Mood Disorders

On this page
🧠 The Neurobiological Architecture: Mood Regulation Command Center
The brain's mood regulation system operates through an intricate network of neurotransmitter pathways, neuroendocrine feedback loops, and structural circuits that maintain emotional homeostasis. Master these foundational mechanisms, and you unlock the logic behind every pharmacological intervention and understand why certain patients respond while others don't.

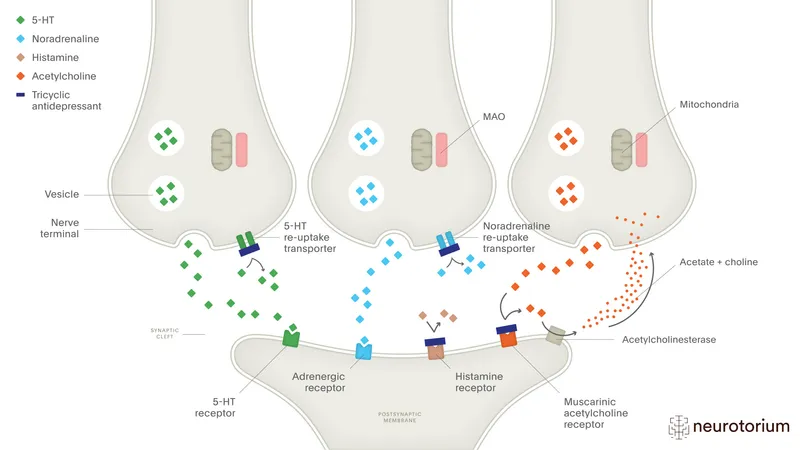
The monoamine hypothesis remains central to understanding mood disorder pathophysiology, though modern neuroscience reveals far greater complexity. Three primary neurotransmitter systems orchestrate mood regulation:
-
Serotonergic System (5-HT)
- Originates in raphe nuclei, projects throughout cortex and limbic structures
- Regulates mood, anxiety, sleep, appetite, and impulse control
- Deficiency correlates with 40-60% of MDD cases
- 5-HT1A receptor density ↓ 20-30% in depression
- Postsynaptic activation improves mood
- Presynaptic autoreceptors inhibit release (treatment target)
- 5-HT2A receptor overactivity linked to anxiety and insomnia
- Serotonin transporter (SERT) polymorphisms affect 15-20% treatment response variance
-
Noradrenergic System (NE)
- Locus coeruleus projects to frontal cortex, limbic system, hypothalamus
- Controls attention, energy, motivation, and arousal
- NE depletion produces psychomotor retardation in 70% of cases
- α2-adrenergic autoreceptor dysfunction impairs negative feedback
- β-receptor downregulation occurs after 2-4 weeks antidepressant therapy
- Norepinephrine transporter (NET) blockade increases synaptic availability
-
Dopaminergic System (DA)
- Ventral tegmental area (VTA) to nucleus accumbens (reward pathway)
- Substantia nigra to striatum (motor function)
- Mediates pleasure, motivation, reward processing, and psychomotor activity
- DA deficiency produces anhedonia in 75-85% of MDD
- Mesolimbic pathway dysfunction underlies bipolar mania
- D2 receptor density ↑ 30-40% in manic episodes
📌 Remember: "The Mood Triad" - Serotonin for Stability, Norepinephrine for eNergy, Dopamine for Drive. Deficits in any component produce distinct symptom clusters: serotonin → anxiety/rumination, norepinephrine → fatigue/concentration, dopamine → anhedonia/psychomotor changes.
The hypothalamic-pituitary-adrenal (HPA) axis dysregulation represents a second critical pathway in mood disorders. Chronic stress exposure produces sustained cortisol elevation, which damages hippocampal neurons and impairs neuroplasticity.
- HPA Axis Dysfunction Markers
- Cortisol levels ↑ 20-50% in 60-80% of MDD patients
- Dexamethasone suppression test (DST) non-suppression in 40-50% of severe depression
- Corticotropin-releasing hormone (CRH) ↑ in cerebrospinal fluid
- Hippocampal volume ↓ 10-15% with recurrent episodes
- Each depressive episode causes 8-10% additional volume loss
- Chronic hypercortisolemia impairs neurogenesis in dentate gyrus
⭐ Clinical Pearl: HPA axis hyperactivity predicts 65-70% of treatment-resistant depression cases. Patients with DST non-suppression require more aggressive initial treatment and have 2-3× higher relapse rates within 6 months of remission.
Neuroplasticity and neurotrophic factors provide the third mechanistic pillar. Brain-derived neurotrophic factor (BDNF) supports neuronal survival, synaptic plasticity, and neurogenesis-all impaired in mood disorders.
- BDNF Pathway Disruption
- Serum BDNF levels ↓ 25-40% in active depression
- Hippocampal BDNF expression ↓ 30-50% in chronic stress models
- Antidepressants ↑ BDNF after 2-4 weeks (correlates with clinical response)
- TrkB receptor activation promotes synaptic remodeling
- Glutamate-BDNF signaling essential for antidepressant efficacy
- BDNF polymorphisms (Val66Met) affect 10-15% treatment response
💡 Master This: The 2-4 week delay in antidepressant response reflects not just receptor changes, but the time required for BDNF-mediated neuroplasticity, dendritic sprouting, and synaptogenesis. This explains why rapid-acting agents like ketamine, which immediately enhance glutamate-BDNF signaling, produce effects within hours rather than weeks.
| Neurotransmitter System | Primary Brain Regions | Key Symptoms When Deficient | Receptor Targets | Time to Receptor Changes | Clinical Response Rate |
|---|---|---|---|---|---|
| Serotonin (5-HT) | Raphe nuclei → cortex, limbic | Anxiety, rumination, insomnia, appetite changes | 5-HT1A, 5-HT2A, SERT | 2-4 weeks | 60-70% |
| Norepinephrine (NE) | Locus coeruleus → frontal cortex | Fatigue, poor concentration, psychomotor retardation | α2, β, NET | 2-3 weeks | 50-60% |
| Dopamine (DA) | VTA → nucleus accumbens, striatum | Anhedonia, amotivation, psychomotor changes | D1, D2, DAT | 3-6 weeks | 40-50% |
| GABA | Cortex, limbic, brainstem | Anxiety, agitation, sleep disruption | GABA-A, GABA-B | 1-2 weeks | 70-80% (anxiety) |
| Glutamate | Widespread cortical | Cognitive dysfunction, treatment resistance | NMDA, AMPA, mGluR | Hours-days (ketamine) | 50-70% (TRD) |
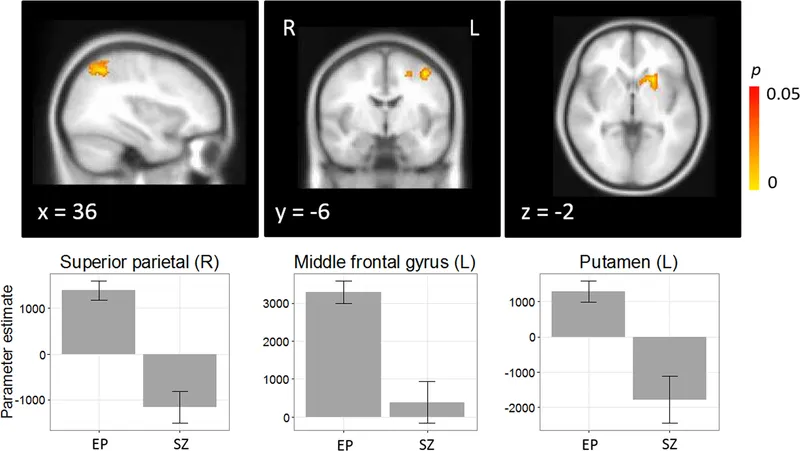
Structural and functional neuroimaging reveals consistent abnormalities across mood disorder subtypes that correlate with symptom severity and treatment response.
- Key Neuroanatomical Findings
- Prefrontal cortex (PFC) volume ↓ 5-10% (executive dysfunction)
- Dorsolateral PFC hypometabolism correlates with cognitive symptoms
- Ventromedial PFC hyperactivity in rumination
- Anterior cingulate cortex (ACC) ↓ 10-15% (emotional regulation)
- Amygdala volume variable: ↑ 10-15% in anxiety, ↓ in chronic depression
- Amygdala hyperreactivity to negative stimuli in 80-90% of MDD
- Hippocampus volume ↓ 8-10% per episode (memory, stress regulation)
- Striatum dysfunction in reward processing (anhedonia substrate)
- Prefrontal cortex (PFC) volume ↓ 5-10% (executive dysfunction)
⭐ Clinical Pearl: Patients with >3 depressive episodes show 20-30% greater hippocampal volume loss than first-episode patients, emphasizing the critical importance of early, aggressive treatment and relapse prevention. Each untreated episode increases future episode risk by 15-20% and shortens time to recurrence by 30-40%.
The inflammatory hypothesis has emerged as a crucial complementary framework, with 30-40% of MDD patients showing elevated inflammatory markers.
- Inflammatory Biomarkers in Depression
- C-reactive protein (CRP) ↑ >3 mg/L in 25-35% of MDD
- Interleukin-6 (IL-6) ↑ 30-50% above controls
- Tumor necrosis factor-α (TNF-α) ↑ 20-40%
- Pro-inflammatory cytokines impair:
- Tryptophan metabolism (↓ serotonin synthesis)
- BDNF expression (↓ neuroplasticity)
- HPA axis regulation (↑ cortisol)
- Inflammatory subtype predicts 40-50% lower SSRI response
- NSAIDs/anti-inflammatory agents may augment treatment
- IL-6 levels >10 pg/mL predict treatment resistance
Understanding these neurobiological systems reveals why combination therapies targeting multiple pathways often succeed where monotherapy fails, and why personalized medicine approaches considering genetic, inflammatory, and neuroimaging biomarkers represent the future of mood disorder treatment.
🧠 The Neurobiological Architecture: Mood Regulation Command Center
🎭 Clinical Phenomenology: The Mood Disorder Spectrum
Mood disorders manifest across a dimensional spectrum from unipolar depression through bipolar variants, each with distinct clinical signatures, course patterns, and treatment implications. Recognizing these presentations with precision determines diagnostic accuracy and prevents catastrophic treatment errors like antidepressant-induced mania.
Major Depressive Disorder (MDD) represents the prototypical unipolar mood disorder, characterized by persistent low mood, anhedonia, and neurovegetative symptoms lasting ≥2 weeks. The lifetime prevalence reaches 15-20%, with 2:1 female predominance and peak onset in the 20s-30s.
- Core Diagnostic Features (DSM-5 Criteria)
- ≥5 symptoms present during same 2-week period, including:
- Depressed mood most of the day, nearly every day
- Markedly diminished interest/pleasure (anhedonia)
- Significant weight change (>5% in 1 month) or appetite disturbance
- Insomnia or hypersomnia nearly every day
- Psychomotor agitation or retardation (observable)
- Fatigue or energy loss
- Feelings of worthlessness or excessive guilt
- Diminished concentration or indecisiveness
- Recurrent thoughts of death or suicidal ideation
- Must include depressed mood OR anhedonia
- Symptoms cause clinically significant distress/impairment
- Not attributable to substances or medical conditions
- No history of manic/hypomanic episodes (excludes bipolar)
- ≥5 symptoms present during same 2-week period, including:
📌 Remember: "SIG E CAPS" - Sleep disturbance, Interest loss (anhedonia), Guilt/worthlessness, Energy deficit, Concentration impairment, Appetite/weight change, Psychomotor changes, Suicidal ideation. Requires ≥5 symptoms including depressed mood or anhedonia for ≥2 weeks.
MDD Severity Specifiers guide treatment intensity and prognosis assessment:
- Mild: Few symptoms beyond minimum, minor functional impairment
- Moderate: Symptom severity/functional impairment between mild and severe
- Severe: Most symptoms present, marked functional impairment
- Without psychotic features: 60-70% of severe cases
- With psychotic features: 15-20% of severe cases
- Mood-congruent delusions (guilt, disease, nihilism) 70%
- Mood-incongruent delusions (persecution, control) 30%
- Requires antipsychotic + antidepressant combination
- ECT first-line for >50% response in 2-4 weeks
⭐ Clinical Pearl: Psychotic depression has <5% placebo response (vs. 30-40% for non-psychotic), <20% antidepressant monotherapy response, but 60-80% response to combined antidepressant-antipsychotic therapy. Missing this diagnosis leads to months of treatment failure.

Persistent Depressive Disorder (PDD/Dysthymia) represents chronic, lower-grade depression lasting ≥2 years (adults) or ≥1 year (children/adolescents). Lifetime prevalence 3-6%, with 2-3× higher rates in women.
- PDD Diagnostic Features
- Depressed mood most of the day, more days than not
- Never without symptoms for >2 months
- Plus ≥2 of:
- Poor appetite or overeating
- Insomnia or hypersomnia
- Low energy or fatigue
- Low self-esteem
- Poor concentration or decision difficulty
- Feelings of hopelessness
- Double depression: 40-50% develop superimposed MDE
- Early onset (<21 years): 50-60% of cases, worse prognosis
- Late onset (≥21 years): Often follows major stressor
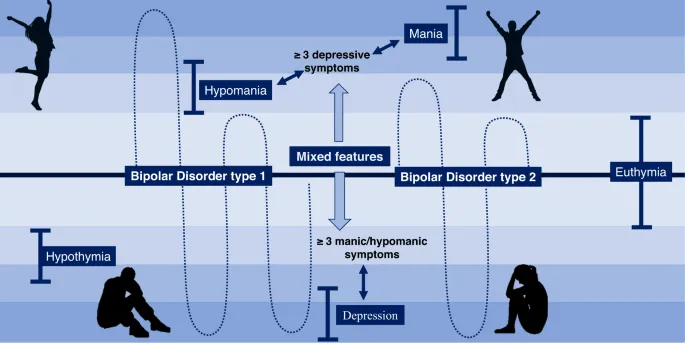
Bipolar Disorder encompasses conditions with manic, hypomanic, or mixed episodes, fundamentally altering treatment approach. Lifetime prevalence 1-2% for Bipolar I, 0.5-1% for Bipolar II, with equal gender distribution.
- Bipolar I Disorder
- ≥1 manic episode (sufficient for diagnosis)
- Manic episode criteria:
- Abnormally/persistently elevated, expansive, or irritable mood
- Increased activity/energy
- Duration ≥7 days (or any duration if hospitalization required)
- ≥3 symptoms (4 if mood only irritable): DIG FAST
- 75-80% also experience major depressive episodes
- 10-15% present with mixed features
- Psychotic features in 50-60% of manic episodes
📌 Remember: "DIG FAST" for manic symptoms - Distractibility, Irresponsibility/Indiscretion, Grandiosity, Flight of ideas, Activity increase, Sleep deficit (decreased need), Talkativeness. Requires ≥3 (or ≥4 if mood only irritable) for ≥7 days or hospitalization.
- Bipolar II Disorder
- ≥1 major depressive episode PLUS ≥1 hypomanic episode
- Never full manic or mixed episode (would be Bipolar I)
- Hypomanic episode criteria:
- Same symptom criteria as mania (DIG FAST)
- Duration ≥4 consecutive days
- Observable mood/functioning change
- Not severe enough to cause marked impairment or require hospitalization
- No psychotic features (would be mania)
- Patients spend 35-40% of time in depressive episodes
- 50-60% misdiagnosed as unipolar depression initially
- Antidepressant monotherapy risk: 20-40% switch to hypomania/mania
⭐ Clinical Pearl: Bipolar II is not a milder form of Bipolar I-patients experience more total days depressed (37% vs. 32%), higher suicide rates (15-20% vs. 10-15%), and greater functional impairment from chronic depressive burden. The "hypo" in hypomania refers to duration and severity thresholds, not clinical significance.
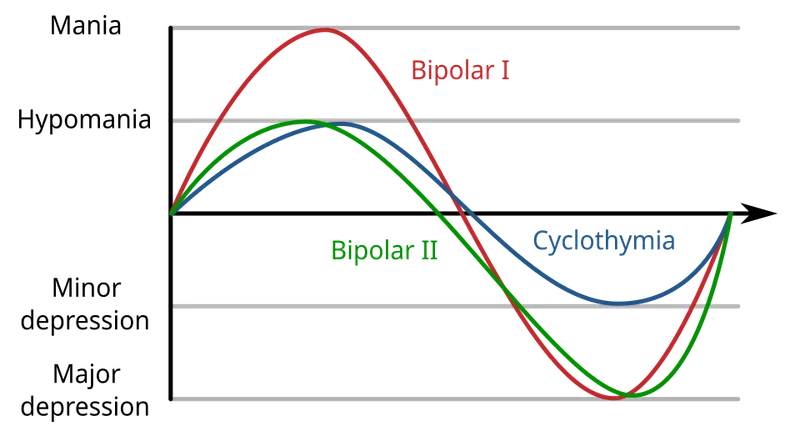
Cyclothymic Disorder presents chronic mood instability with numerous hypomanic and depressive periods that never meet full episode criteria.
- Cyclothymia Diagnostic Features
- Duration ≥2 years (adults) or ≥1 year (children/adolescents)
- Numerous periods with hypomanic symptoms (not meeting full criteria)
- Numerous periods with depressive symptoms (not meeting MDE criteria)
- Symptoms present ≥50% of time
- Never symptom-free for >2 months
- 15-50% eventually develop Bipolar I or II
- Lifetime prevalence 0.4-1%
| Disorder | Key Episodes | Minimum Duration | Prevalence | Female:Male | Suicide Risk | Psychotic Features |
|---|---|---|---|---|---|---|
| MDD | Major depressive | 2 weeks | 15-20% | 2:1 | 15% lifetime | 15-20% (severe) |
| PDD | Chronic low-grade depression | 2 years | 3-6% | 2-3:1 | 10-15% | Rare (<5%) |
| Bipolar I | Manic ± depressive | 7 days (mania) | 1-2% | 1:1 | 10-15% | 50-60% (mania) |
| Bipolar II | Hypomanic + depressive | 4 days (hypomania) | 0.5-1% | 1:1 | 15-20% | Never (by definition) |
| Cyclothymia | Subthreshold hypo/depressive | 2 years | 0.4-1% | 1:1 | 5-10% | Never |
Seasonal Affective Disorder (SAD) represents a specifier for recurrent MDD or bipolar disorder with seasonal pattern, most commonly winter-onset depression.
- SAD Clinical Pattern
- ≥2 consecutive years of seasonal episodes
- Seasonal episodes substantially outnumber non-seasonal
- 80-90% winter pattern (fall/winter onset, spring/summer remission)
- 10-20% summer pattern (spring/summer onset, fall/winter remission)
- Winter SAD features:
- Atypical symptoms: hypersomnia (75%), hyperphagia (65%), carbohydrate craving, weight gain, leaden paralysis
- Latitude-dependent: 9-10% prevalence at 48°N vs. 1-2% at 30°N
- Light therapy response 60-70% within 2-4 weeks
- Prevalence 1-10% depending on latitude
💡 Master This: The 2-week diagnostic threshold for MDD represents a balance between sensitivity and specificity-85-90% of episodes lasting ≥2 weeks represent true MDD requiring treatment, while shorter episodes often remit spontaneously. However, episodes with severe symptoms (psychosis, suicidality, marked impairment) require immediate intervention regardless of duration.
Differential diagnosis demands systematic exclusion of medical causes, substance effects, and other psychiatric conditions that mimic mood disorders.
-
Medical Conditions Mimicking Depression
- Endocrine: Hypothyroidism (10-15% of depression presentations), Cushing syndrome, Addison disease
- Neurological: Stroke (30-50% post-stroke depression), Parkinson disease (40-50%), multiple sclerosis (50%), dementia
- Infectious: HIV, syphilis, Lyme disease
- Metabolic: Vitamin B12 deficiency, folate deficiency, hypercalcemia
- Malignancy: Pancreatic cancer (50% depression), brain tumors
- Workup: TSH, CBC, CMP, B12, folate, RPR/VDRL in appropriate cases
-
Substances Causing Depression
- Medications: Corticosteroids, β-blockers, interferon-α (30-50%), isotretinoin, some antihypertensives
- Substances of abuse: Alcohol (chronic use), cannabis (20-30% heavy users), cocaine/stimulants (withdrawal), sedatives
- Withdrawal states: Benzodiazepines, opioids, stimulants
Understanding these clinical presentations with granular precision enables accurate diagnosis, appropriate treatment selection, and realistic prognostic counseling-the foundation for effective mood disorder management.
🎭 Clinical Phenomenology: The Mood Disorder Spectrum
🔬 Diagnostic Precision: Pattern Recognition Mastery
Accurate mood disorder diagnosis requires synthesizing clinical presentation, temporal patterns, severity markers, and systematic exclusion of mimics. Develop these recognition frameworks, and you distinguish bipolar depression from unipolar, identify treatment-resistant subtypes early, and avoid catastrophic misdiagnosis.
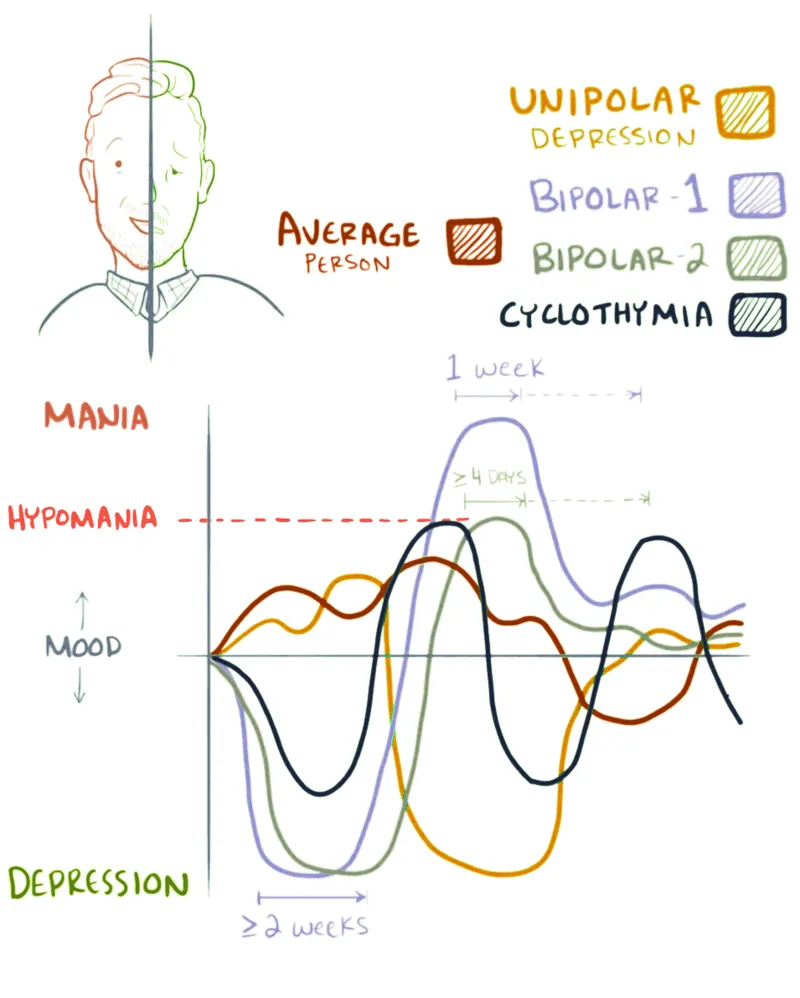
The Diagnostic Evaluation Framework proceeds systematically through history, examination, screening tools, and targeted investigations to establish diagnosis and guide treatment.
Clinical History Components must capture comprehensive symptom inventory, temporal patterns, functional impact, and risk factors.
- Symptom Assessment (SIG E CAPS)
- Sleep: Insomnia (80-90% MDD) vs. hypersomnia (15-30%, more common in atypical/bipolar depression)
- Initial insomnia (trouble falling asleep): anxiety-predominant
- Middle insomnia (frequent awakening): general depression
- Terminal insomnia (early morning awakening): melancholic/severe depression
- Interest/Anhedonia: Loss of pleasure in ≥90% activities
- Differentiates depression from demoralization
- Predicts 20-30% poorer treatment response
- Guilt/Worthlessness: Pathological (excessive/delusional) vs. appropriate
- Energy: Fatigue in 70-80%, not relieved by rest
- Concentration: Impaired in 80-90%, affects work/academics
- Appetite/Weight: Decrease (60-70%) or increase (30-40%, atypical)
- Psychomotor: Retardation (30-40%) or agitation (20-30%)
- Suicidality: Passive ideation (60%) to active planning (15-20%)
- Sleep: Insomnia (80-90% MDD) vs. hypersomnia (15-30%, more common in atypical/bipolar depression)
📌 Remember: "The Bipolar Red Flags" - Family history (first-degree relative 5-10× risk), Age of onset <25 years (60-70% bipolar), Short episodes (<3 months) with full recovery, Treatment resistance (≥2 antidepressant failures), Episode recurrence (≥3 lifetime episodes), Rapid response to antidepressants (<2 weeks) or switch to hypomania/mania. Presence of ≥3 factors suggests 70-80% probability of bipolar disorder.

-
Temporal Pattern Analysis
- Episode duration: MDD typically 6-12 months untreated, bipolar depression 3-6 months
- Episode frequency: ≥3 lifetime episodes → 80-90% recurrence risk
- Seasonal pattern: Winter predominance suggests SAD
- Rapid cycling: ≥4 episodes/year in 10-20% bipolar (3:1 female)
- Postpartum onset: Within 4 weeks delivery, 10-15% of women
- Diurnal variation: Worse mornings suggests melancholic features
-
Functional Impairment Assessment
- Work/school: Absenteeism, decreased productivity, job loss
- Relationships: Social withdrawal (80%), interpersonal conflict
- Self-care: Neglect of hygiene, nutrition, medical care
- Quantify: Days missed, activities abandoned, relationships damaged
Mental Status Examination reveals objective signs complementing subjective symptoms.
-
MSE Findings in Depression
- Appearance: Poor grooming, psychomotor retardation/agitation
- Speech: Decreased rate/volume/spontaneity, increased latency
- Mood: "Depressed," "empty," "hopeless" (patient's words)
- Affect: Constricted, depressed, tearful, anxious
- Thought process: Ruminative, pessimistic, slowed
- Thought content: Worthlessness, guilt, hopelessness, suicidal ideation
- Perception: Auditory hallucinations (10-15% severe), usually derogatory
- Cognition: Impaired concentration, memory, executive function
- Insight: Often intact (differentiates from psychotic disorders)
-
MSE Findings in Mania
- Appearance: Flamboyant dress, poor judgment evident
- Speech: Pressured, loud, difficult to interrupt
- Mood: "Great," "fantastic," "on top of the world" (or irritable)
- Affect: Elevated, expansive, labile, irritable
- Thought process: Flight of ideas, tangentiality, racing thoughts
- Thought content: Grandiosity (75%), paranoia (30-40%)
- Perception: Hallucinations (15-20%), usually mood-congruent
- Cognition: Distractible but often intact
- Insight: Severely impaired (>90%)
⭐ Clinical Pearl: The Cotard delusion (belief that one is dead or organs are rotting) appears in <1% of severe depression but carries 80-90% suicide risk and mandates immediate hospitalization and ECT consideration. Similarly, command auditory hallucinations to self-harm require immediate safety intervention regardless of diagnostic classification.
Validated Screening and Severity Tools provide standardized assessment and monitor treatment response.
-
Depression Screening Instruments
- PHQ-9 (Patient Health Questionnaire-9)
- 9 items mapping to DSM-5 criteria
- Score 0-27: ≥10 indicates MDD (sensitivity 88%, specificity 88%)
- Severity: 5-9 mild, 10-14 moderate, 15-19 moderately severe, ≥20 severe
- Item 9 assesses suicidality
- 2-minute administration, free, widely used
- BDI-II (Beck Depression Inventory-II)
- 21 items, score 0-63
- Severity: 0-13 minimal, 14-19 mild, 20-28 moderate, 29-63 severe
- Excellent for tracking symptom change
- HAM-D (Hamilton Depression Rating Scale)
- Clinician-administered, 17-21 items
- Gold standard for clinical trials
- Score ≥20 indicates moderate-severe depression
- PHQ-9 (Patient Health Questionnaire-9)
-
Bipolar Screening Instruments
- MDQ (Mood Disorder Questionnaire)
- 13 yes/no items about manic symptoms
- Positive screen: ≥7 "yes" + co-occurrence + moderate-serious problems
- Sensitivity 70%, specificity 90% for bipolar disorder
- HCL-32 (Hypomania Checklist-32)
- Better sensitivity (80%) for Bipolar II
- 32 hypomanic symptoms rated yes/no
- Cutoff ≥14 suggests bipolar
- MDQ (Mood Disorder Questionnaire)
| Tool | Type | Items | Time | Cutoff | Sensitivity | Specificity | Best Use |
|---|---|---|---|---|---|---|---|
| PHQ-9 | Self-report | 9 | 2 min | ≥10 | 88% | 88% | Primary care screening, monitoring |
| BDI-II | Self-report | 21 | 5-10 min | ≥20 (moderate) | 85% | 82% | Symptom tracking, research |
| HAM-D | Clinician | 17-21 | 20-30 min | ≥20 | 90% | 85% | Clinical trials, specialty care |
| MDQ | Self-report | 13 | 5 min | ≥7 + criteria | 70% | 90% | Bipolar I screening |
| HCL-32 | Self-report | 32 | 5-10 min | ≥14 | 80% | 70% | Bipolar II screening |
| YMRS | Clinician | 11 | 15-20 min | ≥20 (severe) | 95% | 80% | Mania severity |
Laboratory and Imaging Workup excludes medical mimics and establishes baseline for medication monitoring.
-
Essential Laboratory Tests
- TSH: Hypothyroidism in 10-15% of depression presentations
- CBC: Anemia, infection, malignancy
- CMP: Electrolyte disturbances, renal/hepatic function
- Vitamin B12, Folate: Deficiency mimics depression
- RPR/VDRL: Neurosyphilis in at-risk populations
- Toxicology screen: Substance-induced mood disorder
- Pregnancy test: Reproductive-age women (treatment implications)
-
Medication-Specific Baseline Tests
- Lithium: TSH, creatinine, calcium, ECG (if >40 years or cardiac history), pregnancy test
- Valproate: CBC, LFTs, pregnancy test
- Carbamazepine: CBC, LFTs, sodium
- Antipsychotics: Fasting glucose, lipid panel, weight, prolactin (if symptoms)
- TCAs: ECG (if >40 years or cardiac history)
-
Neuroimaging Indications (not routine)
- First psychotic episode
- New-onset psychiatric symptoms >50 years
- Atypical presentation or rapid progression
- Focal neurological signs
- Cognitive impairment out of proportion to mood symptoms
- Treatment resistance with unclear etiology
💡 Master This: Atypical depression (mood reactivity + ≥2 of: hypersomnia, hyperphagia, leaden paralysis, rejection sensitivity) occurs in 15-30% of MDD but 40-50% of bipolar depression. This pattern predicts 30-40% lower SSRI response, better MAO inhibitor response, and higher risk of antidepressant-induced mood elevation. Recognizing atypical features early guides medication selection and monitoring intensity.
Suicide Risk Assessment represents the highest-priority clinical skill in mood disorder evaluation, requiring systematic approach with documentation.
- Suicide Risk Factors (Cumulative)
- Demographic: Male (3-4× completion), age >45 or <25, white, single/divorced
- Clinical: Prior attempt (30-40× risk), severe depression, psychosis, hopelessness, anxiety/panic, substance use, chronic pain
- Historical: Family history suicide (2-3× risk), childhood trauma
- Social: Social isolation, recent loss, unemployment, access to means
- Protective: Strong social support, religious beliefs, children at home, treatment engagement
⭐ Clinical Pearl: Hopelessness predicts suicide completion better than depression severity (OR 3-5), while psychic anxiety (inner tension, restlessness) increases risk 5-10×. The combination of severe hopelessness + psychic anxiety + insomnia creates 15-20× baseline risk and mandates immediate intervention.
Mastering this diagnostic framework transforms pattern recognition from guesswork to systematic expertise, enabling confident diagnosis even in complex presentations with comorbidity, substance use, or atypical features.
🔬 Diagnostic Precision: Pattern Recognition Mastery
💊 Pharmacological Arsenal: Medication Mastery
Antidepressant and mood stabilizer pharmacotherapy represents first-line treatment for most mood disorders, with 60-70% acute response rates and 40-50% remission rates in MDD. Understanding drug mechanisms, selecting optimal agents based on symptom profiles, and managing side effects separates competent from expert prescribing.

Selective Serotonin Reuptake Inhibitors (SSRIs) dominate first-line treatment due to favorable efficacy-tolerability balance, with 60-65% response rates and 30-40% remission rates.
-
SSRI Mechanism and Clinical Pharmacology
- Selectively block serotonin transporter (SERT)
- Increase synaptic 5-HT concentration
- Downregulate 5-HT2A receptors (anxiety reduction)
- Upregulate 5-HT1A receptors (mood improvement)
- Therapeutic effects emerge 2-4 weeks (neuroplasticity lag)
- Maximum benefit 6-12 weeks
-
Individual SSRI Characteristics
- Fluoxetine (Prozac)
- Longest half-life (4-6 days), active metabolite 7-15 days
- Most activating SSRI
- Dose: 20-80 mg/day, start 20 mg
- Minimal discontinuation syndrome due to long half-life
- CYP2D6 inhibitor (drug interactions)
- Sertraline (Zoloft)
- Mild dopamine reuptake inhibition (may help energy)
- Dose: 50-200 mg/day, start 50 mg
- Most evidence for post-MI depression
- Dose-dependent diarrhea (20-30%)
- Paroxetine (Paxil)
- Most anticholinergic SSRI (weight gain, sedation)
- Shortest half-life (21 hours) → worst discontinuation syndrome
- Dose: 20-60 mg/day, start 20 mg
- Strong CYP2D6 inhibitor
- Avoid in pregnancy (cardiac malformations)
- Citalopram (Celexa)
- Least drug interactions
- QTc prolongation risk: max 40 mg/day (20 mg if >60 years or CYP2C19 poor metabolizer)
- Dose: 20-40 mg/day, start 20 mg
- Escitalopram (Lexapro)
- S-enantiomer of citalopram (more selective)
- Dose: 10-20 mg/day, start 10 mg
- Lower QTc risk than citalopram
- Often best-tolerated SSRI
- Fluoxetine (Prozac)
📌 Remember: "SSRI Side Effect Timeline" - Week 1-2: Nausea (30%), headache (20%), jitteriness, insomnia. Week 2-4: GI symptoms improve, sexual dysfunction emerges (40-60%). Week 4+: Persistent side effects include sexual dysfunction, weight gain (5-10% patients), emotional blunting (20-30%). Early side effects predict 30-40% lower adherence without counseling.
Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs) provide dual-mechanism action with 65-70% response rates, particularly effective for depression with pain or fatigue.
-
SNRI Pharmacology
- Block both SERT and NET
- Dose-dependent: Lower doses predominantly serotonergic
- Noradrenergic effects increase at higher doses
- Effective for neuropathic pain (50-60% reduction)
- May have 10-15% higher response than SSRIs in severe depression
-
Individual SNRIs
- Venlafaxine (Effexor XR)
- Dose-dependent mechanism: <150 mg SSRI-like, >150 mg adds NE
- Dose: 75-225 mg/day (up to 375 mg treatment-resistant)
- Highest discontinuation syndrome risk among SNRIs
- Monitor BP: 10-15% develop hypertension at >300 mg
- Highest efficacy for severe depression among antidepressants
- Duloxetine (Cymbalta)
- FDA-approved for neuropathic pain, fibromyalgia
- Dose: 60-120 mg/day, start 30-60 mg
- More balanced SERT/NET inhibition than venlafaxine
- Hepatotoxicity risk: avoid if liver disease or heavy alcohol use
- Desvenlafaxine (Pristiq)
- Active metabolite of venlafaxine
- Dose: 50 mg/day (minimal titration needed)
- More consistent NE effects across dose range
- Renal excretion (use in liver
- Venlafaxine (Effexor XR)
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app



















