Immediate Post-Op Care - Swift Recovery Start
- Vitals: Continuous monitoring (HR, BP, RR, SpO2); urine output > 0.5 mL/kg/hr.
- Pain: Multimodal analgesia (opioid-sparing techniques).
- Fluids: IV hydration, early transition to oral sips.
- Diet: Clear liquids post-op Day 0-1, advance as tolerated.
- Mobilization & DVT Prophylaxis:
⭐ Early ambulation (within 4-6 hours post-op) prevents VTE & atelectasis.
- Sequential Compression Devices (SCDs).
- LMWH (e.g., Enoxaparin 40mg SC OD).
- Respiratory Care: Incentive spirometry, cough & deep breathing exercises.
- Wound: Monitor for infection/leak signs (erythema, discharge, fever).
Early Complications - Acute Alert Actions
- Anastomotic Leak:
- Key signs: Tachycardia (>120 bpm), fever, abdominal pain.
- Action: Urgent CT (oral contrast).
⭐ Persistent tachycardia >120 bpm is the most sensitive early sign of an anastomotic leak; requires urgent investigation.
- Pulmonary Embolism (PE):
- Key signs: Sudden dyspnea, chest pain, tachycardia.
- Action: CTPA, anticoagulation.
- Hemorrhage (GI/Intra-abdominal):
- Key signs: Tachycardia, hypotension, ↓Hb.
- Action: Resuscitate, locate source (endoscopy/CT), intervene.
- Obstruction/Stenosis:
- Key signs: Persistent nausea, vomiting, food intolerance.
- Action: Imaging (UGI series/CT), NGT, possible endoscopy/surgery.
Dietary Progression - Phased Fueling Plan
- Stage 1 (Wk 1-2): Clear & Full Liquids
- Water, broth, sugar-free drinks, protein shakes (no lumps).
- Sip slowly: 15-30ml every 15-30 min.
- Focus: Hydration, gut rest.
- Stage 2 (Wk 2-4): Pureed Foods
- Blended/strained foods: lean protein, fruits, veg.
- High protein, low sugar/fat.
- Stage 3 (Wk 4-8): Soft Foods
- Tender, moist, easily mashed: ground meat, fish, eggs, cooked veg.
- Chew thoroughly. Small bites.
- Stage 4 (Wk 8+): Regular Texture (Modified)
- Gradual return to solids. Prioritize protein.
- Lifelong healthy eating. Avoid grazing.

⭐ Target protein intake post-bariatric surgery is 60-80g/day to preserve lean body mass.
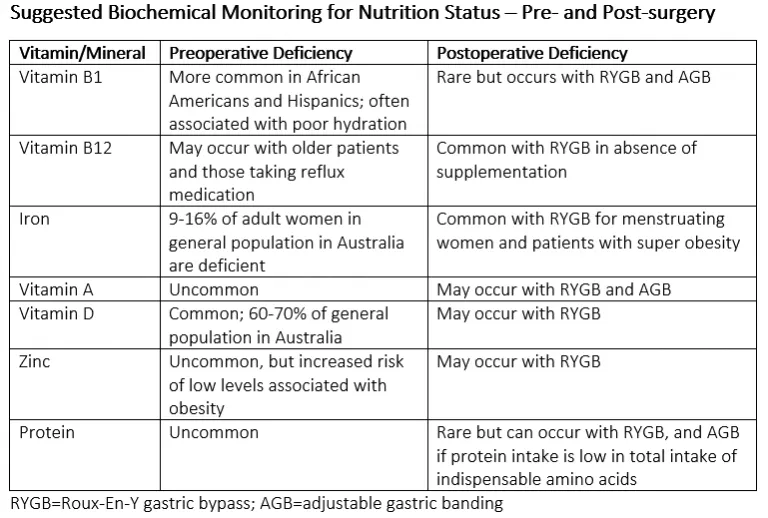
Nutritional Support - Vital Vitamin Vigil
- Lifelong multivitamin & mineral supplementation is mandatory.
- Monitor for common deficiencies:
- Iron: Often requires co-administration with Vitamin C for better absorption.
- Vitamin B12: Parenteral (IM/SC) or sublingual forms often needed, especially post-RYGB or BPD-DS.
- Vitamin D: Target serum 25(OH)D >30 ng/mL; typical dose 3000 IU/day.
- Calcium: Citrate form preferred (less acid-dependent absorption). Aim for 1200-1500 mg/day, in divided doses.
- Thiamine (B1): Crucial; prophylactic administration, especially with persistent vomiting.
- Folate, Zinc, Copper also require regular monitoring and supplementation as needed.
⭐ Wernicke's encephalopathy (thiamine deficiency) can occur with persistent vomiting; prophylactic thiamine is essential, especially in early postoperative period.
Late Issues & Follow-Up - Enduring Health Path
- Nutritional Deficiencies: Common (Fe, B12, Vit D, Ca, Folate, Thiamine). Lifelong supplementation crucial.
- Cholelithiasis: ↑ risk with rapid weight loss.
Rapid weight loss significantly increases the risk of cholelithiasis (up to 30-50%); ursodeoxycholic acid prophylaxis is often recommended for 6 months. ⭐
- Dumping Syndrome: Early (osmotic), Late (reactive hypoglycemia).
- Anastomotic Strictures, Internal Hernias: Potential surgical complications.
- Weight Regain: Requires ongoing lifestyle adherence; monitor closely.
- Follow-Up: Lifelong. Includes regular labs (vitamins, minerals), diet/exercise reinforcement, psychological support.
High‑Yield Points - ⚡ Biggest Takeaways
- Early ambulation is crucial to prevent DVT/PE.
- Lifelong multivitamin/mineral supplementation (Fe, B12, Ca, Vit D, Thiamine) is essential to prevent deficiencies.
- Manage dumping syndrome with small, frequent, low-carb, high-protein meals.
- Anastomotic leak (tachycardia, fever, pain) is a life-threatening early complication requiring prompt action.
- Strictures causing vomiting may need endoscopic dilation; marginal ulcers can occur.
- High risk of cholelithiasis post-rapid weight loss; consider UDCA. Ensure protein intake (~60-80g/day).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more