Bariatric Procedures & Metabolic Goals - Gut Reaction!
- Alters gut anatomy for weight loss & metabolic improvement.
- Key Procedures:
- Roux-en-Y Gastric Bypass (RYGB): Gold standard; restrictive & malabsorptive.
- Sleeve Gastrectomy (SG): Most common; restrictive.
- Metabolic Goals:
- Weight loss >25% total body weight.
- T2DM remission/improvement.
- Enhanced insulin sensitivity.
- Favorable gut hormone changes: ↑ GLP-1, ↑ PYY, ↓ Ghrelin (post-SG).
⭐ RYGB shows rapid T2DM improvement, often pre-weight loss, due to incretin effect & gut hormone modulation.
 oka
oka
Key Hormonal Shifts Post-Surgery - Gut Feeling Fiesta
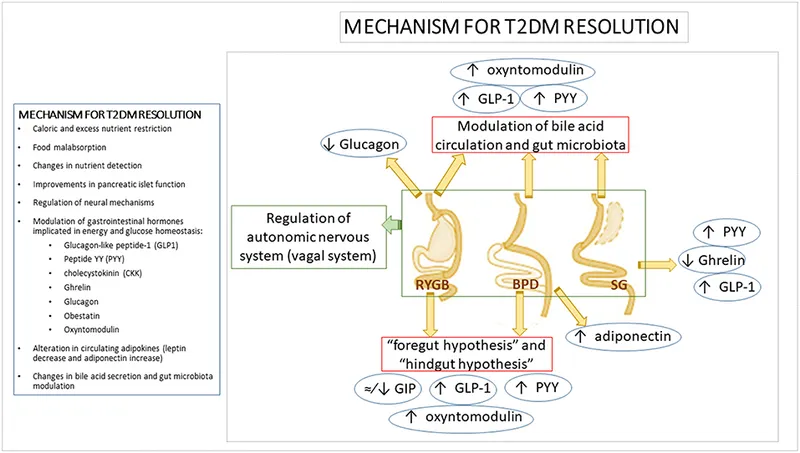 Bariatric procedures trigger major gut hormone shifts: 📌 Mnemonic: Hungry Ghrelin ↓, Full PYY & GLP-1 ↑.
Bariatric procedures trigger major gut hormone shifts: 📌 Mnemonic: Hungry Ghrelin ↓, Full PYY & GLP-1 ↑.
- GLP-1 & PYY: ↑↑ (Hindgut effect: rapid distal nutrient delivery).
- Effects: ↑ Insulin, ↓ Glucagon, ↑ Satiety, ↓ Gastric emptying (GLP-1); ↓ Appetite, ↓ Motility (PYY).
- Ghrelin ("Hunger Hormone"): ↓↓ (esp. Sleeve via fundus removal).
- Effect: ↓ Appetite.
- Leptin: ↓ (due to ↓ fat mass). Sensitivity ↑.
- Theories Explaining ↑GLP-1/PYY & Other Benefits:
- Hindgut: Rapid distal nutrient delivery → ↑GLP-1/PYY.
- Foregut: Proximal gut (duodenum) bypass → ↓putative anti-incretins.
⭐ Post-RYGB/Sleeve, marked ↑ in GLP-1 & PYY are crucial for T2DM remission.
T2DM Remission & Glucose Control - Sugar Surrender
Bariatric surgery significantly improves Type 2 Diabetes Mellitus (T2DM), often leading to remission.
- Primary Mechanisms:
- Altered gut hormone secretion: ↑ Glucagon-Like Peptide-1 (GLP-1), ↑ Peptide YY (PYY).
- ↓ Ghrelin levels (especially post-SG/RYGB).
- Enhanced insulin sensitivity in liver and peripheral tissues.
- Improved β-cell function and mass preservation.
- Remission Rates (approximate):
- Roux-en-Y Gastric Bypass (RYGB): 60-80%.
- Sleeve Gastrectomy (SG): 50-70%.
- Laparoscopic Adjustable Gastric Banding (LAGB): 20-50%.
- Positive Predictors for Remission:
- Shorter T2DM duration (<5 years).
- Lower pre-operative HbA1c.
- Non-insulin dependent T2DM pre-op.
⭐ Rapid improvement in glycemic control, often within days of RYGB, can occur before significant weight loss, attributed to acute hormonal changes (incretin effect).

Lipid Metabolism & Liver Health - Fat Farewell
- Dyslipidemia Correction:
- Significant ↓ in Triglycerides (TGs) by ~50%.
- ↑ HDL cholesterol by ~10-20%.
- LDL cholesterol: often ↓; shift to larger, less atherogenic particles.
- NAFLD/NASH Resolution:
- Dramatic improvement in Non-Alcoholic Fatty Liver Disease (NAFLD) and Non-Alcoholic Steatohepatitis (NASH).
- ↓ Hepatic steatosis, inflammation, and fibrosis.
- Normalization of liver enzymes (ALT, AST).
⭐ Bariatric surgery can lead to NASH resolution in up to 85% of patients and fibrosis regression in ~30-50%.
Micronutrients & Bone Integrity - Vitamin Vigilance
- Key Deficiencies:
- Iron: Most common (RYGB/BPD-DS): malabsorption, ↓acid. Screen regularly.
- Vit B12: ↓IF (RYGB/SG), ↓acid. Neuropathy risk.
- Vit D & Ca: Malabsorption (RYGB/BPD-DS) → 2° HPT, ↑bone loss, osteoporosis.
- Thiamine (B1): Deficiency (vomiting) → Wernicke's (neuro emergency).
- Folate, Cu, Zn also monitored.
- Bone Integrity:
- ↑ Long-term fracture risk.
- Mechanisms: Malabsorption, hormonal shifts (↑PTH), ↓load.
⭐ Iron deficiency: most common post-bariatric surgery, screen routinely.
- Management: Lifelong supplementation & monitoring crucial for prevention.
High‑Yield Points - ⚡ Biggest Takeaways
- RYGB & Sleeve Gastrectomy show highest T2DM remission rates, often independent of weight loss.
- Key hormonal changes: ↑ GLP-1 & PYY (improve glucose control, satiety); ↓ Ghrelin (reduces hunger, mainly post-sleeve).
- Significant improvement in dyslipidemia (↓ Triglycerides, ↓ LDL, ↑ HDL) & hypertension.
- Alterations in gut microbiota & bile acid metabolism contribute to metabolic benefits.
- Nutrient malabsorption (iron, B12, Ca, Vit D) is a crucial long-term metabolic consequence requiring monitoring.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

