Definition & Epidemiology - Mind's Endless Loop
- Obsessions: Recurrent, persistent, intrusive, unwanted thoughts, urges, or images causing significant anxiety or distress.
- Compulsions: Repetitive behaviors (e.g., hand washing) or mental acts (e.g., counting) performed to neutralize obsessions or reduce distress; often excessive or not realistically connected.
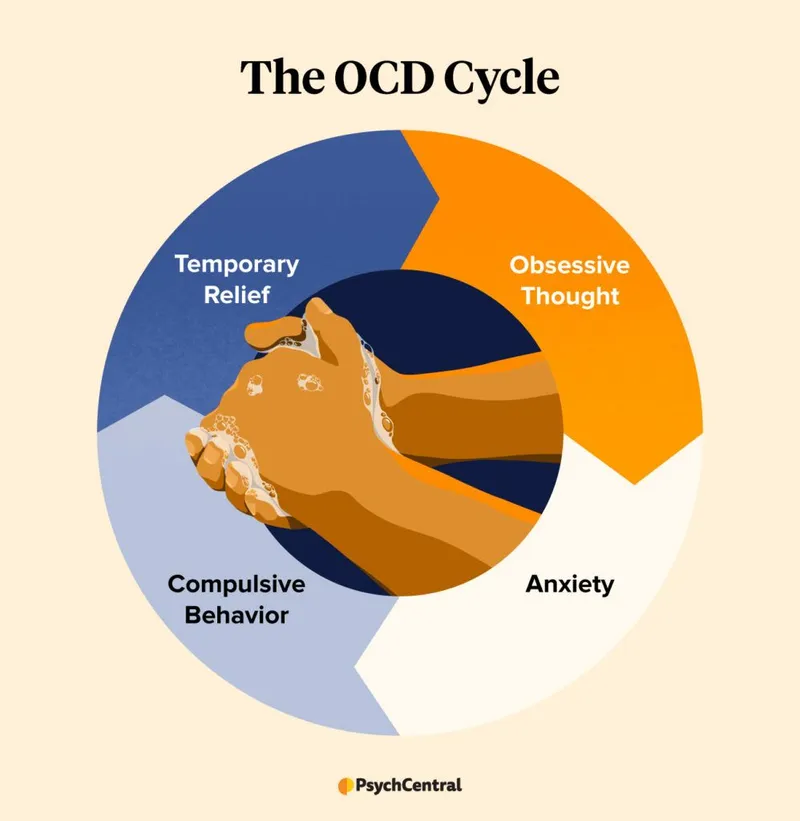
- Core Cycle: Obsession → Anxiety → Compulsion → Temporary Relief.
- Epidemiology:
- Lifetime prevalence: 2-3%.
- Common Age of Onset: Adolescence/early adulthood.
⭐ OCD has a bimodal age of onset, with peaks in early adolescence and early adulthood.
- Gender Distribution: Adults M=F; Childhood M>F.
Clinical Features - Ritual Realm Rules
Obsessions: recurrent, persistent thoughts/urges/images. Compulsions: repetitive behaviors/mental acts responding to obsessions.
- Common Patterns:
Obsessions (Thoughts/Urges) Compulsions (Behaviors/Mental Acts) Contamination (germs, dirt) Washing/Cleaning (hands, objects) Pathological Doubt (uncertainty) Checking (locks, appliances) Symmetry/Exactness (order) Ordering/Arranging (items precisely) Aggressive/Horrific Thoughts (harm) Mental Rituals (praying, counting silently) Unwanted Sexual Thoughts Repeating Actions (touching, tapping) - 📌 Mnemonic for obsessions: 'Can't Stop Doubting Harm' (Contamination, Symmetry, Doubt, Harm/Aggression).
- Specifiers:
- Insight: Good/fair, poor, absent/delusional.
- Tic-related: Current/past tic disorder.
⭐ The most common pattern is contamination obsessions with cleaning compulsions.
Etiology & Pathophysiology - Circuit Overload
- Neurobiological Factors:
- Serotonin (5-HT) dysregulation: Implicated as a key neurotransmitter.
- CSTC Circuit Hyperactivity: Overactivity in Cortico-Striato-Thalamo-Cortical loops.
- Key areas: Orbitofrontal Cortex (OFC), Anterior Cingulate Cortex (ACC), and Striatum.

⭐ Dysfunction in the Cortico-Striato-Thalamo-Cortical (CSTC) pathways is a key neurobiological finding in OCD.
- Genetic Factors:
- ↑ Monozygotic twin concordance suggests genetic link.
- Family history is a significant risk factor.
- PANDAS:
- Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcal infections; linked to childhood OCD onset.
- Psychological Theories:
- Cognitive: e.g., inflated responsibility, thought-action fusion.
- Behavioral: e.g., Mowrer's two-factor theory (classical & operant conditioning).
Diagnosis & DDx - Detective's Toolkit
-
DSM-5 Criteria:
- Presence of obsessions, compulsions, or both.
- Time-consuming (>1 hr/day) OR cause significant distress/impairment.
- Not attributable to substance/medical condition.
- Not better explained by another mental disorder.
-
Assessment: Y-BOCS (Gold Standard severity):
- 0-7 Subclinical, 8-15 Mild, 16-23 Moderate, 24-31 Severe, 32-40 Extreme.
-
DDx:
- Anxiety (GAD), Depression.
- OCPD (vs. OCD's ego-dystonia).
- Psychosis.
- BDD, Hoarding, Trichotillomania, Excoriation.
⭐ OCD is ego-dystonic, meaning individuals perceive their obsessions/compulsions as intrusive and unwanted, unlike OCPD traits which are ego-syntonic.
Management - Freedom Fighters
- Pharmacotherapy:
- First-line: SSRIs (e.g., Fluoxetine, Fluvoxamine, Sertraline) at higher doses & longer duration than depression (trial 8-12 weeks).
- Second-line/SSRI non-responders: Clomipramine (TCA) - highly effective.
- Augmentation (treatment resistance): Antipsychotics (e.g., Risperidone), Memantine (investigational).
- Psychotherapy:
- Cognitive Behavioral Therapy (CBT) with Exposure and Response Prevention (ERP) is gold standard.
⭐ Exposure and Response Prevention (ERP) is the most effective form of psychotherapy for OCD, often used in conjunction with SSRIs.
- Other Treatments (Refractory OCD):
- Deep Brain Stimulation (DBS), Transcranial Magnetic Stimulation (TMS).
- 📌 Mnemonic: 'Effective OCD Meds: Some People Choose CBT First' (SSRIs, Psychotherapy/ERP, Clomipramine, CBT, Fluvoxamine).
High‑Yield Points - ⚡ Biggest Takeaways
- OCD features ego-dystonic obsessions (intrusive thoughts) and compulsions (repetitive acts).
- Common obsessions: contamination, doubt, symmetry; Compulsions: washing, checking, ordering.
- Compulsions aim to reduce distress from obsessions; often not realistically linked to feared event.
- Serotonin dysregulation is a key neurobiological factor.
- Treatment: SSRIs (high dose, long duration) and Exposure and Response Prevention (ERP) are first-line.
- Consider PANDAS for acute childhood onset; Y-BOCS assesses severity_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

