Hepatic Architecture & Vasculature - Liver's Blueprint
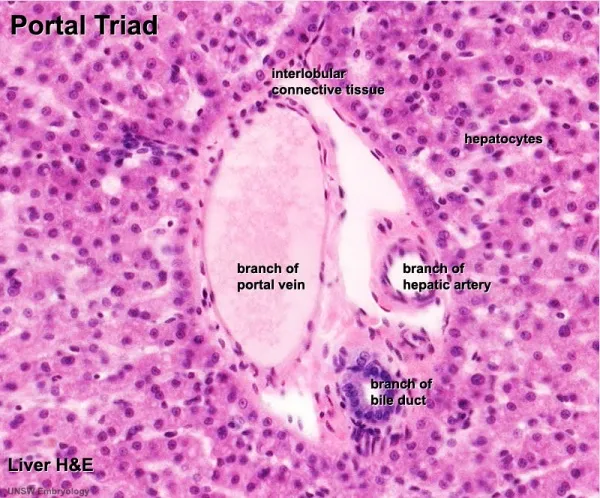
- Structural Units:
- Classic Lobule: Hexagonal, central vein at core.
- Portal Lobule: Triangular, portal triad at center, drains bile.
- Liver Acinus (of Rappaport): Diamond-shaped, functional unit based on $O_2$ gradient. Zone 1 (periportal) = best oxygenated; Zone 3 (pericentral) = least, most susceptible to ischemia & drug toxicity.
- Cellular Components:
- Hepatocytes: Arranged in plates, separated by sinusoids.
- Sinusoids: Fenestrated endothelium, mix portal venous & hepatic arterial blood.
- Space of Disse: Between hepatocytes & sinusoids; contains Stellate (Ito) cells (vitamin A storage, fibrosis).
- Kupffer cells: Macrophages within sinusoids.
- Vasculature:
- Dual Supply: Portal Vein (~75%, nutrient-rich), Hepatic Artery (~25%, $O_2$-rich).
- Flow: Portal triad vessels → Sinusoids → Central Vein → Hepatic Veins → IVC.
- Portal Triad: Bile duct, hepatic artery branch, portal vein branch.
⭐ The liver acinus is the smallest functional unit, with Zone 1 hepatocytes being most active in oxidative metabolism, urea synthesis, and gluconeogenesis, while Zone 3 excels in glycolysis, ketogenesis, and drug detoxification (cytochrome P450).
Bile Production & Flow - Golden River Secrets
- Production: Hepatocytes (500-1000 mL/day); cholangiocytes add $HCO_3^-$, H₂O.
- Stimuli: Secretin (ducts), CCK (GB contraction, Sphincter of Oddi relaxation), Vagal.
- Composition: Bile salts (emulsification), bilirubin (pigment), cholesterol, lecithin (📌 BBCL), electrolytes, H₂O.
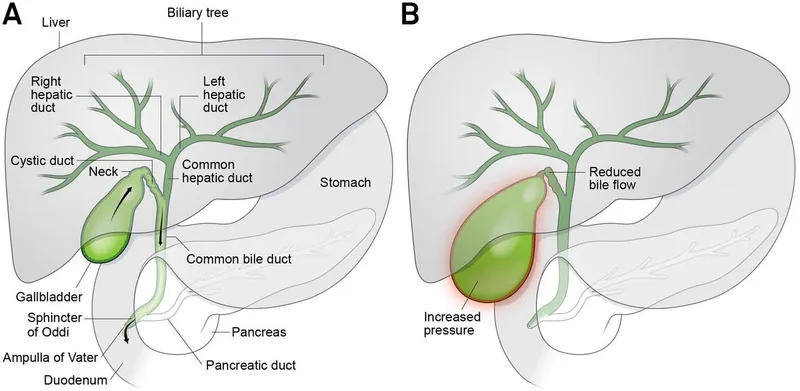
- Flow Path: Canaliculi → Ducts → CHD. CHD + Cystic Duct (GB) → CBD → Duodenum.
- Gallbladder: Stores & concentrates bile (5-20x).
- Enterohepatic Circulation: ~95% bile salts reabsorbed (terminal ileum).
- Bilirubin: Heme → UCB → Liver conjugation (UDP-glucuronyltransferase) → CB → Bile.
⭐ Conjugated bilirubin is water-soluble and excreted in bile; unconjugated bilirubin is lipid-soluble and binds to albumin.
Liver's Metabolic & Synthetic Roles - The Body's Powerhouse
- Carbohydrate Homeostasis:
- Glycogenesis, glycogenolysis (maintains blood glucose)
- Gluconeogenesis (e.g., from lactate, alanine, glycerol)
- Protein Metabolism:
- Synthesis: non-essential amino acids, plasma proteins (except immunoglobulins)
- Urea cycle: converts toxic ammonia ($NH_3$) to urea for excretion
- Lipid Metabolism:
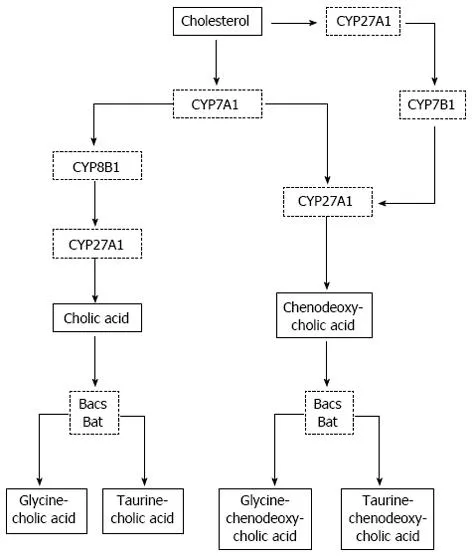
- Synthesis: cholesterol, triglycerides, lipoproteins (VLDL, HDL), bile acids
- Fatty acid oxidation (beta-oxidation)
- Detoxification & Biotransformation:
- Phase I: Cytochrome P450 (oxidation, reduction, hydrolysis)
- Phase II: Conjugation (glucuronidation, sulfation, glutathione)
- Key Synthetic Products:
- Albumin (major contributor to plasma oncotic pressure)
- Clotting factors (II, VII, IX, X; Protein C & S - Vit. K dependent)
- Angiotensinogen, thrombopoietin, IGF-1
⭐ The liver synthesizes most plasma proteins, including albumin and crucial clotting factors (II, VII, IX, X), but notably not immunoglobulins (gamma-globulins).
Gallbladder & Biliary Dynamics - Bile's Holding & Release
- Gallbladder Function:
- Stores bile (capacity 30-60 mL).
- Concentrates bile 5-20x by active absorption of Na+, Cl-, $HCO_3^-$, and water.
- Acidifies bile (pH $↓$ to 7.0-7.4), preventing Ca2+ salt precipitation.
- Bile Release Regulation:
- Primary stimulus: Fatty acids & amino acids in duodenum trigger CCK release from I-cells.
- Cholecystokinin (CCK) actions:
- Potent gallbladder contraction.
- Relaxation of Sphincter of Oddi.
- Vagal stimulation (ACh): Weakly stimulates gallbladder contraction; potentiates CCK effects.
- Secretin: Stimulates biliary ductal cells to secrete $HCO_3^-$-rich watery fluid.
⭐ CCK is the principal physiological stimulus for gallbladder emptying and Sphincter of Oddi relaxation.
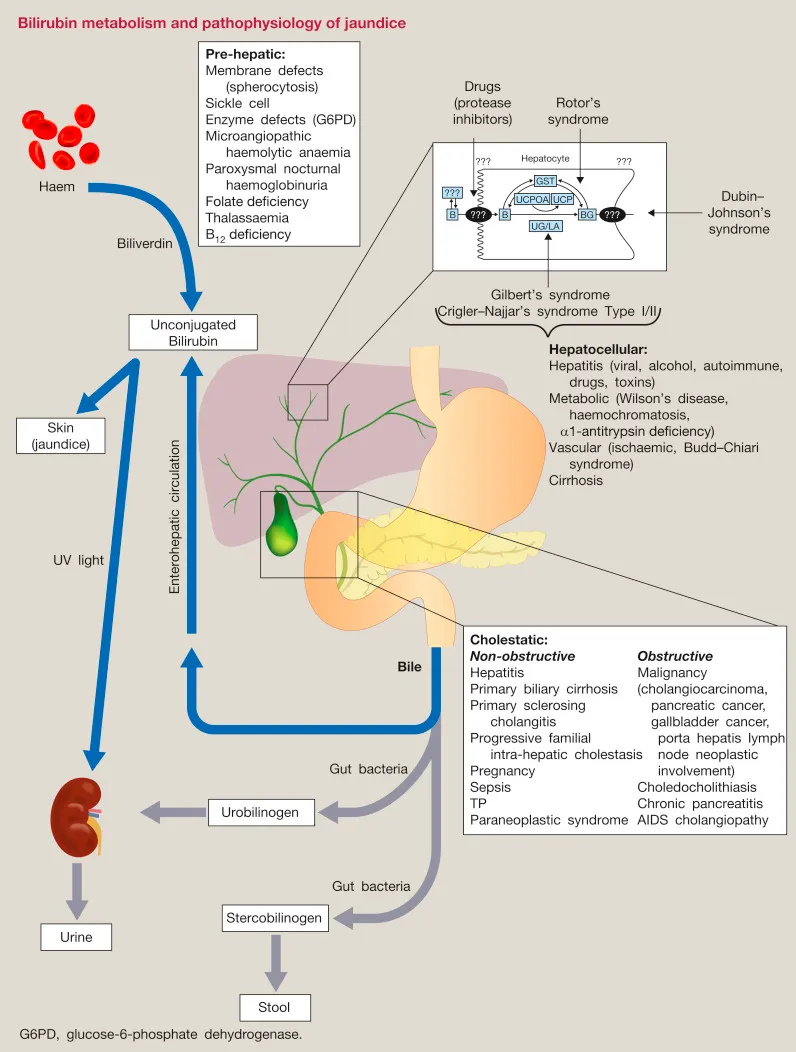
Jaundice & LFT Basics - When Things Go Yellow
- Jaundice: Yellow sclera/skin; Serum Bilirubin >2.5-3 mg/dL.
- Bilirubin: UCB (indirect) conjugated by UDP-glucuronyltransferase to CB (direct).
- Types:
- Pre-hepatic: ↑UCB (e.g., hemolysis).
- Hepatic: ↑UCB/CB (e.g., hepatitis, Gilbert's).
- Post-hepatic (Obstructive): ↑CB (e.g., gallstones).
- LFTs: AST/ALT (hepatocellular), ALP/GGT (cholestatic). Albumin/PT (synthetic function).
⭐ Isolated rise in unconjugated bilirubin with normal LFTs suggests Gilbert's syndrome.
High‑Yield Points - ⚡ Biggest Takeaways
- Bilirubin: Unconjugated (indirect, lipid-soluble) converted to conjugated (direct, water-soluble) in liver for bile excretion.
- Jaundice types: Pre-hepatic (↑unconjugated), hepatic (↑both), post-hepatic (↑conjugated, obstructive).
- Bile salts: From cholesterol, vital for fat digestion/absorption (micelles); enterohepatic circulation conserves them.
- Gallbladder: Stores/concentrates bile; CCK triggers contraction and sphincter of Oddi relaxation.
- Liver detoxification: Phase I (P450) and Phase II (conjugation) metabolize drugs/toxins.
- Portal Hypertension: ↑portal pressure (>5-10 mmHg) leads to varices, ascites.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

