Pancreatic Structure & Function - Gland of Plenty
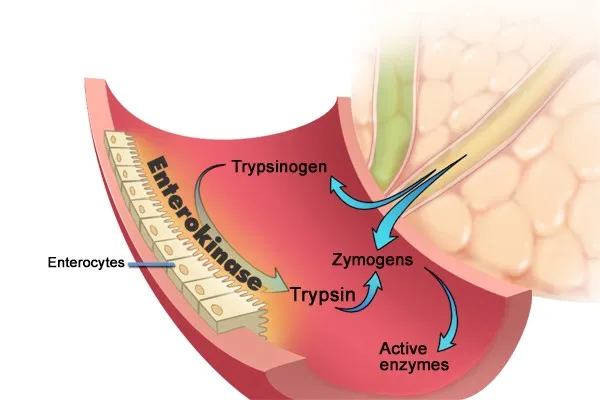
- Exocrine Pancreas: Composed of acinar cells (enzyme synthesis) and ductal cells (bicarbonate secretion).
- Acinar Cells: Synthesize & secrete digestive zymogens (inactive enzymes).
- Key enzymes: Amylase (carbohydrates), Lipase (fats, requires colipase), Proteases (e.g., Trypsinogen, Chymotrypsinogen for proteins).
- Stimulated mainly by Cholecystokinin (CCK) and Acetylcholine (ACh via vagus nerve).
- Contain zymogen granules for enzyme storage.
- Ductal Cells: Secrete an aqueous $HCO_3^-$-rich fluid.
- Neutralizes acidic chyme from the stomach, providing optimal pH for pancreatic enzymes.
- Stimulated mainly by Secretin.
- Involves carbonic anhydrase and the $CFTR$ chloride channel.
- Acinar Cells: Synthesize & secrete digestive zymogens (inactive enzymes).
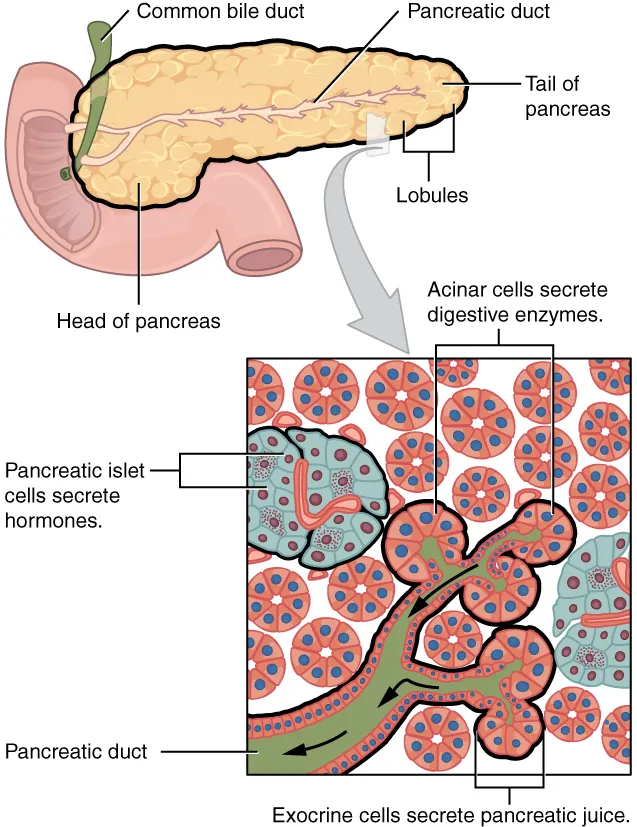
⭐ Trypsinogen is activated to its active form, trypsin, by enteropeptidase (enterokinase), an enzyme located on the duodenal brush border. Trypsin then activates other pancreatic proteases (cascade effect).
Key Pancreatic Secretions - Digestive Dynamos
Pancreas: Exocrine powerhouse for digestion. Secretes enzymes & bicarbonate.
- Enzymes (Acinar cells): 📌 T.C.P.E.A.L. (Trypsinogen, Chymotrypsinogen, Procarboxypeptidase, Proelastase, Amylase, Lipase)
- Amylase: Carbohydrate digestion.
- Lipase (+ Colipase): Fat digestion. Critical.
- Proteases (as zymogens): Protein digestion.
- Trypsinogen $\xrightarrow{\text{Enteropeptidase (duodenum)}}$ Trypsin (key activator).
- Trypsin activates: Chymotrypsinogen, Proelastase, Procarboxypeptidase, more Trypsinogen (autocatalysis).
- Bicarbonate ($HCO_3^-$) & Water (Ductal cells):
- Neutralizes duodenal acid (optimal enzyme pH).
- $H_2O + CO_2 \xrightarrow{CA} H_2CO_3 \rightarrow H^+ + HCO_3^-$ (CA: Carbonic Anhydrase).
- Stimulated by Secretin.
⭐ Pancreatic lipase requires colipase (also from pancreas) for full activity, especially in the presence of bile salts, making it a key target in malabsorption syndromes like cystic fibrosis or pancreatitis.
Regulation of Exocrine Pancreas - Secretion Signals
Pancreatic secretion: neural & hormonal regulation. Three phases: cephalic, gastric, intestinal.
-
Phases:
- Cephalic Phase (20-25%): Vagal (sight, smell, taste). ↑Enzymes, low volume.
- Gastric Phase (10-20%): Gastric distension, vagovagal. ↑Enzymes.
- Intestinal Phase (50-80%): Dominant. Hormonal (CCK, Secretin), vagovagal.
-
Hormonal Control:
- Secretin:
- Stimulus: Acid (H+) in duodenum (pH < 4.5).
- Source: S-cells (duodenum).
- Action: ↑ $HCO_3^-$ & $H_2O$ (ductal cells). "Nature's antacid".
- Cholecystokinin (CCK):
- Stimulus: Fats, peptides in duodenum.
- Source: I-cells (duodenum, jejunum).
- Action: ↑ Enzyme secretion (acinar cells). Potentiates secretin.
⭐ CCK is the most potent stimulator of pancreatic enzyme secretion.
- Secretin:
-
Neural Control:
- Vagal (ACh): Stimulates acinar (enzyme) & ductal ($HCO_3^-$) cells. Potentiates CCK & Secretin.
- Sympathetic: Generally inhibitory.
📌 Mnemonic: Secretin for Sodium bicarbonate; CCK for enZyme (C-Zyme-Kinin).
Clinical Highlights - Pancreatic Perils
- Acute Pancreatitis (AP):
- Etiology: Gallstones (most common), Alcohol. 📌 (Others: Trauma, ERCP, Hypertriglyceridemia).
- Diagnosis: ↑ Serum lipase (>3x ULN; more specific & persists longer), ↑ Serum amylase (earlier rise).
- Complication/Sign: Hypocalcemia (due to saponification of peripancreatic fat).
- Chronic Pancreatitis (CP):
- Etiology: Alcohol (commonest in adults), Cystic Fibrosis (children), Idiopathic.
- Key Features: Pancreatic calcification (X-ray/CT), steatorrhea, diabetes mellitus (late).
- Major Risk: Pancreatic adenocarcinoma.
- Exocrine Pancreatic Insufficiency (EPI):
- Manifestation: Steatorrhea (bulky, greasy, foul-smelling stools).
- Diagnosis: ↓ Fecal elastase-1 (screening); 72-hr fecal fat (confirmatory).
⭐ Lipase is generally preferred over amylase for AP diagnosis; amylase can be elevated in other conditions (e.g., mumps, ectopic pregnancy).
High‑Yield Points - ⚡ Biggest Takeaways
- Acinar cells produce digestive enzymes (amylase, lipase, proteases like trypsinogen).
- Ductal cells secrete bicarbonate-rich fluid to neutralize duodenal pH.
- Secretin (S-cells) is the primary stimulus for bicarbonate secretion by ductal cells.
- Cholecystokinin (CCK) (I-cells) is the main stimulus for enzyme secretion from acinar cells.
- Enterokinase (brush border enzyme) activates trypsinogen to trypsin in the duodenum.
- Trypsin activates other pancreatic proenzymes, initiating a proteolytic cascade.
- Pancreatic insufficiency leads to steatorrhea (fat malabsorption) and weight loss.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

