Pelvic Floor Anatomy & Physiology - Pelvic Powerhouse

- Core Structures:
- Pelvic Diaphragm: Main support layer.
- Levator ani muscles (📌 PRI: Puborectalis, Pubococcygeus, Iliococcygeus).
- Coccygeus muscle.
- Urogenital Diaphragm: Contains external urethral sphincter.
- Fascia: Endopelvic fascia (provides visceral support).
- Innervation:
- Pudendal nerve (S2, S3, S4): Key for sphincter control & perineal sensation.
- Direct sacral branches (S3, S4) to levator ani.
- Pelvic Diaphragm: Main support layer.
- Key Functions:
- Supports pelvic organs (bladder, uterus, rectum).
- Maintains urinary and fecal continence.
- Aids in defecation, micturition, parturition, sexual function.
- Clinical Landmark: Perineal body - central fibrous anchor point.
⭐ The pudendal nerve (S2, S3, S4) is the primary motor and sensory nerve to the perineum, including the external anal and urethral sphincters.
Types of Pelvic Floor Disorders - Droops, Drips & Blocks
Pelvic floor dysfunction manifests as:
- "Droops": Pelvic Organ Prolapse (POP) - organ descent.
- "Drips": Urinary Incontinence (UI) - involuntary urine leakage.
- "Blocks": Obstructive symptoms (e.g., voiding dysfunction, constipation).
Urinary Incontinence (UI) Types:
| Type | Mechanism | Key Symptoms |
|---|---|---|
| Stress | Urethral hypermobility, Intrinsic Sphincter Deficiency (ISD) | Involuntary leakage on effort, exertion, cough, sneeze |
| Urge | Detrusor overactivity | Sudden, intense urge to urinate; often with leakage |
| Mixed | Combination of Stress & Urge | Features of both stress and urge incontinence |
| Overflow | Detrusor underactivity / Bladder Outlet Obstruction (BOO) | Constant dribbling, weak stream, incomplete bladder emptying |
| Prolapse Type | Description | Involved Structure(s) |
|---|---|---|
| Cystocele | Anterior vaginal wall prolapse (bladder) | Bladder into vagina |
| Rectocele | Posterior vaginal wall prolapse (rectum) | Rectum into vagina |
| Enterocele | Apical prolapse (small bowel herniation) | Small bowel into vagina |
| Uterine | Apical prolapse (uterus descent) | Uterus into/out of vagina |
| Vault | Apical prolapse (vaginal cuff post-hysterectomy) | Vaginal apex descent |

⭐ Stress urinary incontinence is the most common type, characterized by involuntary leakage on effort or exertion, such as coughing or sneezing.
Clinical Evaluation & Diagnosis - Decoding the Descent
⭐ The POP-Q (Pelvic Organ Prolapse Quantification) system is the standardized, objective method for describing and staging pelvic organ prolapse.
- History: Focus on symptoms (fecal incontinence (FI), obstructed defecation (ODS), bulge, pain), obstetric/surgical history.
- Physical Exam:
- Inspection: Perineal descent during Valsalva.
- Digital Rectal Exam (DRE): Resting/squeeze tone, puborectalis paradox.
- POP-Q Assessment: For prolapse staging. 📌 Key points: Aa, Ba, C, D, Gh, Pb, TVL, Ap, Bp.

- Key Investigations:
- Anorectal Manometry: Assesses sphincter pressures (e.g., resting pressure <40 mmHg suggests weakness).
- Defecography (Barium/MR): Evaluates dynamic anorectal function, rectoceles, intussusception.
- Endoanal Ultrasound (EAUS): Visualizes sphincter defects.
Management of Pelvic Floor Disorders - Repair & Restore Roundup
-
Conservative First:
- PFMT (Kegels), lifestyle (weight ↓, bladder train).
- Pessaries: For POP & SUI.
-
Medical Options:
- OAB: Anticholinergics (Oxybutynin 2.5-5mg), Mirabegron (25-50mg).
- SUI: Duloxetine (limited).
-
Surgical Interventions:
-
Table: PFD Management Approaches
Disorder Conservative Surgical Options Stress Urinary Incontinence (SUI) PFMT, pessary MUS (TVT/TOT), Burch, bulking agents Pelvic Organ Prolapse (POP) PFMT, pessary Repair (ant/post), Apical (sacrocolpopexy), Colpocleisis Fecal Incontinence (FI) Diet, PFMT, biofeed. Sphincteroplasty, SNS
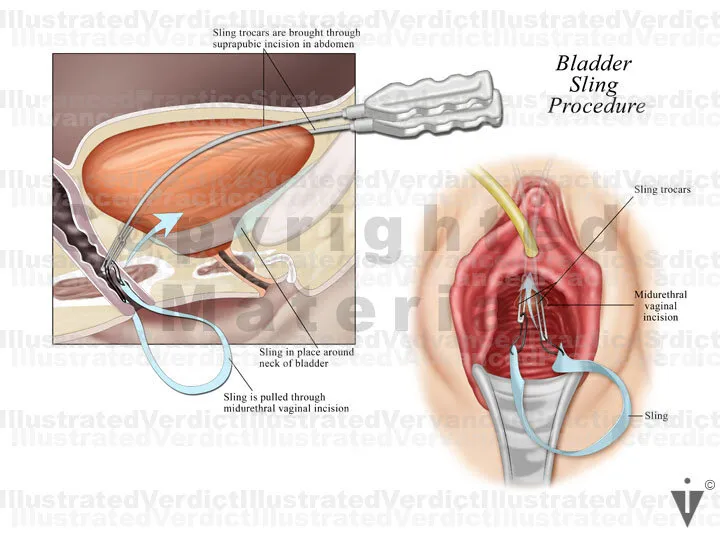
-
⭐ Pelvic floor muscle training (Kegel exercises) is the first-line conservative treatment for stress urinary incontinence and early-stage pelvic organ prolapse.
High‑Yield Points - ⚡ Biggest Takeaways
- Rectal prolapse: True full-thickness protrusion. Altemeier for frail, abdominal rectopexy for fit.
- Fecal incontinence: Anal manometry & EMG for diagnosis. Sacral Nerve Stimulation (SNS) for refractory cases.
- Obstructed defecation syndrome (ODS): Biofeedback is first-line. STARR procedure for selected anatomical defects.
- Solitary rectal ulcer syndrome (SRUS): Linked to straining, internal intussusception. Conservative management is primary.
- Anismus: Paradoxical puborectalis contraction; biofeedback is mainstay treatment.
- Rectocele: Symptomatic anterior rectal wall herniation; may require surgical repair.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

