AUD: Definition & Epidemiology - The Indian Pint‑demic
- Definition (DSM-5): Problematic alcohol use; ≥2 of 11 criteria in 12 months, causing distress/impairment.
- Indian Prevalence (NDDUS 2019, 10-75 yrs):
- Current users: ~14.6% (~160 million).
- Dependence: ~2.7% (~29 million); M:F ratio ~17:1.
- Higher in e.g., Arunachal Pradesh, Tripura, Punjab.
- Key Risk Factors: Genetic predisposition, early initiation, peer pressure, comorbid mental health conditions.
⭐ In India, ~40% of road traffic accidents are attributable to alcohol use (NDDUS 2019).
AUD: Neurobiology & Pathophysiology - Brain Under the Influence
- Acute Effects: Enhances GABAergic (inhibitory) transmission (sedation, anxiolysis); inhibits NMDA glutamatergic (excitatory) transmission. Releases dopamine in mesolimbic pathway (reward).
- Chronic Use & Neuroadaptation:
- ↓ GABA-A receptor function & density.
- ↑ NMDA receptor density & sensitivity (upregulation).
- Dysregulation of dopamine, serotonin, and opioid peptide systems.
- Withdrawal Syndrome: Results from abrupt cessation. Characterized by CNS hyperexcitability (↓GABA, ↑glutamate activity) → tremors, anxiety, seizures, delirium tremens.
- Kindling: Repeated withdrawal episodes sensitize the brain, lowering seizure threshold.

⭐ Chronic alcohol exposure leads to a hyperexcitable state upon cessation due to GABA receptor downregulation and NMDA receptor upregulation, underlying withdrawal symptoms like seizures and DTs.
AUD: Clinical Features & Diagnosis - Signs of the Spirits
- Intoxication: Slurred speech, incoordination, nystagmus, impaired memory.
- Withdrawal (6-24h onset):
- Autonomic hyperactivity (↑HR >100, sweating)
- Tremor, insomnia, N/V, anxiety
- Hallucinations (visual/tactile)
- Seizures ("rum fits", 12-48h)
- Delirium Tremens (DTs, 48-96h): Disorientation, agitation, fever, ↑autonomic signs. Emergency!
- Diagnosis (DSM-5): ≥2 criteria/12mo (impaired control, social issues, risky use, tolerance/withdrawal).
- Severity: Mild (2-3), Moderate (4-5), Severe (≥6).
- Markers: ↑GGT, ↑MCV, AST:ALT >2. CDT for chronic use.
⭐ Wernicke's Encephalopathy triad: Confusion, Ataxia, Ophthalmoplegia (📌 CAO). Often incomplete.
AUD: Complications - The Hangover's Harm
- Neuro: Wernicke-Korsakoff (Thiamine def.), cerebellar degen., neuropathy, seizures, hepatic encephalopathy.
- GI: Gastritis, PUD, Mallory-Weiss, varices, pancreatitis, ALD (steatosis, hepatitis, cirrhosis → HCC).
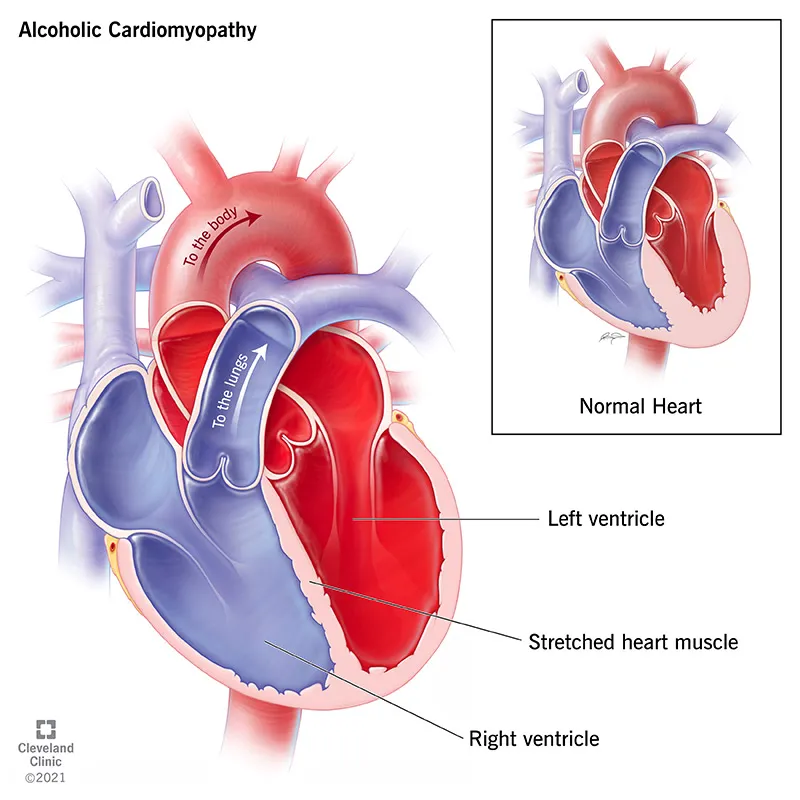
- CVS: Alcoholic cardiomyopathy, HTN, arrhythmias (holiday heart).
- Psych: Depression, anxiety, ↑suicide risk, psychosis.
- Heme: Macrocytosis, thrombocytopenia.
- Metabolic: Hypoglycemia, alcoholic ketoacidosis.
- Other: Fetal Alcohol Syndrome (FAS).
⭐ Wernicke's encephalopathy triad: Confusion, Ataxia, Ophthalmoplegia (📌 CAO). Reversible with IV thiamine before glucose administration to prevent precipitation/worsening of Wernicke's.
AUD: Management - Path to Sobriety
- Withdrawal Management:
- Benzodiazepines (e.g., Chlordiazepoxide, Lorazepam): Symptom-triggered or fixed-schedule, guided by CIWA-Ar (target < 8-10).
- Thiamine 100mg IV/IM daily for 3-5 days (prevents Wernicke-Korsakoff).
- Supportive care: IV fluids, electrolytes.
- Maintenance (Relapse Prevention):
- Naltrexone (50mg OD / long-acting IM): Reduces craving & heavy drinking.
- Acamprosate: Supports abstinence by reducing protracted withdrawal.
- Disulfiram: Aversive therapy (aldehyde dehydrogenase inhibitor). ⚠️ Monitor LFTs.
- Psychosocial therapies (AA, CBT, MI) are essential adjuncts.
⭐ Naltrexone can be initiated while still drinking to reduce consumption; Acamprosate/Disulfiram require abstinence.
High‑Yield Points - ⚡ Biggest Takeaways
- CAGE questionnaire (Cut down, Annoyed, Guilty, Eye-opener) is a key screening tool.
- Delirium tremens (DT): severe, life-threatening withdrawal, peaks 48-96 hours post-cessation.
- Wernicke-Korsakoff syndrome: from thiamine (B1) deficiency; Wernicke's (reversible triad), Korsakoff's (irreversible amnesia).
- Key drugs: Disulfiram (aversive), Naltrexone (↓ cravings), Acamprosate (maintains abstinence).
- Elevated GGT & MCV are common biochemical markers of chronic alcohol use.
- Acute alcohol withdrawal: manage with benzodiazepines (e.g., chlordiazepoxide, lorazepam).
- Fetal Alcohol Syndrome (FAS): distinct facial dysmorphism, growth deficits, CNS issues.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

