Outpatient ED Tx - First Steps
- Context: First-line for many EDs if criteria met.
- Goals: Medical stability, weight restoration (if needed), nutritional rehab, psychoeducation, relapse prevention.
- Initial Assessment:
- Comprehensive: medical, psychiatric, nutritional, social support.
- Determine suitability for outpatient level of care.
- Core Team: Physician, registered dietitian, mental health professional.
- First Actions: Establish therapeutic alliance, collaborative goal-setting, psychoeducation for patient/family.
⭐ Outpatient suitability: BMI > 15 kg/m² (adult AN), medically stable, motivated, adequate support. Not actively suicidal or engaging in severe, frequent purging requiring medical management.
Psychotherapies - Talk Power
Key evidence-based psychotherapies form the cornerstone of outpatient ED management. Each targets specific aspects of the disorder:
| Psychotherapy | Key Target ED(s) | Primary Age Group | Core Therapeutic Focus | Typical Duration / Sessions |
|---|---|---|---|---|
| CBT-E | AN, BN, BED (all severities) | Adolescents, Adults | Modifying dysfunctional cognitions & behaviours maintaining ED; psychoeducation, self-monitoring, cognitive restructuring | 20 sessions (BN/BED) to 40 (AN outpatient) |
| FBT | AN (esp. <18 yrs, moderate-severe) | Children, Adolescents | Phase 1: Parental control of re-feeding. Phase 2: Gradual return of control to adolescent. Phase 3: Normal development. | 15-20 sessions over ~12 months |
| IPT | BN, BED (if interpersonal issues prominent) | Adults | Identifying & resolving current interpersonal problems in specific areas (e.g., grief, role transitions, disputes) that trigger ED. | 16-20 sessions over ~4-5 months |
Meds & Meals - Fuel & Fix
- Nutritional Rehabilitation:
- Primary goal: Restore healthy weight (AN), normalize eating patterns (BN, BED).
- AN target: Outpatient weight gain 0.5-1 kg/week.
- Initial calories (AN): Start 1200-1500 kcal/day, increase by 300-500 kcal every few days.
- Structured eating: 3 meals, 2-3 planned snacks. Psychoeducation & meal support crucial.
- Key Pharmacotherapy:
| Drug | ED Indication | Key Dose/Notes |
|---|---|---|
| Fluoxetine | Bulimia Nervosa (BN) | 60mg/day (often higher than for depression) |
| Olanzapine | Anorexia Nervosa (AN) | 2.5-10mg/day (adjunct for weight gain, ↓ anxiety) |
| Lisdexamfetamine | Binge Eating Disorder (BED) - Mod/Sev | 30-70mg/day (reduces binge frequency) |
Monitoring & MDT - Safety Net
- Medical Monitoring (Regular):
- Vitals (HR, BP, Temp), Weight (weekly), BMI
- Key Electrolytes ($K^+$, $PO_4^{3-}$, $Mg^{2+}$), esp. pre-feeding
- ECG (QTc, bradycardia), Hydration status
- Menstrual cycle restoration
- Multidisciplinary Team (MDT) Roles:
- Psychiatrist: Diagnosis, pharmacotherapy, team lead
- Psychologist: Evidence-based psychotherapy (e.g., CBT-E)
- Dietitian: Nutritional rehabilitation, meal planning
- Physician (GP/Internist): Monitor medical stability
⭐ Closely monitor for refeeding syndrome (hypophosphatemia, fluid shifts, cardiac compromise) in severely malnourished patients initiating nutritional therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- CBT-E (Enhanced Cognitive Behavioral Therapy) is primary for adult Bulimia Nervosa (BN) & Binge Eating Disorder (BED).
- Family-Based Treatment (FBT), or Maudsley method, is first-line for adolescent Anorexia Nervosa (AN).
- Fluoxetine (SSRI) is FDA-approved for BN; can aid BED. Limited role in AN weight gain.
- Nutritional rehabilitation & medical monitoring are crucial foundational elements for all eating disorders.
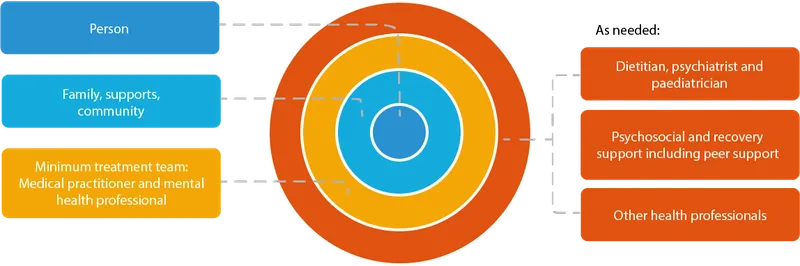
- A multidisciplinary team approach (therapist, dietitian, physician) is optimal for comprehensive care.
- Relapse prevention strategies are essential for achieving and maintaining long-term recovery outcomes.
- Outpatient settings are for medically stable patients with adequate motivation and support systems.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

