Definitions & Overview (2°/3° HPT) - PTH Party Crashers
- Secondary Hyperparathyroidism (2° HPT):
- ↑PTH due to chronic hypocalcemia (e.g., CKD, Vit D deficiency).
- Parathyroid glands: Hyperplastic, reactive.
- Labs: ↓/Normal $Ca^{2+}$, ↑$PO_4^{3-}$ (CKD), ↑PTH, ↓Vit D.
- Tertiary Hyperparathyroidism (3° HPT):
- Autonomous PTH secretion after prolonged 2° HPT.
- Parathyroid glands: Adenomatous, autonomous.
- Labs: ↑$Ca^{2+}$ (hypercalcemia), markedly ↑PTH.
- Core Difference:
- 2° HPT: Reactive PTH surge to low $Ca^{2+}$.
- 3° HPT: Uncontrolled PTH secretion despite normal/high $Ca^{2+}$.
⭐ Tertiary HPT features persistent hypercalcemia & ↑PTH even post-renal transplant, unlike resolving secondary HPT.
Pathophysiology (2°/3° HPT) - Gland Gone Wild
- Secondary HPT (2° HPT):
- Adaptive response to chronic hypocalcemia, often from Chronic Kidney Disease (CKD).
- CKD → ↓ active Vit D ($1,25(OH)_2D_3$) & ↑ $PO_4^{3-}$ retention.
- Leads to: ↓ serum $Ca^{2+}$ & ↑ serum $PO_4^{3-}$.
- Parathyroid glands undergo diffuse hyperplasia → ↑ PTH secretion to normalize $Ca^{2+}$.
- Tertiary HPT (3° HPT):
- Develops from long-standing, severe 2° HPT.
- Parathyroid glands become autonomous (adenomatous or monoclonal hyperplastic change).
- Persistent, excessive PTH secretion despite correction of hypocalcemia (e.g., post-renal transplant).
- Results in hypercalcemia.
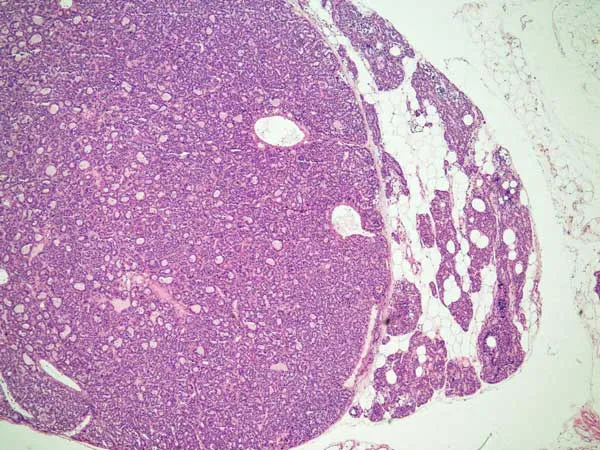
⭐ In tertiary HPT, one or more parathyroid glands develop autonomous function, leading to hypercalcemia that is no longer responsive to medical management aimed at correcting calcium/phosphate balance.
Clinical Features & Diagnosis (2°/3° HPT) - Spotting the Signs
-
Clinical Presentation:
- 2° HPT: Often asymptomatic; CKD features (fatigue, edema), bone pain, pruritus.
- 3° HPT: Hypercalcemia symptoms (📌 "bones, stones, groans, moans"), nephrolithiasis.
- Severe: Renal osteodystrophy (fractures), calciphylaxis (skin necrosis).
-
Key Investigations:
- Laboratory Findings:
Parameter Secondary HPT (2°) Tertiary HPT (3°) Serum $Ca^{2+}$ ↓ / Normal ↑ Serum $PO_4^{3-}$ ↑ Variable (often ↑) ALP ↑ ↑ PTH ↑ (compensatory) Markedly ↑ (autonomous, >800 pg/mL often) - Imaging:
- X-ray: Osteitis fibrosa cystica (subperiosteal resorption of phalanges, "salt & pepper" skull).
- Ultrasound/Sestamibi: Gland localization (3° HPT, pre-surgery).
- Laboratory Findings:
⭐ Autonomous PTH secretion with PTH levels often exceeding 800 pg/mL is characteristic of tertiary hyperparathyroidism.
Management Strategies (2°/3° HPT) - Taming the Glands
- Primary Goal: Normalize serum Ca, P, and PTH levels, preventing complications like bone disease and calciphylaxis.
- Medical Therapy (Foundation for 2° HPT, may be used in 3° HPT):
- Correct underlying cause (e.g., CKD management, Vit D repletion).
- Dietary $PO_4^{3-}$ restriction.
- Phosphate binders (e.g., Sevelamer, Calcium Acetate) to ↓$PO_4^{3-}$ absorption.
- Active Vitamin D sterols (e.g., Calcitriol, Paricalcitol) to suppress PTH (use cautiously if ↑Ca or ↑$PO_4^{3-}$).
- Calcimimetics (e.g., Cinacalcet) - ↑CaSR sensitivity, ↓PTH. 📌 "Cina-Calci-Mimics" Ca.
⭐ In tertiary hyperparathyroidism, autonomous parathyroid function persists even after successful renal transplantation; parathyroidectomy is often required for definitive management of hypercalcemia.
High-Yield Points - ⚡ Biggest Takeaways
- Secondary HPT is most often from CKD, causing diffuse parathyroid hyperplasia.
- Labs in Secondary HPT: PTH ↑↑, Ca ↓ or normal, PO₄ ↑ (in CKD).
- Tertiary HPT develops from prolonged secondary HPT (e.g., post-renal transplant) with autonomous PTH secretion.
- A key feature of Tertiary HPT is hypercalcemia (Ca ↑) alongside markedly ↑ PTH.
- Medical management for Secondary HPT includes phosphate binders, Vitamin D analogs, and Cinacalcet.
- Surgery (e.g., subtotal parathyroidectomy) is for refractory secondary or symptomatic tertiary HPT.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

