TF-CBT Fundamentals - Trauma Tamer Toolkit
- Evidence-based psychotherapy for trauma in children & adolescents (3-18 years) and their caregivers.
- Addresses emotional, behavioral, and cognitive difficulties post-trauma.
- Core components: Psychoeducation, parenting skills, relaxation, affect regulation, cognitive coping, trauma narrative, gradual exposure, conjoint sessions, safety planning.
- Goal: Reduce PTSD, depression, anxiety; improve coping & family communication.
⭐ TF-CBT significantly involves non-offending parents/caregivers in treatment to support the child's recovery and improve family dynamics.
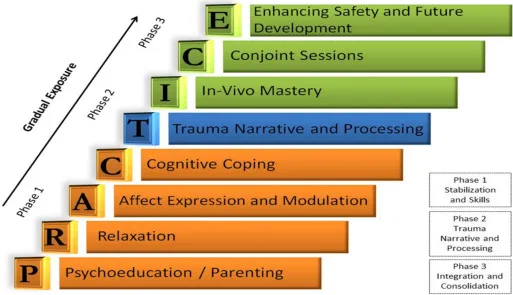
PRACTICE Model - Healing Alphabet Soup
TF-CBT employs the 📌 PRACTICE mnemonic, a structured, evidence-based psychotherapy model for children and adolescents exposed to trauma. Each letter signifies a core therapeutic component:
| Component | Focus |
|---|---|
| P - Psychoeducation & Parenting Skills | Educating child/caregivers on trauma's impact; effective parenting (praise, behavior management). |
| R - Relaxation Skills | Teaching techniques (deep breathing, PMR, mindfulness) to manage physiological arousal, anxiety. |
| A - Affective Modulation | Helping child identify, express, regulate emotions; developing coping for difficult feelings. |
| C - Cognitive Coping | Addressing maladaptive thoughts via Cognitive Triangle (Thoughts-Feelings-Behaviors); cognitive restructuring. |
| T - Trauma Narrative & Processing | Gradually developing and processing a detailed trauma account to reduce associated distress. |
| I - In Vivo Exposure | Systematically confronting feared, trauma-related situations/reminders safely and gradually. |
| C - Conjoint Child-Parent Sessions | Child shares trauma narrative with parent; improving family communication and mutual support. |
| E - Enhancing Safety & Future Development | Creating safety plans; building skills for future stressors, healthy relationships, and positive coping. |
Mechanism Unveiled - How Healing Happens
TF-CBT facilitates healing by targeting key trauma-induced changes:
- Cognitive Restructuring: Modifies distorted trauma cognitions (e.g., self-blame, danger overestimation), promoting realistic thinking.
- Emotional Desensitization & Regulation: Gradual exposure to trauma cues reduces fear (habituation). Teaches skills to manage emotional distress.
- Trauma Narrative Processing: Develops a coherent trauma narrative, integrating memories, thoughts, and feelings, reducing their emotional power.
- Adaptive Skills Application: Replaces maladaptive behaviors (e.g., avoidance) with positive coping strategies; reinforces safety.
⭐ TF-CBT's power lies in simultaneously addressing distorted cognitions about the trauma and maladaptive emotional/behavioral responses through integrated techniques.
Clinical Impact - Real-World Wins
- High Efficacy: Gold standard for youth PTSD, anxiety, depression post-trauma.
- Strong Evidence: Most empirically supported treatment for traumatized children/adolescents.
- Symptom Reduction: Significant ↓ in PTSD, shame, guilt, externalizing behaviors.
- Skill Enhancement: Improves coping skills, emotional regulation, and positive parent-child interactions.
- Broad Applicability: Effective for various trauma types (abuse, disasters).
- Superior Outcomes: Often outperforms other non-trauma-focused therapies.
- Long-Term Gains: Sustained improvement, reduces risk of chronic issues.
⭐ TF-CBT shows robust efficacy, often achieving >50% reduction in PTSD symptom severity in children and adolescents_._
High‑Yield Points - ⚡ Biggest Takeaways
- TF-CBT is a first-line treatment for children & adolescents with PTSD post-trauma.
- Core: Psychoeducation, coping skills (relaxation, affect, cognitive), trauma narrative, parental involvement.
- Trauma narrative: Gradual exposure and processing of traumatic memories.
- Cognitive restructuring targets unhelpful trauma-related thoughts and beliefs.
- Caregiver participation is integral for skill reinforcement and safety.
- Typically 12-16 structured sessions.
- Highly effective for reducing PTSD symptoms and improving youth functioning.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

