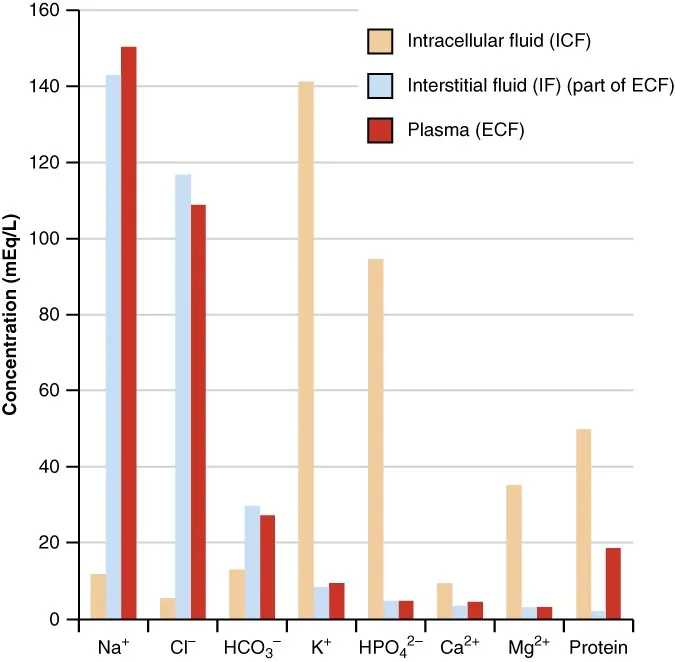
Body Fluid Compartments - Compartment Secrets
- Total Body Water (TBW): ~60% body weight (adult male), ~50% (female). 📌 Rule of 60-40-20: 60% TBW, 40% ICF, 20% ECF of body weight.
- Compartments:
- Intracellular Fluid (ICF): 2/3 TBW. Major cation: $K^+$; Major anions: $PO_4^{3-}$, proteins.
- Extracellular Fluid (ECF): 1/3 TBW. Major cation: $Na^+$; Major anions: $Cl^-$, $HCO_3^-$.
- Plasma: 1/4 ECF. Contains proteins (e.g., albumin).
- Interstitial Fluid (ISF): 3/4 ECF. Protein-poor.
- Transcellular Fluid: Small volume (e.g., CSF, intraocular fluid).
- Measurement (Indicator Dilution Principle):
- TBW: $D_2O$, Antipyrine.
- ECF: Inulin, Mannitol, $SO_4^{2-}$.
- Plasma Volume: Evans blue (T-1824), $^{131}I$-albumin.
- Osmolality: Equal across compartments (~280-295 mOsm/kg $H_2O$).
- Calculated Plasma Osmolality: $2 \times [Na^+]{plasma} + (\text{Glucose}{mg/dL}/18) + (\text{BUN}_{mg/dL}/2.8)$.
⭐ Plasma oncotic pressure, primarily due to albumin, is crucial for maintaining fluid balance between plasma and interstitial fluid (Starling forces).
Thirst Regulation - Brain's SOS
- Primary Thirst Stimuli:
- Hyperosmolality: ↑ Plasma osmolality (> 280-290 mOsm/kg), sensed by osmoreceptors. Main stimulus.
- Hypovolemia: ↓ Blood volume/pressure (activates baroreceptors, RAAS → ↑Angiotensin II).
- Angiotensin II: Potent dipsogen.
- Neural Pathway - "Brain's SOS":
- Sensors (CVOs - No BBB):
- OVLT (Organum Vasculosum Lamina Terminalis) & SFO (Subfornical Organ).
- Detect plasma osmolality & Angiotensin II.
- Integrator: Median Preoptic Nucleus (MnPO) - inputs from OVLT, SFO, baroreceptors.
- Conscious Perception: Anterior Cingulate Cortex, Insula → thirst sensation.
- Sensors (CVOs - No BBB):
- Thirst Satiation:
- Oropharyngeal signals (cold water): Rapid, pre-absorptive.
- Gastric distension: Slower.

⭐ Angiotensin II is a potent dipsogen (thirst-inducing agent), acting directly on the Subfornical Organ (SFO) and Organum Vasculosum of the Lamina Terminalis (OVLT).
Hormonal Water Control - Hormonal Harmony
- Antidiuretic Hormone (ADH/Vasopressin):
- Origin: Hypothalamus (SON, PVN) → Post. Pituitary.
- Triggers: ↑ Plasma osmolality (main); ↓ blood volume/pressure.
- Action: V₂ receptors (collecting ducts) → Aquaporin-2 insertion → ↑ H₂O reabsorption.
- Effect: Concentrated urine, ↓ plasma osmolality, ↑ blood volume.
- Aldosterone (RAAS component):
- Origin: Adrenal Cortex (Zona Glomerulosa).
- Triggers: Angiotensin II, ↑ plasma K⁺.
- Action: ↑ Na⁺ reabsorption (ENaC, Na⁺/K⁺ ATPase) & K⁺ secretion (DCT/CD). Water follows Na⁺.
- Effect: ↑ Blood volume/pressure, ↓ plasma K⁺.
- Atrial Natriuretic Peptide (ANP):
- Origin: Atrial Myocytes.
- Triggers: Atrial stretch (↑ blood volume).
- Action: Natriuresis/diuresis; inhibits Na⁺ reabsorption, ADH & aldosterone release; afferent arteriole dilation.
- Effect: ↓ Blood volume/pressure.
⭐ SIADH: excessive ADH → euvolemic/hypervolemic hyponatremia; inappropriately concentrated urine (Urine Osm > 100 mOsm/kg despite serum hypo-osmolality).

Fluid Imbalances - Balance & Bumps
- Homeostasis: Fluid Intake = Output. Disruption causes imbalance.
- Assess: Clinical signs, weight, urine output, serum Na⁺, osmolality.
- Dehydration (↓ECF Volume):
- Types: Isotonic (diarrhea), Hypertonic (fever, ↓H₂O), Hypotonic (diuretics).
- Causes: Vomiting, diarrhea, burns, fever, diuretics, ↓intake.
- Signs: Tachycardia, hypotension, orthostasis, dry mucosa, ↓skin turgor, oliguria.
- Overhydration (↑ECF Volume / Edema):
- Types: Isotonic (IV overload), Hypotonic (SIADH).
- Causes: Renal/heart failure, cirrhosis, SIADH, iatrogenic.
- Signs: Pitting edema, ↑JVP, pulmonary crackles, S3, weight gain, dyspnea.

⭐ In dehydration, a BUN/Creatinine ratio > 20:1 is a classic sign of pre-renal azotemia, indicating kidneys are conserving volume.
High‑Yield Points - ⚡ Biggest Takeaways
- Hypothalamic osmoreceptors (OVLT, SFO) detect ↑plasma osmolality, stimulating thirst & ADH release.
- Angiotensin II acts on SFO, powerfully increasing thirst and ADH secretion.
- ADH (Vasopressin) release is primarily triggered by ↑osmolality and ↓blood volume/pressure.
- Baroreceptors (carotid, aortic, atrial) modulate ADH and thirst via blood pressure signals.
- ↓Effective circulating volume is a potent non-osmotic stimulus for thirst and ADH.
- Hyponatremia (e.g., SIADH, excess water) contrasts with Hypernatremia (usually water deficit).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more