Phases of Healing - Speedy Recovery Stages
- Hemostasis: Immediate. Vasoconstriction, platelet aggregation (plug), coagulation cascade activation → fibrin clot.
- Inflammation (Substrate Phase): Days 1-4. Neutrophils (peak 24-48h), followed by Macrophages (key for transition). Phagocytosis, cytokine release.
- Proliferation (Fibroblastic Phase): Day 3 to 3 weeks. Fibroblasts deposit Collagen Type III. Angiogenesis (new vessels), granulation tissue. Epithelialization. Myofibroblasts cause wound contraction.
- Remodeling (Maturation Phase): 3 weeks to 1-2 years. Collagen Type III gradually replaced by stronger Type I. ↑ Tensile strength. Scar flattens.
⭐ Maximum tensile strength achieved is about 70-80% of original tissue, typically by 3 months.

Types of Healing - Gap Closing Goals
- Primary Intention: Clean wound, edges apposed (sutured). Minimal tissue loss. Goal: Rapid closure, fine scar.
- Secondary Intention: Edges not apposed, large defect. Heals by granulation, contraction, epithelialization. Goal: Body heals open wound.
⭐ Myofibroblasts are key for wound contraction in secondary intention.
- Tertiary Intention (Delayed Primary Closure): Initially left open (e.g., due to contamination), later surgically closed. Goal: Manage issues (infection), then close.
Factors Affecting Healing - Repair Roadblocks
- Local Factors:
- Infection (Most common delay)
- Poor perfusion/Hypoxia (pO₂ < 40mmHg impairs collagen synthesis)
- Foreign body, Hematoma, Seroma, Necrotic tissue
- Trauma, Tension
- Radiation, Edema
- Systemic Factors:
- Age (Advanced: ↓cell activity, ↓collagen)
- Nutrition: ↓Protein, ↓Vit C, ↓Vit A, ↓Zinc, ↓Copper
- Diabetes (DM) (↓PMN function, ↓angiogenesis, ↓collagen)
- Meds: Steroids (↓inflammation, ↓collagen), Chemo, NSAIDs (early)
- Smoking (↓O₂ delivery, ↑CO), Obesity (↓perfusion)
- Systemic Illness: Uremia, Jaundice, Malignancy, Anemia (Hb < 10g/dL)

⭐ Vitamin C is crucial for hydroxylation of proline and lysine, essential for collagen cross-linking; deficiency leads to impaired healing and scurvy.
Wound Care Principles - Bandage & Beyond
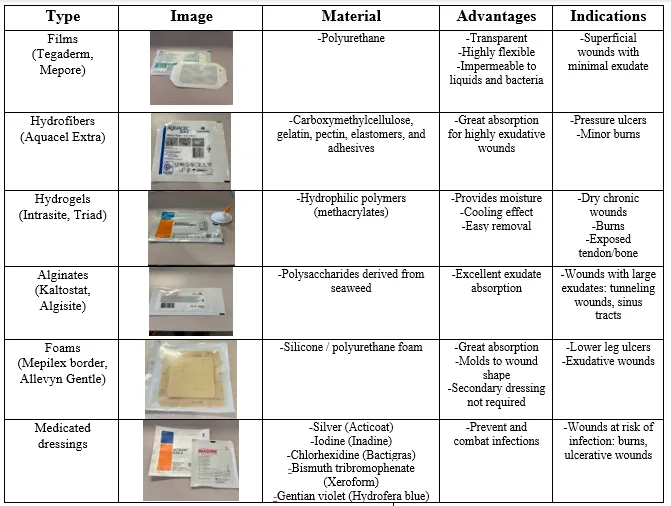
- Dressing Goals: Protect, absorb exudate, debride, compress, deliver medication.
- Dressing Types & Key Uses:
- Gauze: Packing, absorption.
- Films (e.g., Tegaderm): Superficial wounds, autolytic debridement, visualization.
- Foams: Moderate/heavy exudate, cushioning.
- Hydrocolloids (e.g., Duoderm): Autolytic debridement, light/moderate exudate, occlusive.
- Alginates: Heavy exudate, hemostatic, cavity wounds.
- Hydrogels: Hydrate dry/necrotic wounds, slough removal.
- Negative Pressure Wound Therapy (NPWT/VAC):
- Mechanism: Subatmospheric pressure (typically -75 to -125 mmHg).
- Benefits: ↓edema, ↑granulation tissue, ↑perfusion, ↓bacterial load.
- Indications: Acute, chronic, traumatic wounds; grafts/flaps.
- ⚠️ Contraindications: Malignancy in wound, untreated osteomyelitis, non-enteric/unexplored fistulas, necrotic tissue with eschar, exposed vessels/organs.
- Bandaging: Apply distal to proximal; even, firm pressure; avoid tourniquet effect.
⭐ NPWT is generally contraindicated directly over exposed blood vessels, nerves, anastomotic sites, or organs due to risk of erosion or fatal hemorrhage. Use a protective barrier if unavoidable and monitor closely.
Complications of Healing - Scar Wars
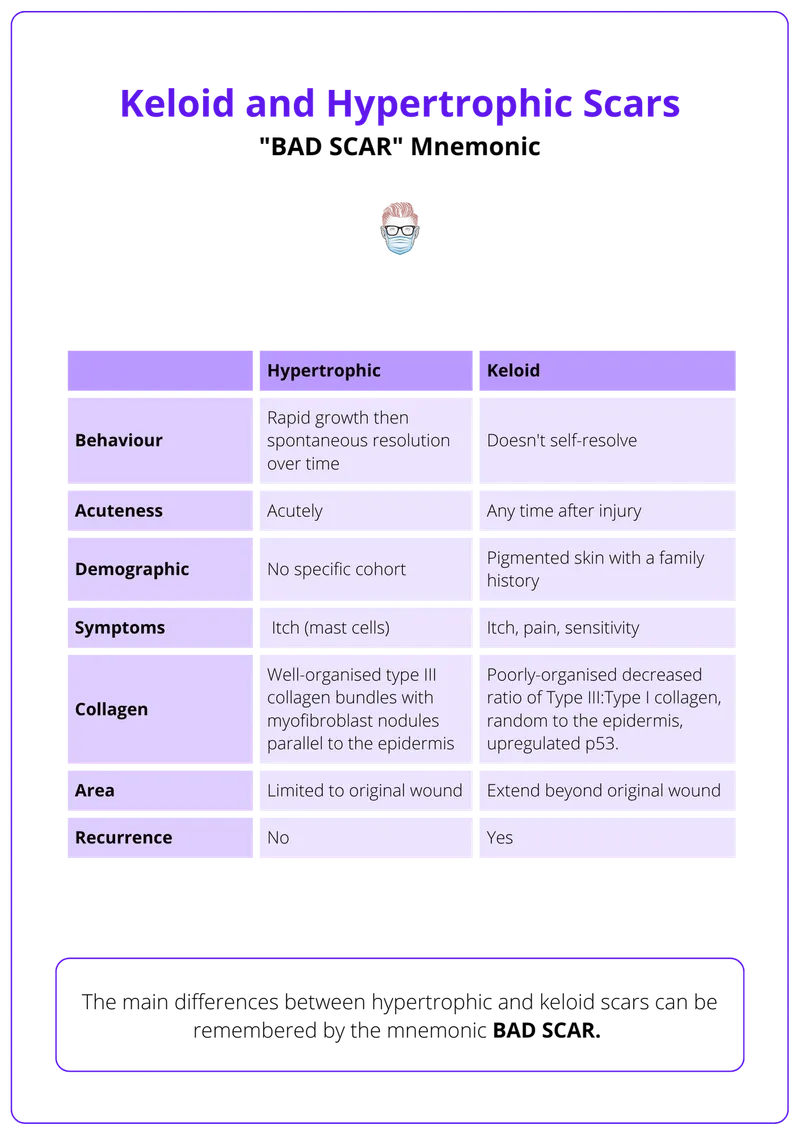
- Hypertrophic Scar: Raised, red, itchy. Develops within weeks.
- Keloid: Rubbery, overgrows boundaries. Develops months later. Common in darker skin. 📌 KELOID: Keeps Extending.
- Contractures: Limit movement, deformity. Esp. joints, burns.
- Ulceration: Chronic non-healing.
⭐ Marjolin's ulcer: SCC in chronic wounds, burn scars, osteomyelitis sinuses.
- Others: Dyspigmentation, persistent pain, pruritus.
High‑Yield Points - ⚡ Biggest Takeaways
- Healing Phases: Inflammatory (PMNs, MΦ), Proliferative (fibroblasts, new vessels), Remodeling (collagen I for III).
- Collagen Facts: Type III (early) replaced by Type I (strong); max strength ~80% at 3 months.
- Wound Closure: Primary (sutured), Secondary (granulation), Tertiary (delayed primary).
- Major Inhibitors: Infection, hypoxia, malnutrition (Vit C, zinc), diabetes, steroids.
- Problematic Scars: Keloids grow beyond wound; Hypertrophic scars stay within boundaries.
- Myofibroblasts: Crucial for wound contraction, especially in secondary intention healing.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

