Introduction & Epidemiology - Cyclo‑Lite Intro
- A chronic, fluctuating mood disorder; a milder form of bipolar disorder.
- Features numerous periods of subsyndromal hypomanic symptoms and subsyndromal depressive symptoms.
- Duration: At least 2 years (adults), 1 year (children/adolescents); symptom-free periods ≤ 2 months.
- Lifetime prevalence: ~0.4% - 1%.
- Onset: Typically adolescence or early adulthood.
- ⭐ > High risk (15-50%) of progression to Bipolar I or II Disorder.
Clinical Presentation - Up‑Down Rollercoaster
- Chronic, fluctuating mood for ≥ 2 years (adults) / ≥ 1 year (children/adolescents).
- Many periods with hypomanic symptoms (not meeting full criteria for a hypomanic episode).
- Many periods with depressive symptoms (not meeting full criteria for a major depressive episode).
- Symptoms present for at least half the time during this overall period.
- Symptom-free intervals do not exceed 2 months at a time.
- Full criteria for major depressive, manic, or hypomanic episodes have never been met.
- Causes clinically significant distress or impairment in social, occupational, or other important areas of functioning.
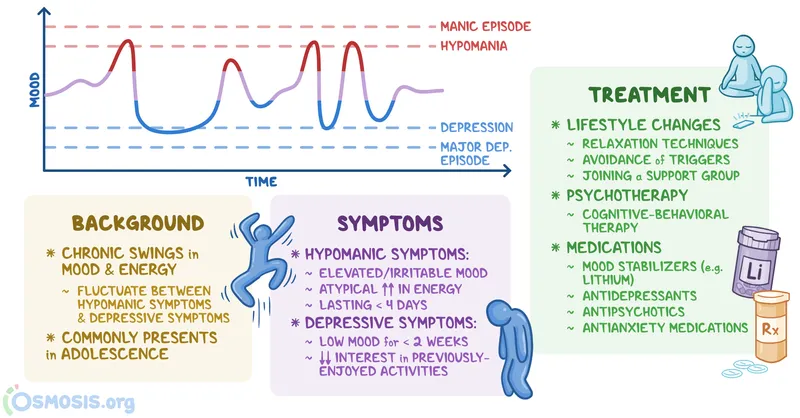
⭐ Consider cyclothymia in patients with long-standing "moodiness" or perceived unstable personality, especially if they don't meet criteria for other specific mood disorders.
Diagnostic Criteria (DSM-5) - Rulebook Reveal
- Numerous periods with hypomanic symptoms (not meeting full criteria for hypomanic episode) AND numerous periods with depressive symptoms (not meeting full criteria for major depressive episode).
- Duration: At least 2 years (adults) / 1 year (children/adolescents).
- Symptom-free intervals: Not longer than 2 months during the 2-year (or 1-year) period.
- Criteria for major depressive, manic, or hypomanic episode have never been met.
- Not better explained by another mental disorder (e.g., schizoaffective disorder, schizophrenia).
- Symptoms cause clinically significant distress or impairment.
⭐ Symptoms must be present for at least half the time during the initial 2-year (or 1-year) period, and the individual has not been without symptoms for more than 2 months at a time.
Differential Diagnosis & Comorbidity - Who Else Is Invited?
- Key DDx:
- Bipolar I/II: Many subthreshold symptoms; no full manic/major depressive episodes.
- MDD (mixed features): Chronic, fluctuating course (not episodic like MDD).
- Persistent Depressive Disorder: Lacks the required distinct hypomanic periods.
- Borderline Personality Disorder: Mood shifts often interpersonal-reactive, rapid; unstable self-image.
- Common Comorbidities:
- Substance use disorders (SUD) common.
- Sleep-wake rhythm disorders.
- ADHD (especially youth).
- Co-occurring anxiety disorders.
⭐ High risk (15-50%) of future conversion to full Bipolar I or II Disorder.
Management & Prognosis - Calm the Current
- Psychosocial First: Cornerstone of management.
- Psychoeducation: Essential for patient/family understanding of illness chronicity, triggers, and treatment adherence.
- Psychotherapy: Cognitive Behavioral Therapy (CBT) for coping skills; Interpersonal and Social Rhythm Therapy (IPSRT) for stabilizing routines.
- Pharmacotherapy: Adjunctive, for severe symptoms or significant functional impairment.
- Mood stabilizers (e.g., valproate, lamotrigine) are preferred if medication is indicated.
- Antidepressants: High caution; risk of inducing hypomanic/manic episodes.
- Prognosis:
- Typically chronic, with lifelong fluctuating hypomanic and depressive periods.
- Requires consistent long-term monitoring.
-
⭐ 15-50% risk of progression to Bipolar I or Bipolar II Disorder over time.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic (≥2 years; ≥1 year in children/adolescents) fluctuating mood with many hypomanic and depressive symptom periods.
- These symptoms do not meet full criteria for hypomanic or major depressive episodes.
- Symptoms present for at least half the time; symptom-free periods ≤2 months.
- Never met criteria for major depressive, manic, or hypomanic episodes.
- Causes clinically significant distress or impairment in functioning.
- Often considered a temperamental predisposition or milder bipolar II disorder form.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

