferative Phase (3 days - 3 weeks):
- Cells: Fibroblasts, myofibroblasts.
- Events: Collagen Type III, granulation tissue, angiogenesis, epithelialization.
- Remodeling/Maturation Phase (3 weeks - 1 year+):
- Events: Collagen Type I (replaces III), ↑ tensile strength, scar formation.
- Enzymes: MMPs, TIMPs.
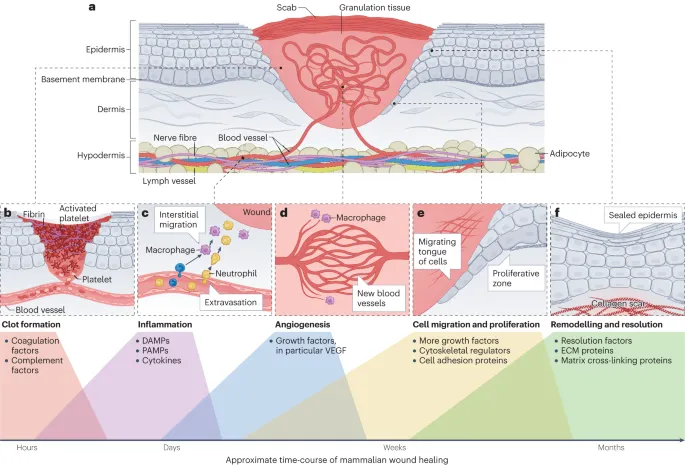
⭐ Maximum collagen deposition occurs by 3 weeks, but wound strength reaches only ~20-30% of normal tissue; it reaches ~80% by 1 year but never 100%.
Healing Intentions - Stitch in Time
| Feature | Primary Intention | Secondary Intention | Tertiary Intention (Delayed Primary) |
|---|---|---|---|
| Edges | Clean, approximated | Open, not approximated | Initially open, later approximated |
| Tissue Loss | Minimal | Significant | Variable, often present |
| Process | Direct closure | Granulation, contraction, epithelialization | Initial debridement, delayed closure |
| Infection Risk | Low | High | Moderate (initially high, then reduced) |
| Scar | Minimal, linear | Large, irregular; significant contraction | More than primary, less than secondary |
| Examples | Surgical incision | Abscess cavity, burns, pressure sores | Contaminated traumatic wound, burst abdomen |
⭐ Wound contraction is a key feature of secondary intention healing, primarily mediated by myofibroblasts.
📌 Mnemonic: Primary = Perfect; Secondary = Slow & Scarring; Tertiary = Two-stage/ Time-delayed closure
Healing Hurdles - Repair Roadblocks
- Local Factors:
- Infection (most common cause of delay)
- Hypoxia/Ischemia
- Foreign body
- Hematoma/Seroma
- Radiation
- Edema, Pressure
- Poor surgical technique
- Systemic Factors:
- Age (advanced)
- Nutrition: Deficiencies (Protein, Vit C, Vit A, Zinc, Copper)
- Diabetes Mellitus
- Corticosteroids
- Smoking
- Chemotherapy/Immunosuppression
- Uremia, Jaundice
- Malignancy
- Genetic disorders (e.g., Ehlers-Danlos) 📌 Mnemonic (DIDN'T HEAL):
- Diabetes
- Infection
- Drugs (e.g., steroids)
- Nutrition deficiencies
- Tissue necrosis
- Hypoxia
- Excessive tension
- Another wound
- Low temp / Local factors
⭐ Vitamin C is essential for collagen synthesis (hydroxylation of proline and lysine), and Vitamin A can counteract the inhibitory effects of steroids on wound healing.
Scar Stories - Healing Gone Rogue
| Feature | Hypertrophic Scar | Keloid |
|---|---|---|
| Boundaries | Stays within wound margins | Extends beyond wound margins |
| Collagen | Mainly Type III | Type I & III |
| Natural History | May regress | Rarely regresses; recurs |
| Skin Type | All | Dark skin predilection |
- Acute Complications:
- Wound Dehiscence: Separation of wound layers.
- Evisceration: Protrusion of viscera.
- Chronic Wounds (Impaired healing >3 months):
- Types: Diabetic foot ulcers, Venous stasis ulcers, Arterial insufficiency ulcers.
- Pressure Sores (Decubitus): Staged I-IV.
⭐ Pressure ulcers are staged I-IV: Stage I (non-blanchable erythema), Stage II (partial-thickness loss), Stage III (full-thickness skin loss), Stage IV (full-thickness tissue loss with exposed bone/tendon/muscle).
- Marjolin's Ulcer: SCC arising in chronic wounds or old scars (e.g., burn scars).
High‑Yield Points - ⚡ Biggest Takeaways
- Healing phases: Inflammation (0-3d), Proliferation (3d-3wks), Remodeling (3wks-2yrs).
- Macrophages are pivotal, bridging inflammation and repair; neutrophils are first responders.
- Collagen switch: From Type III (early, weak) to Type I (late, strong scar).
- Scar strength: Reaches ~80% of original tissue strength by 3 months, never 100%.
- Keloids grow beyond original wound margins; hypertrophic scars remain within.
- Myofibroblasts mediate wound contraction, reducing defect size.
- Factors impairing healing: Infection, ischemia, diabetes, steroids, malnutrition.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

