Female Reproductive Aging - Ovary's Ovation
- Menopause Definition: Permanent cessation of menstruation for 12 consecutive months due to loss of ovarian follicular activity.
- Average age: 51 years (range 45-55).
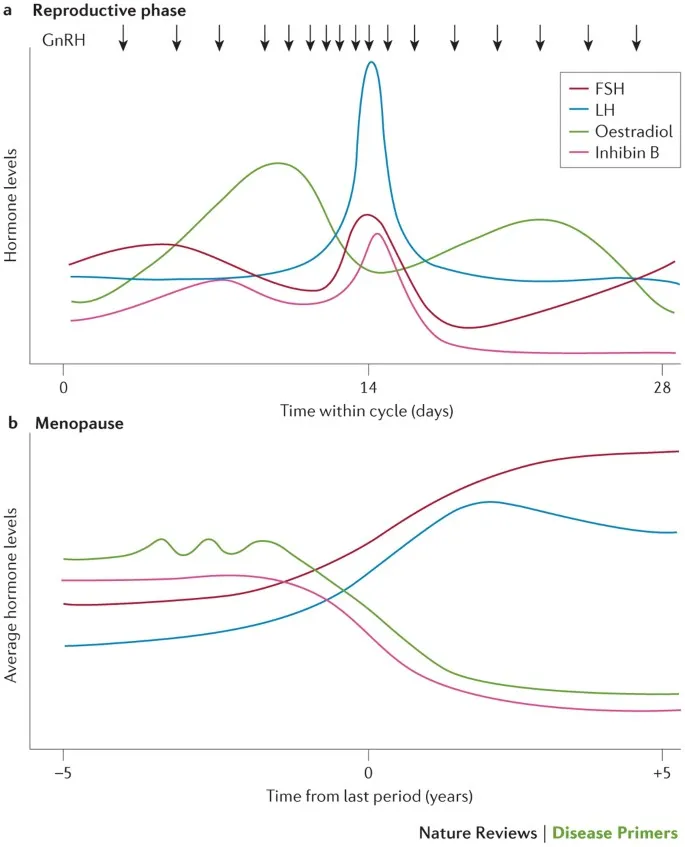
- Hormonal Hallmarks:
- ↓ Estrogen (E2), ↓ Progesterone
- ↓ Inhibin B (early indicator of ↓ granulosa cell function)
- ↓ Anti-Müllerian Hormone (AMH) (reflects ↓ ovarian reserve, declines earliest)
- ↑ FSH (most sensitive marker, often >30-40 IU/L)
- ↑ LH
- Pathophysiology Flow:
- Clinical Manifestations (Estrogen Deficiency): 📌 Mnemonic: HAVOCS
- Hot flushes, night sweats (vasomotor)
- Atrophy of urogenital tract (vaginal dryness, dyspareunia)
- Osteoporosis (↓ bone density)
- Cardiovascular disease risk ↑
- Sleep disturbances, mood changes.
- Premature Ovarian Insufficiency (POI): Menopause before age 40.
⭐ The hallmark of menopause is a persistently elevated FSH level (typically >40 mIU/mL) in the context of amenorrhea.
Menopause Manifestations - Systemic Symphony
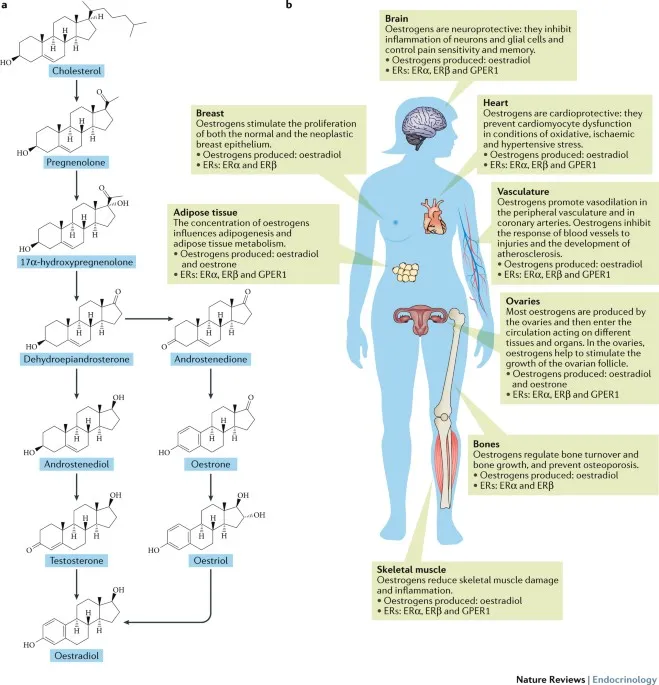
Widespread effects due to estrogen (E2) ↓:
- Vasomotor Instability (VMS):
- Hot flushes (sudden warmth, sweating), night sweats. Most prevalent.
- Urogenital Atrophy (Genitourinary Syndrome of Menopause - GSM):
- Vaginal dryness, dyspareunia, pruritus.
- Urinary: urgency, frequency, recurrent UTIs. Vaginal pH ↑.
- Skeletal System:
- ↑ Bone resorption, ↓ Bone Mineral Density (BMD) → Osteoporosis.
- ↑ Risk of fragility fractures (vertebral, hip, Colles').
- Cardiovascular System (CVS):
- Adverse lipid profile: ↑ LDL, ↓ HDL, ↑ Triglycerides.
- ↑ Risk of coronary artery disease (CAD), hypertension.
- Neuropsychiatric & Cognitive:
- Mood lability, depression, anxiety.
- Sleep disturbances (insomnia).
- Cognitive changes: "brain fog", memory impairment.
- Skin & Connective Tissue:
- ↓ Collagen: skin thinning, dryness, ↓ elasticity, wrinkles.
- Brittle nails, dry hair.
⭐ The most common and characteristic symptom of menopause is the hot flush, experienced by up to 75% of women, often disrupting sleep and daily activities.
Male Reproductive Aging - Testo's Twilight
- Andropause/Late-Onset Hypogonadism (LOH): Gradual ↓ serum testosterone (T) & associated symptoms, typically post age 40-50.
- Key Hormonal Shifts:
- Total T: ↓ ~1%/year after age 30.
- Free/Bioavailable T: ↓ more significantly (due to ↑ SHBG).
- LH/FSH: ↑ (compensatory, often blunted pituitary response).
- DHEA/DHEA-S: Marked ↓.
- Common Manifestations:
- Sexual: ↓ libido, erectile dysfunction (ED), ↓ morning erections.
- Physical: ↓ muscle mass & strength (sarcopenia), ↑ visceral fat, ↓ bone density (osteoporosis risk).
- Psycho-cognitive: Fatigue, mood swings, ↓ concentration, sleep issues.
- Sperm Parameters: ↓ quality (motility, morphology), ↓ semen volume; count may persist longer.
⭐ Andropause: gradual T ↓, unlike abrupt female menopause hormonal shifts.
High‑Yield Points - ⚡ Biggest Takeaways
- Menopause: 12 months amenorrhea; average age 51 years. Follicular depletion is key.
- Hormonal Shift: ↓ Estrogen, ↓ Progesterone; ↑ FSH (earliest/best marker), ↑ LH.
- Inhibin B & AMH: ↓ Inhibin B (↑FSH cause) & ↓ AMH (↓ovarian reserve marker).
- Perimenopause: Characterized by irregular cycles, vasomotor symptoms (hot flashes, night sweats).
- Andropause (Male): Gradual ↓ testosterone; symptoms include ↓ libido, ↓ muscle mass, fatigue.
- Consequences of Estrogen Deficiency: Osteoporosis, urogenital atrophy, increased cardiovascular risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

