CBT Basics for OCD - Unraveling OCD Knots
- Goal: Reduce distress & functional impairment from obsessions & compulsions.
- Theoretical Underpinning:
- Intrusive thoughts are normal; misinterpretations (e.g., thought-action fusion, inflated responsibility) cause distress.
- Compulsions are learned behaviours to ↓ anxiety, but paradoxically maintain OCD by preventing disconfirmation of fears.
- Key Elements:
- Psychoeducation: Understanding the OCD cycle & CBT rationale.
- Cognitive Techniques: Identifying & challenging distorted thoughts (e.g., overestimation of threat, perfectionism).
- Behavioural Techniques: Primarily Exposure and Response Prevention (ERP).
- Mechanism: Habituation to anxiety; learning that feared consequences don't occur or are manageable.
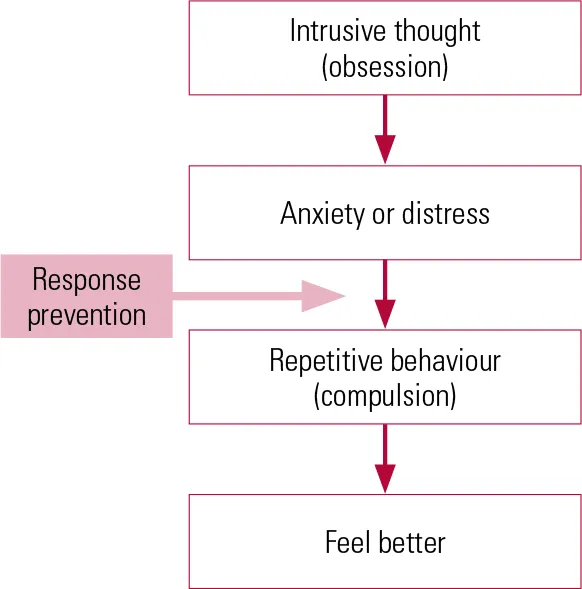
⭐ CBT, particularly incorporating Exposure and Response Prevention (ERP), is the first-line, evidence-based psychological treatment for OCD with the strongest efficacy.
ERP Deep Dive - Facing the Fear Monster
- Core: Systematically confront feared stimuli/thoughts (Exposure) while actively resisting compulsive rituals/avoidance (Response Prevention). Goal: Extinguish conditioned anxiety & sever the obsession-compulsion link.
- Mechanism:
- Habituation: Anxiety ↓ with prolonged, non-escaped exposure, leading to reduced fear response over time.
- Inhibitory Learning: Forms new, safer memories that compete with original fear associations.
- Process:
- 1. Psychoeducation & Hierarchy:
- Explain ERP rationale; collaborative goal setting.
- Create fear hierarchy (SUDS 0-100); start SUDS 40-60.
- 2. Exposure Sessions:
- Gradual & repeated: In vivo (real-life), imaginal, interoceptive.
- Prolonged duration: typically 45-90 min.
- 3. Response Prevention (RP):
- Strictly block/delay rituals & all avoidance. Absolutely critical.
- 4. Homework:
- Daily self-exposure & RP tasks for generalization.
- 1. Psychoeducation & Hierarchy:
- 📌 Mnemonic: "FACE"
- Fear hierarchy
- Approach feared stimuli
- Cease rituals
- Expect anxiety to decrease
⭐ ERP is considered the gold standard psychological treatment for OCD, demonstrating superior long-term efficacy compared to pharmacotherapy alone in many cases.

Cognitive Strategies - Rewiring Worries
- Aim: Modify distorted thoughts & beliefs fueling OCD; complements ERP.
- Targets (Dysfunctional Beliefs):
- Inflated Responsibility: Exaggerated role in causing/preventing harm.
- Thought-Action Fusion (TAF):
- Moral: Bad thought = bad action.
- Likelihood: Bad thought ↑ event probability.
- Overestimation of Threat: Exaggerating danger likelihood/severity.
- Perfectionism: Intolerance for errors.
- Intolerance of Uncertainty: Difficulty with ambiguity.
- Techniques:
- Psychoeducation: Normalizing intrusive thoughts.
- Identifying & Challenging Thoughts: Using thought records.
- Cognitive Restructuring: Socratic questioning, evidence analysis.
- Behavioral Experiments: Testing belief validity.
- Pie Chart Technique: Re-attributing responsibility.

⭐ Thought-Action Fusion (TAF) is a key cognitive distortion in OCD, where thinking an unwanted thought is equated with the action itself (moral TAF) or believed to increase its likelihood (likelihood TAF).
CBT Application & Outcomes - OCD Management Pro
- Core: Exposure & Response Prevention (ERP) pivotal; Cognitive Restructuring targets distorted thoughts.
- Sessions: 12-20 weekly; therapist-guided ERP. Homework crucial for generalization.
- Efficacy: High; 50-70% symptom reduction.
- Relapse Prevention: Maintenance plan, booster sessions, ongoing skill use.
- Special Populations: Adaptations for children, those with comorbidities.
⭐ ERP is the cornerstone of CBT for OCD, directly targeting the maintenance of obsessions and compulsions.
High-Yield Points - ⚡ Biggest Takeaways
- Exposure and Response Prevention (ERP) is the cornerstone of CBT for OCD.
- ERP involves gradual exposure to feared stimuli and preventing compulsive rituals.
- Cognitive restructuring challenges maladaptive thoughts (e.g., inflated responsibility, thought-action fusion).
- Homework assignments are crucial for generalizing skills and ensuring treatment adherence.
- CBT aims to reduce distress and functional impairment, not necessarily eliminate all obsessions.
- Habit Reversal Training (HRT) is often used for comorbid tics and Body-Focused Repetitive Behaviors (BFRBs).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

