BER & Smooth Muscle - Gut's Electric Beat
- Basic Electrical Rhythm (BER):
- Rhythmic slow waves (oscillating membrane potentials) in GI smooth muscle.
- Generated by specialized pacemaker cells (see ⭐ below).
- Determine maximum contraction frequency.
- Frequency varies: Stomach (3/min), Duodenum (12/min), Ileum (8-9/min).
- Do not directly cause contraction (except stomach); require additional stimuli for spike potentials.
- GI Smooth Muscle Contraction:
- Unitary type; cells electrically coupled by gap junctions.
- Contraction occurs when slow wave peak + excitatory stimuli depolarize membrane to threshold.
- This triggers Ca²⁺ influx and spike potentials (true action potentials) superimposed on slow waves → contraction.
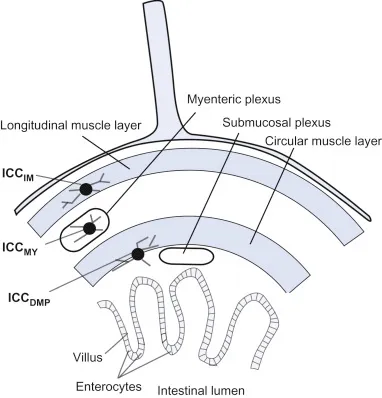
⭐ Interstitial Cells of Cajal (ICCs) are the pacemakers of the gut, generating slow waves (BER).
Regulation of Motility - Motility's Masterminds
- Neural Control:
- Enteric Nervous System (ENS) - "Gut's brain":
- Myenteric (Auerbach's) plexus: Motility control. 📌 Auerbach = Action.
- Submucosal (Meissner's) plexus: Secretion, blood flow. 📌 Submucosal = Secretion.
- Autonomic Nervous System (ANS):
- Parasympathetic (ACh): ↑ Motility (Vagus, pelvic nerves).
- Sympathetic (NE): ↓ Motility.
- Enteric Nervous System (ENS) - "Gut's brain":
- Hormonal Control:
- Excitatory:
- Motilin (M cells): MMC Phase III initiation.
- Gastrin (G cells): ↑ Gastric, intestinal motility.
- CCK (I cells): ↑ Gallbladder contraction; ↓ gastric emptying.
- Serotonin (5-HT, EC cells): ↑ Motility.
- Inhibitory:
- Secretin (S cells): ↓ Gastric emptying & motility.
- Somatostatin (D cells): Universal GI inhibitor.
- VIP: Sphincter relaxation; ↓ intestinal motility.

- Excitatory:
⭐ Motilin, secreted from M cells of the duodenum and jejunum, initiates Phase III of the Migrating Motor Complex (MMC) during fasting.
Regional Motility - The GI Transit Show
- Swallowing (Deglutition):
- Phases: Oral (voluntary), Pharyngeal (involuntary reflex, airway protection via epiglottis & vocal cords, apnea), Esophageal (involuntary peristalsis).
- UES & LES relaxation coordinated.
- Esophageal Motility:
- UES (cricopharyngeus): prevents aerophagia. LES: prevents GERD.
- Peristalsis: Primary (swallow-initiated), Secondary (distension-clears refluxate).
- Gastric Motility:
- Storage: Receptive relaxation (vagovagal), gastric accommodation.
- Mixing: Antral peristalsis (BER by ICC, ~3/min). Retropulsion.
- Emptying: Pyloric sphincter control. Factors: ↑volume, ↓fat, ↓acid in duodenum. Liquids > Solids.
- Migrating Motor Complex (MMC): Interdigestive, motilin-driven, "housekeeping".
- Small Intestine Motility:
- Segmentation: Mixing, ↑contact time. BER gradient (duodenum ~12/min, ileum ~8/min).
- Peristalsis: Propulsive.
⭐ The 'Law of the Gut' states that peristaltic contraction typically occurs on the oral side of a bolus with relaxation on the anal side, propelling contents aborally.
- Large Intestine Motility:
- Haustrations (mixing, slow shuttling).
- Mass movements: Propulsive (1-3/day), gastrocolic & duodenocolic reflexes.
- Defecation: Rectal distension → internal anal sphincter relaxation (involuntary) → external anal sphincter control (voluntary).
Motility Disorders - Motility Mishaps
- Achalasia Cardia: Failure of LES relaxation, aperistalsis. Dysphagia to solids & liquids.
⭐ Achalasia cardia is characterized by impaired LES relaxation and aperistalsis of the esophageal body, often presenting with a 'bird's beak' appearance on barium swallow.
- GERD: ↓LES tone. Heartburn, regurgitation.
- Gastroparesis: Delayed gastric emptying. Nausea, vomiting. Common in diabetes.
- Hirschsprung's Disease: Aganglionic megacolon. Neonatal constipation.
- IBS: Altered bowel habits, abdominal pain. Motility & visceral hypersensitivity issues.
High‑Yield Points - ⚡ Biggest Takeaways
- BER (Basal Electrical Rhythm) by ICCs (Interstitial Cells of Cajal) dictates max contraction frequency: Stomach ~3/min, Duodenum ~12/min.
- MMC (Migrating Motor Complex): Fasting "housekeeper" driven by motilin; feeding abolishes it.
- Peristalsis: ENS (Enteric Nervous System) coordinated; proximal ACh/Substance P (contraction), distal NO/VIP (relaxation).
- Segmentation: Primary mixing movement, prominent in the small intestine.
- Gastrocolic reflex: Food in stomach → ↑ colon motility; involves gastrin and extrinsic nerves.
- Achalasia cardia: LES (Lower Esophageal Sphincter) fails to relax, esophageal aperistalsis; due to loss of myenteric plexus inhibitory (NO/VIP) neurons.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

