Gut Microbiome - Meet Your Inner Ecosystem
- Definition: A complex community of $10^{13}-10^{14}$ microorganisms (bacteria, viruses, fungi, archaea) residing in the gastrointestinal tract. Their collective genetic material is termed the "microbiome".
- Key Phyla (approximate abundance):
- Firmicutes (~60-80%)
- Bacteroidetes (~20-40%)
- Actinobacteria (~1-10%)
- Proteobacteria (variable, <5% in health)
- Diversity:
- Alpha diversity: Richness and evenness of species within a single sample.
- Beta diversity: Extent of similarity or difference in microbial composition between samples.
- Stability/Resilience: The ability of the microbiome to resist change (stability) and return to its baseline state after a disturbance (resilience).
- Factors Influencing Gut Microbiome:
- Mode of birth: Vaginal (Lactobacillus, Prevotella) vs. C-section (skin flora like Staphylococcus).
- Diet: High fiber promotes diversity; high fat/sugar can alter balance.
- Antibiotics: Can cause short or long-term dysbiosis, reducing diversity.
- Age: Colonization starts at birth, diversifies through infancy, stabilizes in adulthood, may decline in diversity in the elderly.
- Host genetics: Influences immune interaction with microbes.
- Geography & Lifestyle.
⭐ The Firmicutes/Bacteroidetes (F/B) ratio is a frequently discussed biomarker. An elevated F/B ratio is often observed in obesity, but its interpretation is complex and context-dependent. It is not a standalone diagnostic marker but an area of active research for its potential role in metabolic health and disease.
Gut Microbiome - Functions & Favours
The gut microbiome has crucial physiological roles:
-
Metabolic Functions:
- SCFA Production: $Dietary Fiber \xrightarrow{Microbiota} SCFAs$ (📌 BAP: Butyrate, Acetate, Propionate)
- Butyrate: Colonocyte fuel; anti-inflammatory.
- Acetate: Cholesterol synthesis, lipogenesis.
- Propionate: Hepatic gluconeogenesis, satiety.
- Vitamin Synthesis: Vit K, B vitamins (B12, folate, biotin).
- Bile Acid Metabolism: Primary $\rightarrow$ Secondary bile acids (e.g., deoxycholic acid).
- Xenobiotic & Drug Metabolism: Detoxification, drug processing.
- SCFA Production: $Dietary Fiber \xrightarrow{Microbiota} SCFAs$ (📌 BAP: Butyrate, Acetate, Propionate)
-
Protective Functions:
- Colonization Resistance: Against pathogens (e.g., C. difficile); nutrient competition.
- Gut Barrier Integrity: Enhances mucus layer, tight junctions.
-
Immune System Development & Modulation:
- Immune Education: Matures innate & adaptive immunity.
- IgA Production: ↑ Secretory IgA (sIgA).
- Treg Induction: Promotes regulatory T cells (Tregs).
- Cytokine Balance: Modulates pro/anti-inflammatory cytokines.
⭐ Butyrate, a key SCFA produced by gut bacteria from dietary fiber, is the preferred energy source for colonocytes and exerts potent anti-inflammatory effects.
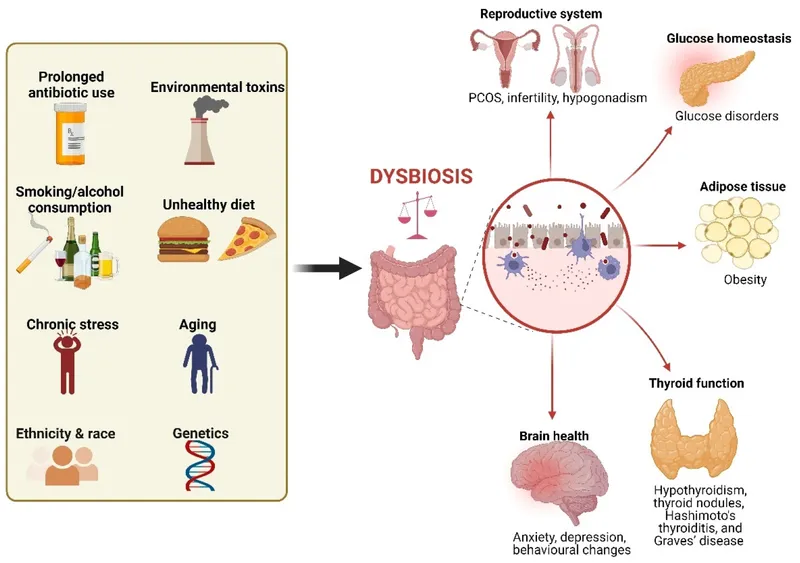
Gut Microbiome - Dysbiosis & Drama
Dysbiosis: Imbalance in gut microbial composition, diversity, or function.
- Mechanisms:
- Loss of beneficial microbes (e.g., Lactobacillus).
- Pathobiont overgrowth.
- Reduced microbial diversity.
Associated Diseases:
- IBD (Crohn's, UC): ↓Faecalibacterium prausnitzii.
- IBS: Variable dysbiosis.
- Obesity & Metabolic Syndrome: Altered F/B ratio, ↓diversity.
- T2DM: Links to insulin resistance.
- C. difficile Infection (CDI): Post-antibiotic.
- Allergies/Asthma: Immune dysregulation.
- Colorectal Cancer (CRC): ↑Fusobacterium nucleatum.
- NAFLD/NASH: Gut-liver axis.
- Gut-Brain Axis Disorders (Autism, Depression, Anxiety).
Modulation Strategies:
- Probiotics: Live beneficial microbes.
- Prebiotics: e.g., inulin, FOS (fuel good bacteria).
- Synbiotics: Pro + Prebiotics.
- Diet: Fiber-rich.
- FMT: For recurrent CDI (efficacy >90%).
⭐ Fecal Microbiota Transplantation (FMT) demonstrates high efficacy (often >90%) in treating recurrent Clostridioides difficile infection, a condition frequently precipitated by antibiotic-induced dysbiosis.
High-Yield Points - ⚡ Biggest Takeaways
- Gut microbiome: Predominantly anaerobic bacteria; Firmicutes & Bacteroidetes are dominant.
- Functions: Vitamin K & B synthesis, SCFA production (butyrate), immune modulation, colonization resistance.
- Dysbiosis linked to IBD, obesity, metabolic syndrome.
- Probiotics (live microbes) & prebiotics (substrates) modulate microbiome.
- FMT effective for recurrent C. difficile infection.
- Diet is a major modulator of gut microbiome.
- Butyrate (an SCFA) is key energy for colonocytes; anti-inflammatory効果 (kouka - effect/efficacy, but sticking to English as per general style).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

