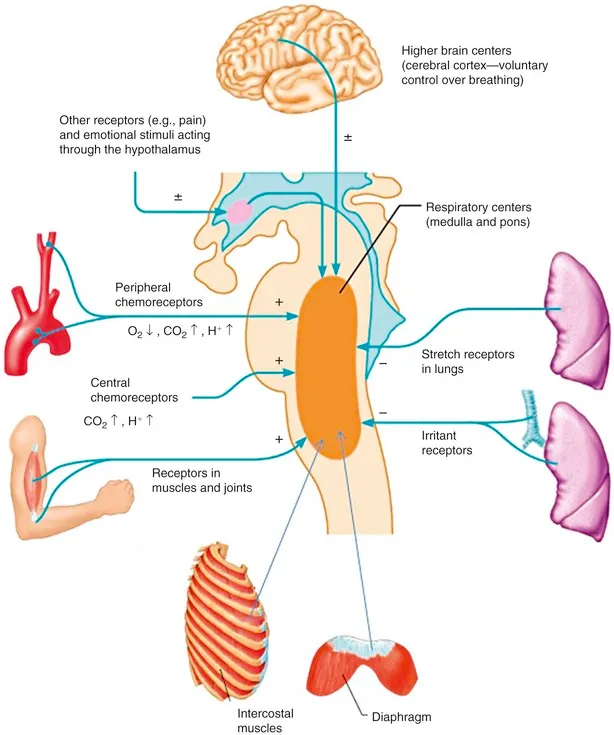
Control of Breathing: Neural Control - Brain's Breath Bosses
- Medulla Oblongata: Primary rhythm generator.
- Dorsal Respiratory Group (DRG): Inspiratory pacemaker (basic rhythm). Input: CN IX, X (chemo/baroreceptors). Output: Phrenic nerve.
- Ventral Respiratory Group (VRG): Inspiratory & expiratory neurons. Includes Pre-Bötzinger, Bötzinger (expiration). Active in forced breathing.
- Pre-Bötzinger Complex: Main rhythm generator for eupnea.
⭐ Pre-Bötzinger complex is the primary pacemaker for normal respiratory rhythm.
- Other VRG parts: For forced expiration & inspiration.
- Pons: Modulates medullary activity.
- Pneumotaxic Center (Pontine Respiratory Group - PRG): Upper pons. Limits inspiration duration ("switch-off"). ↑Rate, ↓Depth. Fine-tunes rhythm.
- Apneustic Center: Lower pons. Stimulates DRG, prolongs inspiration (apneusis if vagi cut). Overridden by pneumotaxic, vagal input.
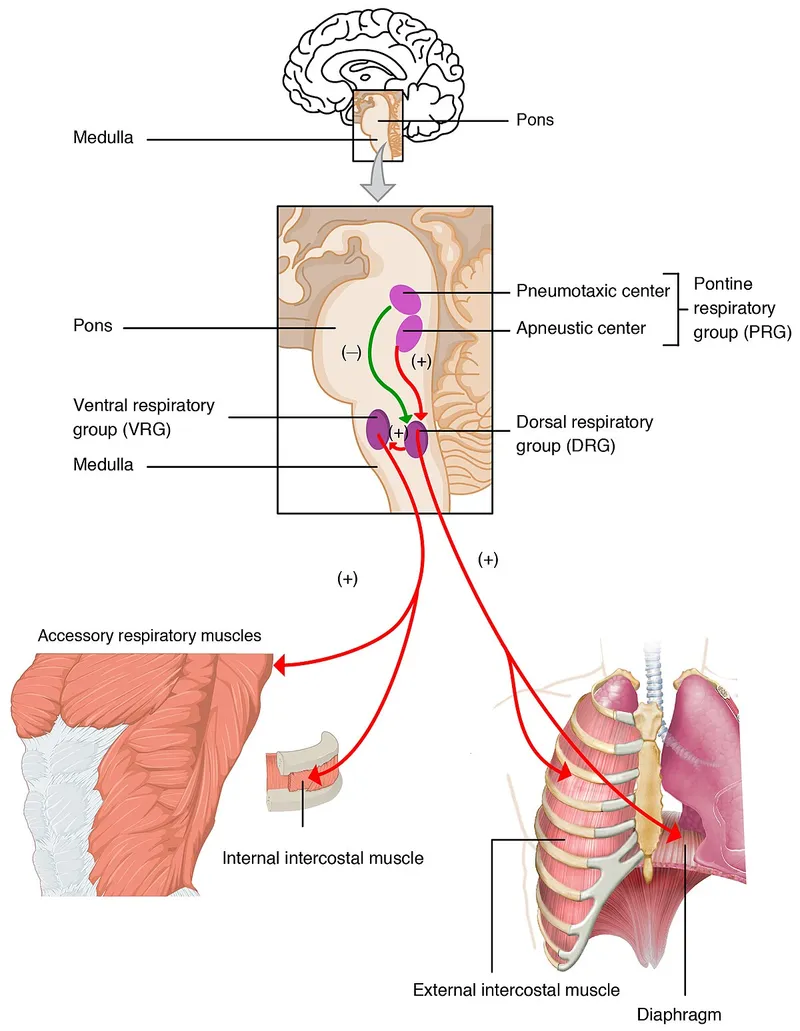
Control of Breathing: Chemical Control - Gas Gauge Gurus
- Central Chemoreceptors (CC)
- Location: Ventrolateral Medulla.
- Primary Stimulus: ↑ $H^+$ in CSF, reflecting ↑ $PaCO_2$. ($CO_2$ crosses BBB easily).
- Equation: $CO_2 + H_2O \rightleftharpoons H_2CO_3 \rightleftharpoons H^+ + HCO_3^-$.
- Response: Major drive for ventilation (70-80%); slow onset.
- Adaptation: Chronic hypercapnia (e.g., COPD) due to renal $HCO_3^-$ compensation in CSF.
- Peripheral Chemoreceptors (PC)
- Location: Carotid Bodies (afferent: CN IX 📌 SİNus nerve), Aortic Bodies (afferent: CN X).
- Stimuli:
- ↓ $PaO_2$ (hypoxemia) - main stimulus, esp. < 60 mmHg.
- ↑ $PaCO_2$ (hypercapnia).
- ↑ Arterial $H^+$ (acidemia).
- Response: Rapid ↑ ventilation; crucial for hypoxic drive.
⭐ Peripheral chemoreceptors (carotid bodies) are primarily stimulated by a fall in PaO₂ below 60 mmHg.
Control of Breathing: Reflexes & Receptors - Lung's Little Listeners
- Pulmonary Stretch Receptors (PSR):
- Location: Airway smooth muscle; Afferent: Vagus (CN X).
- Stimulus: Lung inflation → Hering-Breuer inflation reflex (↓ respiratory rate, ↑ expiratory time).
- Hering-Breuer deflation reflex: Lung deflation → ↑ respiratory effort.
⭐ The Hering-Breuer inflation reflex, mediated by pulmonary stretch receptors, is more important in regulating breathing depth and rate in neonates and during large tidal volumes in adults.
- Irritant Receptors:
- Location: Airway epithelium (trachea, bronchi); Afferent: Vagus (CN X).
- Stimulus: Noxious gases (smoke, SO₂), dust, cold air → cough, bronchoconstriction, ↑ respiratory rate.
- J-Receptors (Juxtacapillary Receptors):
- Location: Alveolar walls near capillaries; Afferent: Slow Vagal C-fibers.
- Stimulus: Pulmonary congestion, edema, emboli, capsaicin → rapid shallow breathing (tachypnea), dyspnea.
- Chest Wall Proprioceptors:
- Location: Muscle spindles (intercostals, diaphragm), Golgi tendon organs.
- Function: Sense chest wall position & muscle tension → modulate breathing depth & effort.

Control of Breathing: Applied Aspects - Breath Under Pressure
- High Altitude (↓ $P_{atm}$):
- Hypobaric hypoxia (↓ $P_{O_2}$) → HVR (peripheral chemoreceptors) → Respiratory alkalosis.
- Acclimatization:
- Renal $HCO_3^-$ excretion → CSF pH normalizes, sustains HVR.
- ↑ EPO → Polycythemia; ↑ 2,3-DPG (ODC right shift).
- Chronic hypoxic pulmonary vasoconstriction → Pulmonary HTN.
⭐ During acclimatization to high altitude, CSF pH normalizes due to renal compensation (bicarbonate excretion), which helps maintain the hypoxic ventilatory drive.
- Diving (↑ Ambient Pressure):
- Nitrogen narcosis (> 30m); Oxygen toxicity (> 1.6 ATA $P_{O_2}$).
- Decompression Sickness (DCS): N2 bubbles on rapid ascent.
- Shallow water blackout: Pre-dive hyperventilation → ↓ $P_{CO_2}$ → ↓ respiratory drive → Hypoxic LOC.

High‑Yield Points - ⚡ Biggest Takeaways
- Medulla contains DRG (inspiration) and VRG (forced expiration).
- Pons: Pneumotaxic center (limits inspiration, ↑rate), Apneustic center (prolongs inspiration).
- Central chemoreceptors detect CSF H⁺ (from CO₂); Peripheral chemoreceptors sense ↓PaO₂, ↑PaCO₂, ↑H⁺.
- Hering-Breuer inflation reflex (vagal nerve) prevents lung overinflation.
- CO₂ is the primary ventilatory stimulus; hypoxic drive (peripheral chemoreceptors) is vital in COPD.
- Kussmaul breathing signifies metabolic acidosis; Cheyne-Stokes respiration suggests CHF or stroke.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more