Menstrual Cycle Overview - The Monthly Clock
- Menstrual Cycle: Rhythmic physiological changes in fertile females, preparing for potential pregnancy.
- Menarche: Onset of menstruation.
- Menopause: Cessation of menstruation.
- Normal length: 28 ± 7 days.
- Two Interconnected Cycles:
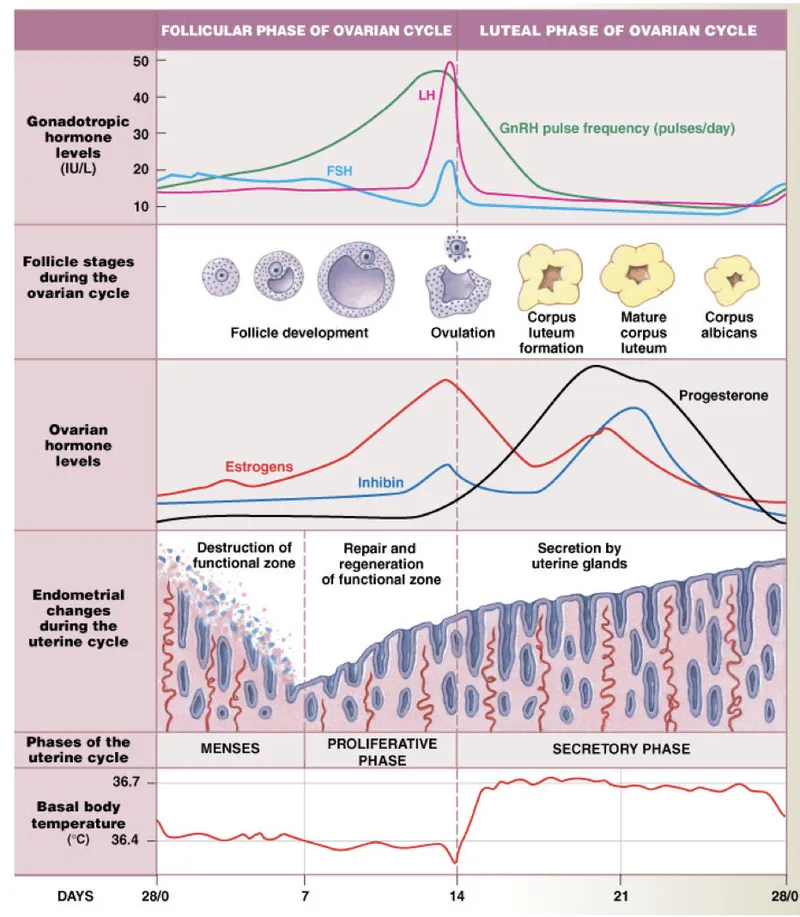
- Ovarian Cycle: Governs egg development. Key phases:
- Follicular (maturation)
- Ovulation (release)
- Luteal (corpus luteum)
- Uterine Cycle: Prepares uterine lining. Key phases:
- Menstrual (shedding)
- Proliferative (rebuilding)
- Secretory (thickening)
- 📌 Mnemonic (Ovarian phases): FOLlow Ovulation Luckily.
- Ovarian Cycle: Governs egg development. Key phases:
⭐ Day 1 of the cycle is the first day of menstruation.
 oka
oka
Hormonal Control - Hormone Harmony
- Hypothalamic-Pituitary-Ovarian (HPO) Axis: Master regulator.
- Hypothalamus: Pulsatile Gonadotropin-Releasing Hormone (GnRH).
- Anterior Pituitary: Follicle-Stimulating Hormone (FSH) & Luteinizing Hormone (LH).
- Ovary: Estrogen (E2), Progesterone (P4), Inhibins (A & B).
- Key Hormone Actions:
- FSH: Follicular development, ↑E2.
- LH: Ovulation, corpus luteum (CL) formation & P4 secretion.
- Estrogen (E2): Endometrial proliferation. Dual feedback:
- Low E2: Negative feedback on FSH/LH.
- Sustained high E2 (>200 pg/mL for >48 hrs): Positive feedback → LH surge.
- Progesterone (P4): Secretory endometrium, maintains pregnancy. Negative feedback.
- Inhibins: Suppress FSH (Inhibin B - follicular; Inhibin A - luteal).
⭐ The LH surge is the primary trigger for ovulation, occurring approximately 24-36 hours before follicle rupture.
Ovarian Cycle - Egg's Grand Show

1. Follicular Phase (FSH-driven, variable length):
- Recruitment: Primordial → Primary → Antral follicle.
- Selection: One dominant Graafian follicle (~20-25 mm) matures.
- FSH: Stimulates follicle growth, estrogen synthesis.
- Estrogen: ↑FSH receptors; high levels induce LH surge.
- Two-cell, two-gonadotropin:
- Theca (LH): Androgens.
- Granulosa (FSH): Androgens → Estradiol (aromatase).
2. Ovulation (~Day 14, LH surge-triggered):
- LH surge (from ↑estrogen): Oocyte meiosis I completion, stigma formation, oocyte release.
3. Luteal Phase (Progesterone-dominant, fixed ~14 days):
- Corpus Luteum (CL) forms from ruptured follicle.
- CL secretes: Progesterone (dominant), Estrogen.
⭐ Corpus luteum is the main source of progesterone in the luteal phase, vital for endometrial receptivity and early pregnancy.
- Fate:
- No pregnancy: CL degenerates → Corpus Albicans (↓hormones → menses).
- Pregnancy: hCG maintains CL.
Ovarian Cycle Flow:
Uterine Cycle - Womb's Wallpaper Reno
- Menstrual Phase (Days 1-5):
- Shedding of stratum functionalis due to ischemia.
- Trigger: ↓ Progesterone & Estrogen → spiral artery constriction.
- Endometrial thickness: ~1-2 mm.
- Proliferative Phase (Days 6-14): "Rebuilding the lining"
- Driven by ↑ Estrogen (ovarian follicles).
- Regeneration & growth of stratum functionalis.
- Glands: straight, tubular; Arteries: spiral, elongate.
- Endometrial thickness: up to ~8-10 mm.
- Secretory Phase (Days 15-28): "Preparing for implantation"
- Driven by ↑ Progesterone (corpus luteum).
- Differentiation: glands become tortuous, secrete glycogen-rich fluid.
- ↑ Vascularity, edema; spiral arteries become highly coiled.
- Maximal thickness: ~12-16 mm.
- 📌 Mnemonic: Secretory phase = Soft, Spongy, Swollen.

⭐ Pinopodes, small protrusions on endometrial cells, appear during the implantation window (mid-secretory, days 20-24), crucial for blastocyst adhesion.
High-Yield Points - ⚡ Biggest Takeaways
- FSH initiates follicular growth; LH surge is crucial for ovulation.
- Estrogen (follicular) drives proliferative phase; Progesterone (luteal) drives secretory phase.
- Corpus luteum secretes progesterone; its regression causes menstruation.
- Ovulation occurs ~14 days before menses, triggered by LH surge.
- LH surge is the best hormonal marker for predicting ovulation.
- Menstruation signifies endometrial shedding due to progesterone withdrawal.
- Mid-cycle estrogen peak causes positive feedback for LH surge.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

