Introduction - Binge-Purge Cycle Basics
- Definition: Recurrent episodes of binge eating (large food amount, loss of control) AND recurrent inappropriate compensatory behaviors (e.g., vomiting, laxatives, fasting, excessive exercise) to prevent weight gain.
- Occurs at least once a week for 3 months.
- Self-evaluation is unduly influenced by body shape/weight.
- Epidemiology:
- Prevalence: ~1-1.5% in young women; F:M ratio ~10:1.
- Age of onset: Late adolescence/early adulthood.
- Indian context: Underreported; prevalence may be similar to Western countries in urban settings.
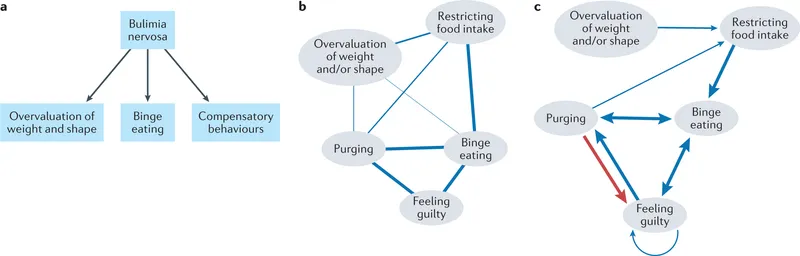
⭐ Bulimia Nervosa often co-occurs with mood and anxiety disorders, particularly depression and borderline personality disorder (Cluster B).
Diagnosis - Spotting the Signs
DSM-5 Diagnostic Criteria:
| Criterion | Description |
|---|---|
| A | Recurrent binge eating (large amount, loss of control) |
| B | Recurrent inappropriate compensatory behaviors (purging/non) |
| C | Both ≥ once/week for 3 months |
| D | Self-worth tied to body shape/weight |
| E | Not during Anorexia Nervosa |
- Purging: Vomiting, laxatives, diuretics.
- Non-purging: Fasting, excessive exercise.
Key Physical Signs:
- Russell's sign: Knuckle calluses (self-induced vomiting).
- Dental enamel erosion (lingual surfaces).
- Parotid gland enlargement (non-tender, bilateral).
- Electrolyte imbalance (e.g., ↓K+, metabolic alkalosis).
- Facial petechiae, subconjunctival hemorrhages (vomiting strain).

Psychological Features:
- Intense fear of weight gain; body shape/weight preoccupation.
- Distorted body image.
- Shame, guilt, secrecy about eating.
- Impulsivity, mood lability.
⭐ Russell's sign (knuckle calluses) indicates self-induced vomiting.
Complications - Body Under Siege
Bulimia Nervosa's (BN) recurrent purging (vomiting, laxatives, diuretics) causes severe multi-systemic damage.
- Metabolic:
- Hypokalemia ($K⁺ < \textbf{3.5} mEq/L$) - critical cardiac risk!
- Hyponatremia ($Na⁺ < \textbf{135} mEq/L$)
- Metabolic alkalosis (vomiting) or acidosis (laxative abuse)
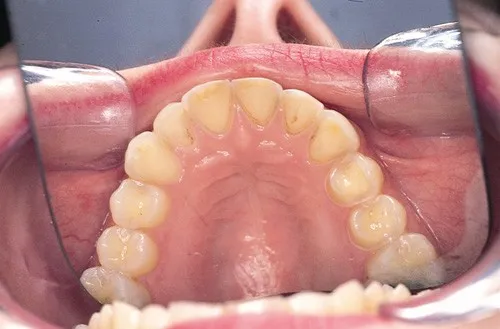
- Dental:
- Enamel erosion (perimylolysis, especially lingual surfaces)
- Increased dental caries, periodontitis
- Gastrointestinal (GI):
- Esophagitis, Mallory-Weiss tears (esophageal)
- Salivary gland hypertrophy (sialadenosis, "chipmunk facies")
- Laxative dependence, chronic constipation
- Cardiovascular:
- Arrhythmias (often due to hypokalemia)
- Cardiomyopathy (chronic ipecac use)
- Endocrine & Renal:
- Menstrual irregularities (amenorrhea, oligomenorrhea)
- Renal dysfunction, electrolyte wasting
⭐ Hypokalemia ($K⁺ < \textbf{3.5} mEq/L$) is a common, potentially life-threatening complication in BN, primarily from purging behaviors.
Management - Path to Recovery
Multimodal: Psychotherapy, pharmacotherapy, nutritional rehabilitation. Manage medical complications.
- Psychotherapy:
- CBT-BN: First-line.
- IPT (Interpersonal Psychotherapy).
- Pharmacotherapy:
- SSRIs: Fluoxetine 60mg/day (FDA approved).
- Other antidepressants considered.
- Nutritional Rehabilitation: Essential for healthy eating.
- Medical Complications: Address electrolyte imbalance, dental issues.
⭐ Cognitive Behavioral Therapy tailored for Bulimia Nervosa (CBT-BN) is the most evidence-based psychotherapy.
- Stepped-Care Model:
Differentials & Prognosis - Similar & Future
- Differential Diagnosis:
- Anorexia Nervosa (binge-eating/purging type): Distinguished by low body weight.
- Binge Eating Disorder: Lacks compensatory behaviors.
- Kleine-Levin Syndrome: Episodic hypersomnia, hyperphagia.
- MDD (atypical features): Mood symptoms primary; overeating present.
- GI disorders, CNS tumors: Rule out organic causes for vomiting/bingeing.
- Prognosis:
- Course: Often chronic and fluctuating; relapse common (30-50% within 6 months).
- Good outcome factors: Shorter illness duration, younger onset, good social support.
- Poor outcome factors: Comorbid personality disorder (esp. borderline), substance abuse, childhood obesity.
⭐ Unlike Anorexia Nervosa, individuals with Bulimia Nervosa are typically of normal weight or overweight, which can delay diagnosis.
High-Yield Points - ⚡ Biggest Takeaways
- Recurrent binge eating followed by inappropriate compensatory behaviors (e.g., purging, excessive exercise).
- Diagnosis requires episodes at least once a week for 3 months.
- Self-esteem is disproportionately linked to body shape and weight.
- Patients are typically normal weight or overweight, distinguishing from Anorexia Nervosa.
- Key complications: Russell's sign, dental erosion, parotid hypertrophy, hypokalemia, and metabolic alkalosis.
- Cognitive Behavioral Therapy (CBT) is the cornerstone of therapy; Fluoxetine (SSRI) is the drug of choice.
- Often associated with impulsivity, mood disorders, and anxiety disorders.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

