OUD Basics - The Poppy Problem
- Definition: A problematic pattern of opioid use leading to clinically significant impairment or distress (DSM-5). ICD-11: Opioid Dependence. Key features: craving, tolerance, withdrawal.
- Common Opioids:
- Natural: Opium, Morphine, Codeine.
- Semi-synthetic: Heroin (diacetylmorphine), Buprenorphine, Oxycodone.
- Synthetic: Fentanyl, Methadone, Tramadol, Pethidine.
- Routes of Administration: Oral, intranasal (snorting), intravenous (IV), inhalation (smoking, e.g., "chasing the dragon").
- Indian Epidemiology (AIIMS, 2019): Approx. 2.8% of population (10-75 yrs) reported past-year opioid use; ~2.1% are users of concern. Heroin is the most common illicit opioid.

⭐ Heroin (diacetylmorphine) is rapidly hydrolyzed to 6-monoacetylmorphine (6-MAM) and then to morphine in the body, both of which are active. This contributes to its potent and rapid effects.
Brain Hijack - How Opioids Work
Opioids bind to μ, κ, δ receptors, primarily Gi-coupled.
- Receptor Functions:
- μ (Mu): Euphoria, analgesia, respiratory depression, miosis, ↓GI motility. 📌 Key for analgesia & addiction.
- κ (Kappa): Spinal analgesia, dysphoria, sedation, miosis.
- δ (Delta): Analgesia, antidepressant/anxiolytic effects.
- Cellular Mechanism:
- ↓Adenylyl cyclase → ↓cAMP.
- Postsynaptic: ↑K+ efflux → hyperpolarization.
- Presynaptic: ↓Ca2+ influx → ↓neurotransmitter release.
- Reward Pathway Activation:
- VTA: μ-agonism inhibits GABAergic neurons.
- → Disinhibition of VTA dopamine neurons.
- → ↑Dopamine in Nucleus Accumbens (NAc) → euphoria & reinforcement.
- Neuroadaptation:
- Tolerance: ↓Receptor response → ↓drug effect.
- Dependence: Physiological adaptation; withdrawal on cessation.
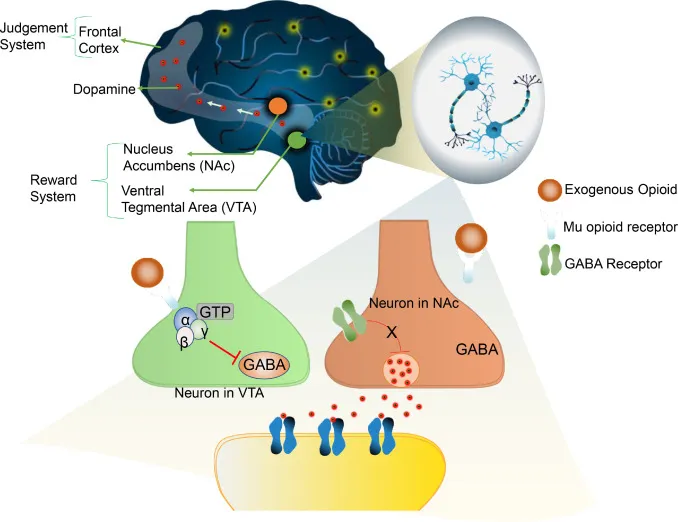
⭐ The μ (mu) opioid receptor is primarily responsible for euphoria and respiratory depression.
Signs & Symptoms - Highs and Lows
Opioid Intoxication vs. Withdrawal
| Feature | Intoxication ("High") | Withdrawal ("Low") |
|---|---|---|
| Key Triad | Miosis, Resp. Depression, Coma | - |
| CNS | Euphoria, drowsiness | Dysphoria, anxiety, insomnia, yawning |
| Pupils | Miosis (pinpoint) | Mydriasis (dilated) |
| GIT | Constipation | N/V/D, cramps |
| Autonomic | ↓HR, ↓BP (severe) | ↑HR, ↑BP, sweating, piloerection, lacrimation, rhinorrhea, fever |
| Muscles | - | Myalgia, arthralgia |
- 📌 Mnemonic: e.g., 'MY LEGS CRAMP' (Myalgia, Yawning, Lacrimation, Emesis, Gooseflesh, etc.)
- COWS Scale (Severity): Mild **5-12**, Mod **13-24**, Mod Sev **25-36**, Sev **>36**.
- ⭐ > Piloerection ("gooseflesh") during opioid withdrawal is the origin of the term "cold turkey".
Flowchart: Opioid Withdrawal Timeline
Diagnostic Criteria (DSM-5/ICD-11)
- Problematic opioid use → impairment/distress. ≥2 criteria/12mo (e.g., tolerance, withdrawal, craving, loss of control).
Treatment Toolkit - Road to Recovery
-
Pharmacological Management
-
Detoxification:
- Clonidine, lofexidine for autonomic symptoms.
- Gradual opioid agonist taper (e.g., methadone, buprenorphine).
-
Maintenance Therapy:
Drug MOA Key Pro(s) Key Con(s) Critical Dosing/Timing Methadone Full $\mu$-agonist Effective, ↓craving QTc risk, OD risk Start 20-30mg, supervised Buprenorphine Partial $\mu$-agonist; $\kappa$-antagonist Ceiling effect (safer), ↓stigma, sublingual Precipitated withdrawal Start COWS ≥8-12; often +Naloxone Naltrexone $\mu$-antagonist Non-addictive, oral/IM Needs full detox, hepatotoxicity Opioid-free 7-10 days
-
-
Non-Pharmacological Interventions: Key psychosocial interventions include:
- Cognitive Behavioral Therapy (CBT)
- Motivational Interviewing (MI)
- Contingency Management (CM)
- Support groups (e.g., Narcotics Anonymous - NA)
-
Harm Reduction Strategies: Strategies to minimize negative consequences:
- Needle and syringe programs (NSPs)
- Distribution of naloxone kits for overdose reversal
⭐ Buprenorphine's ceiling effect on respiratory depression makes it safer in overdose than full agonists like methadone.
High‑Yield Points - ⚡ Biggest Takeaways
- Opioid intoxication triad: pinpoint pupils (miosis), respiratory depression, altered mental status/coma.
- Naloxone is the life-saving antidote for acute overdose, rapidly reversing respiratory depression.
- Opioid withdrawal: severe flu-like symptoms (lacrimation, rhinorrhea, mydriasis, piloerection, muscle aches); not typically life-threatening.
- Methadone (long-acting agonist) and buprenorphine (partial agonist) are crucial for Opioid Substitution Therapy (OST/MAT).
- Naltrexone (antagonist) aids relapse prevention in detoxified individuals.
- Clonidine alleviates autonomic hyperactivity during withdrawal.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

