Salivary Secretions - Mouth's Magic Mix
- Daily Volume: 1-1.5 L. pH 6.0-7.0.
- Composition: 99.5% water; electrolytes ($Na^+$, $K^+$, $Cl^-$, $HCO_3^-$); enzymes (α-amylase, lingual lipase); mucus; lysozyme, IgA.
- Functions: Lubrication, speech, starch digestion (amylase), fat digestion (lingual lipase), taste, antibacterial, buffering ($HCO_3^-$).
- Regulation (ANS):
- Parasympathetic (CN VII, IX): ↑ copious, watery saliva. 📌 "Salivation: Seven & Nine's Design".
- Sympathetic (T1-T3): Transient ↑ viscous saliva, then ↓.
⭐ Saliva is always hypotonic to plasma. Key reason: ductal cells reabsorb more sodium & chloride than they secrete potassium & bicarbonate.
oka
Gastric Secretions - Stomach's Acid Bath
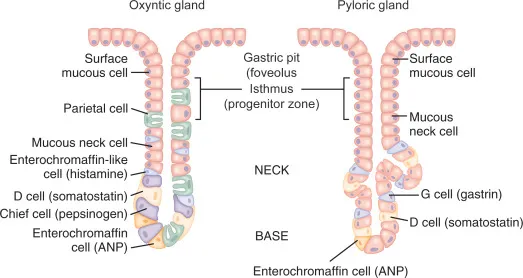
- Parietal (Oxyntic) Cells:
- HCl (via $H^+$/$K^+$ ATPase); pH 1.5-3.5, activates pepsinogen, antimicrobial.
- Intrinsic Factor (IF) essential for Vitamin B12 absorption (terminal ileum).
- Chief (Peptic) Cells: Pepsinogen.
- Pepsinogen $\xrightarrow{HCl}$ Pepsin (protein digestion).
- Mucous Cells (Neck & Surface): Mucus & $HCO_3^-$ (protective mucosal barrier).
- G Cells (Antrum): Gastrin (↑ HCl, motility, mucosal growth).
- ECL Cells: Histamine (potent HCl stimulant via H2 receptors).
- D Cells (Antrum, Body): Somatostatin (↓ HCl, gastrin, histamine).
HCl Regulation:
- Stimulants: Gastrin, Acetylcholine (ACh - vagal), Histamine.
- Inhibitors: Somatostatin, Prostaglandins (PGE2), Secretin.
- Phases: Cephalic (vagal), Gastric (food/distension), Intestinal (hormonal).
⭐ Zollinger-Ellison Syndrome: gastrinoma → ↑gastrin → ↑HCl → severe peptic ulcers.
Pancreatic Secretions - Pancreas' Enzyme Party
Exocrine pancreas:
- Acinar cells: Synthesize & secrete digestive enzymes (zymogens).
- Ductal cells: Secrete aqueous bicarbonate ($HCO_3^-$) solution, neutralizing duodenal pH.
Phases of Secretion: Cephalic & Gastric (vagal, minor), Intestinal (hormonal, major).
Enzymatic Component (Acinar Secretion):
- Proteolytic: Trypsinogen (activated by enterokinase to trypsin), Chymotrypsinogen, Procarboxypeptidase, Proelastase (all activated by trypsin).
- Amylolytic: Pancreatic α-amylase (digests starch).
- Lipolytic: Pancreatic lipase (main fat digestion, requires colipase), Phospholipase A2, Cholesterol esterase.
Aqueous Component (Ductal Secretion):
- Rich in $HCO_3^-$; neutralizes gastric acid.
- $CFTR$ channel crucial for $HCO_3^-$ secretion.
Regulation (Intestinal Phase Dominant):

⭐ Secretin primarily stimulates bicarbonate secretion from pancreatic ductal cells, while CCK is the main stimulant for enzyme release from acinar cells. Pancreatic lipase is essential for fat digestion.
Bile & Intestinal Secretions - Gut's Dynamic Duo
- Bile:
- Liver (production), Gallbladder (storage, concentration).
- Key components: Bile salts (fat emulsification), bilirubin, cholesterol, lecithin.
- Aids fat digestion/absorption (Vits A,D,E,K); neutralizes chyme; excretes bilirubin, cholesterol.
- Regulators: CCK (contracts gallbladder), Secretin (↑ $HCO_3^-$ in bile).
- Enterohepatic circulation: >90% bile salts reabsorbed (terminal ileum).
- Intestinal Secretions (Succus Entericus):
- Source: Crypts of Lieberkühn; Brunner's glands (duodenum: alkaline mucus).
- Daily volume: 1-2 L; pH: 7.5-8.0.
- Composition: Water, mucus, electrolytes. Enzymes (brush border: disaccharidases, peptidases; lumen: enterokinase).
- Role: Final nutrient digestion, mucosal protection.
- Regulated by: Local reflexes, VIP.

⭐ Bile salt-independent bile flow, crucial for ductal $HCO_3^-$ secretion, is primarily stimulated by Secretin.
High‑Yield Points - ⚡ Biggest Takeaways
- Parietal cells: Secrete HCl (via H+/K+ ATPase) and Intrinsic Factor (for Vit B12 absorption).
- Chief cells: Release Pepsinogen, activated to pepsin by HCl.
- Pancreas: Enzymes (amylase, lipase, proteases) stimulated by CCK; Bicarbonate (neutralizes acid) by Secretin.
- Bile: From liver/gallbladder, bile salts emulsify fats; CCK stimulates release.
- Gastrin stimulates acid secretion; Somatostatin is a key inhibitor of GI secretions.
- Brunner's glands in duodenum secrete alkaline mucus protecting mucosa.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

