SAD Basics - Sunny Day Blues
- Definition: Recurrent Major Depressive Disorder (MDD) exhibiting a regular seasonal pattern of onset and remission.
- Subtypes:
- Winter-pattern (most common): Fall/winter onset. Atypical symptoms: hypersomnia, overeating, weight gain, carbohydrate craving.
- Summer-pattern (less common): Spring/summer onset. Symptoms: insomnia, poor appetite, weight loss, agitation.
- Epidemiology:
- Prevalence: 1-10%, varies by geography (e.g., higher in Alaska vs. Florida).
- Age of onset: Typically 20-30 years.
- Gender: More common in women (♀:♂ ≈ 4:1).
- Key Risk Factors:
- Family history of SAD or other mood disorders.
- Living at higher latitudes (reduced sunlight exposure).
⭐ SAD prevalence increases with distance from the equator.
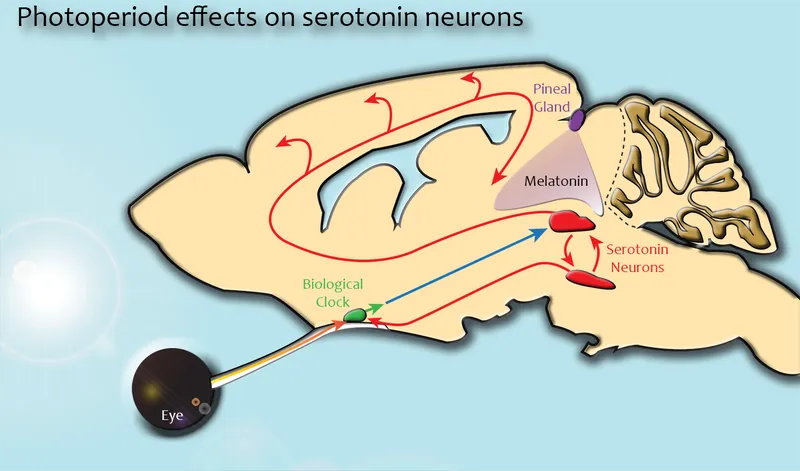
Pathophysiology - The Gloom Creators
- Melatonin Dysregulation:
- Phase-delay theory: Melatonin release delayed in winter, causing circadian misalignment with sleep/wake cycle.
- Altered total melatonin secretion.
- Serotonin (5-HT) Pathway Changes:
- ↓ Brain serotonin levels or transporter (SERT) activity, especially in winter.
- SERT gene polymorphism (e.g., 5-HTTLPR) associated with vulnerability.
- Vitamin D Deficiency:
- Reduced sunlight exposure leads to ↓ Vitamin D, impacting serotonin synthesis and mood regulation.
- Genetic Factors:
- Significant heritability; polymorphisms in genes related to circadian rhythms and serotonin pathways.
- Neurotransmitter Imbalances:
- Dopamine and norepinephrine systems may also be dysregulated.
📌 Mnemonic: 'SAD M&Ms': Serotonin, Melatonin, Morning light.
⭐ The phase-delay hypothesis of melatonin secretion is a key theory in winter-pattern SAD.
Clinical & Diagnosis - Seasonal Signs
DSM-5 Criteria (MDD with Seasonal Pattern):
- Regular temporal link: MDE onset & full remission at predictable times of year (e.g., fall onset, spring remission).
- Minimum 2 years: Two such MDEs in consecutive years, no non-seasonal MDEs during this period.
- Seasonal MDEs significantly outnumber any non-seasonal MDEs over lifetime.
⭐ Atypical depressive symptoms like carbohydrate craving and hypersomnia are characteristic of winter-pattern SAD.
Symptom Patterns:
| Feature | Winter-Pattern SAD (Atypical Features) | Summer-Pattern SAD |
|---|---|---|
| Sleep | Hypersomnia (↑) | Insomnia (↓) |
| Appetite | Overeating (↑), carb craving | Poor appetite (↓) |
| Weight | Weight gain (↑) | Weight loss (↓) |
| Energy | Fatigue, anergia (↓) | Agitation, anxiety |
| Social | Withdrawal | Irritability, restlessness |
- MDD (non-seasonal)
- Bipolar disorder
- Hypothyroidism
- Chronic fatigue syndrome
- Vitamin D deficiency
Management - Sunshine Strategies

- Light Therapy (Phototherapy): First-line for winter SAD.
- Standard regimen: 10,000 lux exposure for 30 minutes daily, ideally in the morning.
- Mechanism: Corrects circadian phase delay.
- Side effects: Generally mild; may include eyestrain, headache, nausea, or insomnia.
- Pharmacotherapy:
- SSRIs (e.g., fluoxetine, sertraline): Effective for SAD symptoms.
- Bupropion XL: Can be initiated prophylactically before autumn.
- Psychotherapy:
- Cognitive Behavioral Therapy for SAD (CBT-SAD): Specifically adapted, as effective as light therapy.
- Lifestyle Modifications:
- Regular physical exercise.
- Maximize natural sunlight exposure.
- Vitamin D supplementation if deficiency is present.
- Maintain good sleep hygiene.
⭐ Morning light therapy is the cornerstone of treatment for winter SAD, aiming to correct the circadian phase delay.
High-Yield Points - ⚡ Biggest Takeaways
- Seasonal Pattern: Recurrent depression, typically winter onset and spring/summer remission.
- DSM-5 Criteria: At least two years of seasonal episodes, outnumbering non-seasonal ones.
- Atypical Symptoms: Common, including hypersomnia, ↑ appetite/weight gain, and carbohydrate craving.
- Pathophysiology: Involves melatonin dysregulation, serotonin dysregulation, and circadian rhythm shifts.
- First-line Treatment: Light therapy (phototherapy).
- Pharmacotherapy: SSRIs (e.g., fluoxetine) and bupropion are also effective options.
- Geography: More prevalent at higher latitudes due to reduced sunlight.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

